iStock #137417360
By Nicole Wetsman
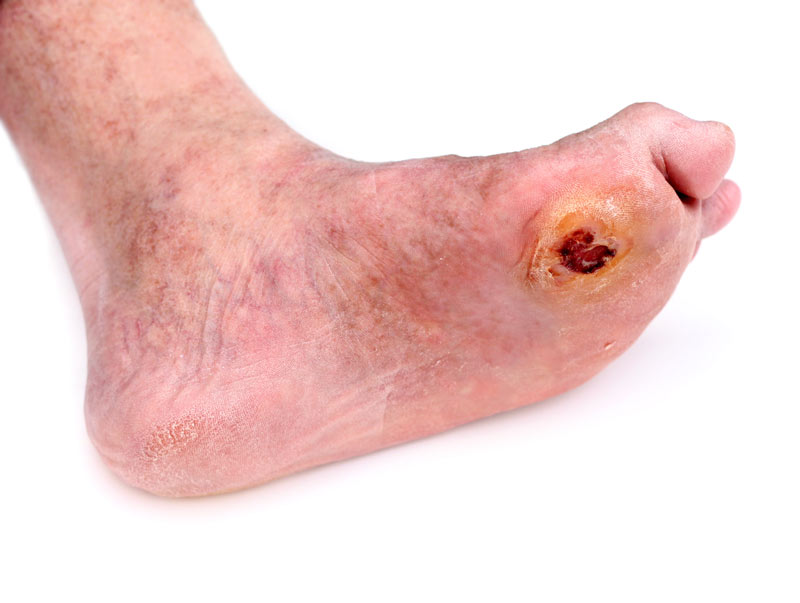
Spraying insulin into an open wound improves the healing of diabetic foot ulcers in diabetic patients—both type 1 and type 2, reported a poster entitled, The Outcomes of Local Flushing of Insulin on Wound Healing in Patients with Diabetic Foot Ulcers.1
Patients with diabetes have a 25 percent chance of developing a foot ulcer in their lifetime, and the disease is associated with impaired wound healing — which arises from a host of factors, including dysfunction in glucose metabolism, inflammatory responses, and repair cell activity. Animal studies have shown that topical insulin can facilitate wound healing: it speeds the growth of new tissue, improves the development of new blood vessels, and is involved in inflammatory processes important for healing.
“This is a new innovation in podiatry,” lead poster author and resident physician Azza Alalwee, DPM, MD, told Lower Extremity Review in a post-meeting interview. Prior studies have shown the effect of injected insulin on wound healing, both in diabetic and non-diabetic patients. However, the strategy of applying insulin topically had not previously been tested in humans.
In the study, 26 patients with diabetes foot ulcers of 8 weeks or more duration who were being seen at the New York Community Hospital wound clinic had topical insulin spray added as part of their treatment. After the wounds were debrided, they were sprayed with either 1 mL of insulin, if the wound was 5 centimeters or larger, or 0.5 milliliters of insulin, if the wound was smaller than 5 centimeters; after 3 to 5 minutes, the wound was dressed. Patients were treated twice a week in the clinic through the course of the wound management and did not receive any other medications or grafts for their wound.
The topical insulin spray led to improved wound healing and faster growth of tissue across the wound, the authors observed. Patients averaged 80 percent wound closure within 4 weeks, and 3 patients had complete wound closure within 4 weeks. There were no adverse effects from the insulin spray, Alalwee said, and patients were satisfied with the treatment. “We’ve had amazing results,” she said. “These are not easy wounds to deal with.”
The authors reported several other notable findings: From week 1 with the insulin spray, wound base granulation and epithelialization occurred at a faster rate than expected. They also saw a decreased rate of infection and a decrease in anticipated graft usage. The authors also reported that 14 of the 26 patients showed a marked decrease in the amount of exudate.
The most unusual finding the team noted was the improvement in patient’s fine touch sensation, leading to improved neuropathy gradation from 4/10 to 6-7/10.
The team is continuing to enroll patients from multiple clinics, and hopes to treat 100 patients with topical insulin in the next two years. Eight additional patients have entered the study on top of the initial 26 included in the poster presentation. Because the technique is new and experimental in humans, the team is not comparing results to a control group, Alalwee said, noting that the work is pilot research to ensure that the topical insulin works well and is safe. They plan to conduct a randomized controlled trial in the future.
Should topical insulin continue to prove to be effective, it could offer a cheap and easy-to-use method to promote healing in diabetic foot ulcers, which can significantly impair quality of life for patients with diabetes. “We want to provide something affordable, that any doctor can apply,”
Posters presented at American Podiatric Medical Association 2018 Annual Meeting
- Alalwee, A, Spergel, G, Santi, L et al. The Outcomes of Local Flushing of Insulin on Wound Healing in Patients with Diabetic Foot Ulcers.
- Moisan, G, Descarreaux, M, Cantin, V, et al. Effects of Two Types of Foot Orthoses on the Biomechanics of Participants with Cavus Feet During Walking.
- Schick, F, Taweel, N. A Non-surgical Approach to Arteriovenous Malformation of the Foot.
- Brock, K, Walters, J. Is the Operating Room Always Necessary? Office Based Toe Amputations for Osteomyelitis.
- Cole, W. Management of Small, Lower Extremity Wounds in the Ambulatory Setting Using a Disposable, Mechanically Powered Negative Pressure Wound Therapy System.