This chapter concerns the study of gait from an office setting, the understanding of what is considered normal, and the symptoms related to gait variations.
In my training, gait evaluation was a crucial part in assessing how the [orthotic device] worked in controlling excessive motion, correcting for a short leg, improving someone’s posture, but also in spotting all sorts of problems. These gait problems could be very obvious, like limping from pain, or more subtle, like a twist in the foot at propulsion from abnormal pronation (abductory twist).
I have had my share of patients over the years who stated my findings on gait evaluation led to the proper diagnosis of a neurological disease, or an arthritic hip, and many other problems, and then the proper treatment. Even though a thorough understanding of structural deviations is vital to our training as taught with Root Biomechanics, gait evaluation really became my key to unraveling why someone hurts and sometimes where they hurt. In gait evaluation, you should look for signs of excessive pronation or supination or both (called medial-lateral instability), signs of short leg syndrome, signs of poor shock absorption, signs of limping and tight muscles, signs of weak muscles or instabilities, and signs of obvious structural problems, like bow legs, knock knees, tibial varum, genu valgum, high arches, etc. You never waste anyone’s time doing gait evaluations, and no other profession seems to be doing it.
I have also had a patient tell me after 4 years of unsuccessful treatments elsewhere, that my gait evaluation was the only thing that unlocked the answer to their particular problem. I believe in gait evaluation and try to make sense of my biomechanical measurements and what I see in gait. If one third of patients with pes cavus pronate, one third stay near neutral, and the last one third supinate, I want to know why. The general rule is that all patients with pes cavus supinate. If you only take static measurements, and forget gait evaluation, you may miss the entire reason for the patient’s problem.
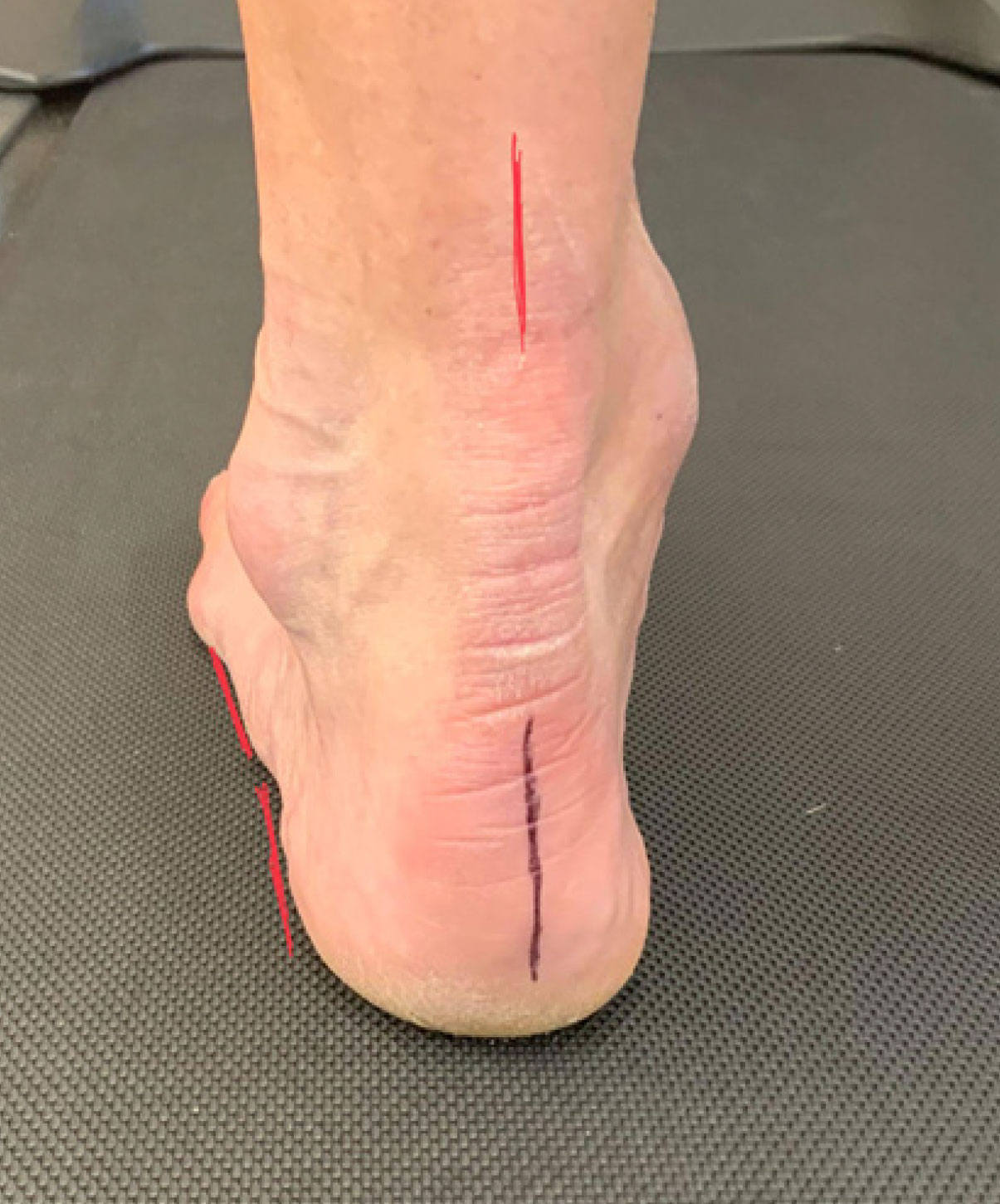
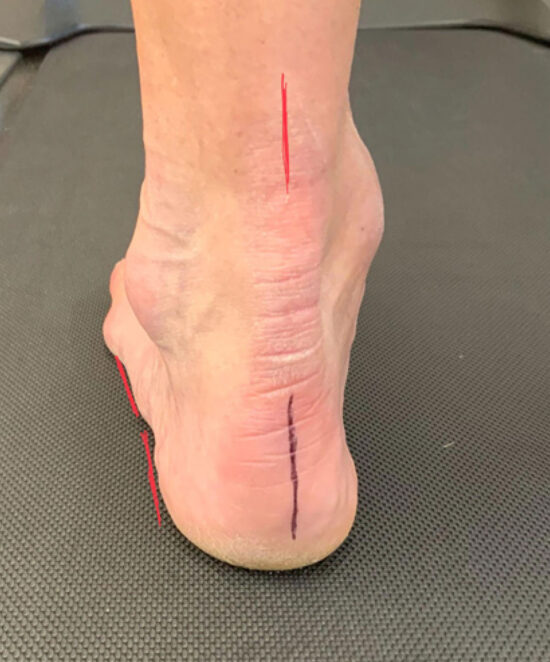
So, where do we begin? When you watch someone walk, even from a podiatrist’s standpoint, you want to start at the top. You need the patient in shorts, with their shirt tucked in, not looking down at their feet, and walking at a normal pace. I love to place a dot on the center of the knee cap and bisect both heels for easier observation. Hopefully, you can find a well lit hallway (all of these are ideals and most podiatrists will have to settle for less). You want them to walk 5 to 10 times up and down the longest hallway you can access so that they can get into a normal stride.
