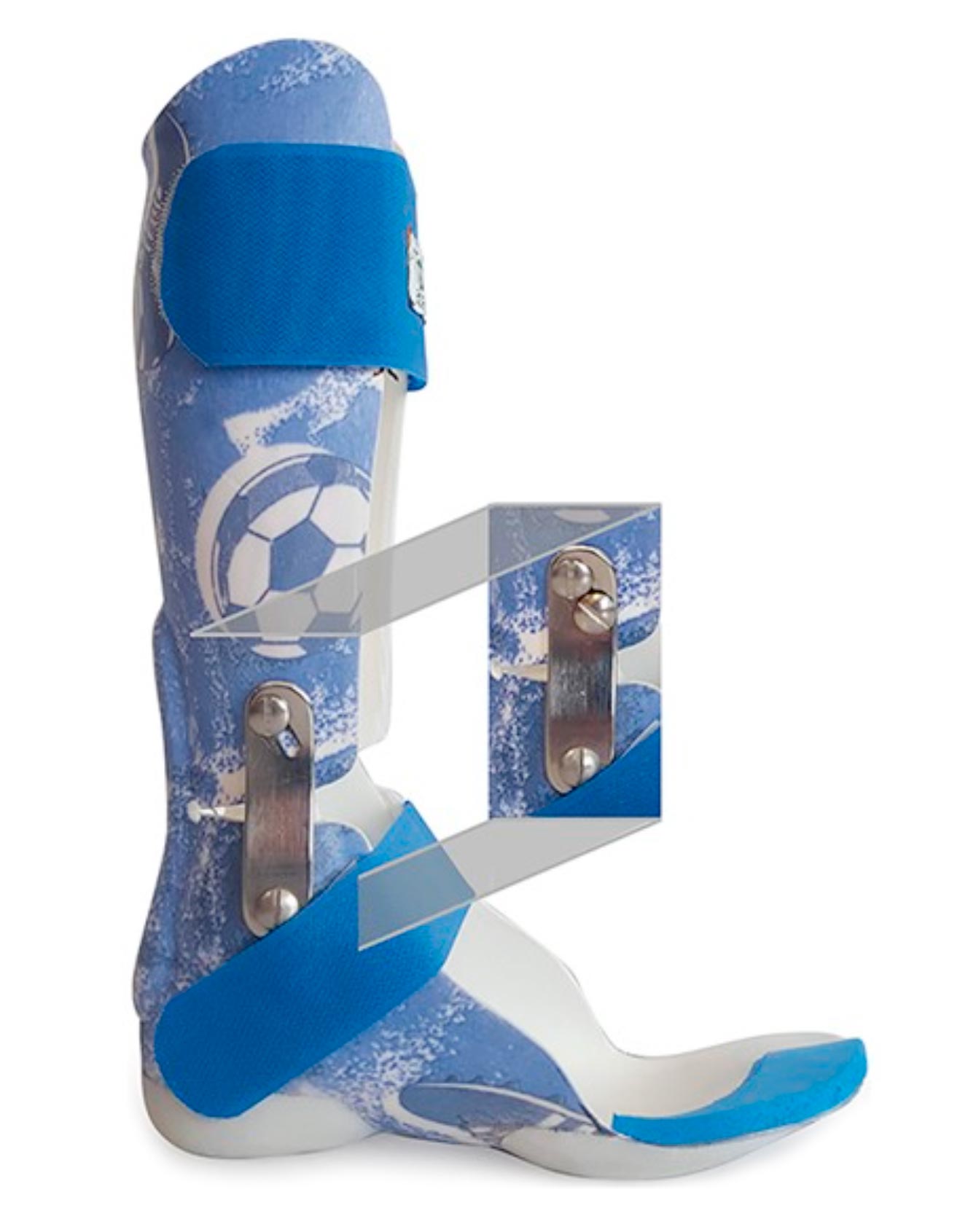
Figure. The ankle-foot orthosis used in the study showing the 2 configurations: hinged AFO, which is hinged at the ankle joint to allow limited dorsi-flexion (full image); the hinge can be clamped using the screw shown in the box to make it a solid AFO. Photo courtesy of ITOP SpA Officine Ortopediche, Palestrina (Rome), Italy, who supplied the orthosis for the study.
