By Windy Cole, DPM, CWSP
With increasing demand for biomaterials that have the ability to support wound healing, tissue engineers have been challenged to develop innovative bioactive scaffold materials. In general, bioactive materials have the mechanical properties of the tissue to be replaced while supporting biological activities such as cellular adhesion, proliferation, differentiation, and angiogenesis. Ideally, tissue scaffolds should be biocompatible, non-toxic, have similar porosity to the tissue to be replaced, be degradable, resorb at the same rate as new tissue is produced, be excretable, and be sterilized for clinical use.1
Borate bioactive glass (BBG) is one such material gaining favor in the wound care space. Research has shown that BBG has demonstrated the ability to assist in cellular chemotaxis, proliferation, and differentiation in vivo.2 BBG has distinctive properties that can support repair and regeneration of soft tissue defects. When implanted, BBG forms a direct bond to living tissues.3 The specific architecture of the BBG scaffold contributes to the material degradation rate while the pore structure provides the support for cellular ingrowth and new tissue formation.1
Herein the author details 3 patient case reports in which BBG in the form of MIRRAGEN® Advanced Wound Matrix was used to treat chronic hard-to-heal wounds of varying etiology. In all cases, wounds were treated with standard of care which included cleansing wounds with normal sterile saline, debridement to appropriate level to remove devitalized tissues, application of MIRRAGEN wound matrix, and application of a secondary dressing to ensure a moist healing environment. Patients were monitored weekly. Wound assessments including wound measurements were obtained. Normal saline solution irrigation was used to flush away any loose MIRRAGEN still present in the wound base. Reapplication of MIRRAGEN was performed weekly until evidence of wound closure was noted.
Case 1
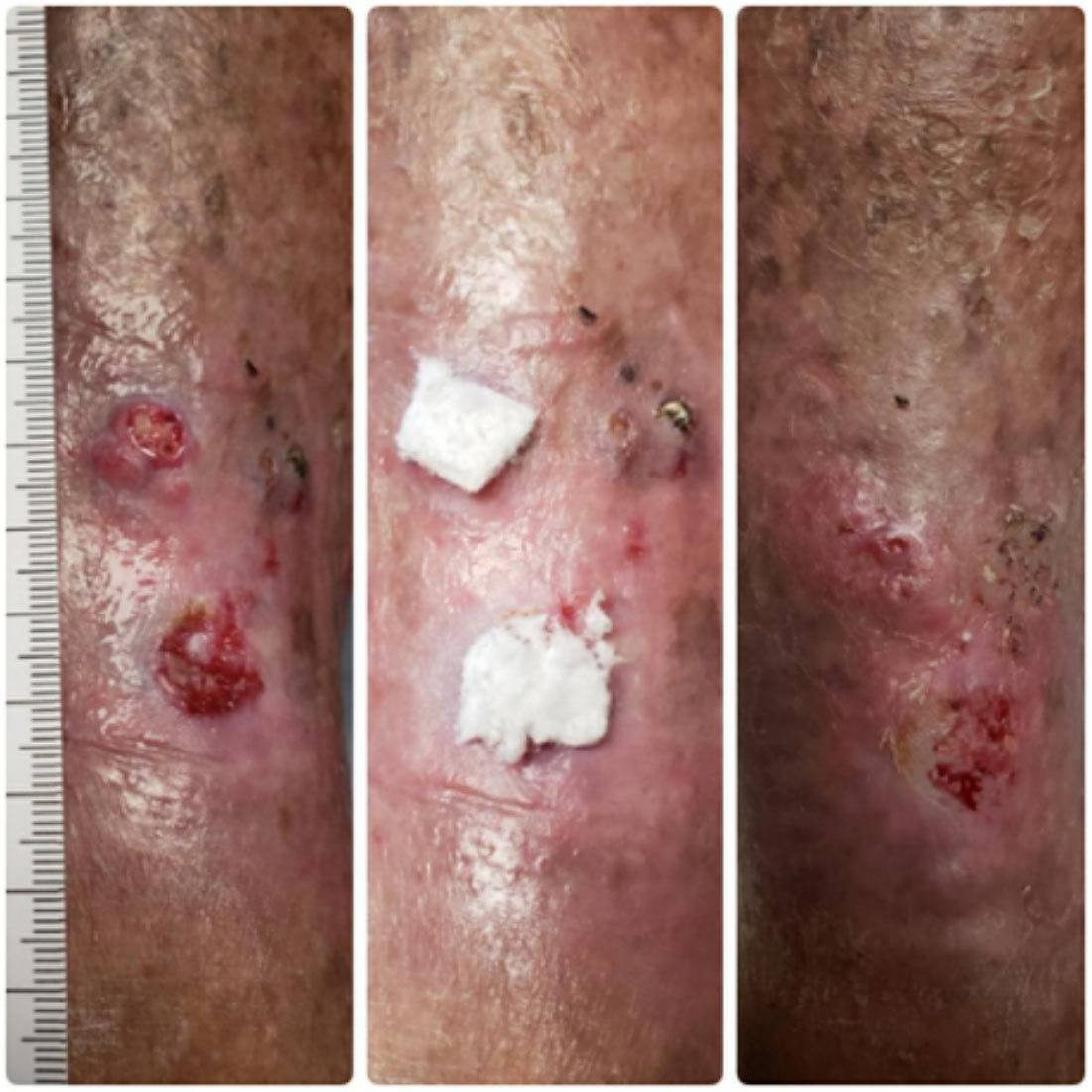
Case 1 (see image, above) is a 78-year-old male who presents to the wound care center with a long-standing history of chronic ulcers of the right lower leg. Patient relates that he has suffered from various areas of ulceration on the leg for several years. He states that the wounds crust over and then breakdown again. These particular open wounds have been present for 6 months. He has tried and failed numerous wound care therapies including collagen, alginates, and hydrogels. His past medical history includes