
With Healogram telehealth technology, wound surface area is automatically calculated using a disposable calibration sticker and computer vision techniques. A hologram (or watermark) of the original image is displayed to guide subsequent photos for consistency. (All images courtesy of Healogram.)
By Hank Black
Many experts believe that comprehensive acceptance of telemedicine for prevention and monitoring of diabetic wounds and other lower extremity care is right around the corner.
In 2005, Howard Umansky, DPM, of St. Petersburg, FL, founded the Diabetic Rural Outreach Project (DROP International), which utilizes telemedicine to remotely monitor patients with diabetic wounds in China, the Caribbean, and the US. He started with relatively simple technology–furnishing basic computers with webcams and using services like Skype. Where no Internet was available, landline-linked videophones sufficed.
“Today, smartphones have decreased our cost and provided a host of even better options for imaging and monitoring diabetic complications,” Umansky said in a recent podcast.1 “In almost ten years, and across thousands of patients, our team has experienced only one amputation due to a lower extremity wound, and I credit that largely to telemedicine.”
Umansky’s relatively small organization uses a simple “see it, snap it, send it” model for monitoring of wound care and prevention of additional wounds.
“Prevention is the best alternative, of course. Wounds don’t usually start out five centimeters across but as a small red dot or series of dots that coalesce, so daily self-examination is critical in order for us to intervene at the earliest possible stage,” he said.
But giant systems like the US Department of Veterans Affairs (VA) have set up linked platforms that enable a nurse to take and securely transmit even 3D images for evaluation by specialists. And, between home visits, veterans’ diabetes and wound data are regularly transmitted to a dedicated patient alignment team watching for danger signs that would necessitate an intervention.
Those examples and others illustrate the potential of telemedicine to revolutionize delivery of diabetic foot care around the world. In research labs and high-tech business incubators across the nation, countless more projects are in development for the next generation of advances.
Into the mainstream?
Lower extremity healthcare practitioners and researchers and officials from health organizations, state legislatures, and telecommunications enterprises are among many who believe that comprehensive acceptance of telemedicine for prevention and monitoring of diabetic wounds and other care is right around the corner. Is this the year that federal and other insurers will finally cover, in a comprehensive manner, medical services delivered remotely? Bean counters in cash-strapped state governments, millennials pursuing the next “killer app,” and practitioners who see parity in quality of care from telemedicine are joining a chorus of other hopefuls who say the promise will become reality soon, and telemedicine will finally integrate into the medical mainstream.
And none too soon. As an aging “time bomb” ticks away in advanced societies and epidemics of obesity, diabetes, and other chronic diseases loom while numbers of practitioners are stretched thin, the delivery of healthcare from a distance is seen as a promising strategy for confronting these threats.2
Plenty of hurdles remain before this happens–none more difficult to solve than whether, as currently constituted, telemedicine is financially viable–but technological advances, plus the lure of providing standard-of-care healthcare to off-site and underserved patients with the cost-efficiency of electronic communications, are spurring rapid growth in the field, say many experts.3,4
Telemedicine (or telehealth, a broader term) takes many forms. To the American Telemedicine Association (ATA), it is the exchange of medical information from one site to another via electronic communications to improve a patient’s clinical health status. It includes the use of two-way video, email, smart phones, wireless tools, and other telecommunications technology. It may include consultations between practitioners and may use live interactions or store-and-forward transmission of images, vital signs, patient data, and the like. Consumer medical and health information and professional medical education may also be included.5
The government-funded National Telehealth Resource Center says that, in principle, no regulatory distinction should exist between telehealth services and those delivered in person. Quality and practice standards should be the same for both, and as both types of services merge, the “tele” prefix should disappear.6
Recent changes in the ATA’s operational guidelines make it clear that telemedicine is no longer considered fringe care.7
“Telemedicine has been around some twenty-five years and is becoming very much mainstream, reimbursable in certain circumstances,” said former ATA President Elizabeth A. Krupinski, PhD, professor and vice chair of medical imaging research at the University of Arizona in Tucson. “One major change we have made is that telemedicine is no longer considered to be research, so we dropped the idea of informed consent for patients in favor of enhanced patient and provider education. Patients sign the same forms pertaining to consent to care, HIPAA [the Health Information Privacy and Accountability Act], and others as they would if they were in the doctor’s office.”
