By Shahram Attarian, Peter Young, Thomas H. Brannagan, and Colleagues
By Shahram Attarian, Peter Young, Thomas H. Brannagan, and Colleagues
Charcot–Marie–Tooth (CMT) disease is a group of rare, hereditary, chronic, and debilitating diseases of the peripheral nerves that result first in weakening and atrophy of the foot and leg muscles as well as the hand and arm muscles, then in distal sensory loss and, in some patients, limb deformity. Patients suffer from progressive reduced mobility and fine motor skills that impact quality of life. There is no cure; current disease management options are limited to symptomatic treatment, such as medications for pain and fatigue; the use of support measures, such as ankle/foot orthoses and arm crutches; and corrective surgery.
The most common form of the disease, Charcot–Marie–Tooth type 1A (CMT1A), originates in the duplication of the peripheral myelin protein (PMP22) gene located in chromosome 17p11.2, which results in overexpression of PMP22, a key component of the myelin sheath produced by Schwann cells. This overexpression leads to altered structure and dysfunction of the myelin sheath and causes demyelination, reduced motor nerve conduction velocities (< 38 m/s), and length-dependent axonal loss. Therefore, regulating PMP22 expression could be a plausible treatment for CMT1A. Past clinical trials of pharmacologic agents aimed at reducing PMP22 expression were unsuccessful: ascorbic acid did not improve patient condition, and the progesterone receptor antagonist onapristone was not safe in humans. However, a combination of baclofen, naltrexone, and D-sorbitol in low doses (PXT3003) could be effective as each agent interferes with PMP22 expression differently. Baclofen, a γ-aminobutyric acid (GABA)-B receptor agonist prescribed to relieve spasticity, acts via the cyclic adenosine monophosphate (cAMP)-dependent silencer element to negatively regulate PMP22 transcription in Schwann cells. Low doses (0.1 mg/kg) of naltrexone, an opioid antagonist used to treat opiate and alcohol dependence, raise endogenous endorphin release, increase cell surface targeting of cognate opioid receptors, and are expected to potentiate the adenylate cyclase-inhibiting effect of endogenous opioids on the level of PMP22 expression. D-Sorbitol, a carbohydrate alcohol used as a sweetener in the food industry and as a laxative, can bind with high affinity to muscarinic receptors that are involved in PMP22 expression, and possibly improve protein folding. Pre-clinical studies showed that PXT3003 limits PMP22 production, alleviates abnormal Schwann cell differentiation and improves neuromuscular function.
A subsequent phase 2 clinical trial involving 80 subjects with mild-to-moderate CMT1A investigated the efficacy and safety of 3 PXT3003 doses (highest baclofen/naltrexone/D-sorbitol daily dose [mg]: 6/0.7/210), demonstrating its safety and tolerability and provided preliminary evidence of efficacy for the highest dose. Because the efficacy of PXT3003 increased with dose, higher doses of PXT3003 were anticipated to have greater efficacy while maintaining a good safety profile.
Thus, a multi-center, randomized, double-blind, placebo-controlled phase 3 study was conducted exploring the efficacy and safety of 2 PXT3003 doses (baclofen/naltrexone/D-sorbitol [mg]: 6/0.70/210 and 3/0.35/105) administered twice daily compared to placebo in 323 subjects diagnosed with mild-to-moderate CMT1A. The results are reported here.
