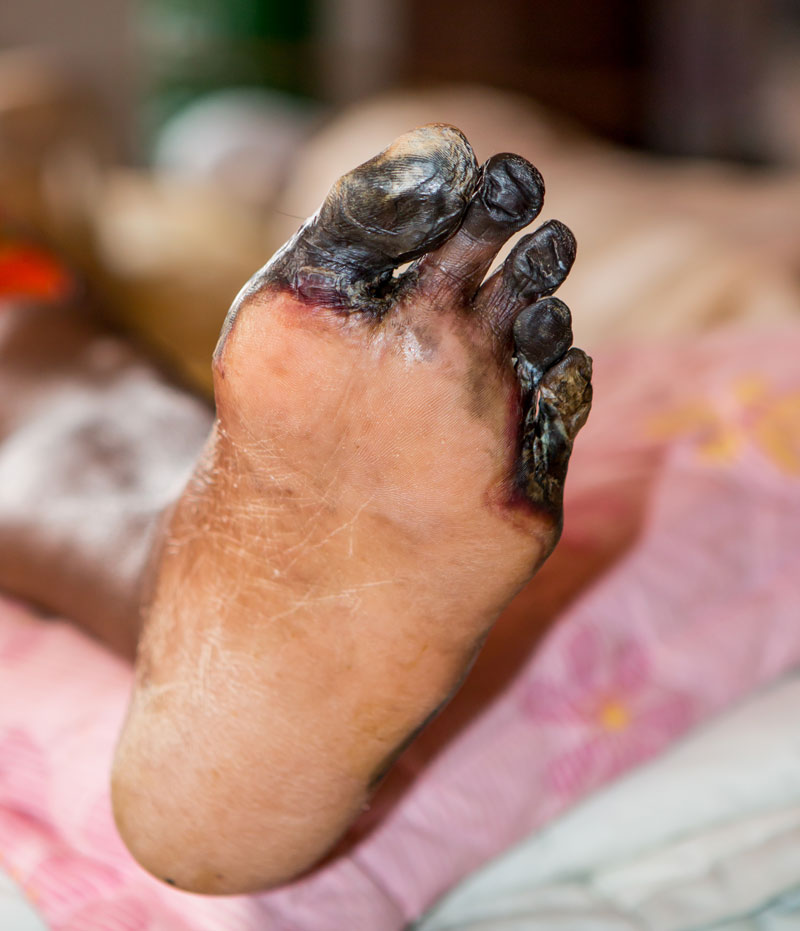
iStockphoto.com #583995670
New research invigorates arguments about limb salvage vs. more proximal amputations
By Cary Groner
A recent paper from researchers in Australia has reignited the ongoing debate about the relative merits of partial-foot versus transtibial amputations, particularly in diabetes patients.1 For clinicians who deal with limb salvage and rehabilitation, it’s a challenging topic, as their decisions carry significant implications for their patients’ longevity and quality of life.
In the January issue of Disability and Rehabilitation, the researchers interviewed 10 patients about their experiences after they had undergone sequential partial-foot amputations (PFAs) followed by transtibial amputations (TTAs). The authors reported that participants tended to report positive reactions to their eventual TTAs, largely because of the physical and emotional suffering that came with the poorly healing wounds and sequential surgeries associated with multiple PFAs. A related theme of the interviews was that patients had often received incomplete information about PFAs, whereas the facts available about TTAs were relatively robust. The study’s participants generally expressed the wish that they’d had more informative conversations—and better involvement in decision making—with their caregivers throughout the process, rather than just when it came to the more proximal surgery.
The paper’s lead author, Michael Dillon, PhD, BPO(Hons), an associate professor at National Centre for Prosthetics & Orthotics at La Trobe University in Melbourne, told LER that he and his colleagues were interested in what these patients’ path through the healthcare system was like—and in particular whether they might have made other choices had they known in advance what they would endure.