hypertension, degenerative join disease (DJD), psoriasis, atrial fibrillation (A-fib), anxiety, restless leg syndrome, and sleep apnea. Upon physical exam it is noted that the proximal wound measures 0.7cm x 0.5cm x 0.1cm and the distal wound measures 1.2cm x 1.1cm x 0.1cm. The wounds are granular and clean without clinical evidence of infection. Moderate serous exudate was noted on the previous bandage, but no active drainage is noted at the time of examination. No erythema or malodor is present. Ankle Brachial Index (ABI) is 1.02. At the initial visit, MIRRAGEN was placed in the base of both wounds and covered with foam and a multilayer compression bandage. The patient was directed to keep the bandage dry and intact and reappoint for weekly wound assessment visits. Patient complied with the treatment regimen without any issues or complaints. Both wounds went on to complete healing with 3 weekly MIRRAGEN applications.
Case 2
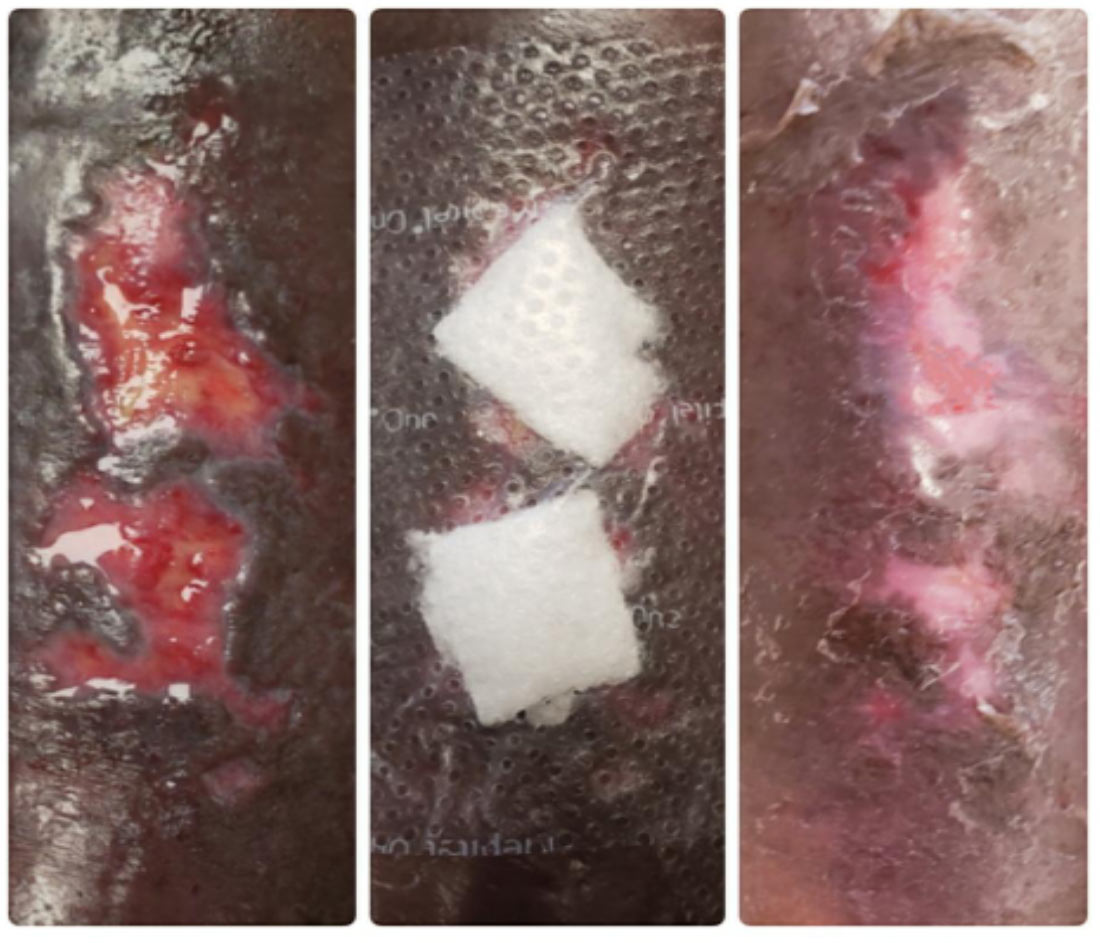
Case 2 (see image, right) is a 68-year-old female who presented to the wound center with a 6-week history of a right lower leg wound. It originally began as a small blister that opened and drained a bloody discharge. The area has continued to enlarge, and the patient made an appointment at the wound care center for this issue. Past medical history is positive for varicose veins, peripheral vascular disease, DJD, COPD, pulmonary hypertension, aortic stenosis, and obesity. Upon initial presentation, the wound measured 0.5cm x 0.7cm x 0.6cm. ABI was 1.14 on the right leg. At her first wound care visit, the wound was packed with alginate ribbon and a multi-layer compression wrap was applied to the leg. Patient presented for follow up the next week. Wound measurements had not progressed. It was then decided that we would discontinue the alginate and begin treatment with MIRRAGEN. After debridement, the wound base was packed with MIRRAGEN, covered with foam and a multi-layer compression bandage. She was compliant with the wound care regimen without issues or complaints. Weekly wound assessments were performed. The wound completely healed with 2 weekly MIRRAGEN applications.
Case 3
Case 3 (see image, page 29) is a 62-year-old female who presented to the wound center with a 4-week history of a right lower leg ulcer. She relates that she has been applying Neosporin to the area daily. She relates that the wound is heavily draining and painful. Past medical history includes type 2 diabetes and Rheumatoid arthritis. Upon intake the wound measures 8.1cm x 2.2cm x 0.1cm. The wound base is clean and granular. Moderate serous exudate present. No clinical signs and symptoms of wound infection noted. We began weekly MIRRAGEN application under multi-layer compression bandaging. Patient was compliant with the wound care regimen. No adverse events were reported. The wound completely resolved after 4 weekly applications.