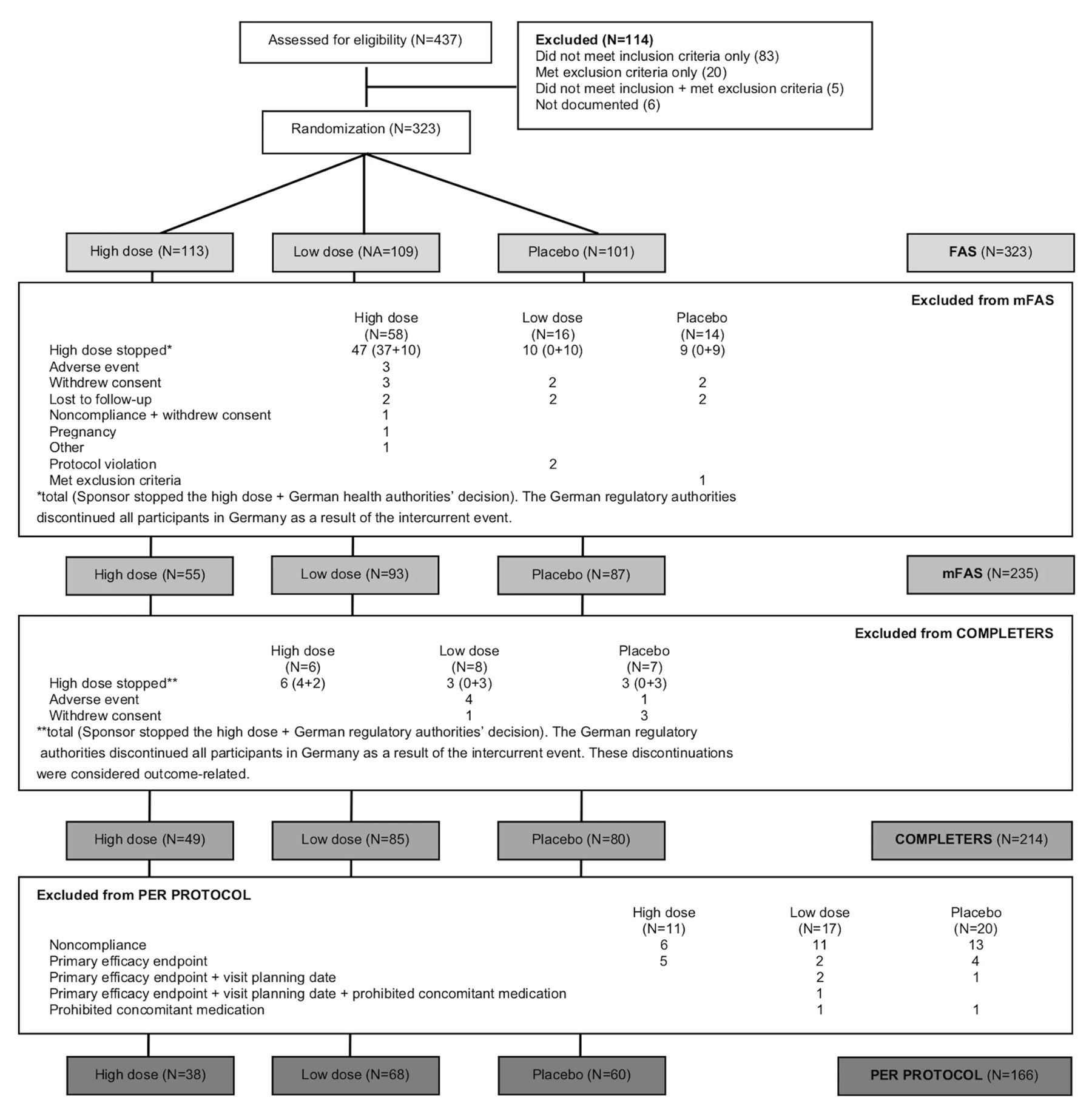
Figure 1: Subject disposition. The full analysis set (FAS) consisted of all randomized subjects. The modified FAS (mFAS) consisted of all randomized subjects except those who dropped out for reasons unrelated to outcome as judged by an independent adjudication committee. The completers population included all subjects who had at least a 12-month visit. The per protocol population consisted of all subjects who had no major protocol violation between randomization and at least the 12-month visit. N is the number of subjects in each group.
Methods
Eligible subjects were men or women, aged 16–65 years, with a genetically proven diagnosis of CMT1A of mild-to-moderate severity (i.e., a CMT Neuropathy Score version 2 [CMTNS-v2] score of 2–18), clinically confirmed muscle weakness in at least the foot dorsiflexors, and motor nerve conduction of at least 15 m/s in the ulnar nerve. Subjects diagnosed with any other type of concomitant peripheral neuropathy were excluded.
