Taping is a mainstay of preventive foot blister management in athletes and active people. Its use is based on the premise that rubbing causes blisters, and that tape protects the skin from this rubbing and/or provides thermal insulation from the heat generated by rubbing. This commentary highlights research that casts doubt on these assumptions and discusses alternative mechanisms of action for preventive blister taping.
By Rebecca Rushton, Bsc(Pod)
Taping is one of the favoured modalities for preventing blisters in athletic and active patients. Runners, hikers, tennis players, golfers, and other athletes frequently use either rigid or flexible tape, for either treatment or prophylaxis. Taping is definitely the favoured preventative option at aid stations of running/walking events as well. At a guess, taping could make up 80%-90% of all preventative interventions for blisters.
But how does it work?
Effectiveness of Preventive Blister Taping?
Both Brennan1 in 2002 and Richie2 in 2010 state that the scientific evidence behind the use of adhesive tape for blister prevention is lacking. “Athletes, athletic trainers and other sports medicine specialists have anecdotally used these products with varying degrees of success.”1
Since then, Lipman et al have published two papers on the use of paper tape in ultramarathon runners. The first in 20143 found it to not be protective against blisters, while the second, in 2016,4 found it was protective against blisters.
Mechanism of Action?
While there is little evidence that taping prevents foot blisters, there is also little discussion about how taping might accomplish this.
Most dialogue in both medical and mainstream literature seems to assume that tape prevents blisters by protecting the skin from rubbing. But is rubbing on the skin required for blister development?
What Causes Blisters
Blisters form when shear stress exceeds the shear strength of the skin, resulting in a separation within the stratum spinosum of the epidermis. This was established 40-60 years ago with the work of Naylor,5 Sulzberger et al,6 Akers and Sulzberger7 and Comaish,8 among others. Consider this explanation of the mechanics of shear during gait from Richie:2
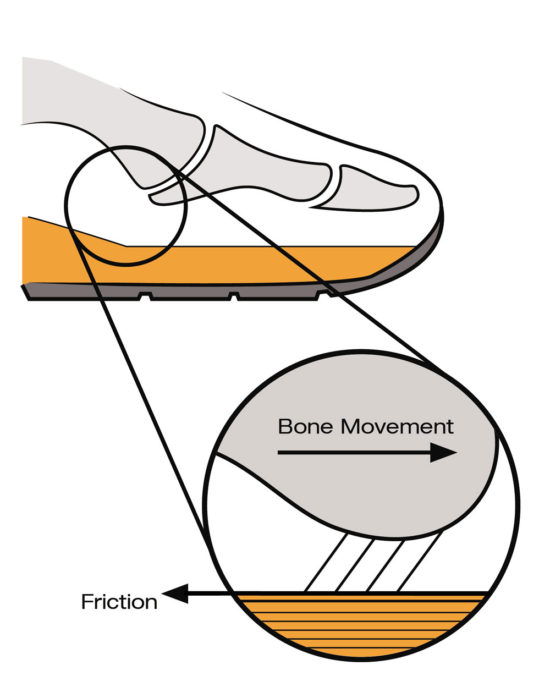
“Shear forces are applied to the human foot during walking and running because of the mechanics of foot alignment during contact and propulsion. The foot approaches the ground at a tangential angle (not a purely vertical angle) and then pushes off in a similar tangential direction. The foot [bones] must skid to a stop and then push into the ground to propel forward. The skidding will occur in both an anterior-posterior and medial-lateral direction, depending on the activity and demands of the sport.”
The force of friction acts in the opposite direction to bone movement (see Figure 1). It acts to keep the skin surface stationary (for longer than the bones). During gait, because internal tissue layers are structurally connected, soft tissues between skin and bone undergo shear distortion. During a shear distortion, these connected tissue layers move parallel to one another. If shear occurs to excess, it results in a “mechanical fatigue” within the layer of the stratum spinosum of the epidermis.5, 7-9 Presumably this is the layer of cells with the least resistance to shear. These microscopic tears are the initial blister injury. The higher the shear magnitude, the fewer repetitions required to cause a blister.5,6,8

Figure 2. Shear will peak in a state of static friction (no rubbing). A state of kinetic friction (rubbing) brings about reduced shear strain.
Rubbing Not Required
In spite of experimental blister studies using rubbing to produce blisters,5-8,10 and in spite of real-life blister situations often involving rubbing, skin surface rubbing is not necessary to produce skin damage such as blisters.3,11,12 In fact, shear distortions peak in a state of static friction – the state in which there is no relative motion between two surfaces. As soon as the transition to kinetic friction occurs (relative motion between two surfaces), shear distortions reduce, as seen in Figure 2. Veijgen et al found static friction coefficients to be 18% higher than dynamic friction coefficients.13 This phenomenon can easily be observed when pushing a heavy piece of furniture across the floor – the force required to get the furniture moving is much higher than that required to keep it moving.14
An easy demonstration of shear on the human body:
Step 1: The tip of the index finger is pressed against the back of the opposing hand.
