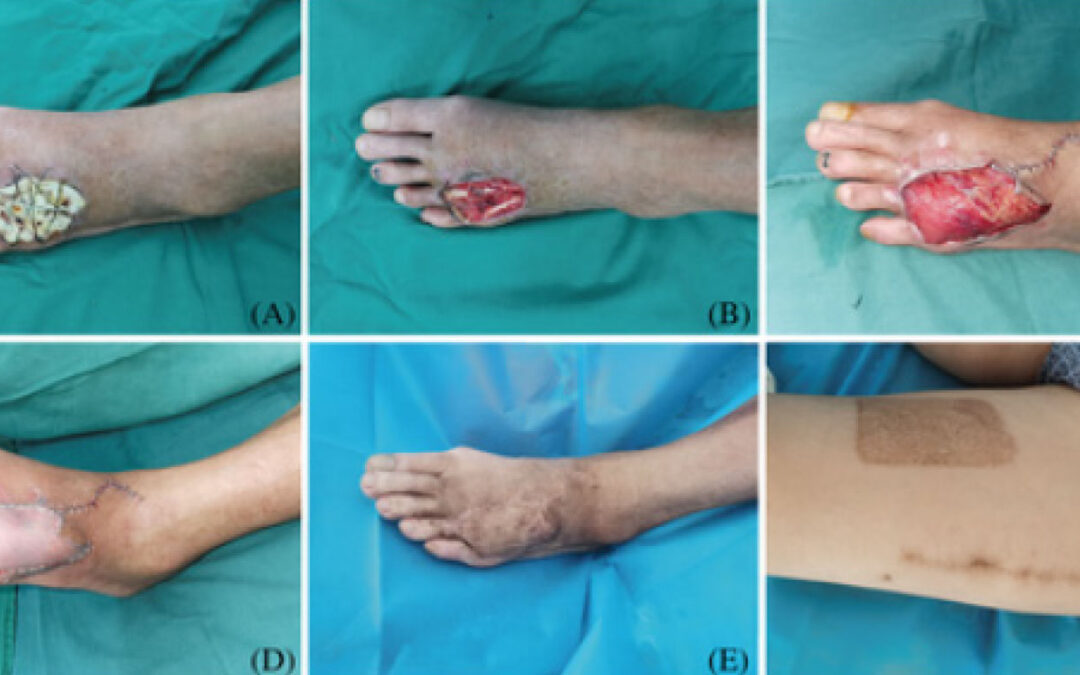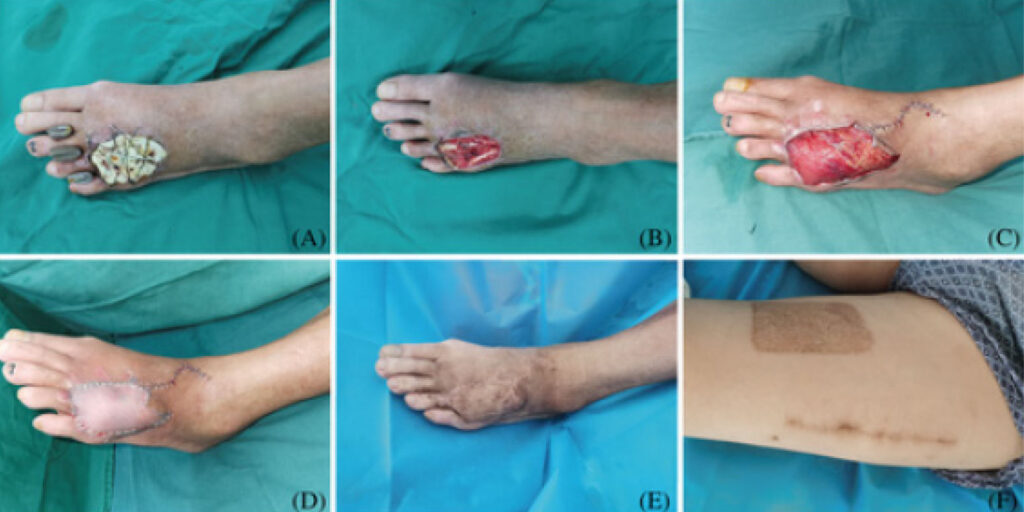
Case Study: A 54-year-old male had diabetes and dorsum DFU on the left foot. (A) After stage I debridement, the wound was covered with bone cement. (B) During stage II, after ALBC’s removal and tendon exposure, the formation of an ‘induction membrane’ could be seen. (C) A free VLMS flap was used to cover the wound. (D) The thigh STSG was used to cover the muscle. (E) At the 12-month postoperative follow-up, the flap showed a full and soft appearance. (F) The donor site scar was minor and easily concealed.
Diabetic foot ulcers (DFUs) present significant challenges due to associated amputation rates, mortality, treatment complexity and excessive costs. Earlier work by these authors introduced a wound surgical integrated treatment (WSIT) for DFUs, yielding promising outcomes. This study focuses on a specific WSIT protocol employing antibiotic-loaded bone cement (ALBC) in the first Stage, and free vastus lateralis muscle-sparing (VLMS) flaps and split-thickness skin grafts (STSGs) in the second stage to repair non-weight-bearing DFUs.
From July 2021 to July 2023, seven DFU patients (aged 47–71 years) underwent this treatment. Demographic data, hospital stay, and repair surgery times were collected. Histological and immunohistochemical analyses assessed angiogenesis, collagen deposition and inflammation. SF-36 questionnaire measured pre- and postoperative quality of life. Preoperative ultrasound Doppler showed that the peak blood flow velocity of the recipient area artery was significantly >30 cm/s (38.6 ± 6.8 cm/s) in all patients. Muscle flap sizes varied from 8 × 3.5 × 1 to 18 × 6 × 2 cm. The operation time of the repair surgery was 156.9 ± 15.08 minutes, and the hospital stay was 18.9 ± 3.3 days.
Histological analysis proved that covering DFUs with ALBC induced membrane formation and increased collagen deposition (CVF: preoperatively: 20.41 ± 5.78%; postoperatively: 41.10 ± 5.20%, P < 0.0001), neovascularization (CD31 blood vessels: preoperatively: 6.57 ± 2.44/HPF, postoperatively: 9.71 ± 2.56/HPF, P < 0.05), and M2 macrophages fraction (CD206+ cells: preoperatively: 9.43 ± 3.51/HPF, postoperatively:182.14 ± 44.54/HPF, P < 0.0001) while reducing M1 macrophages (iNOS+ cells: preoperatively: 24.29 ± 1.89/HPF, postoperatively: 7.14 ± 1.95/HPF, P < 0.0001). All grafts survived without amputation during a 7- to 24-month follow-up, during which SF-36 scores significantly improved.
The authors concluded that a combination of ALBC with free VLMS flaps and STSGs proved to be safe and effective for reconstructing non-weight-bearing DFUs. The protocol rapidly controlled infection, enhanced life quality and foot function, and reduced hospitalization time. They advocate integrating this strategy into DFU treatment plans.
Source: Chang S, Jian Y, Liu C, et al. Combining antibiotic-loaded bone cement-based free vastus lateralis muscle-sparing flap with split-thickness skin grafts: A reliable strategy for reconstructing diabetic foot ulcers at non-weight-bearing areas. Int Wound J. 2024;21(5):e14900. doi: 10.1111/iwj.14900.