Umansky points to the increasing ability to remotely collect patients’ biometrics through nanofiber sensors in bandages and other means as a dramatic improvement in wound care.
“The pace of technology today is phenomenal–from smartphone attachments such as a dermatophone or an ankle brachial index cuff to the wearable sensors that can transmit temperature and other changes in a wound,” he said. “The ability to monitor blood flow is coming soon, and that will be an added game-changer. The ability to monitor depth, volume, and temperature of diabetic ulcers, along with a wide host of other innovations, gives us a wealth of data that makes us ever more secure in our management of these wounds.”
Getting in the game
Some envision a gold rush on the tech side as numerous start-up companies jostle for prominence and established telecommunications giants integrate platforms and applications to tie health systems together.3
New enterprises that seek to disrupt the traditional healthcare model with telemedicine applications are flooding high-tech incubators around the country. At least one mobile platform that helps practitioners remotely monitor healing of postsurgical and other types of wounds has entered pilot studies to assess the cost savings of remote versus in-person follow-ups, quality of care, and patient and clinician satisfaction.
Large information and technology communications companies are in the game too, wooing providers and patients with application portfolios based in cloud servers that are HIPAA-compliant. The American Diabetes Association’s free 24/7 app that gives users help in monitoring their disease is included in Microsoft’s HealthVault and others. AT&T has boosted the ability of hospital networks to centrally manage radiologic images and collaborate with other networks and practitioners. And Verizon is only one of several companies that has launched Federal Drug Administration-approved remote patient monitoring platforms that enable use of biometric devices to automatically send patient data to its secure cloud.3
In some other countries, practitioners can rely on simpler technology without having to jump through HIPAA and other US privacy hoops. The issues of device and privacy regulations are moot in China, for example. That enables Umansky’s nonprofit organization to operate on a model that merely asks patients with diabetes to examine their skin daily and send pictures of even minor changes with their name to one of two wound centers for evaluation.
“Everybody in Chongqing and Wuhan has a smartphone, so it’s simple, cheap, and cost-efficient by preventing major problems from developing from the simplest epidermal change,” he said.
Mississippi, which has high poverty levels, a low ratio of physicians to residents, and some of the worst rates of obesity and diabetes in the US, uses patient-based smartphones or tablet computers and a care management application to monitor glucose and other pertinent data from patients remotely and connect them with providers. Kristi Henderson, DNP, chief telehealth and innovation officer at the University of Mississippi Medical Center in Jackson and head of its Diabetes Telehealth Network care management program, said these tools help give many people with diabetes in the rural Delta region control of their illness for the first time since diagnosis.8
And from a patient satisfaction point of view, Henderson said, “We’re hearing from patients, ‘Don’t take this away.’”
Mississippi officials began adopting telehealth several years ago to help a state in which 65% of people have to go more than 40 miles to see a specialist. That state’s regulatory and policy changes have made it one of only seven in the nation to receive an A rating from the ATA, Henderson said. For example, telehealth appointments are reimbursed on par with in-person visits by all public and private payers in the state. Henderson said many other states have not overcome resistance to change due to fears about the quality of telehealth and outdated policies.9
Numerous projects have demonstrated that telemonitoring and telehealth interventions, however low-tech, can improve clinical outcomes for people with diabetes. Even texting has been shown to have the ability to sustainably improve diabetic health metrics in both rural and urban populations, and across multiple languages.10-12
If low-tech solutions can keep diabetic symptoms under control, remote diabetic wound care is heavily dependent on observation of images by expert practitioners, and better images and transmission usually mean specialists can provide a more accurate clinical report. No providers are ahead of the VA in employing these capabilities.
Patients are now beginning to receive the benefit of the latest technology to image wounds in both 2D and 3D for remote transmission to specialists. David Chmielewski, MBA, the VA Cleveland Facility telehealth coordinator, said the programs will be piloted this year in the 14 VA primary care clinics in Ohio before being rolled out across the country.