Step 2: Wobbling the finger back and forth while keeping it in contact with the same patch of skin results in skin stretching. This is shear, and it is the true cause of blisters.
Shear might seem to involve rubbing, but it does not. Notice in the above demonstration that the fingertip has not moved relative to the skin of the back of the hand. But the skin on the back of the hand has moved relative to the underlying bone – it has undergone shear distortion. Blister causation is a “duck under water” scenario – below the surface is where the action is occurring! Blister causation is about stretching (shear), not rubbing.
Thankfully, the tissues of the feet can tolerate a high amount of shear. While blisters will only form when shear is excessive and repetitive, the blister-causing threshold will vary between individuals. This was evident in research by:
- Naylor in 1955 on 19 volunteer British medical students and doctors.5 He showed blistering occurred between 27 and 138 repetitions. The middle of the shin was used in this experiment.
- Sulzberger et al in 1966 conducted on 54 American army personnel.6 Some soldiers blistered in 3 minutes and others still had not blistered even after 50 minutes. The frictional force repetitions were applied to the palmar skin.
- Hashmi et al in 2013 on 30 volunteers at the University of Salford.10 They found that blister onset ranged from between 4 and 32 minutes. The frictional force repetitions were applied to the back of the heel.
How Might Taping Prevent Blisters?
Personal experience and research3 shows a blister can occur underneath the tape applied to prevent it. But divergent personal experience and research4 also shows taping can prevent blisters. This is why many practitioners use taping on patients.
With an understanding of what causes blisters, the following are four potential hypotheses for how preventive taping works:
- Thermal insulation
Rubbing any two surfaces together causes the production of heat, and it is no different for the skin.15-17 Assuming heat is a causative factor in blister formation, perhaps tape applied to the skin provides thermal insulation to lessen the effect of frictional heat. Although plausible, research to date does not support the theory that local surface heat generated by rubbing is a significant factor in blister formation, as explained below.
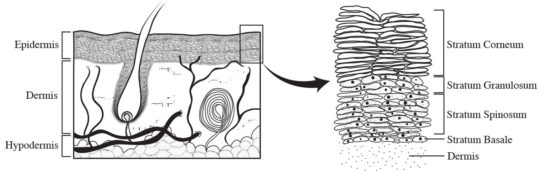
If heat transfer from the surface of the stratum corneum to the stratum spinosum (see Figure 3) were a major factor in blister development, one would expect faster rubbing to increase blister occurrence. Naylor found this not to be the case.5 In his experimental blister research, he compared blister rates at two rubbing speeds – the faster rubbing speed did not cause blisters to form any more quickly than the slower rubbing speed. Separately, he compared rubbing with 2 materials that differed in thermoconductivity. No difference in blistering rate was found.
Hashmi et al produced experimental blisters at the posterior heel of 30 subjects with an intermittent rubbing force.10 The median temperature increase at the blister site at the time of blister formation was 5.1°C (range: 1.7 – 9.9°C) and did not exceed 35°C.
Li et al demonstrated that rubbing causes a moderate increase in skin temperature, and that this warmer area of skin increases sweat production, which increases skin friction.17 This perspiration/friction mechanism
[rubbing heat → more perspiration → higher friction level → blister]
differs from the burn mechanism
[rubbing → heat → burn → blister]
and this distinction should be recognized. Besides, remembering that the initial blister injury is within the stratum spinosum of the epidermis, if heat transfer from the skin surface to the stratum spinosum were a major factor in blister development, one would expect the thicker stratum corneum of the plantar surface to afford a level of blister protection. The reality is, a thick corneum is one of the requisites for blister formation.5-7
Heat is not a requirement for blister formation. Although friction blisters on the feet are more common in warmer temperatures, blisters can occur in cold temperatures too.18,19 Griffin et al18 produced experimental blisters on chilled, warmed, and “normal” temperature skin and noted:
- blisters formed more quickly when initial skin temperature was higher
- blisters took longer to form on chilled skin (14°C) compared to normal (30°C ) and warmed skin (46°C )
- when the initial skin temperature was low, the skin temperature at the time of blistering was also lower.
