By Rachelle Bordlee, sDPT, and Christopher Kevin Wong, PT, PhD
By Rachelle Bordlee, sDPT, and Christopher Kevin Wong, PT, PhD
With evidence-based protocols in hand, practitioners can feel more comfortable clinically integrating surface electromyography (sEMG) assessment, creating more sophisticated sEMG treatment protocols, and demonstrating the effectiveness of interventions.
Muscle weakness, timing of muscle activation, and proprioception are driving factors in many physiological dysfunctions involving the lower extremities. Researchers are beginning to identify the best exercises for patients to target these muscles with the assistance of surface electromyography (sEMG), which measures the electrical output of muscles noninvasively using sensors on the skin.1 This technology can be further incorporated in the clinic in the form of real-time biofeedback devices that visually or audibly alert patients when they are properly recruiting their forgotten musculature, thus facilitating proprioceptive and neuromuscular reeducation.
sEMG technology visually displays the magnitude of the effort of target muscle contraction to patients and clinicians in real time, often with video overlay and slow-motion replay to further pinpoint the biomechanics associated with the muscle activation. For years, owning a sEMG system was impractical for many clinics because of the numerous wires, long setup time, and complex software required. Now, thanks to the digital revolution, the technology is maturing rapidly, and there is an emergence of wireless sensors that allow free movement and streamlined software for easy setup and interpretation.
Today, the bulk of research into biofeedback uses wired sEMG systems. Visual and audio biofeedback from wired sEMG units have been shown to be effective augmentation therapies in the treatment of many lower limb dysfunctions. A 19-trial systematic review2 evaluated studies of poststroke patients who were outfitted with sEMG sensors that gave either audio or visual biofeedback of each patient’s lower limb muscular activation during gait training. Individuals using sEMG units achieved significantly greater improvements in gait speed, step length, and cycle time than those undergoing only usual or placebo therapy. One to five months after interventions ended, patients who underwent sEMG still had greater improvements in lower limb activities than patients who had received usual or placebo therapy.2
Individual trials have also shown statistically significant improvements in patient rehabilitation outcomes when usual care is combined with sEMG biofeedback, including increases in gluteus maximus activation and gait parameters in patients after incomplete spinal cord injury;3 decreases in days using an assistive device for ambulation after partial meniscectomy;4 increases in tibialis anterior activation and gastrocnemius relaxation during ambulation in children with cerebral palsy;5,6 increases in targeted muscular activation for healthy subjects with knee extension exercises;7 and improvements in vastus medialis/vastus lateralis ratios during walking and stair negotiation in patients with patellofemoral pain syndrome.8
Standardized protocol
Widespread implementation of sEMG as a biofeedback therapy has been slow because protocol standardization is lacking. Most systematic reviews of studies involving patients with biomechanical diagnoses are unable to pool data for interpretation because the vast majority of studies do not adhere to a consistent standard of sensor placement on the muscles.9,10
The number-one reason for inconsistencies in sEMG data is variability in placement of sensors along the muscles,11 as each brand of sEMG system comes with a different how-to manual, and the placements of sensors are often nonspecific or nonvalidated. This can affect the consistency of measurements for a given patient at different time points, as well as when comparing patients with controls. However, there do exist evidence-based standards for sensor placement and setup, and these must be integrated into research and clinician protocols. With evidence-based protocols on hand, practitioners can feel more comfortable clinically integrating sEMG assessment, creating more sophisticated sEMG treatment protocols, and demonstrating the effectiveness of interventions to justify reimbursement.12
The most validated recommendations come from Surface ElectroMyoGraphy for the Non-Invasive Assessment of Muscles (SENIAM), a project contracted by the EU to standardize sEMG placement for practice and research.13,14 Starting postures, sensor placement, and clinical testing has been streamlined into a series of well-organized charts.13 The SENIAM clinical recommendations, however, do not detail the specifics of clinician palpation and force required for accuracy.
To optimize accuracy, the clinician must alter the gain to read the minimum and maximum levels of activation associated with clinical significance before the computational system measures sEMG inputs. The clinician must therefore perform two tests for calibration—one test of minimal muscle activity, and one test of maximal muscle and agonist recruitment. Muscolino’s palpation manual15 offers a guide to eliciting minimal yet accurate muscle recruitment, which may serve as the sEMG’s low parameter activity. Slight activation of the targeted muscle should be recorded into the sEMG system first for calibration of the lowest electrical outputs, which can sense the finer details of the patient’s muscular coordination. Large resistance to the targeted action, which recruits the muscle and its agonists, should be recorded second to calibrate the largest parameter and represent the patient’s gross motor activity.
