LER Cover Story:
Wound Talk with Dr. Windy Cole: Giving Lymphedema the Squeeze: All Things Compression
In traditional medicine, we often treat the vascular, integumentary, and lymphatic systems as separate silos. However, the “Veil Theory,” championed by Dr. Heather Hettrick, reveals that these systems are inextricably linked. At the center of this connection is the endothelial glycocalyx, a microscopic, sieve-like layer within our blood vessels that regulates the movement of fluid and proteins.
By Dr. Windy Cole, DPM, CWSP, FACCWS, FFPM RCPS (Glasg) with Dr. Loan Lam DPM, FAWPHc, FAPWCA, CWSP, CHWS, CLWT and guest Cam Ayala
lerEXPO Upcoming Events
Feature Articles
lerEXPO Highlights: AI-Assisted Risk Stratification and Management in Diabetic Limb Salvage
The global prevalence of diabetes is increasing and is projected to affect 642 million people by 2040, highlighting the growing need for effective prevention, management, and supportive care. Diabetes can be associated with a range of health complications that require ongoing medical attention. Among these, diabetic foot conditions–particularly ulcerations and infections–are leading contributors to non-traumatic lower-limb amputations.
By Dr. Laura Shin
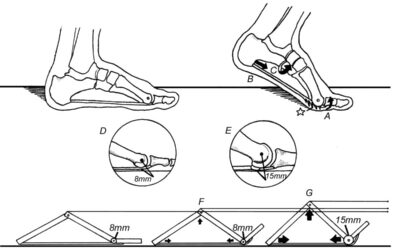
Rethinking the Role of the Plantar Fascia’s Windlass Mechanism
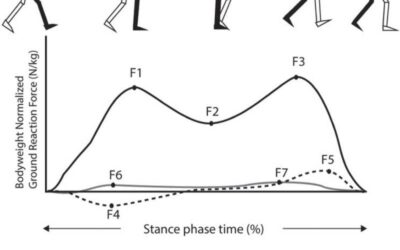
Ever since Sahelanthropus tchadensis stood upright 7 million years ago, the feet of our common ancestors have undergone a series of important structural changes necessary to accommodate the functional requirements of bipedal locomotion. While the feet of arboreal primates were well-adapted for grasping branches during movement through tree canopies, their hypermobile midfoot and adducted great toe led to instability and buckling during the push-off phase of gait…
By Tom Michaud, DC, and Nicolas Haelewijn, Ph. D.
The Halo Effect of Technology in Podiatric Practice
When patients enter a podiatry office, their impressions begin forming immediately. Before any history is taken or exam performed, they are already processing what they see. Eyes are drawn to the physical space, the efficiency of the front desk, the demeanor of the staff. They enter the treatment room and notice the equipment in the room while waiting for the physician. These early signals shape expectations in ways that are both subtle and powerful.
By Mikel D. Daniels, DPM, MBA, President and Chief Medical Officer, WeTreatFeet Podiatry
Questions, Answers & Commentaries About AFOs
I would like to thank the reader for acknowledging my expertise. I want to reiterate that the literature supports functional context as a focus of rehabilitation as opposed to just impairment-based interventions. We must treat the person as a whole entity (person: mental, emotional, physical, spiritual, intellectual) of who they are in their lived spaces (environment) and what they do in that space (tasks).
By Dr. Jennifaye V. Brown
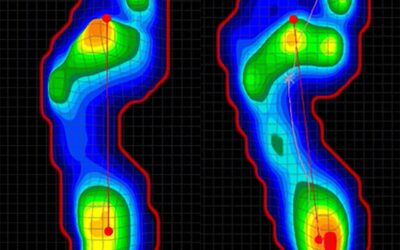
CAGA 101: The 12 Dirty Truths of Foot Mechanics
If you have been following our articles, you may have noticed a trend in how computer-aided gait analysis (CAGA) data can help characterize unavoidable and avoidable truths about your 2 feet and the long-term consequences. When it comes to footwear, even research supports the fact that improper footwear and “wear and tear” over time will have negative impacts on foot health.
