More than “just a sprain,” accurately diagnosing peroneal tendonitis in a timely manner helps patients recover faster and avoid long-term sequelae from this painful condition.
By Kevin Haag, DPM, PGY-3, and Marshall Solomon, DPM
 Peroneal tendon disorders have traditionally been considered a rare source of ankle symptoms. However, contemporary studies have brought the significance and frequency of peroneal pathology to light. It is critical to assess the patient for peroneal tendon pathology, including peroneal tendonitis. This condition can be a challenge to accurately diagnose as it is often overlooked in the face of the ever-present ankle sprain. Unfortunately, missed diagnoses or delayed treatment are associated with long-term sequelae.1 Developing a knowledge of the anatomy, epidemiology, diagnosis, and treatment of peroneal tendonitis is crucial for providing comprehensive care.
Peroneal tendon disorders have traditionally been considered a rare source of ankle symptoms. However, contemporary studies have brought the significance and frequency of peroneal pathology to light. It is critical to assess the patient for peroneal tendon pathology, including peroneal tendonitis. This condition can be a challenge to accurately diagnose as it is often overlooked in the face of the ever-present ankle sprain. Unfortunately, missed diagnoses or delayed treatment are associated with long-term sequelae.1 Developing a knowledge of the anatomy, epidemiology, diagnosis, and treatment of peroneal tendonitis is crucial for providing comprehensive care.
Anatomy and Normal Function
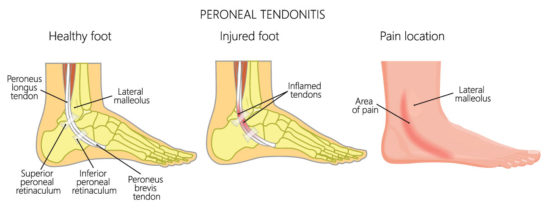
Both peroneus longus and brevis tendons begin their course along the lateral compartment of the leg and curve around the lateral malleolus in the peroneal tunnel together before heading separate ways to perform different tasks in the foot. They are separated at the peroneal tubercle on the calcaneus. The peroneus brevis tendon then inserts distally onto the base of the 5th metatarsal at the styloid process, while the peroneus longus tendon curves plantar to the peroneal sulcus of the cuboid bone and heads medially to insert onto the plantar lateral aspect of the medial cuneiform and first metatarsal base.
These tendons perform critical roles in balancing the foot and ankle. Both tendons are powerful everters of the foot. They serve this function during midstance and propulsion during the normal gait cycle. They also serve to stabilize the first ray and 5th metatarsal once contact has been made with the ground. In the face of excess strain on a foot or ankle, they both dynamically stabilize the lateral ankle complex to prevent damage and injury.
How Damage Develops
The peroneal tendons can develop pathology due to anatomic variants, direct and associated injuries, and altered biomechanics.
There are several known anatomic variants that increase the chance of a patient developing peroneal pathology. The concept of “overstuffing” of the peroneal tunnel has been mentioned as an important factor of anatomic variation leading toward peroneal tendonitis.1 Anatomic variations, such as a low-lying muscle belly (when a peroneal muscle extends past the tip of the lateral malleolus), accessory peroneal muscles, and altered shape of the retro-malleolar groove, can all create this effect.1,2,3 Other anatomic variants that can increase the risk of peroneal tendinopathy include a prominent peroneal tubercle and a calcified os peroneum.4,5 It is important to realize that, although variants exist, they are not a guarantee of pathology. In fact, a study of patients with asymptomatic feet and ankles revealed 72% possessed abnormal peroneal anatomy.3
It must be stressed that the peroneal tendons are designed to work in conjunction with an intact and healthy lateral ankle complex, as well as a biomechanically functional foot. If the lateral ankle (lateral ligaments and superior peroneal retinaculum) has been damaged, the peroneal tendons must shoulder an increased workload to keep the ankle stabilized throughout the gait cycle. This overuse results in inflammation and tendon damage. In fact, one classic study found that 77% of patients with a history of chronic ankle sprains and instability had inflammation in or around their peroneal tendons.6
Biomechanically, planovalgus and cavovarus deformities are often associated with peroneal tendon pathology. These foot types enable these tendons to experience overuse or compression-type injuries along their course.7 Several studies have pointed to the peroneal longus tendon as a major contributor of deformity in cavovarus feet.8 One study of cavovarus feet found enlargement of the peroneus longus tendon in more than 74% of the cases.9
While a history of previous ankle sprains or anatomic variants are common causes of peroneal tendonitis, not all individuals present like this. Other causes of peroneal tendonitis include unsupportive or inadequate footwear in an active individual or a recent significant increase in a new activity or training program that results in high demand on the peroneal complex. Almost all of these instances involve prolonged or repeated activity.
