 Dry needling is gaining momentum as an alternative therapy for myofascial pain, and is supported by a small but growing body of research as well as anecdotal evidence. But the training and expertise required to perform the procedure has become a topic of debate.
Dry needling is gaining momentum as an alternative therapy for myofascial pain, and is supported by a small but growing body of research as well as anecdotal evidence. But the training and expertise required to perform the procedure has become a topic of debate.
By P.K. Daniel
In recent years, integrative medicine–the combining of conventional practices with alternative therapies–has become more popular in treating a variety of maladies. Dry needling, performed using acupuncture needles, is an East-meets-West modality for treating painful conditions related to the musculoskeletal and nervous systems that has also become more mainstream. Among the lower extremity applications for dry needling, with varying degrees of evidence-based success, are Achilles tendinopathy, plantar fasciitis, chronic lateral hip and thigh pain, and the prevention of pain after total knee arthroplasty.1-4
The technique, also known as intramuscular stimulation and trigger-point dry needling, uses a thin, monofilament needle, which can vary in length and gauge depending on the body part being worked on, to penetrate the skin and stimulate underlying muscular trigger points to treat conditions like myofascial pain syndrome.
Myofascial pain researching pioneer Janet Travell, MD, studied dry needling therapy for treating myofascial trigger points (MTrPs) and muscle dysfunction as early as the 1940s, and developed the trigger point model on which the therapy is based.5 Modern dry needling, however, is credited to Czech neurologist Karel Lewit, MD, DSc, one of the founders of the Prague School of Rehabilitation and Manual Medicine, in 1979.6 Lewit emphasized the needling effect was distinct from that of any injected substance. “In reviewing techniques for therapeutic local anesthesia of pain spots, it appeared that the common denominator was puncture by the needle and not the anesthetic employed,” Lewit noted in his research.6
Targeting trigger points
Although the actual mechanism by which dry needling works is unclear, its utilization is largely based on the trigger point model.
“Trigger points can produce local pain as well as referred pain,” said John Mason, DPT, DSc, SCS, CSCS, a physical therapist and dry needling researcher currently practicing in the Fort Bragg, NC, area.
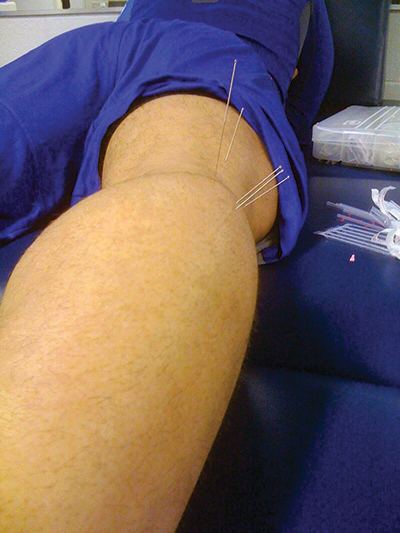
Figure 1. Professional baseball player being treated with dry needling for distal hamstring tendinopathy. (Photo courtesy of Sue Falsone, PT, MS, SCS, ATC, CSCS, COMT.)
The intent is inactivation of the involved trigger point through intramuscular stimulation with the needle, he said.
Jaime Salom-Moreno, PT, PhD, a professor in the Department of Physical Therapy, Occupational Therapy, Physical Medicine and Rehabilitation at the Universidad Rey Juan Carlos in Alcorcón, Spain, explained that a needle is inserted into discrete focal points of taut bands within the muscle and manipulated until local twitch responses (LTRs) are elicited. Once the first local twitch response is obtained, the needle is moved up and down 4 to 5 mm for 25 to 30 seconds.
“The LTR is an involuntary spinal reflex contraction of muscle fibers,” he said. “The main theory presupposes the dysfunction on the endplate of the muscle, which could cause the onset of the pain and motor impairment. The effect of dry needling is to change the activity of endplate dysfunction.”
Mason noted that trigger-point needling should be utilized in combination with stretching, joint mobilizations, strengthening, and neuromuscular re-education to help relax tight bands, normalize muscle tone, and improve the flow of neurochemicals in the affected tissue.