“The mobile wound management system will be incorporated into our home telehealth program to provide a 2D imaging system in the form of a dedicated smartphone for use by patients in their homes. Patients or a family member or neighbor will be trained in their use by nurses in the home or in a clinic visit,” he said.
A separate, portable system uses stereography to record 3D images taken by VA employees in the patients’ homes, Chmielewski said.
“Those pictures of wounds will automatically upload to a secure website for specialists to review on a desktop computer,” he said. “Our intent is to avoid the exacerbation of wounds that often occurs when patients travel to primary care clinics or specialized centers.”
He explained that both 2D and 3D systems eliminate unnecessary visits to clinics and specialized centers.
“Home telehealth modalities save two thousand dollars per patient, and even more when wound management is involved, because foot ulcers in particular get worse with movement travel. A patient may have a wound rated a three on a scale of one to ten when they leave the house, but it may be a six or seven by the time they get to clinic because of all the movement involved,” Chmielewski said. “That raises the cost associated with seeing the patient in a clinic, so that’s a major impetus for us to roll out a program to remotely monitor wounds. It’s not just the cost of getting to the clinic but the cost of more expensive treatment for a wound that is even more advanced.”
Minimizing the need for patient transportation is also a priority at the Louis Stokes Cleveland VA Medical Center in Ohio, said Richard Strozewski, telehealth master preceptor.
“If a patient has a neuropathic ulcer in the bottom of the foot and has to drive even a couple of miles to the primary clinic or two to three hours to a specialized center and then walk in, this obviously will irritate the wound. The best-case scenario is to get the image right out of the patient’s home,” Strozewski said. “This is where we start to combine technologies based on patient needs. The image is taken at the home and the doctor may then want to do a live video visit with the patient about how they are feeling, or a nurse may be on site in the home and may be asked to do some palpations, or other diagnostic tools may come into play.”
Almost one-third of patients in the Ohio VA system participate in some form of telehealth or telemedicine, and about half are in some form of virtual care, Chmielewski said. The former category includes the home telehealth program, clinical live (synchronous) video telehealth, and store-and-forward telehealth. Virtual care also includes a patient portal MyHealth eVet, E-Consult, and an education program for primary care physicians called Specialty Care Access Network (SCAN).
While one stereography system is getting a major boost through the VA, others are not far behind. A system that provides a portable 3D color representation of a wound with several different measurement tools, including color analysis, although not intended for use by patients, has undergone considerable evaluation with published results,13,14 and the UK’s National Health Service has authorized it for further development as a promising technology.
The more complex and physically larger systems are designed both to assess wound images and maintain wound records for a large number of patients, with an associated high acquisition cost, and are thus not intended for self-utilization by patients. Other products seek to fill that niche or are in the pipeline. The advanced systems are costly and require on-site professionals to take the images. However, advances in smartphone technology are prompting researchers to develop more patient-friendly products.
Thinking inside the box
Peder C. Pedersen, PhD, professor of electrical and computer engineering at Worcester Polytechnic Institute in Worcester, MA, said the computational capability of current smartphones has spurred his research group to develop a wound imaging and analysis system for patients with chronic foot ulcers. The smartphone system allows patients or their caregivers to capture consistent images of their wound, at regular intervals, on a smartphone combined with a low-cost image capture box containing specifically positioned mirrors. The box was built in his laboratory for about $100, he said.