Making the Diagnosis
A comprehensive history is imperative to gain a full appreciation for this diagnosis, and it is important to ask specific and detailed questions about activity and recent changes, as well as acute injury, recent trauma, or chronic repetitive loading leading to injury. Eliciting a history that includes pain-causing activities, the nature of this pain, and localization of the pain will assist with making the diagnosis.
If one suspects peroneal pathology, the physical exam itself is not a challenge; however, it must be thorough. Several studies have found the history and physical examination to be of greater value than advanced imaging or other workup for this diagnosis.10,11 Patients will classically have pain and swelling along the path of the peroneal tendons. If the pathology has been present long enough, the findings can become more subtle and diffuse. Pain can also become focused overlying the posteriolateral ankle. For isolated inflammation of the brevis tendon, pain will follow the tendon into its insertion at the fifth metatarsal base. Focused inflammation of the longus tendon will often be present along the lateral aspect of the cuboid bone.12
A lateral stress test of the ankle can help uncover peroneal pathology. This test can be followed-up by stretching the peroneals via passive inversion and plantarflexion, as well as active eversion and dorsiflexion.13
Tools for Further Workup
As noted above, a thorough history and physical examination plays a large role in diagnosis of peroneal tendonitis. However, imaging studies can be used to support and confirm these findings.
Standard X-ray imaging should be obtained during any lateral ankle workup. This can help assess for bone-related sources of the pain, including an abnormal fibular groove, peroneal tubercle, hypertrophic 5th metatarsal base or other findings. Ultrasound imaging can also be a useful diagnostic tool which enables dynamic examination of the lateral ankle ligaments and peroneal tendons. It is cost effective and can be used to compare to the contra-lateral ankle and foot.14
Magnetic Resonance Imaging (MRI), considered the gold standard when evaluating the peroneal tendons, allows for clear visualization of the tendons and associated structures including the tendon sheath and excessive fluid found with inflammation. More than 3mm of fluid within the peroneal tendon sheath is considered diagnostic.15 However, an MRI is not without faults. Providers should be aware of false-negatives and false-positives. The famous “magic angle” occurs when a tendon is at 55 degrees from the magnetic field. Because the peroneals wrap around the ankle and change angles multiple times, they are at a higher likelihood than other tendons to produce this phenomenon. The magic angle can give the false impression of a tear. However, a truly damaged tendon will also have significant inflammation present.
While conservative therapy can be successful for most patients with peroneal tendonitis, if imaging reveals a hypertrophic tubercle with tendonitis, surgery should be pursued earlier on. Conservative therapy cannot remove this physical source of continual stress and damage to the tendons.4
Treatment
The majority of peroneal tendonitis can be addressed without surgical intervention. Early recognition and treatment will increase the odds of successful conservative therapy. However, many times patients presenting with peroneal tendonitis have been misdiagnosed and incorrectly treated in the past. It is critical to explain to the patient why their “ankle sprain” is really much more than a “just a sprain,” and what must be done to move toward a positive outcome. Empowering patients with an understanding of their real diagnosis is a powerful tool in any successful healthcare provider’s skill set.
