By Joanna Reeves, Richard Jones, Anmin Liu, Leah Bent, Ana Martinez-Santos, and Christopher Nester
By Joanna Reeves, Richard Jones, Anmin Liu, Leah Bent, Ana Martinez-Santos, and Christopher Nester
Some have worried that foot orthoses that shift plantar load may alter the mechanical work of internal structures and change the size of muscle and connective tissues, and actually make them smaller. These authors challenge that notion.
The effect of foot orthoses (FOs) has not been well studied with respect to adaptations to the internal foot structures and skin sensitivity over time. Plantar pressure is altered with FOs, consequently altering the distribution of resultant force through foot tissues. Muscles and tendons can change their activity, size, and structure as a result of a change in loading with training, and intrinsic foot muscles can also change size in response to modified loading of the foot with altered footwear. Therefore, redistributing the external loading of the foot with FOs could alter muscle and connective tissue morphology. It has been suggested that FOs and arch support from footwear leads to smaller and weaker foot muscles. However, intervention studies on the effect of FOs on muscle are limited. Although there is evidence for altered tissue thickness and stiffness of the Achilles tendon and plantar fascia in pathologies such as diabetes, which will influence the distribution of plantar stress, the effect of FOs on these connective tissue also requires investigation.

Figure 1. Salfordinsole foot orthosis. The majority of participants (n=18) wore medium density ethylene vinyl acetate (EVA) or thermoplastic (Shore A 70) depicted.
Foot orthoses can alter the contact area at specific regions of the foot, like increase the contact area in the medial arch, which could influence skin sensitivity. Skin sensitivity is comprised of both peripheral (alterations to the cutaneous mechanoreceptor activation or transmission) and central influences (cortical plastic changes based on input). Changes in contact area could alter, and potentially increase, the capacity for cutaneous mechanoreceptors to detect mechanical stimuli. There are 4 different classes of mechanoreceptors in glabrous skin, like on the foot sole, which respond to stretch, contact forces, vibration, and pressure. Cortical plasticity allows for the potential for increased skin sensitivity through increasing the relevant area in the primary somatosensory cortex, and neurophysiological changes with training has been shown in primates following stroke. Increased pressure in the medial arch could increase sensitivity due to the increases in the relative weighting given to receptors from that region, or skin sensitivity could decrease if the receptors become desensitized. Altered stimulation of mechanoreceptors can modulate afferent feedback to the central nervous system, influencing muscle activity and movement of the lower and upper limbs. Consequently, the skin’s contribution to gait and posture could be influenced with use of FOs through long-term stimulation of mechanoreceptors (a response to mechanical load being elicited in mechanoreceptors repetitively over time).
Preliminary work (n=12) has shown using a metatarsal bar to increase pressure can increase skin sensitivity in the forefoot; however, the effect of increases in pressure on skin sensitivity in other regions of the foot with FOs has not been investigated. Skin sensitivity in the medial arch may adapt differently to pressure changes from the forefoot because the medial arch is not normally loaded, and is the most sensitive region of the foot, despite having potentially fewer mechanoreceptors than other regions. The arch region of the foot is of particular interest as it is frequently loaded in FOs interventions. The arch region also has the lowest perceptual threshold (greatest sensitivity), while the heel has the greatest perceptual threshold.

Figure 2. The foot sole with blue dots depicting the approximate locations of skin sensitivity testing. An additional site was on the dorsum at approximately the level of the distal interphalangeal joint between the hallux and second toe.
Prefabricated FOs were used by 93% of responders to a national survey of clinicians prescribing FOs in the UK, and ethylene vinyl acetate (EVA) and rigid plastic were the most commonly used materials for prefabricated FOs. The effect of FOs that affect loading under the heel and medial arch on soft tissue size and structure and foot/ankle skin sensitivity is unknown. The purpose of this study was to enhance our understanding of the mechanisms behind the effect of prefabricated FOs by investigating whether skin sensitivity and soft tissue morphology would be altered when plantar loading was changed with FOs.