David Armstrong, DPM, MD, PhD
“Every patient wants the least amputation possible, and every doctor wants to give them that,” Dillon said. “But we had this group of people who’d gone through multiple amputation surgeries, and when we talked to them, we found that many of them wished they had made different decisions.” Specifically, most wished they’d had the TTA sooner and skipped some of the intervening steps.
Dillon has a longtime interest in this subject, but he said his research was influenced in part by his wife’s experience with breast cancer. After consulting with a genetic counselor, she ultimately decided on a double mastectomy to most effectively reduce her risk of recurrence.
“The counselor was very skillful in facilitating some difficult conversations related to mortality and the evidence for more invasive surgery,” Dillon said. “Having walked that journey with her, I started to see parallels with the decisions people have to make about lower-extremity amputations.”
Dillon and his colleagues were often surprised by what they found when they talked to the study participants. One patient, for example, was so cognitively impaired by the pain medications he received after his PFAs that he was largely unable to process what his doctors were saying about his treatment. Once, in a waiting room, he realized to his shock that two hours had passed while he’d stared into a fish tank.
“It makes absolutely no difference how good of a consult you’ve had with your surgeon if you aren’t capable of absorbing anything he told you,” Dillon said. “Some patients need multiple opportunities to learn in order for doctors to feel confident they’ve made an informed decision. The one-stop consult before you go into surgery isn’t going to cut it.”

iStockphoto.com #1129812327
Dillon’s study has limitations—it’s a small sample size with subjective and retrospective outcomes. Moreover, it contains a selection bias, in that every patient in it had already undergone a TTA; those who’d had long-term success with PFAs, and hadn’t needed more proximal amputations, might have told a different story. In fact, a 2017 article said as much: in that study, 94% of patients who’d undergone a series of PFAs said they’d prefer to repeat those procedures rather than have a TTA.2
These issues aside, Dillon’s article sheds light on important issues caregivers deal with every day as they work with their patients to make the best possible decisions.
Nearing the End
A theme returned to repeatedly by the clinicians LER spoke with has to do with end-of-life choices. People with lower-extremity amputations typically have grim long-term prognoses, and it’s even worse for those with diabetes. One in 5 foot ulcers ultimately leads to some level of amputation, and in the U.S., diabetes patients have about 80,000 amputations every year.3 Despite these interventions, within 5 years roughly 40% of patients diagnosed with new diabetic foot ulcers will die.4 As Dillon told LER in a previous article, “When you consider that a large proportion of them will be dead in 5 years, a PFA that takes months to heal is a poor outcome, irrespective of how much of the foot is left.”5
Others noted the complexity of clinical decision making.
“The real answer is that there is no answer,” said David Armstrong, DPM, MD, PhD, a professor of surgery and director of the Southwestern Academic Limb Salvage Alliance (SALSA) at USC’s Keck School of Medicine. “It depends on what the patient needs at a given time, what they’re going through, and what the doctor thinks will be most helpful. If you’re considering a high-level amputation, sometimes people need time to grieve for the part of their body they’re going to lose. There are other people who want to go the distance with PFAs, and they want you to do that with them. And there are people in between, which is where 95% of our patients are.”
For Armstrong, the most important message from Dillon’s study has to do with communication.
“This problem is like cancer, but we’re not talking to our patients as if they have cancer,” he said. “When we talk in terms not of cure but of remission, they start to see it differently. Some people just opt to have their foot amputated, but many others understand that if they keep part of the foot it’s likely they’ll get another wound. In those cases, the goal is to make that wound as uncomplicated and as infrequent as possible. Our goal is ulcer-free days, hospital-free days, and if possible, activity-rich days—sort of a holy trinity of outcomes. It’s easy to say, ‘Just cut the thing off and be done with it,’ but that’s not always for the best.”