Typically, if they have orthotic devices, I watch them walk with shoes and their orthotic devices first, then shoes tied up tightly without their orthotic devices. I want to see the difference in gait with and without their present orthotic devices. Then I will watch them walk barefoot to check any differences from shoe walking. Some people are more stable with shoes than barefoot, and some the opposite. Sometimes the most stable environment is barefoot, with shoes second, and shoes with orthotic devices third (which should be the opposite of what you would have expected). You have to look and make observations. You are a scientist making observations.
You have to not use general rules, but here is where you begin to individualize for the patient in front of you. Gait evaluation can help slow the pace of your practice and allow great observations to help your patients. Some orthotic devices take a slight adjustment to make them more stable, and some need to be completely redone as an example. Some patients only need to learn power lacing, also called runner’s knot or stability lacing, to achieve more stability. Sometimes patients just come in with very poor shoes, and the proper evaluation of the function of orthotic devices will not occur until they purchase a better shoe.
I also like to have patients bring in 2-4 pairs of shoes at times, especially some with a lot of wear, so I can see how they break down their shoes. It can take several visits to get a good gait analysis done. They may not have appropriate shoes, like runners rushing from work and not having their actual running shoes. They may be in enough pain that gait evaluation has to be postponed. I also do not like to look at their orthotic devices (especially if I did not make them originally and recently) until I watch them walk or run with them. The best-looking inserts can function terribly, and the worst looking orthoses can function the best. If I make any adjustment for comfort, fit, or stability of an orthotic device, I want to watch the patient walk and/or run to decide if I achieved that goal. Always lean toward making someone more stable with inserts, unless there is nerve pain (from arch pressure) that you have to compromise by lowering the arch.
Biomechanics Question #80: What factors are not part of typical gait evaluation?
- Comparison of orthotic devices to no orthotic devices
- Looking at what environment the patient is the most stable
- Starting at the feet for clues of stability
- One walk down a long hallway should be enough
- Never watch a patient barefoot, since they are never barefoot in real life for more than a few seconds.
Richard Blake, DPM, MS, is adjunct faculty at the California School of Podiatric Medicine. He has practiced podiatry at the Sports and Orthopedic Institute of St. Francis Memorial Hospital in San Francisco, CA. His book, Practical Biomechanics for the Podiatrist, Book 1, is available from Amazon.com and Barnesandnoble.com, as well as from the publisher at bookbaby.com.