“One of the goals of dry needling is production of a localized twitch response within the muscle,” he said. “It is believed that this twitch response may interrupt dysfunction of the motor endplate.”
Mason published a case study in which a combination of trigger-point dry needling and exercises were utilized on a 16-year-old female ballet dancer who presented with a two-month history of right posterior knee pain. She was treated with dry needling twice to the right gastrocnemius, soleus, and popliteus muscles, with 48 hours between sessions. Palpation identified the MTrPs that reproduced her primary symptoms. The patient also underwent an at-home exercise program (HEP) promoting lower extremity flexibility and hip stability. The HEP, which included daily stretches, got progressively more challenging over one month. There were one-month and three-month follow-ups.7
At the one-month follow-up, the dancer said she had complied with the HEP and had gradually resumed her intensive dance training program. At the three-month follow-up, she again reported being able to continue with her full-training routine without recurrence of symptoms. No additional treatment was needed.7
Evidence and experience
While extensive studies on dry needling have not yet been done, and practitioners acknowledge further research is necessary, there is some evidence of dry needling’s effectiveness, said Salom-Moreno, who was the lead author of a 2014 study published in the Journal of Manipulative and Physiological Therapeutics on the effects of dry needling on stroke spasticity.8
“In the lower limb, there are few studies, but my experience in this area is very positive,” he said.
Dry needling includes both superficial and deep techniques. While deep trigger-point dry needling targets mostly dysfunctional motor units, superficial needling targets primarily peripheral sensory nerve fibers, according to Peter Baldry, MD, who discovered the superficial technique in the early 1980s. Baldry has said the majority of his patients with MTrP pain are treated with superficial dry needling, while those with concomitant MTrP pain and nerve root compression pain may require deep dry needling, which differs in the needle manipulation and the neurophysiological effects.9,10
The objective of Salom-Moreno’s study was to determine the effects of deep dry needling (DDN) on spasticity, pressure sensitivity, and plantar pressure in stroke patients. The researchers concluded that, after just a single session of DDN, both spasticity and widespread pressure sensitivity decreased. They also found that DDN was associated with changes in plantar pressure related to an increased support surface and a decrease in mean pressure.8
Leslie McCoy, LAc, DAOM, who is the chair of the Oriental Medicine department at Pacific College of Oriental Medicine (PCOM) in San Diego, also acknowledged the limited number of studies but pointed to the acupuncture literature as supporting the efficacy of dry needling. For example, a systematic review in the Journal of Orthopaedic and Sports Physical Therapy supported the use of acupuncture to manage musculoskeletal disorders of the extremities, including Achilles tendinopathy and plantar fasciitis.11,12
“Dry needling has a smaller evidence base using the words ‘dry needling,’” McCoy said. “But clinicians performing dry needling can use some acupuncture studies to support efficacy, as they are essentially identical interventions.”
Another Salom-Moreno-led study compared the combined treatment of trigger-point dry needling in the lateral peroneus muscle plus eight weeks of proprioceptive/strengthening exercises to proprioceptive/strengthening exercises alone in patients with painful chronic ankle instability. One month after the intervention, patients who received the combined therapy had better pain and function outcomes than those who did not receive dry needling.13
“In these cases, the patients who met protocol exercises and dry needling produced better results in pain and function,” Salom-Moreno said.
Risks and side effects
As with any treatment, dry needling comes with potential risks and side effects, including soreness and bruising, local hemorrhages at the needling sites, infection, organ puncture, and syncope. The application involves pushing the needle, which can be up to 4 inches long to reach the affected muscle, through the skin to stimulate a trigger point. The process can be uncomfortable, as the practitioner must locate the exact point of pain (the MTrP) to relieve it effectively. This method differs from that of acupuncture, in which the needles are generally inserted a few millimeters below the surface, into the meridian pathway.
“Dry needling is painful, and acupuncture isn’t,” Salom-Moreno said. “This is an important consideration because the people who receive dry needling normally feel soreness for some hours afterward, in contradistinction to acupuncture, where patients are more emotionally influenced.”
Mason concurred that dry needling can be painful.