Materials and methods
This study investigated the effects of FOs on foot soft tissue morphology and skin sensitivity over 3 months of use. Forty-one healthy participants wore prefabricated FOs (n=23) (Figure 1) or no insert (n=18) for 3 months. The FOs were prescribed specific to each participant, using criteria of a change in peak pressure of 8% in the medial arch (pressure increase) and medial heel (pressure decrease). Ultrasound images were recorded pre- and post-FOs use to derive cross-sectional area and thickness of abductor hallucis, flexor hallucis brevis, flexor digitorum brevis, and the Achilles tendon at the insertion and mid-portion (Figure 3). Plantar fascia thickness was measured at the insertion and midfoot. The minimal detectable difference (MDD) was established in piloting (n=7). Skin sensitivity (Figure 2) was measured with monofilaments at the dorsum (between the hallux and second toe), medial and lateral heel, medial and lateral arch, and the 1st metatarsal head.
For specifics, see full article at https://doi.org/10.1080/19424280.2021.1961880.
Results
Participants: Twelve of the 53 participants recruited dropped out, including 4 from the FOs group. One in the FOs group dropped out due to hip pain which they attributed to
the FOs. The other 3 participants in the FOs group who dropped out did not report an adverse event, but did not respond to the invitation to return for postintervention assessments. Several included participants experienced some foot soreness using the FOs, but this did not persist beyond week 1 and is typical, and these participants continued with the study.

Figure 3. Ultrasound image of the flexor hallucis brevis with 3 thickness measurements
(yellow lines).
Foot orthoses
The actual mean (± SD) change in peak pressure due to FOs was significantly larger than the minimum requirement. In the medial heel the mean reduction was 21% (± 14%, p=0.012) and for the lateral heel 17% (± 14%, p=0.004). Mean (± SD) peak pressure at the medial arch was significantly greater at 15% (± 19%, p=0.005), though not significantly greater at the lateral arch 7% (± 17%, p=0.106).
Compliance
Sixteen of the 23 participants in the FOs group completed the postintervention compliance questions and all, bar 1, wore the FOs for more than the minimum of 4 hours per day (mean ± SD: ~8.5 ± 3 h). The 7 participants who did not complete these questions had confirmed via email that they were wearing the FOs more than the minimum of 4 hours per day.
Physical activity levels
In the FOs group, 21/23 (91%) were active pre-intervention and 22/23 (96%) were active postintervention. In the control group, 14/18 (78%) were active pre-intervention and all remained so.

Figure 4. Median difference in ultrasound thickness from pre- to post-three months in the foot orthoses group (FOs) and control group for abductor hallucis (ABH), flexor digitorum brevis (FDB), flexor hallucis brevis (FHB), Achilles tendon at the insertional site on the calcaneus (ATINS) and the mid-portion (ATMID), proximal plantar fascia (PFINS) and mid-portion plantar fascia (PFMID).
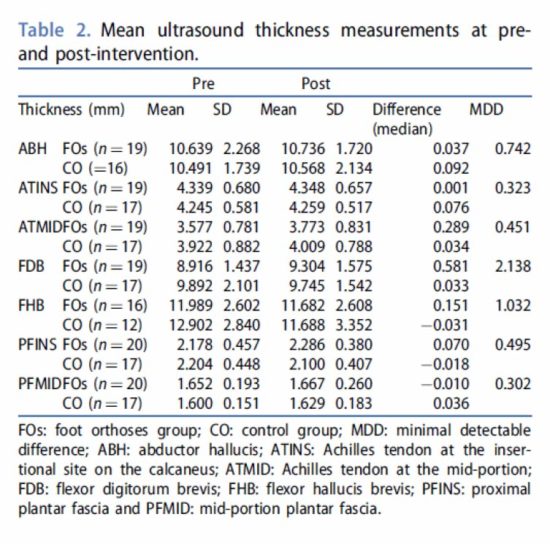
Ultrasound
Difference in ultrasound measurements pre- and post-intervention are presented in Figures 4 and 5 for thickness and cross-sectional area (CSA) respectively and mean values pre- and post-intervention are presented in Tables 2 and 3. No average difference in ultrasound measurement was greater than the MDD (Tables 2 and 3). There was a trend for an effect of time for ATMID thickness (p=0.056, ηp2 = 0.103) and a main effect of group for ATMID CSA (p=0.049, ηp2 ¼ 0.127) and other effect sizes were also small (<0.1).