By Keith Loria
Cerebral Palsy (CP) represents the most common cause of motor disability in childhood with dysfunctional gait being one of the main problems.
Early adoption of intervention programs adapted to the patient’s functional limitation and disability represent the current standard of care; therapeutic approaches include Ankle-Foot Orthoses (AFOs) for which the evidence shows they influence spatio-temporal, kinematic, and kinetic gait parameters, improving coordination, and reducing walking energy cost.
Eugenio Di Stanislao, MS, with the I.T.O.P. SpA Officine Ortopediche in Rome, Italy, was part of a study designed to develop an instrumented assessment protocol based on the use of magneto-inertial measurement units (MIMU), which could provide clinicians with biomechanical parameters having a clinical relevance and supporting the selection of a patient-specific AFO configuration, improving the efficacy of the orthotic intervention on gait patterns.
In the study, “A wearable gait analysis protocol to support the choice of the appropriate ankle-foot orthosis: A comparative assessment in children with Cerebral Palsy,” which appeared in Clinical Biomechanics, 10 children diagnosed with diplegic CP were selected and an observational pre- and post-cross over design was adopted.
Eligibility criteria were: age from 3 to 12 years, functionally classified as Gross Motor Function Classification System I or II; no history of focal treatment with botulinum toxin A injection or orthopaedic surgery in the previous six months; and cognitively able to understand the given instructions. Observation took place in the Bambino Gesù Hospital in Rome.
“In a preliminary session, a clinical evaluation was performed, analyzing strength, muscle tone, possible joint contractures, autonomy, and stability during gait and postural passages,” Di Stanislao told LER via email. “The Observational Gait Scale was used for qualitative characterization of gait.”
Subsequently, participants were instrumentally evaluated in 3 different conditions 20 days apart, in which the subjects wore orthoses during daily activities: walking barefoot and while walking with 2 types of custom-made AFOs—a hinged AFO (hAFO) and a solid AFO (sAFO) (see Figure), which allowed the tibia to move forward over the weight-bearing foot during stance, introducing a slight spring-controlled ankle dorsi-plantarflexion.
“Specifically, for patients in crouch, only 5 plantar-flexion degrees were allowed; conversely for patients with genu recurvatum associated to a flat foot at initial contact, the hAFO allowed only 3 dorsi-flexion degrees,” Di Stanislao explained. “Both configurations were accommodated in the same off-the-shelf shoe model, characterized by the same heel height of 2 cm, extra-flexible, and shock-absorbing outsoles in microporous EVA, longer stiffeners and padded lining.”
The key findings of the study, he shared, highlight how different AFO configurations have varying levels of effectiveness dependent on the gait pattern of the lower extremity kinematic impairment and gait domain of interest. While no common trend appeared evident among the resulting differences, few individuals displayed significant improvements after sAFO prescription, others benefited more from the use of hAFO, whereas the remaining 5 patients had similar effects for both orthotic solutions.

iStockphoto.com #1158611911
Di Stanislao said the proposed assessment protocol can increase the clinical application and ecological validity of gait analysis, for the following reasons:
- biomechanical parameters are measured through the use of sensors (MIMUs)
- ease of protocol use
- rapidity of the evaluation
- overcoming of some laboratory setting limitations
- reduced equipment costs; and
- the protocol could easily be translated into a clinical orthotic practice thanks to its affordable and practical approach.
“The clinicians integrated their qualitative observation with the quantitative analysis deriving from the instrumental assessment, provided to them as pictorial feedback using the radar plots,” he said. “So, the proposed sensor-based assessment protocol represents a quantitative and useful tool to support patients’ assessment and selection of the most appropriate orthotic solution. Clinicians can use this integrated assessment in the decision-making process with the result of either supporting the initial decision or to reconsider the option for a different treatment.”
Keith Loria is a Washington, DC-based freelance writer.
Source: Contini BG, Bergamini E, Alvini M, et al. A wearable gait analysis protocol to support the choice of the appropriate ankle-foot orthosis: A comparative assessment in children with Cerebral Palsy. Clin Biomech. 2019;70:177-185.