“But that can vary from patient to patient based on multiple factors,” he said. “The treatment technique involves targeting and inserting the needle directly into sensitive, painful muscle tissue, which may explain, in part, why it can be painful.”
Pneumothorax is a dangerous potential complication in the upper trunk, but is unusual if practitioners have experience with dry needling, Salom-Moreno said. Nerve irritation is a potential risk anywhere in the body.
“In the lower limb, caution should be exercised with the neurovascular area or vessel injuries,” Salom-Moreno said. “However, clinically, there are improvements in pain and functions.”
Controversy can sometimes accompany newly adopted therapies, which has been the case with dry needling. The debate seems to center around the nomenclature. Some clinicians insist the practice is not acupuncture, while some acupuncturists insist that it is. This has to do with nonacupuncturists utilizing acupuncture needles, explained McCoy, a licensed acupuncturist. However, acupuncture needles were not always used for dry needling. Initially, a hollow bore needle (a hypodermic needle) was used by Travell in the 1940s, who later coined the term “myofascial trigger point” after learning that nodules can be present and refer pain to both muscle and overlying fascia.5,14
“Dry needling has been defined as a subset of acupuncture,” said Sue Falsone, PT, MS, SCS, ATC, CSCS, COMT, who is an associate professor of athletic training at Still University in Mesa, AZ. Acupuncture utilizes traditional meridians based on Chinese medicine dating thousands of years, whereas dry needling is based on modern neuroanatomical science.
“In my opinion, the way a person uses a tool defines their profession,” said Falsone, who owns Phoenix, AZ-based SF Dry Needling and S&F: Structure and Function. “In the same way using a hammer to hang a picture in my house does not make me a carpenter, or using a calculator does not make me an accountant, using a fine filiform needle does not make me an acupuncturist.”
There are other attitudes about the two practices.
“As a technique, dry needling and acupuncture are the same,” McCoy said. “The difference, though, lies in the paradigm that guides where the needles should be inserted. A physical therapist might look at a patient’s hip and think, ‘I need to stimulate the gluteus medius muscle.’ An acupuncturist might look at the hip and say, ‘I need to stimulate the shao-yang channel.’ In fact, both clinicians will needle in the same region. The nomenclature will differ, however.”
McCoy, who has worked with the integrative pain team at Rady Children’s hospital in San Diego and whose unpublished doctoral work explored the use of manual needle techniques in the treatment of painful conditions, also said, “Acupuncture could also use needle insertion sites that are distal to the area needing attention. For instance, hip pain treatment might also use insertion of needles in the foot or hand.”
Training
The issue for some in the acupuncture community regarding dry needling comes down to training and licensing.
“While acupuncturists train for four years to safely insert needles, some dry needling practitioners might only have training during a weekend seminar,” McCoy said. “This has led to some controversy in the acupuncture camp, as acupuncturists are worried that an undertrained clinician with a needle might make the treatment look unsafe.”
Novice dry needling practitioners can be too timid, and not fully engage the target tissue, leading to ineffective treatment, McCoy said. Conversely, a novice practitioner might be overly confident, and run the risk of damaging tissue or organs. Some of these concerns were debated in the comments section of an article in the May 2015 issue of PT in Motion.15
Mason said a common mistake of novice practitioners is treating only the location where the patient feels pain.
“Taking the whole body into account in terms of regional interdependence [how one region can affect other regions] is necessary when employing this modality and comes with increased experience,” he said.
One of the foremost authorities on myofascial pain in Spain is clinical researcher and educational physical therapist Orlando Mayoral del Moral, PhD, of Hospital Provincial de Toledo. He said dry needling is very user-specific.
“It is important to have training and experience to get proficiency in its use,” he said. “Not just for the use of the technique, but mainly for the correct diagnosis of the relevant trigger points.”
He said a poor diagnosis of myofascial pain syndrome can lead to treatment of the wrong muscles and a painful, fruitless outcome.
Salom-Moreno agreed the success of dry needling is based in part on the technique of the practitioner. “The experience of the therapist and understanding in neurophysiological, biomechanical, and anatomical concepts are very important,” he said. “However, the clinical examination and a good diagnosis will ensure that the approach is more effective. When the therapist demonstrates the above, dry needling is not difficult.”