By Jay Segel, DPM; Sally Crawford, MS
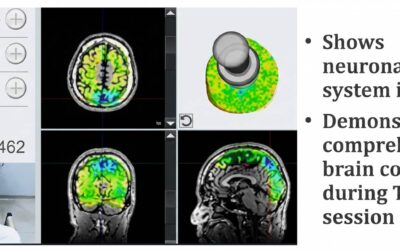
Application Of Transcranial Pulse Stim in Rehab: Pain Management in Knee Osteoarthritis
Knee osteoarthritis (KOA) is the most prevalent form of arthritis among adults and a leading cause of disability worldwide. The condition affects hundreds of millions of individuals and represents a substantial burden on healthcare systems. Chronic knee pain is the primary symptom and frequently prompts individuals to seek medical care. However, the management of chronic osteoarthritis pain remains challenging.
Trending Now
Lower Extremity Review
ShortTakes From the Literature
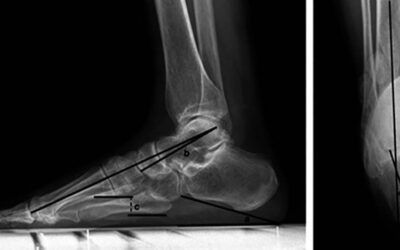
CLAI Patients with Subtle Cavus Foot: Is Calcaneal Osteotomy an Essential Procedure?
Chronic lateral ankle instability (CLAI), frequently resulting from ankle...
Inflammation and Nutrition-Based Indicators for Predicting DFUs
Inflammation and nutritional status are increasingly recognized as key...
Honey Dressing for Diabetic Foot Ulcers: A Systematic Review
Researchers conducted a systematic review and meta-analysis following PRISMA...
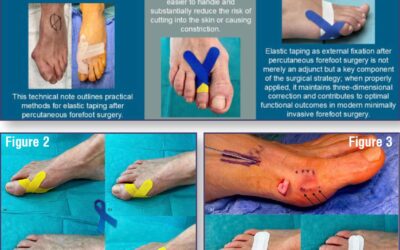
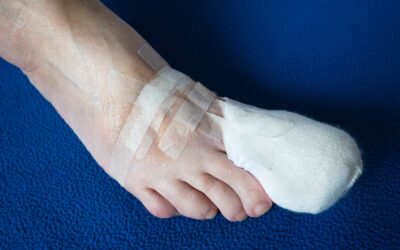
Elastic Taping of Toes after Percutaneous Forefoot Surgery: Technical Tip
Figure 2. The tape is applied centrally on the lateral aspect around the base...
Ewing Sarcoma of The Great Toe: A Rare Case Report
Ewing sarcoma (ES) rarely arises in the toes, where nonspecific pain and...
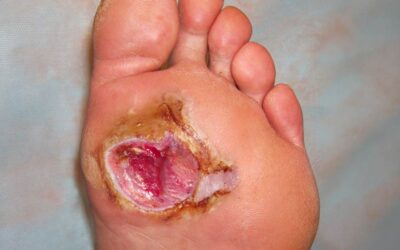
Foot To Fatality: Alarming Outcomes Following Acute Diabetic Foot Infections
Acute, deep infections of diabetes-related foot ulcers can present as surgical...
Treatment and Cost of Athletic Training in High Schools for Knee and Ankle
The monetary costs of sport-related injuries are significant, but complexity...
The Relationship Between Clinical Outcomes and Gait Biomechanics in PF
Plantar fasciitis (PF) is a common musculoskeletal disorder characterized by...
A Foot Forward for Optimum Health
Questions, Answers & Commentaries About AFOs
I would like to thank the reader for acknowledging my expertise. I want to reiterate that the literature supports functional context as a focus of rehabilitation as opposed to just impairment-based interventions. We must treat the person as a whole entity (person: mental, emotional, physical, spiritual, intellectual) of who they are in their lived spaces (environment) and what they do in that space (tasks).
By Dr. Jennifaye V. Brown
Industry News & Updates
CMS Announces 2 New L-codes
The Centers for Medicare & Medicaid Services (CMS) recently released their...
Implantable Neurotechnology Could Help Prosthetic Legs Work More Like Intact Limbs
A research team led by researchers at Chalmers University of Technology in...
Researcher Developing New Diabetic Neuropathy Treatment
A University of Central Florida (UCF) College of Medicine scientist is...