Michael Pinzur, MD
Decisions
Michael Pinzur, MD, a professor of orthopedic surgery and rehabilitation at Loyola University Medical Center in Maywood, IL, advocates a four-step approach to such decisions.6 First, will limb salvage do better than a higher-level amputation and prosthetic limb? Second, what is a realistic expectation for either salvage or amputation? Third, what are the costs of limb salvage to the patient—particularly given the risk of multiple surgeries—not just financially but in terms of suffering and lost time? And fourth, what are the risks associated with treatment, especially the relatively greater risks of reinfection in a PFA versus a TTA?
“The goal is not limb salvage, it’s salvage of functional independence,” Pinzur said. “You have to think about the patient as a whole, learn about the level of their disease, consider their potential for rehabilitation and their possible life span. I don’t want a patient spending the last year of their life dealing with a wound.”
Pinzur acknowledged that surgeons would much prefer to do a PFA than a below-knee procedure; and indeed, since the year 2000, the number of PFAs performed has risen while that of TTAs has declined.7 The advantages of PFA include improved mobility and QOL as well as lower mortality—though the higher death rate associated with TTA is likely associated with disease severity rather than the procedure itself.8,9
Only about half of PFAs heal, however, and two-thirds of PFA patients ultimately require a more proximal amputation.10 The decision-making process is particularly complex given the variables associated with recovery and rehabilitation, and for that matter TTAs are certainly no panacea.
Armstrong explained the difficulties.
“Sometimes we think that once somebody gets a transtibial amputation, they’re done with surgery, but it isn’t true,” he said. “All things being equal, a TTA is more likely to heal, but a good result is not a foregone conclusion.”
Pinzur agreed. “Up to 15% of below-knee amputations have will have significant complications,” he said. “Half of those can be resolved with second and third surgeries, and half can’t. You can’t guarantee that people will heal at the BK level, and the 2-year mortality rate is about 36%.”

iStockphoto.com #898328226
On the other hand, there are the problems with PFAs that Dillon and his colleagues pointed out in their recent paper. Pinzur noted that certain patient profiles make PFA a poor choice.
“People with renal failure will not heal distal operations,” he said. “If a patient’s serum albumin is below 3, there’s a 60% failure risk—which means going to a higher amputation.”
Pinzur has his own guidelines for assessing whether surgeons are choosing the correct level at which to amputate.
“If you use a multidisciplinary evaluation, the surgery should heal at the level you choose about 90% of the time,” he said. “If you have 100% success, it means you’re amputating too high.”
These considerations reflect the dizzying array of PFAs surgeons can perform. Amputation options, from distal to proximal, include the toes, metatarsal ray, transmetatarsal, Lisfranc (a tarsometatarsal disarticulation), Chopart (disarticulation through the talonavicular and calcaneocuboid joints), the Pirogoff and Boyd (which preserve some of the calcaneus), and the Syme, which ends at the distal base of the tibia.11 Perhaps not surprisingly, a lack of clear definitions of what constitutes a PFA has muddied the waters when it comes to collecting data about success rates.12
Teams
Pinzur’s reference to a multidisciplinary approach is worth noting. One factor that’s significantly changed the game in decisions about limb salvage is the team approach to care, which incorporates not just surgeons but diabetologists, podiatrists, physical therapists and other rehabilitation specialists, and particularly vascular surgeons.13
“In the past 25 years, there have been so many advances in endovascular surgery, and in management of patients with good-quality open surgery, that it’s now rare to see patients who are not vascular candidates,” Armstrong said. “But when you’re working with your colleagues, knowing statistically there’s so much we can do to prolong the life of the limb, we still have to marry that with a little emotional intelligence and experience. That’s a good combination, so that we constantly check ourselves and our patients and calculate how things are going. We call it limb salvage, but it’s really life salvage.”
For Jonathan Labovitz, DPM, medical director of the Foot & Ankle Center at the Western University of Health Sciences in Pomona, CA, communication between the care team and the patient is crucial.