Salom-Moreno also agreed that failure to find the myofascial trigger point is a common mistake, along with incorrect palpation of the muscle.
“If you don’t puncture in the dysfunction point, you don’t have good results,” he said. “Therefore, it is very important that the diagnosis and palpation are correct.”
Falsone concurred: “Every tool, in my opinion, is only as good as its practitioner. Patients with all types of pathologies and dysfunctions can benefit. It is important to find a dry needling practitioner or acupuncturist who is very familiar with your pain, disease, or dysfunction. My specialty is orthopedic and sports rehab and sports performance, so that is where and how I utilize dry needling.”
Scope of practice
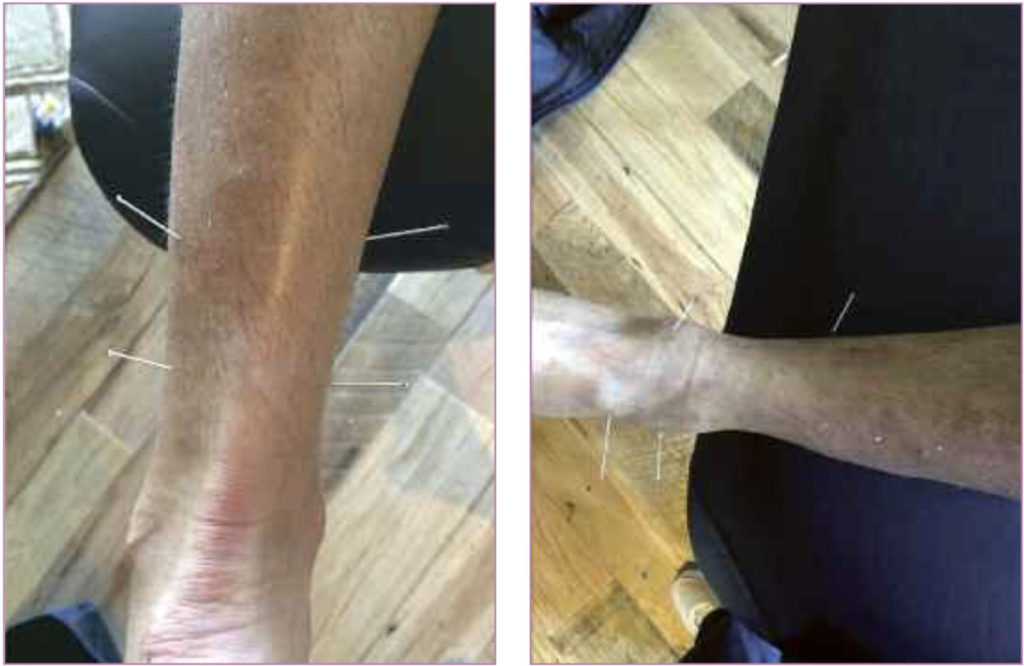
Figure 2. Professional baseball player (not the same as in figure 1) with an anterior ankle impingement. Dry needling was performed at the syndesmosis, posterior tibialis, and ankle joint. (Photo courtesy of Sue Falsone, PT, MS, SCS, ATC, CSCS, COMT.)
Multiple healthcare professionals, including physical therapists, chiropractors, certified athletic trainers, physicians, osteopathic physicians, naturopaths, and nurses, practice dry needling. So, on top of some acupuncturists worrying about the safety issue of undertrained clinicians needling, there are those who worry that allowing other professions to essentially perform acupuncture might limit access to patients for acupuncturists, and therefore their economic livelihood.15
“I don’t share the same concern,” McCoy said. “I think acupuncture—even dry needling—is a viable treatment option for so many musculoskeletal complaints that every patient should have access to it, whether they visit an acupuncturist or a well-trained physical therapist. I think this will actually expand the patient pool, not contract the patient pool. And, it will be of benefit to the patient.”