A how-to guide to sEMG use
This how-to guide combines recommendations for sEMG setup from SENIAM8 and for clinical muscle testing from Muscolino.15
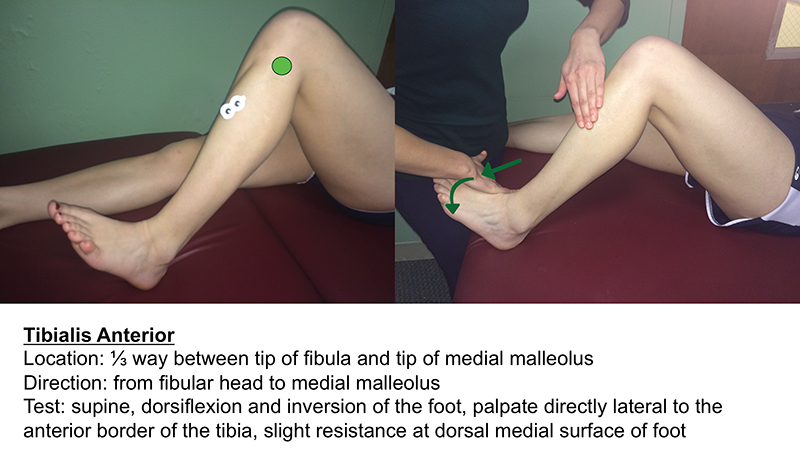
SENIAM provides recommendations for 13 muscles in the lower limb: the gluteus maximus, gluteus medius, tensor fascia latae, rectus femoris, vastus lateralis, vastus medialis, biceps femoris, semitendinosus, tibialis anterior, peroneus longus, peroneus brevis, soleus, and gastrocnemius (separate medial and lateral portions). Here, these recommendations have been paired with those of Muscolino for muscle testing. The figures on this page and the next two pages are visual adaptations of the 14 validated lower limb recordings.
Preparing the skin. The surface electrodes best pick up electrical signals through a clean barrier. For optimal recordings, shave the skin beneath the electrodes, clean the skin with an alcohol wipe, and allow the alcohol to vaporize before the electrode is applied.
Bipolar electrodes. Electrodes are organized into bipolar pairings to pick up electrical signaling from active muscle fibers. Any electricity that passes between the two electrodes is calculated and analyzed with the sEMG software for time and magnitude of electrical activity. Most bipolar electrodes come preprepared and secured to a plastic sheet, so the distance between positive and negative electrodes is reproducibly standardized for precision of calculation.
Securing the sensors. Bipolar sensors must be placed parallel to the muscle fibers below. Knowledge of anatomy and changes in muscle fiber orientation are crucial for accurate orientation. If the sensors are not sticky enough to remain connected throughout the patient’s movements once they are placed, they must be secured to the skin. Athletic tape for added security is recommended, but must not give additional pressure on top of the sensors as the patient’s movements put tension on the tape, and this may report false increases in electrical activity. Taping over the plastic that connects the bipolar sensors together often produces good results. If the sEMG system uses wires, secure them against the body to prevent pulls on the sensors, but make sure that the wires are not placed in a way that alters the patient’s movement patterns.
Reference electrode. The reference electrode is necessary to filter out excess electrical noise. This electrode should be placed over a superficial bony landmark, such as the malleoli, lateral epicondyle, or anterior superior iliac spine. These landmarks are considered the most electrically inactive tissue, as the sensor receives electricity only through the skin and subcutaneous tissues before the superficial bone tissue dulls transmission of the electrical signal. Any electric activity picked up by an electrode at this site will be filtered out of the muscular recordings as “noise” to help better detect muscular activation signals.
Calibration and muscle testing. Once the electrodes are secured, it is important to test each muscle so that the parameters of electrical activity can be individually calibrated using the analysis software. Each muscle’s electrical activity sums to different magnitudes, so each coupling of bipolar electrodes should be calibrated to its specific muscle. Ideally, the examiner should test the muscle at both trace levels of activity and maximum activity. Trace activity isolates the muscle as much as physiologically possible to ensure that the electrode is over the correct muscle to be tested and that fine motor adjustments are recorded. Maximum activity reads the target muscle and activity from the surrounding muscles, and is often more representative of functional activity. If this summed electrical activity is very large, an incorrectly calibrated window could be too small, meaning that the upper magnitude of activity would not be recorded. Adjust the gain to ensure the computer system has a sufficiently large window to record both trace and maximum activity.