Skin sensitivity: Mean skin temperature was 26.3°C (± 1.6°C) pre- and 29.8°C ± 1.3°C post-intervention, both above the recommended minimum threshold of 20°C. The monofilament results are presented in Table 4 and Figure 6, which are presented in the original article. There was a main effect of time for the 1st metatarsal head. Monofilament threshold increased with time for both control (0.34 ± 0.53 to 0.60 ± 0.55 g) and FOs groups (0.27 ± 0.42 g to 0.55 ± 0.62 g, p=0.003, ηp2 =0.211). There were no significant effects in other locations, with effect sizes <0.1 and large variability in thresholds across regions.
Discussion
This study investigated whether skin sensitivity and selected soft tissue morphology were altered when plantar loading changed due to use of FOs. Despite successfully altering pressure across the foot sole, the FOs did not significantly change soft tissue morphology or skin sensitivity when compared to the control group. There may be a number of reasons why this was the case. The neurophysiological and active and passive systems of the foot are thought to be flexible in coping with changing demands. So the change of demand with altered plantar loading due to FOs may have been accommodated without changing soft tissue morphology or sensory function. However, effects could have occurred in muscles other than those we could reliably assess with ultrasound, or other muscle properties or aspects of skin sensitivity that we did not measure. The daily wear time of FOs and study duration might also have been insufficient to cause changes. However, mean FOs wear time (8.5 hour/day) was arguably close to what could be expected in clinical practice and comparable to previous research and might therefore be considered a pragmatic dose of altered plantar loading. Several participants reported not wearing the FOs some days on weekends when indoors, which also likely reflects clinical practice. In a trial of custom FOs for patients with rheumatoid arthritis, FOs were worn 6 days/week on average. Increases in muscle CSA have been documented after 8–12 weeks, so it is conceivable that a 12-week FO intervention would be long enough to see change in intrinsic foot muscle CSA. Physical activity levels were comparable throughout and so unlikely to confound results.

Figure 5. Median difference in ultrasound cross sectional area (CSA) from pre- to post-three months in the foot orthoses group (FOs) and control group for abductor hallucis (ABH), flexor digitorum brevis (FDB), Achilles tendon at the insertional site on the calcaneus (ATINS) and the mid-portion (ATMID).
Soft tissue measures
A lack of change in the FOs group conflicts with previous research investigating FOs, whereby CSA decreased in the FOs group and not the control group and an earlier study that found an increase in CSA of ABH with FOs with and without the addition of short foot exercises. However, the study by Jung et al [2011] is difficult to interpret without a control group. The study by Protopapas and Perry [2020] only evaluated the cross-sectional area of 5 participants in each of a control and intervention group, reporting that FDB reduced 9.6% and ABH reduced 17.4% over 12 weeks. However, the MDDs of measures were not reported and the reduction in FDB CSA was smaller than the MDD in this study. Given the small sample size, the reported change might be measurement error and not meaningful. Furthermore, the results from this and earlier reliability work (2014) showed better measurement reliability for thickness rather than CSA. For example, limits of agreement were 13% and 13.5% for ABH and FDB thickness respectively, and 16% and 17% for ABH and FDB CSA. Using prefabricated FOs in this study rather than customized FOs could also explain the different outcomes, if match between FOs and foot shape influences neuromuscular adaptations. However, prefabricated and customized FOs have similar effects on peak plantar pressure and can be equally effective in reducing pain in a clinical population. Without knowledge of the change in plantar pressures or the material of the FOs in the earlier study, we cannot compare the changes in loads achieved. In the current study the mean 21% decrease in peak pressure at the medial heel and 15% increase in peak pressure at the medial arch with prefabricated FOs were similar or greater than a previous study using custom FOs that reflect common clinical practice, in which there was a 13% reduction in the medial heel and 15% increase in the medial midfoot.