But the concerns have led to efforts to stop the practice at the legislative level. The Chicago campus of PCOM, in conjunction with other alternative medicine organizations and the Illinois State Medical Society, was instrumental in getting the Illinois Department of Professional Regulation to agree in 2014 that the practice of dry needling is not in the scope of practice of physical therapy.
Although there are more than two dozen states plus the District of Columbia where dry needling has been determined to be within the scope of practice for a physical therapist, California, New York, and Hawaii have ruled that it is not. Other states are examining the issue. However, physical therapists (or physiotherapists) in South Africa, the Netherlands, Spain, Switzerland, Canada, Chile, Ireland, the UK, and New Zealand use it.
“Some will tell you there is no difference between the two [treatments], which is why there is so much controversy surrounding its use in healthcare by people who are not acupuncturists,” said Falsone, who became the first and only female head trainer in Major League Baseball when she was promoted by the Los Angeles Dodgers in 2011.
Falsone thinks there is room for practitioners of both types.
“Personally, I have worked side by side with an acupuncturist, and it was wonderful,” she said. “We would discuss, professionally debate, compare and contrast treatment interventions. We both had great results and worked very well together.”
- Mayoral O, Salvat I, Martín MT, et al. Efficacy of myofascial trigger point dry needling in the prevention of pain after total knee arthroplasty: a randomized, double-blinded, placebo-controlled trial. Evid Based Complement Alternat Med 2013;2013:694941.
- Cotchett MP, Munteanu SE, Landorf KB. Effectiveness of trigger point dry needling for plantar heel pain: a randomized controlled trial. Phys Ther 2014;94(8):1083-1094.
- Pavkovich R. Effectiveness of dry needling, stretching, and strengthening to reduce pain and improve function in subjects with chronic lateral hip and thigh pain: a retrospective case series. Int J Sports Phys Ther 2015;10(4):540-551.
- Wheeler PC, Mahadevan D, Bhatt R, Bhatia M. A comparison of two different high-volume image-guided injection procedures for patients with chronic noninsertional Achilles tendinopathy: A pragmatic retrospective cohort study. J Foot Ankle Surg 2016 Jun 7. [Epub ahead of print]
- Travell JG, Rinzler SH. The myofascial genesis of pain. Postgrad Med 1952;11(5):434-452.
- Lewit K. The needle effect in the relief of myofascial pain. Pain1979;6(1):83-90.
- Mason JS, Tansey KA, Westrick RB. Treatment of subacute posterior knee pain in an adolescent ballet dancer utilizing trigger point dry needling: a case report. Int J Sports Phys Ther 2014;9(1):116-124.
- Salom-Moreno J, Sánchez-Mila Z, Ortega-Santiago R, et al. Changes in spasticity, widespread pressure pain sensitivity, and baropodometry after the application of dry needling in patients who have had a stroke: a randomized controlled trial. J Manipulative Physiol Ther 2014;37(8):569-579.
- Baldry P. Superficial versus deep dry needling. Acupunct Med 2002;20(2-3):78-81.
- Baldry P. Superficial dry needling at myofascial trigger point sites. J Musculoskelet Pain 1995;3(3):117-126.
- Dunning J, Butts R, Mourad F, et al. Dry needling: a literature review with implications for clinical practice guidelines. Phys Ther Rev 2014;19(4):252-265.
- Cox J, Varatharajan S, Côté P, Optima Collaboration. Effectiveness of acupuncture therapies to manage musculoskeletal disorders of the extremities: a systematic review. J Orthop Sports Phys Ther 2016;46(6):409-429.
- Salom-Moreno J, Ayuso-Casado B, Tamaral-Costa B, et al. Trigger point dry needling and proprioceptive exercises for the management of chronic ankle instability: a randomized clinical trial. Evid Based Complement Alternat Med 2015;2015:790209.
- Unverzagt C, Berglund K, and Thomas, JJ. Dry needling for myofascial trigger point pain: a clinical commentary. Int J Sports Phys Ther 2015;10(3):402-418.
- Reis E. Dry needling: getting to the point. PT in Motion. American Physical Therapy Association website. http://www.apta.org/PTinMotion/2015/5/DryNeedling/. Published May 2015. Accessed August 29, 2016.