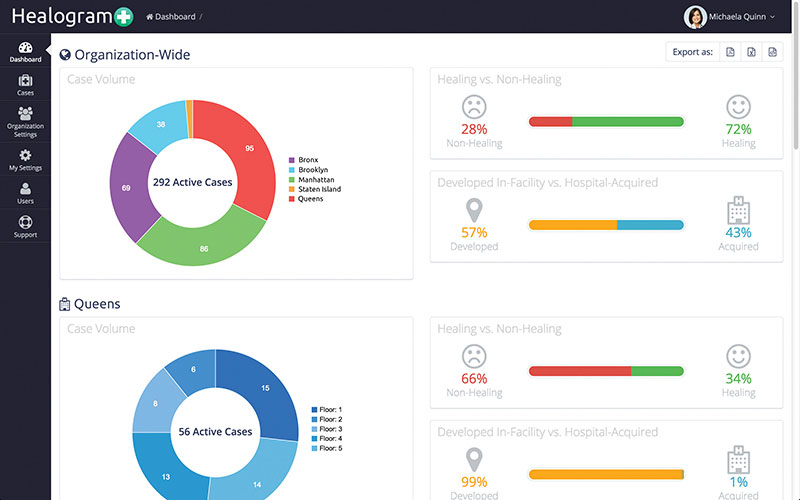
A view of the clinicians’ electronic dashboard, which gives care teams a quantitative population-level snapshot of how their wound patients are faring by territory, facility, and other measures.
“You clip the phone on the box, put the affected foot on the rectangular opening on the box, and take the picture with a voice command. Once FDA regulations are met, the system can automatically transmit the data to the patient’s electronic health record at the wound clinic,” Pedersen said.
The system employs simple algorithms that calculate the outline of the foot and the wound boundary and assesses quantitative healing status based on color spectral analysis. Pedersen said a pilot study of the system’s efficacy will be carried out in 2015.15
Early adopters of telemedicine such as the VA are seeing transformations in remote care for diabetic and other wounds coming sooner rather than later. Technologies now in early release or under development that are being evaluated for utility include stereography; holography, as in vector imaging; the advancement of devices in products like Google Glass; and multiple other wearable technologies.
“In addition, through developing and incorporating the use of smartphones and their apps for telehealth, we can provide patients with better tools and give them the ability to be active participants in managing their healthcare,” Strozewski said.
For example, that might involve transmitting data to guide footwear modifications in patients at risk for neuropathic foot ulcers. The patient might stand on an instrumented platform that could collect pressure and temperature data and transmit it to a specialist who would then make the appropriate modifications to the shoe, he said.
“As digital technologies evolve and become more cost-effective and user-friendly, we continuously evaluate how they can be incorporated into telehealth as tools that collect current, pertinent, and useful data that can be delivered rapidly in summarized forms to providers, allowing them to make better, more precise, and quicker clinical decisions,” Strozewski said.
Reimbursement is key
Reimbursement is seen as the key impediment to telemedicine that, once conquered, will carry it into the healthcare mainstream.
“Telemedicine will explode in the next couple of years because everything is falling into place for when Medicare rolls out a reimbursement schedule; insurers will then follow suit and the last barrier will fall,” Umansky said.
In fact, the Centers for Medicare and Medicaid Services (CMS) is incrementally loosening requirements for reimbursement and use of telemedicine services. In December 2014, CMS proposed waiving certain restrictions on the use of telemedicine by the nation’s 330 Accountable Care Organizations, which are responsible for managing care for large groups of patients under what is labeled “population management.” The ATA recently called on CMS to use similar flexibility in Medicare’s managed care plans.16
As for Medicaid, a patchwork of insurance requirements and various payment streams does not allow providers and patients to take complete advantage of available telemedicine services. Each state has different policies. Nevertheless, a recent ATA analysis of gaps in reimbursement and policy showed the number of states with laws giving parity to telemedicine and traditional healthcare models has doubled in the past three years.17
With payers coming on board, and technology improving exponentially, it is apparent the future of medicine will include telemedicine. There are barriers, but as Mississippi’s Henderson said, they are not insurmountable.
“We have overcome them here with visionary leaders. And if you can do it in Mississippi, you can do it anywhere,” she said.9
Hank Black is a medical writer in Birmingham, AL.
- The Health Crossroad: Where the Stories Behind Health Converge. Podcast #36: Dr. Howard Umansky: Pioneering Telemedicine and mHealth to Drive Improved Outcomes. Health Crossroad website. http://www.thehealthcrossroad.com/podcasts/entrepreneurs/umansky/. Published April 21, 2014. Accessed January 7, 2015.