Overall, Knape’s review summarizes it nicely: “Skin temperature appears to be a minor factor in blister formation. Blisters form somewhat more rapidly when the skin temperature is higher but blisters also occur when the skin temperature is low. In experimental rubbing studies, local heat is produced and skin temperatures have been reported between 41 degrees Celsius and 50 degrees Celsius. However, friction blisters do not resemble second-degree thermal burns either clinically or histologically.”20
- Protection from rubbing
By the admission of sports medicine practitioners and athletes alike, the most common understanding of how taping prevents blisters is “by protecting the skin from rubbing.” But as explained earlier, rubbing on the skin is not necessary to cause a blister, and blisters can occur under tape.3
What does rubbing do? It removes cells from the skin surface, exposing progressively deeper and deeper layers. This is not a blister. This is an abrasion.
So tape does not prevent blisters by stopping rubbing. Taping protects the skin from abrasion. But this is abrasion prevention, not blister prevention.
Consider another blister prevention strategy: that of lubricants. Lubricants facilitate rubbing of the sock against the skin to prevent blisters by way of reducing friction levels (more below).
- Reducing friction levels
In-shoe conditions result in high-friction levels. This is partly by design as materials are chosen to provide traction for the foot,2,11 and partly due to the high density of sweat glands and enclosed environment, because there is minimal evaporation of moisture when shod.21
It is plausible that tape reduces shear by lowering friction levels. By replacing the higher friction skin-sock interface with a lower friction tape-sock interface, earlier rubbing movement occurs between the two surfaces. This earlier state of dynamic friction means shear peak will be lower, potentially providing blister prevention.
Zhang and Mak articulate this idea well, stating: “The injurious effects of friction on the skin and the underlying tissues can be divided into two classes, those without slip and those with slip. The former may rupture the epidermis and occlude blood and interstitial fluid-flows by stretching or compressing the skin. The latter adds an abrasion to this damage.”22
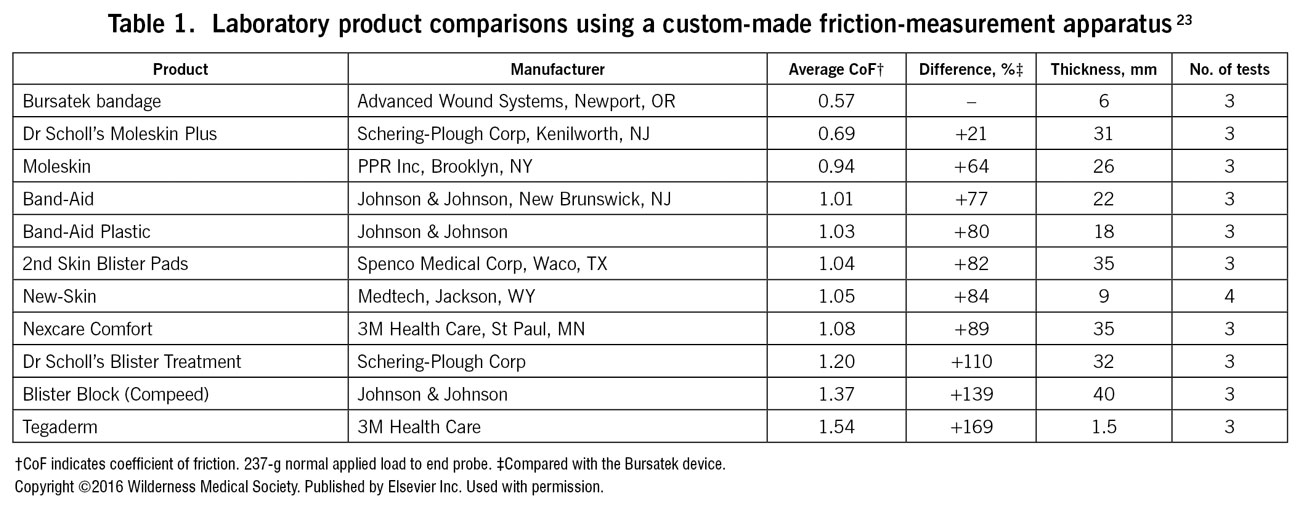
Understanding this, Polliack and Scheinberg gathered a number of blister dressings and tested their friction properties, observing coefficients of friction ranging from 0.57 to 1.54 (see Table).23
Other in-shoe coefficient of friction data can be found in Carlson,14 including insights into the effect of moisture.
Unfortunately, few of the adhesive tapes used for the prevention of blisters have had their friction properties tested in any research – only Moleskin from these charts. What’s more surprising is that we could find no coefficient of friction data available from the manufacturers for these tapes! Perhaps this is because most tapes used in blister prevention are not specifically made for blister prevention. This represents an area for improving our understanding of this modality’s mechanism of action.