Discussion
MIRRAGEN Advanced Wound Matrix is a resorbable and biocompatible borate-based bioactive glass specifically designed for wound healing.4 The BBG material slowly dissolves upon exposure to body fluid. As the borate glass dissolves, it releases regenerative ions at the wound site.4 The fibrous structure of MIRRAGEN Advanced Wound Matrix was specifically engineered to absorb fluid from the wound bed.4 The product can absorb 400% of its weight in exudate, making it ideal for use in heavily exudating venous leg ulcers. In this case series, application was performed weekly without evidence of secondary dressing saturation or peri-wound tissue maceration. The spacing of the fibers within the matrix creates a pore network similar to dermal tissue, facilitating accelerated cellular ingrowth and angiogenesis. Additionally, room temperature storage and long shelf life allowed the product to be easily stocked in the wound clinic. MIRRAGEN Advanced Wound Matrix proved to be an effective treatment in this case series of hard-to-heal chronic wounds.
Windy Cole, DPM, CWSP, serves as Adjunct Professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine and Student Rotation Coordinator, UH Richmond Medical Wound Center both in Cleveland, Ohio. She is a dedicated healthcare advocate with interests focused on medical education, diabetic foot care, wound care, limb salvage, clinical research and humanitarian efforts. Dr. Cole has published extensively on these topics and is a sought-after speaker both nationally and internationally. Dr. Cole also serves as a member of the Editorial Advisory Board for LER.
- Rahaman MN, Day DE, Bal BS, et al. Bioactive glass in tissue engineering. Acta Biomater. 2011;7(6):2355-73.
- Thyparambil NJ, Gutgesell LC, Bromet BA, et al. Bioactive borate glass triggers phenotypic changes in adipose stem cells. J Mater Sci Med. 2020;31(4):35.
- Balasubramanian P, Buttner T, Miguez Pacheco V, Boccaccini AR. Boron-containing bioactive glasses in bone and soft tissue engineering. J Eur Ceramic Soc. 2018;38(3):855-869
- ETS Wound Care. MIRRAGEN Advanced Wound Matrix. Available at https://www.etswoundcare.com. Last updated 2019.