- Dowsett C, Bielby A, Searl, R, et al. Reconciling increasing wound care demands with available resources. J Wound Care J Wound Care 2014;23(11):552-562.
- Banerjee S, Chanmugam R, Samtani M. An app a day: Enabling the digital doctor. Outlook 2014;27(1):28-37.
- Kharif O. Telemedicine: Doctor visits via video calls. Bloomberg Businessweek website. http://www.businessweek.com/articles/2014-02-27/health-insurers -add-telemedicine-services-to-cut-costs. Published February 27, 2014. Accessed January 7, 2015.
- What is Telemedicine. American Telemedicine Association website. http://www.americantelemed.org/about-telemedicine/what-is-telemedicine#.VK2UP2TF-c. Accessed January 7, 2015.
- A Framework for Defining Telehealth. National Telehealth Resource Centers website. http://www.telehealthresourcecenter.org/sites/main/files/file-attachments/telehealth_definintion_framework_for_trcs_1.pdf. Accessed January 7, 2015.
- Core Operational Guidelines for Telehealth Services Involving Provider-Patient Interactions. American Telemedicine Association website. http://www.americantelemed.org/resources/telemedicine-practice-guidelines/telemedicine-practice-guidelines/core-operational-guidelines-for-telehealth-services-involving-provider-patient-interactions#.VK2U7WTF-c8. Published May 2014.
- Perma G. Solving Mississippi’s Health Care Problems with Telehealth and Care Management. Healthcare Informatics website. http://www.healthcare-informatics.com/article/solving-mississippi-s-diabetes-problem-telehealth-and-care-management. Published November 14, 2014. Accessed January 8, 2014.
- Mississippi leads the nation in telehealth. Robert Wood Johnson Foundation website. http://www.rwjf.org/en/about-rwjf/newsroom/newsroom-content/2014/12/mississippi-leads-the-nation-in-telehealth.html. Published Dececember 12, 2014. Accessed January 8, 2015.
- Shane-McWhorter L, Lenert L, Petersen M, et al. The Utah remote monitoring project: Improving health care one patient at a time. Diabetes Technol Ther 2014;16(10):653-660.
- Nundy S, Mishra A, Hogan P, et al. How do mobile phone diabetes programs drive behavior change? Evidence from a mixed methods observational cohort study. Diabetes Educ 2014;40(6):806-819.
- Arora S, Peters AL, Agy C, Menchine M. A mobile health intervention for inner city patients with poorly controlled diabetes: proof-of-concept of the TExT-MED program. Diabetes Technol Ther 2012;14(6):492-496.
- Bowling FL,Paterson J, Ndip A. Applying 21st century imaging technology to wound healing: An avant-gardist approach. J Diabetes Sci Technol 2013;7(5):1190-1194
- Hallam MJ, McNaught K, Thomas AN, et al. A practical and objective approach to scar colour assessment. J Plast Reconstr Aesthet Surg 2013;66(10):e271-276.
- Wang L, Pedersen, PC, Strong DM, et al. Smartphone based wound assessment system for patients with diabetes. IEEE Trans Biomed Eng 2014 Sep 17. [Epub ahead of print]
- CMS answers American Telemedicine Association’s call for telehealth by ACOs. American Telemedicine Association website. http://www.americantelemed.org/news-landing/2014/12/02/cms-answers-american-telemedicine-association-s-call-for-telehealth-by-acos#.VKg0puk5Bjo. Published December 2, 2014. Accessed January 7, 2015.
- State Telemedicine Gaps Analysis, Coverage and Reimbursement. American Telemedicine Association website. http://www.americantelemed.org/policy/state-telemedicine-policy#.VKiIfDY5Bjo. Published April 2014. Accessed January 7, 2015.









Hank, great article, thanks for the read. I think telemedics can be a great device for diabetics. With all of the foot pathology that can go wrong, a picture is worth a thousand words. How about a diabetic ulcer patient who can not be on their feet? Let’s get a picture via Skype and have the physician follow the progress, change treatment plans and discuss prognosis with the patient. The future is here.
Teri Green
Atlas Biomechanics