Trigger of Tendon Disease Discovered
Overuse of our tendons can cause painful medical conditions, known as...

GLP1 Receptor Agonist Use Is Associated with Increased Risk of Osteoporosis, Gout, and Osteomalacia in Adults with Type 2 Diabetes and Obesity
INTRODUCTION: Glucagon-like peptide-1 receptor agonists (GLP-1 RAs) have become central to the...
Robotic-Assisted Total Knee Arthroplasty is Associated with Improved Quality of Life and Increased Patient Satisfaction One Year after Surgery
INTRODUCTION: Approximately 15–20% of patients undergoing conventional total knee arthroplasty...
Early Sports Specialization Is Associated with Increased Orthopaedic Injury Incidence in NFL Athletes
INTRODUCTION: Single-sport specialization during adolescence has been increasingly adopted by...
E-Bike Orthopaedic Injuries Amongst Pediatric and Adolescent Patients at a Level I Trauma Center
INTRODUCTION: Electronic bicycle (E-bike) use is on the rise in the United States. E-bikes are a...
AAOS Highlights New AJRR Data
The American Academy of Orthopaedic Surgeons (AAOS) Registry Program highlighted new findings from...
A Message From the Publisher
Welcome to Lower Extremity Review or LER as we call it. This long awaited magazine fills the lower extremity information gap for practitioners in the fields of Podiatry, Physical Therapy, O&P Pedorthics, and Orthopedics. With over 20 years experience in multi-disciplinary editorial development and publishing, the collaboration of this incredible team has made this publication possible

Rich Dubin
Publisher and Chief Executive Officer
Featured Products
Lower Extremity Review
Pickleball Footwear
The All Court Vehicle (ACV) Pro delivers all-court performance with every move, while providing the comfort, support, and confidence players need to dominate a match. The breathable Aero-Step™ insert technology provides targeted airflow to keep feet cool and dry...
Performance Socks
Revitalign® Performance Socks are designed to meet the demands of a dynamic lifestyle. Recognizing that support shouldn’t end with shoes, the company developed a sock that incorporates biomechanical technology to enhance foot wellness throughout the day. Each pair is...
Clog Built Around a Custom Orthotic
The Surefoot footwear collection was engineered entirely around a patient’s custom orthotic. Powered by Amfit® full-contact foot-scanning technology, the collection represents a fundamental shift in how supportive footwear is designed, prescribed, and worn. The result...
Sensory Insole Program to Combat Diabetes-Related Complications
Orpyx® Medical Technologies’ next-generation sensory insole program is a proactive, scalable solution to prevent diabetes-related foot complications. This new platform combines durable wearable technology and behavioral support to enable healthcare providers to...
Dynamic Air Compression Device for Hips, IT Bands, Lower Back
The Normatec Elite Hips is a fully portable dynamic air compression device specifically engineered for the hips, iliotibial (IT) bands, and lower back. This standalone device represents a new era of targeted recovery, eliminating the need for separate control units...
Bio-Integrative, Metal-Free Implants to Improve Soft Tissue Fixation
OSSIOfiber® 2.5mm Suture Anchors offer 55% greater pull-out strength over the market-leading 2.4 mm biocomposite suture anchor. They feature a novel material engineered without metal to integrate into bone. Indications for use include suture or tissue fixation in the...
Lined Clog Built Around a Custom Orthotic
Surefoot has launched a footwear collection engineered entirely around a patient’s custom orthotic. Powered by Amfit® full-contact foot-scanning technology, the collection represents a fundamental shift in how supportive footwear is designed, prescribed, and worn. The...
Ankle Fusion Cage System
restor3d’s Ossera™ AFX Ankle Fusion Cage System, a comprehensive platform engineered to address complex ankle fusion cases, is available in both standard off-the-shelf and made-to-order configurations. The Ossera AFX portfolio includes a standardized implant offering...
Robotically Enabled Saw for Knee Replacements
The Mako RPS (Robotic Power System) for Total Knee is an intuitive handheld robotic system that combines Stryker’s proven robotics and power tool legacies and represents Mako’s expansion into a new robotics platform. Compatible with Stryker’s Triathlon® Total Knee...