 Skin sensitivity
Skin sensitivity
As participants were young, healthy, and mostly active, it is possible that they had little capacity to increase skin sensitivity. Baseline monofilament threshold in the medial arch was low, indicating high sensitivity (~0.1 g vs. ~1.0 g at the heel), which reflects the level of sensitivity previously reported in the literature. In this young healthy population, it may be that increased loading in this area would not increase sensitivity because it was already very sensitive. Alternatively, decreased sensitivity in one region could have increased sensitivity in another region that perhaps was not measured. Previous preliminary work has shown increased forefoot sensitivity following the use of a hard metatarsal pad. This differs from our results here. Differences could be attributed to the different methods of measuring skin sensitivity (the previous study used a bespoke loading device), different regions of pressure change (they used the forefoot, which is less sensitive than the medial arch), and/or the density of FOs material.
Mean skin temperature at the time of measurement increased by ~3.5°C from pre- to postintervention assessments, possibly due to seasonal weather variation, but remained within the typical range. This was not felt to mask any underlying change in sensitivity. The increase in monofilament threshold at the 1st metatarsal head with time in both groups could be interpreted simply as noise in the measurement.
 Nil effects could have been due to sample size, characteristics, or group allocation. The sample was pseudo-randomized as participants at one site were randomly allocated into groups (n=39) whereas at the other they were allocated on convenience (n=14), based on the sizes of FOs that were available at that location. There were no statistical differences in participant characteristics between the FOs and control groups for the latter sample, which refutes the idea that a lack of randomization contributed to a nil effect. The nil effects are unlikely due to a lack of power, as effect sizes were typically less than small (≤0.1). Although on visual inspection no differences in responses were observed between foot types, recruitment did not target specific foot types and so most participants had a neutral foot posture. Given the potential importance of sub-groups, perhaps the mixed sample of foot postures masked an effect of FOs for a specific foot type, as foot type and medial arch height in particular will influence the contact area of FOs with the foot and may also influence soft tissue size. Our sample size was insufficient to account for the effect of foot posture on foot soft tissue morphology or skin sensitivity. However, we used plantar pressure measures to ensure all participants experienced minimum changes in pressure independent of foot type. We were also not able to account for any changes in skin thickness, which partially influences skin sensitivity.
Nil effects could have been due to sample size, characteristics, or group allocation. The sample was pseudo-randomized as participants at one site were randomly allocated into groups (n=39) whereas at the other they were allocated on convenience (n=14), based on the sizes of FOs that were available at that location. There were no statistical differences in participant characteristics between the FOs and control groups for the latter sample, which refutes the idea that a lack of randomization contributed to a nil effect. The nil effects are unlikely due to a lack of power, as effect sizes were typically less than small (≤0.1). Although on visual inspection no differences in responses were observed between foot types, recruitment did not target specific foot types and so most participants had a neutral foot posture. Given the potential importance of sub-groups, perhaps the mixed sample of foot postures masked an effect of FOs for a specific foot type, as foot type and medial arch height in particular will influence the contact area of FOs with the foot and may also influence soft tissue size. Our sample size was insufficient to account for the effect of foot posture on foot soft tissue morphology or skin sensitivity. However, we used plantar pressure measures to ensure all participants experienced minimum changes in pressure independent of foot type. We were also not able to account for any changes in skin thickness, which partially influences skin sensitivity.
Conclusion
This study found no detectable change in foot soft tissue morphology nor skin sensitivity after 3 months of FOs use. Future study on the effects of FOs on the neuromuscular system could consider using alternative measurement techniques and foot posture subgroups. Although this study does not explain the mechanism of FOs benefits, it challenges the notion that FOs reduce muscle size.
This article has been excerpted from “No change in foot soft tissue morphology and skin sensitivity after three months of using foot orthoses that alter plantar pressure” by the same authors, which was published online August 18, 2021, in the journal Footwear Science. https://doi.org/10.1080/19424280.2021.1961880. Editing has occurred, including the renumbering of figures, and references have been removed for brevity. Use is per CC BY 4.0.