Immobilization of the overworked peroneal tendons is a cornerstone of treatment. CAM boots, AFO bracing, or even casting can be utilized to achieve immobilization. Standard protocol with adequate time (usually a minimum of 6–8 weeks) for healing and reassessment should be used. Activity modification and alterations in shoe-gear and training can also be very effective.
Oral NSAIDs can also be safely used as a front-line treatment for this pathology. They are well tolerated in the majority of the patient population experiencing peroneal issues.
A recent study demonstrated that ultrasound-guided corticosteroid injection was relatively effective in patients with symptomatic peroneal tendon tears or tendinopathy. The steroid can be accurately injected into the peroneal tendon sheath offering another means of nonsurgical treatment.16
The use of platelet-rich plasma injection (PRP) for treatment of painful tendinopathy has become popular in recent years. While one randomized controlled trial17 which included PRP injections into peroneal tendons had promising results, a meta-analysis18 of 13 similar tendinopathy PRP trials found mixed results and no strong indication.
If patients continue to experience symptoms and pain for more than 3 months, extracorporeal shock wave therapy can be considered as a treatment option. A meta-analysis of 13 studies found that shock wave therapy can be a useful treatment modality and should be contemplated when initial nonoperative treatments have failed.19
Physical therapy with a focus on balance, strengthening, and proprioceptive rehabilitation can be a very beneficial treatment for both athletes and nonathletes. For nonathletic patients, all physical therapists will be able to provide excellent care. However, it is crucial to set up athletic patients with therapists that have sports medicine training due to their very specific needs.
Overall, conservative therapy tends to work very well in patients with lower functional demands, while patients with higher functional needs, such as elite athletes, may require surgery should conservative therapy fail. This is why developing a rigorous treatment plan that actively involves one’s patients is of utmost importance.
While the above treatments are effective tools in the direct treatment of peroneal tendonitis, providers must address contributing pathology if present. If a high school athlete developed peroneal tendonitis that resolved with treatment, it would be short-sighted to allow him/her to resume the exact same training regime without recommendations, modifications, and therapy.
In conclusion, peroneal tendonitis, while uncommon, is a unique pathology that is often misdiagnosed and overlooked. Fortunately, if a provider has a high index of suspicion, it can be diagnosed and managed successfully. It is critical to perform a thorough history and comprehensive examination. This should be followed up with the appropriate imaging studies, including X-rays, ultrasounds, and MRI, as needed. Conservative therapy can then produce excellent outcomes if applied correctly. If these steps are taken, providers can help patients overcome peroneal tendonitis without intervening surgically or developing long-term sequelae.
Kevin Haag, DPM, is a third-year resident in foot and ankle surgery at Beaumont Hospital, Farmington Hills, Michigan.
Marshall Solomon, DPM, is a foot and ankle surgeon at the Foot Care Institute of Michigan and the Beaumont Hospital Podiatry Clinic and is the podiatry residency program director at the Beaumont Hospital, Farmington Hills, all in Farmington Hills, Michigan.
LER is proud to partner with the American College of Podiatric Medicine to present clinically relevant peer-reviewed content, curated by Jarrod Shapiro, DPM, FACFAS, FACPM, FFPM RCPS (Glasg).
- van Dijk PA, Miller D, Calder J, et al. The ESSKA-AFAS international consensus statement on peroneal tendon pathologies. Knee Surg Sports Traumatol Arthrosc. 2018;26(10):3096-3107.
- Yammine K. The accessory peroneal (fibular) muscles: peroneus quartus and peroneus digiti quinti. A systematic review and meta-analysis. Surg Radiol Anat. 2015;37(6):617–627.
- Saupe N, Mengiardi B, Pfirrmann CW, Vienne P, Seifert B, Zanetti M. Anatomic variants associated with peroneal tendon disorders: MR imaging findings in volunteers with asymptomatic ankles. Radiology. 2007;242(2):509–517.
- Hyer CF, Dawson JM, Philbin TM, Berlet GC, Lee TH. The peroneal tubercle: description, classification, and relevance to peroneus longus tendon pathology. Foot Ankle Int. 2005;26(11):947–950.