In this study, the full analysis set (FAS) comprised 323 subjects who were randomly assigned in a 1:1:1 ratio to receive 5mL of high- or low-dose PXT3003, or placebo, orally twice daily for up to 15 months. During the study, subjects were asked to attend up to 6 visits after the initial screening. Efficacy was assessed using the change in Overall Neuropathy Limitations Scale (ONLS) total score from baseline to months 12 and 15 (primary endpoint). Secondary endpoints included the 10-meter walk test (10MWT), the 9-hole peg test, quantified muscle testing (dorsiflexion and grip strength), and the EQ-5D-5L quality of life questionnaire, which included a visual analog scale ranging from “the best health you can imagine” to “the worst health you can imagine.” Safety was assessed at each treatment visit, including physical and neurological examinations, electrocardiography, clinical laboratory tests, vital signs measurements, and recording of adverse events.
The high-dose group was discontinued early due to unexpected crystal formation in the high-dose formulation. The statistical analysis plan was adapted to account for the large amount of missing data before database lock, and a modified full analysis set (mFAS) was used in the main analyses. Two sensitivity analyses were performed to check the interpretation based on the use of the mFAS.

Figure 2: Primary efficacy endpoint results. Mean change in Overall Neuropathy Limitations Scale (ONLS) total score in the modified full analysis set (mFAS, no imputation) high-dose PXT3003 (dark grey), low-dose PXT3003 (medium grey) and placebo (light grey) groups over the course of the study (panel A, error bars are standard error of the mean). The treatment effect vs placebo as measured by baseline-adjusted change with multiple imputation in ONLS score is shown in panel B for the primary analysis and the first sensitivity analysis (FAS: full analysis set). Panel C shows the second sensitivity analysis (LG: longitudinal model). The error bars in B and C are 97.5% confidence intervals. Axes are reversed to emphasize that lower ONLS scores indicate improvement.
Results
The mFAS consisted of 235 subjects. There were no notable differences between the mFAS and FAS in terms of baseline disease characteristics or demographics. However, the mean treatment duration was slightly reduced in the high-dose arm compared to the low-dose and placebo arms in the mFAS (398.9 ± 59.2 days vs 420.2 ± 86.8 and 418.9 ± 88.7 days, respectively) due to the discontinuation of the high-dose group (intercurrent event.)
Efficacy
From baseline to treatment end, the ONLS score decreased (indicating disability improvement) in both the high-dose and low-dose groups but increased (indicating disability worsening) in the placebo group (Fig. 2A). The change in ONLS score was greatest in the high-dose group (Fig. 2A), for which the mean effect was − 0.37 points (p = 0.008) (Fig. 2B). The mean effect of the low dose vs placebo was not statistically significant (p = 0.287). A responder analysis was performed on the completers population to assess the likelihood of a subject’s total ONLS score not deteriorating. The odds ratio for not deteriorating (improvers and non-decliners combined) was 3.39 (p = 0.026, 97.5% CI: [0.99, 11.62]) in the high-dose vs placebo and 1.26 (p = 0.569, 97.5% CI [0.50, 3.16]) in the low-dose vs placebo. Pre-specified analyses also showed a significant dose effect on the relationship between study drug dose and ONLS total score; an effect of − 0.17 points (p = 0.013, 95% CI [− 0.31, − 0.04]) was estimated per unit increase in dose.
Sensitivity analyses
The treatment effect was consistent between the primary and sensitivity analyses (Fig. 2B, C). The similarity between the mFAS and the FAS in the first sensitivity analysis shows that no particular bias was introduced from the use of the mFAS as the primary efficacy population. The per protocol population showed the greatest treatment effect. Notably, the second sensitivity analysis showed the smallest difference between the high-dose and low-dose groups. The second sensitivity analysis also estimated changes of − 0.16 (p = 0.006, 95% CI [− 0.27, − 0.05], FAS) and − 0.16 (p = 0.008, 95% CI [− 0.28, − 0.04], mFAS) in the ONLS total score per unit increase in drug dose, which was similar to the dose effect estimated in the primary analysis.
Safety and tolerability
There were no treatment-related serious adverse events. Treatment-emergent adverse events (TEAEs) were reported in a similar proportion of subjects across treatment groups, and most events were mild/moderate in severity. The most frequent TEAEs were related to the gastrointestinal and nervous systems (nausea, diarrhea, headache, and dizziness). No adverse events were reported in relation to the appearance of crystals in the high-dose formulation. There were no notable changes during the study in laboratory parameters and no notable differences were observed between the treatment groups. Treatment compliance was 90.5%, 94.4%, and 91.7% in the high-dose, low-dose, and placebo groups, respectively, indicating good tolerability.