- Spreading shear load
Cushioning spreads vertical load over a larger area to reduce peak pressure. Does tape spread the tangential shear load over a larger area of skin to reduce peak shear in a similar way?24
Could it be that without adhesive tape applied, shear peaks at a certain discrete location? And could it be that with adhesive tape applied to a wider area of skin, shear is dispersed over that wider area, reducing the peak? In other words, by spreading the shear load, shear per unit area of skin may be lessened. If this is the case, a stiffer tape would exert this effect better than a compliant tape.
Conclusion
For a modality that is arguably the most common blister prevention strategy used, it is odd that we know so little about how it works. Once a mechanism is established, more could be understood about which tapes are best in certain conditions and for certain anatomical regions. Specifics about application technique could also be identified. The mechanism of preventing blisters is an area that deserves much more research.
Rebecca Rushton, BSc(Pod), is a podiatrist in private practice at Esperance Podiatry in Perth, Australia. She is the owner of the foot blister website blisterprevention.com.au and BlisterPod, which sells blister products.
- Brennan FH. Managing blisters in competitive athletes. Curr Sports Med Rep. 2002;1(6):319-322.
- Richie D. How to manage friction blisters. Podiatry Today. 2010;23(6):42-48.
- Lipman G, Ellis M, Lewis E, et al. A Prospective Randomized Blister Prevention Trial Assessing Paper Tape in Endurance Distances (Pre-TAPED). Wilderness Environ Med. 2014;25(4):457-61.
- Lipman GS, Sharp LJ, Christensen M, et al. Paper Tape Prevents Foot Blisters: A Randomized Prevention Trial Assessing Paper Tape in Endurance Distances II (Pre-TAPED II). Clin J Sport Med. 2016 Sep;26(5):362-8.
- Naylor P. Experimental friction blisters. British J Dermatol. 1955;67:327–342.
- Sulzberger M, Cortese T, Fishman L, Wiley H. Studies on blisters produced by friction: I. Results of linear rubbing and twisting technics. J Invest Dermatol. 1966;47(5):456-465.
- Akers W, Sulzberger M. The Friction Blister. Mil Med. 1972;137:1-7.
- Comaish JS. Epidermal Fatigue as a Cause of Friction Blisters. Lancet. 1973;Jan:81-83.
- Cortese T, Griffin T, Layton L, Hutsell T; Experimental friction blisters in macaque monkeys. J Invest Dermatol. 1969;53(2):172-177.
- Hashmi F, Richards B, Forghany S, Hatton A, Nester C. The formation of friction blisters on the foot: the development of a laboratory-based blister creation model. Skin Res Technol. 2013;19(1)479-489.
- Carlson J. Functional limitations from pain caused by repetitive loading on the skin: A review and discussion for practitioners, with new data for limiting friction loads. J Prosthet Orthot. 2006;18(4):93-103.
- Carlson J. The mechanics of soft tissue damage: removing the “teeth” from the “rub”. The Academy TODAY. 2011;7.1 (Feb):A5-7.
- Veijgen N, Van der Heide E, Masen M. A multivariable model for predicting the frictional behaviour and hydration of the human skin. Skin Res Technol. 2013;19(3):330-338.
- Carlson J. The friction factor. OrthoKinetic Review 2001;1.7(Nov-Dec):1-3.
- Akers WA. Sulzberger on friction blistering. Internat J Dermatol. 1977;16:369-72.
- El-Shimi AF. In vivo skin friction measurements. J Soc Cosmetic Chemists 1977;28(Feb):37-51.
- Li W, Pang Q, Jiang Y, Zhai Z, Zhou Z. Study of physiological parameters and comfort sensations during friction contacts of the human skin. Tribological Letters. 2012;8:1-12.
- Griffin C, Cortese T, Layton L, Sulzberger M. Inverse time and temperature relationship in experimental friction blisters. J Invest Dermatol. 1969;52:384-401.
- Knapik J, Reynolds K, Staab J, Vogel JA, Jones B: Injuries associated with strenuous road marching. Mil Med. 1992;157:64–67.
- Knapik J, Reynolds K, Duplantis K, Jones B. Friction blisters – pathophysiology, prevention and treatment. Sports Med. 1995;20(3):136-147.
- Deng F, Gong T, Jin H, Du S. Research on factors influencing temperature and relative humidity inside of shoes. College of Resources and Environments, Shanxi University of Science and Technology. 2009. Available at https://www.aaqtic.org.ar/congresos/china2009/download/2-6/2-218.pdf. Accessed March 10, 2019.
- Zhang M, Mak A. In vivo friction properties of human skin. Prosthet Orthot Internat. 1999;23:135-141.
- Polliack A, Scheinberg S. A New Technology of Reducing Shear and Friction Forces on the Skin: Implications for Blister Care in the Wilderness Setting. Wilderness Environ Med. 2006;17:109-119.
- Carlson J, personal communication, 2013.









Trackbacks/Pingbacks