Technical and clinical limitations
It is important to understand that sEMG does not represent strength; instead, it represents an estimate of an increase in motor unit recruitment and firing rate. However, “strength” is a result of both neural
activation and muscle size.16 When a patient first begins strength training, the first few weeks of strength gain are generally due to increased neuromuscular recruitment. Skeletal muscles have a threshold for increases in neural adaptation, but additional increases in strength can still be gained through muscular hypertrophy.16 Beyond the neural plasticity stages, changes in sEMG activity may not correlate with increases in strength.
sEMG is a raw measure of electrical activity that can be filtered by computational settings. It can be used to compare data on the same day, for the same muscle, or between trials. However, because it indirectly measures from the surface rather than from within the muscle, recordings can be polluted.12 The surface sensors will pick up any electrical recording, which might include not just the target muscle, but also agonists and possible antagonists if those signals reach the surface electrode.12
sEMG is also affected by the electrical conductivity of the skin and all tissue between the skin and the muscle (eg, subcutaneous tissue thickness, local blood flow, local temperature).12 The same individual could have a different recording after sweating, on a dry day, or after starting a new medication, even if muscle activity is unchanged.
It is therefore important that clinicians recognize these extraneous factors, minimize any that can be clinically controlled, and ultimately employ realistic expectations of sEMG as an estimation of neuromuscular recruitment.
Interpretation
Due to these limitations, it can be simpler to describe sEMG data as “active” or “not active” for specific muscles during an activity. While some researchers have analyzed their data using categories such as minimally, moderately, and maximally active, these categories have not been standardized objectively and do not allow comparison between study participants. Documenting muscle activity as active or not active during biofeedback therapy, especially if the patient can compare relative magnitudes to their own previous trials on the same day, can simplify the feedback process for patients and make integrating sEMG analysis into a rehabilitation protocol more patient-friendly.
Future considerations
With a standard for sEMG sensor placement, further research can explore the efficacy of sEMG biofeedback as an augmentation to therapy for any muscular contractions and functional movements a practitioner deems clinically appropriate. For instance, published data on gluteus medius muscle activation during different therapeutic exercises1 could inform an sEMG feedback protocol with placement of sensors on the gluteus medius to facilitate proper patient activation of hip abductors during clamshells, lateral walks, and, finally, return to functional activity and sports.
Potentially, patients could wear wireless sEMG sensors and receive feedback while running outside, biking, lifting large objects for work, dancing, or simply walking down the street. The technology gives clinicians the means to join the nationwide integration of telerehabilitation into physical therapy treatment17 (see “Telerehabilitation after TKA,” August LER, page 15). Clinicians could monitor their patients’ activities in their true participation settings to determine if therapeutic gains in the clinic translate to real-world functional goals.
Currently, the most common and validated sEMG systems are still wired, which limit those potential applications of biofeedback therapies. However, academic clinicians have begun using wireless EMG technologies for kinesiologic inquiry and diagnostic purposes, such as detection of muscle fatigue,18 muscle activation in sit to stands,19 muscular changes in ambulation after anterior cruciate ligament reconstruction,20 effects of tai chi on older adults,21 and studies of sEMG reliability in detecting muscular activation for functional reaching tasks.22 Wireless sEMG is now being used in biotechnologies for exoskeleton prosthetics23 and intraoral controllers for assistive devices.24 However, most studies on the wireless technology itself are limited to description of invention and self-test by the developers.25,26 If clinicians are to adhere to our profession’s standards of evidence-based practice, more evidence is needed to confirm the reliability and validity of these technologies before full integration into clinics.
With the proper setup and muscular specification outlined in this article, clinicians and researchers can join together in furthering the application of both wired and wireless sEMG technologies into patient rehabilitation. Integration of these highly informative and noninvasive biotechnologies has the potential to allow clinicians to be creative in developing therapies for individual patients, using sEMG biofeedback and telerehabilitation monitoring to facilitate each patient’s learning, muscular proprioception, exercise adherence, and return to participation.
Rachelle Bordlee, sDPT, is a third-year student in the Program in Physical Therapy at Columbia University Medical Center in New York City, with anticipated completion of her doctorate in physical therapy in May 2016. Christopher Kevin Wong, PT, PhD, is an associate professor of rehabilitation and regenerative medicine and the associate director of the Physical Therapy Program at Columbia University Medical Center.
Acknowledgment: Special thanks to Harriet Russell, sDPT, (modeling) and Brandon HK Nguyen (photography).
- Distefano LJ, Blackburn JT, Marshall SW, Padua DA. Gluteal muscle activation during common therapeutic exercises. J Orthop Sports Phys Ther 2009;39(7):532-540.