Jonathan Labovitz, DPM
“We need to have systems in place to help people with information,” he said. “Health literacy is extremely important, because if the patient doesn’t understand what’s wrong with them and what to expect, they’re less likely to adhere to treatment.”
Pinzur added, “You’ve got to look at their rehabilitation potential, their biological capacity to heal,” he said. “But 2 portents of bad outcomes are covert psychiatric disease and cognitive dysfunction.”
Cognitive impairment may arise from diabetes itself as well as from the painkillers used to ameliorate the effects of surgery. And not surprisingly, patients facing life-altering surgeries and drastically shortened life spans may be prone to depression. As a result, clinicians increasingly recognize how much the patient’s mental health may affect recovery, and psychiatrists and psychologists have come to constitute a more important part of the care team as well.
“I do a depression assessment prior to doing an amputation, unless it’s emergent,” said Labovitz. “If they have moderate to severe depression, I automatically refer them to psychiatry first.”
Labovitz has had cases in which foot ulcers and other wounds stubbornly refused to heal until the patients addressed their psychological issues, at which point things began to improve.
“I found out by talking to the psychiatrist that one person was alcoholic but was in denial to me,” he said. “Psychiatrists talk to them differently; they have their own ways of doing things. Once the patient’s depression or other issues are addressed, they start healing better.”
Labovitz echoed Pinzur and Armstrong in terms of the importance of understanding patients’ goals.
“If their goal is to complete a triathlon, but they haven’t walked in a year, that may be unrealistic,” he said. “But if we take the time to talk to our patients—discuss the procedure and the length of rehabilitation, the potential complications and benefits—then we can adjust those expectations. That will improve adherence to the plan and reduce complication rates. The question is how to help them function and live the life they want; in one patient that might be a transmetatarsal amputation, and in another, a transtibial.”
Michael Dillon pointed out that patients are often dealing with psychosocial issues beyond just their medical concerns.
“We sometimes miss that many of these people are dealing with multiple other problems,” he said, noting that one patient had to manage a difficult teenage daughter and a husband who had just lost a job, all while simultaneously navigating decisions about amputation.
Dillon was also taken aback by how little information his study participants had received on their journey through the health system.
“Most of them come through a high-risk foot service,” he said. “They’ve had diabetes, an injury, or an infection that’s led to ulceration, and they’ve been having treatment for months or even years. So it was surprising to us that most of them seemed to have no idea what was likely to happen if that ulcer didn’t heal. At some point you’ve got to have that conversation. In Australia, those systems are much better for people facing a TTA than for those considering a PFA, and it was disheartening that about 15% of those in the group had 3 or more amputation surgeries on that limb within 12 months of their PFA. I can’t imagine how horrendous that would be.”
Fears and Support
Support and information should go beyond conversations with surgeons, rehab specialists, and psychiatrists, according to Dane Wukich, MD, who holds the Dr. Charles F. Gregory Distinguished Chair in Orthopedic Surgery at the University of Texas Southwestern Medical Center in Dallas.
“It’s important that patients who are contemplating an amputation talk to someone who’s had that surgery,” Wukich told LER. “These patients fear losing their foot more than they fear dying.14 It’s a big mental issue for them, and certainly depression, if unrecognized or untreated, results in higher morbidity and mortality.”
In making decisions about amputation level, Wukich primarily considers the condition of the bones and soft tissue. One issue with PFAs is that they create a variety of problems in the foot that require different forms of intervention.
“When you’re doing any foot amputation, you have to recognize that the soft tissues, tendons, and ligaments are very important,” he said. “You really have to think about tendon balancing and reconstructive procedures once the infection is eradicated.”
Michael Dillon, PhD, BPO(Hons)
Wukich acknowledged mixed feelings about sequential PFAs, however. As in many cases, it depends on how you define the term.
“If you do a toe amputation and it doesn’t heal, but a vascular surgeon can do a procedure to provide enough blood supply to heal a transmetatarsal amputation, absolutely you should try that,” he said. “Nine times out of 10 that will be a better procedure for the patient than a TTA. If a toe amputation doesn’t work, to jump to a below-knee makes no sense to me.”