- Sobel M, Pavlov H, Geppert MJ, Thompson FM, DiCarlo EF, Davis WH. Painful os peroneum syndrome: a spectrum of conditions responsible for plantar lateral foot pain. Foot Ankle Int. 1994;15(3):112–124.
- DiGiovanni BF, Fraga CJ, Cohen BE, et al. Associated injuries found in chronic lateral instability. Foot Ankle Int. 2000;21(10):809-815.
- Slater HK. Acute peroneal tendon tears. Foot Ankle Clin. 2007;12(4):659–674.
- Boffeli TJ, Collier RC. Surgical technique for combined Dwyer calcaneal osteotomy and peroneal tendon repair for correction of peroneal tendon pathology associated with cavus foot deformity. J Foot Ankle Surg. 2012;51(1):135–140.
- Helliwell TR, Tynan M, Hayward M, Klenerman L, Whitehouse G, Edwards RH. The pathology of the lower leg muscles in pure forefoot pes cavus. Acta Neuropathol. 1995;89(6):552–559.
- Ferran NA, Maffulli N, Oliva F. Management of recurrent subluxation of the peroneal tendons. Foot Ankle Clin. 2006;11(3):465-474.
- Squires N, Myerson MS, Gamba C. Surgical treatment of peroneal tendon tears. Foot Ankle Clin. 2007;12(4):675-695.
- Heckman DS, Reddy S, Pedowitz, D, Wapner KL, Parekh SG. Operative treatment for peroneal tendon disorders. J Bone Joint Surg Am. 2008;90(2):404-418.
- Selmani, E, Gjata V, Gjika E. Peroneal tendon disorders. Foot Ankle Int. 2006;27(3):221-228.
- Taljanovic S, Alcala JN, Gimber LH, Rieke JD, Chilvers MM, Latt LD. High-resolution US and MR imaging of peroneal tendon injuries. Radiographics. 2015;35(1):179-199.
- Kijowski R, De Smet A, Mukharjee R. Magnetic resonance imaging findings in patients with peroneal tendinopathy and peroneal tenosynovitis. Skeletal Radiol. 2007;36(2):105–114.
- Fram BR, Rogero R, Fuchs D, Shakked RJ, Raikin SM, Pedowitz DI. Clinical outcomes and complications of peroneal tendon sheath ultrasound corticosteroid injections. Foot Ankle Int. 2019;40(8):888-894.
- Dallaudière B, Pesquer L, Meyer P, et al. Intratendinous injection of platelet-rich plasma under US guidance to treat tendinopathy: a long-term pilot study. J Vasc Interv Radiol. 2014;25(5):717-723.
- Andia I, Latorre PM, Gomez MC, Burgos-Alonso N, Abate M, Maffulli N. Platelet-rich plasma in the conservative treatment of painful tendinopathy: a systematic review and meta-analysis of controlled studies. Br Med Bull. 2014;110(1):99-115.
- Mani-Babu S, Morrissey D, Waugh C, Screen H, Barton C. The effectiveness of extracorporeal shock wave therapy in lower limb tendinopathy: a systematic review. Am J Sports Med. 2015;43(3):752-761.










Hi, my 11 year old son has flexible planovalgus deformity bilaterally worst on the right. He was able to walk on toes and heels and had no contractures of gastrocnemius or Achillies tendon. He does not have cerebral palsy he just had long flat feet. He had surgery 3 yrs ago but will go back again because he ended up with a tight gastroc, his peroneus was lengthened, he got a lateral plantar injury and his osteotomy was not ideally placed. lots of things went wrong and he is still in planovalgus foot. Can I send you some medical notes regarding his condition. I would appreciate some independant advice. Thanks
Recovery from foot strain requires patience and awareness. A side foot sprain can linger if ignored, showing how important it is to respect foot pain and allow proper healing before returning to normal activity levels.