- Stanton R, Ada L, Dean CM, Preston E. Biofeedback improves activities of the lower limb after stroke: a systematic review. J Physiother 2011;57(3):145-155.
- Govil K, Noohu MM. Effect of EMG biofeedback training of gluteus maximus muscle on gait parameters in incomplete spinal cord injury. Neurorehabil 2013;33(1):147-152.
- Akkaya N, Ardic F, Ozgen M, et al. Efficacy of electromyographic biofeedback and electrical stimulation following arthroscopic partial meniscectomy: a randomized controlled trial. Clin Rehabil 2012;26(3):224-236.
- Darsun E, Darsun N, Alican D. Effects of biofeedback treatment on gait in children with cerebral palsy. Disabil Rehabil 2004;26(2):116-120.
- Bolek JE. A preliminary study of modification of gait in real-time using surface electromyography. Appl Psychophys Biof 2003;28(2):129-138.
- Ekblom MM, Eriksson M. Concurrent EMG feedback acutely improves strength and muscle activation. Eur J Appl Physiol 2012;112(5):1899-1905.
- Ng GY, Zhang AQ, Li CK. Biofeedback exercise improved the EMG activity ratio of the medial and lateral vasti muscles in subjects with patellofemoral pain syndrome. J Electromyogr Kines 2008;18(1):128-133.
- Drost G, Stegeman DF, van Engelen BGM, Zwarts MJ. Clinical applications of high-density surface EMG: A systematic review. J Electromyogr Kines 2006;16(6):586-602.
- Hogrel JY. Clinical applications of surface electromyography in neuromuscular disorders. Neurophysiol Clin 2005;35(2-3):59-71.
- Kamen G, Caldwell GE. Physiology and interpretation of the electromyogram. J Clin Neurophysiol 1996;13(5):366-384.
- Electromyography (EMG) Talking Points. American Physical Therapy Association website. http://www.apta.org/StateIssues/EMG/. Published February 20, 2013. Accessed September 8, 2015.
- Hermens HJ, Freriks B. Sensor locations. SENIAM website. http://seniam.org/sensor_location.htm. Accessed September 8, 2015.
- Hermens HJ, Freriks B, Disselhorst-Klug C, Rau G. Development of recommendations for SEMG sensors and sensor placement procedures. J Electromyogr Kines 2000;10(5):361-374.
- Muscolino JE. The muscle and bone palpation manual: with trigger points, referral patterns, and stretching. St. Louis, MO: Mosby/Elsevier: 2009.
- Brooks GA, Fahey TD, Baldwin KM. Exercise physiology: human bioenergetics and its applications. 4th ed. New York, NY: McGraw-Hill: 2005;468-474.
- Lee AC, Harada N. Telehealth as a means of health care delivery for physical therapist practice. Phys Ther 2012;92(3):463-468.
- Chang KM, Liu SH, Wu XH. A wireless sEMG recording system and its application to muscle fatigue detection. Sensors 2012;12(1):489-499.
- Jang EM, Yoo WG. Comparison of the gluteus medius and rectus femoris muscle activities during natural sit-to-stand and sit-to-stand with hip abduction in young and older adults. J Phys Ther Sci 2015;27(2):375-376.
- Arosha Senanayake SM,Ahmed Malik O, Mohammad Iskandar P, Zaheer D. Assessing post-anterior cruciate ligament reconstruction ambulation using wireless wearable integrated sensors. J Med Eng Technol 2013;37(8):498-510.
- Varghese R,Hui-Chan CW, Bhatt T. Effects of tai chi on a functional arm reaching task in older adults: a cross-sectional study. J Aging Phys Activ 2015;23(3):361-368.
- Varghese R,Hui-Chan CW, Wang E, Bhatt T. Internal consistency and test-retest reliability of an instrumented functional reaching task using wireless electromyographic sensors. J Electromyogr Kines 2014;24(5):593-600.
- Ho NS, Tong KY, Fung KL, et al. An EMG-driven exoskeleton hand robotic training device on chronic stroke subjects: Task training system for stroke rehabilitation. IEEE Int Conf Rehabil Robot 2011;2011:5975340
- Maloney SR. Wireless intraoral controller disposed in oral cavity with electrodes to sense E.M.G. signals produced by contraction of the tongue. US patent 5212476 A. May 18, 1993.
- Balouchestani M,Krishnan S. Effective low-power wearable wireless surface EMG sensor design based on analog-compressed sensing. Sensors 2014;14(12):24305-24328.
- Jovanov E, Milenkovic A, Otto C, de Groen PC. A wireless body area network of intelligent motion sensors for computer assisted physical rehabilitation. J Neuroeng Rehab 2005;2(1):6.