That said, Wukich acknowledged that for the right patient, a TTA is a good surgery. “The best results for those are in people who will be able to ambulate with a prosthesis,” he said. “Patients who can get their function back and walk actually do very well, and the energy expenditure isn’t significantly higher than walking with a PFA.”
Wukich admitted, however, that many patients are simply not ready to take that step.
“I’ve done it both ways, but unless someone is really, really sick, I try to let the patient make the decision,” he said. “I ask if they want to try to save their leg, and if the answer is yes, I’ll do everything I can. But I don’t consider a below-knee amputation a failure, and some patients do very well with them. The goal is physical quality of life, which is directly related to ambulation.”
The Gist
What it all comes down to, essentially, seems to be this: Distal is better until it isn’t. Presented with this stark formula, Armstrong agreed.
“I think that’s absolutely true,” he said. “We have to bear in mind that people generally deal with emergencies much better than with chronic problems like the diabetic foot, and doctors are no exception to that. Our goal as clinicians is to reduce the number of acute complications so that ideally patients don’t have to choose between life and limb.”
Cary Groner is a freelance writer in the San Francisco Bay area.
- Dillon MP, Anderson SP, Duke EJ, Ozturk HE, Stuckey R. The lived experience of sequential partial foot and transtibial amputation. Disabil Rehabil. 2019:1-9.
- Hong CC, Tan JH, Lim SH, Nather A. Multiple limb salvage attempts for diabetic foot infections: is it worth it? Bone Joint J. 2017;99-b(11):1502-1507.
- Walsh JW, Hoffstad OJ, Sullivan MO, Margolis DJ. Association of diabetic foot ulcer and death in a population-based cohort from the United Kingdom. Diabet Med. 2016;33(11):1493-1498.
- Lavery LA, Armstrong DG, Wunderlich RP, Mohler MJ, Wendel CS, Lipsky BA. Risk factors for foot infections in individuals with diabetes. Diabetes Care. 2006;29(6):1288-1293.
- Groner C. Debating the complexities of partial foot amputation. LER. 2013;4(10):25-30.
- Pinzur MS. Outcomes-oriented amputation surgery. Plast Reconstr Surg. 2011;127 Suppl 1:241s-247s.
- Dillon MP, Fatone S, Quigley M. Describe the outcomes of dysvascular partial foot amputation and how these compare to transtibial amputation: a systematic review protocol for the development of shared decision-making resources. Syst Rev. 2015;4:173.
- Groner C. Limb salvage or amputation of the diabetic foot? LER. 2018;10(4):17-25.
- Dillon M, Fatone S, Quigley M. While Mortality Rates Differ After Dysvascular Partial Foot and Transtibial Amputation, Should They Influence the Choice of Amputation Level? Arch Phys Med Rehabil. 2017;98(9):1900-1902.
- Izumi Y, Satterfield K, Lee S, Harkless LB. Risk of reamputation in diabetic patients stratified by limb and level of amputation: a 10-year observation. Diabetes Care. 2006;29(3):566-570.
- Levy LA, Hetherington VJ.. Principles and practice of podiatric medicine. 2d ed. Brooklandville, MD: Data Trace; 2006.
- Dillon MP, Quigley M, Fatone S. A systematic review describing incidence rate and prevalence of dysvascular partial foot amputation; how both have changed over time and compare to transtibial amputation. Syst Rev. 2017;6(1):230.
- Groner C. Taking a team approach to diabetic limb salvage. LER. 2012;3(3):55-63.
- Wukich DK, Raspovic KM. Assessing Health-Related Quality of Life in Patients With Diabetic Foot Disease: Why Is It Important and How Can We Improve? The 2017 Roger E. Pecoraro Award Lecture. Diabetes Care. 2018;41(3):391-397.