Discussion
Outcomes: Although the intercurrent event reduced the statistical power of the study, the high-dose PXT3003 group demonstrated statistically significant improvements in ONLS scores (primary endpoint) and 10MWT compared to placebo. The treatment effect of the low-dose group was not statistically significant. Because the ONLS is based on functional motor tasks, stabilization of the ONLS score would be expected to be beneficial in a chronic progressive disease. Therefore, even though the choice of a 0.3-point change in ONLS score was prespecified as the anticipated treatment effect based on observations from the phase 2 study and for statistical reasons rather than established clinical evidence, the statistically significant and measurable change in ONLS scores between the high-dose and placebo groups is promising.
The efficacy demonstrated in the primary analysis was supported by the longitudinal model used in the second sensitivity analysis. The second sensitivity analysis showed the smallest difference between the high-dose and low-dose groups and estimated a change of − 0.31 points per year (p = 0.013) in the high-dose group, which suggests that PXT3003 may have a promising long-term treatment effect. However, long-term data are needed to assess the safety and efficacy of PXT3003 on timescales comparable with the slow disease progression. Such data is being obtained from an open-label continuation study (ClinicalTrials.gov identifier: NCT03023540).
The secondary endpoints all showed improvement in the point estimates in the PXT3003 groups compared to placebo, but improvement was only statistically significant in the 10MWT. The lack of statistical significance was probably strongly influenced by an inability to detect an effect as the study was underpowered due to the unexpectedly high discontinuation rate. In fact, the detection of any statistically significant changes in secondary endpoints was unexpected. However, because CMT1A tends to affect legs and feet more and earlier than hands and arms, given that the statistically significant secondary endpoint was the 10MWT was not surprising. The improvement in the 10MWT was consistent with improvement in the ONLS leg score (exploratory endpoint) and suggests that subjects taking high-dose PXT3003 experienced improved mobility due to treatment.
Both PXT3003 doses demonstrated an acceptable safety profile. Considering the higher efficacy and similar safety profile of high-dose PXT3003 compared to low-dose PXT3003, high-dose PXT3003 has a better risk/benefit ratio than low-dose PXT3003. The safety profile of the high dose will be better understood when data from the open-label continuation study becomes available.
Drawbacks and limitations: The intercurrent event, which led to a smaller sample size, caused the statistical power of the study to drop from the expected 90% to 75% for the primary endpoint. It is noteworthy that the high-dose group, which had the most discontinuations, showed the greatest treatment effect.
Also due to the reduced sample size, the study had limited power to detect statistically significant changes in many of the secondary and exploratory endpoints.
The formation of crystals in the high-dose formulation was a result of precipitation of some of the active ingredients, which did not result in any degradation products but did lead to a slight decrease in potency. A double volume of the low-dose formulation: i.e., 10mL low-dose PXT3003, is being used in the open-label continuation study and will be investigated in a confirmatory phase 3 clinical trial.
Conclusions
Subjects receiving PXT3003 demonstrated stabilization of disease progression by showing improvement or no change in ONLS scores, and this positive result is further validated by the improvement observed in the 10MWT. The treatment benefit observed over the limited duration of a clinical trial should be evaluated within the context of the known and well-characterized progression of CMT1A. In other words, if PXT3003 delivers a sustained therapeutic effect over a longer treatment period and achieves disease stabilization by modifying its chronically progressive course, PXT3003 may address a current unmet need in CMT1A treatment.
This article has been excepted from “A double-blind, placebo-controlled, randomized trial of PXT3003 for the treatment of Charcot-Marie-Tooth type 1A,” by Attarian S, Young P, Brannagan TH, Adams D, et al., which was published online October 16, 2021, in the journal Orphanet Journal of Rare Diseases.
PMID: 34656144 PMCID: PMC8520617 DOI: 10.1186/s13023-021-02040-8. Editing has occurred, including the renumbering of figures, and references have been removed. Use is per CC BY 4.0.