 By Zeeshan Husain, DPM, FACFAS, FASPS
By Zeeshan Husain, DPM, FACFAS, FASPS
Hind foot non-unions are a complex orthopedic challenge that clinicians face, particularly due to the unique anatomy and weight-bearing responsibilities of this part of the foot. Non-unions occur when a fracture fails to heal nine months after injury or shows no radiographic improvement over a consecutive 3-month period. This condition is not only painful but can also severely impact mobility and quality of life. Understanding non-unions in the hind foot involves examining various contributing factors such as host medical status, presence of infection, and prior surgical interventions. These factors all play a significant role in the healing process and can complicate treatment, making comprehensive management strategies essential.
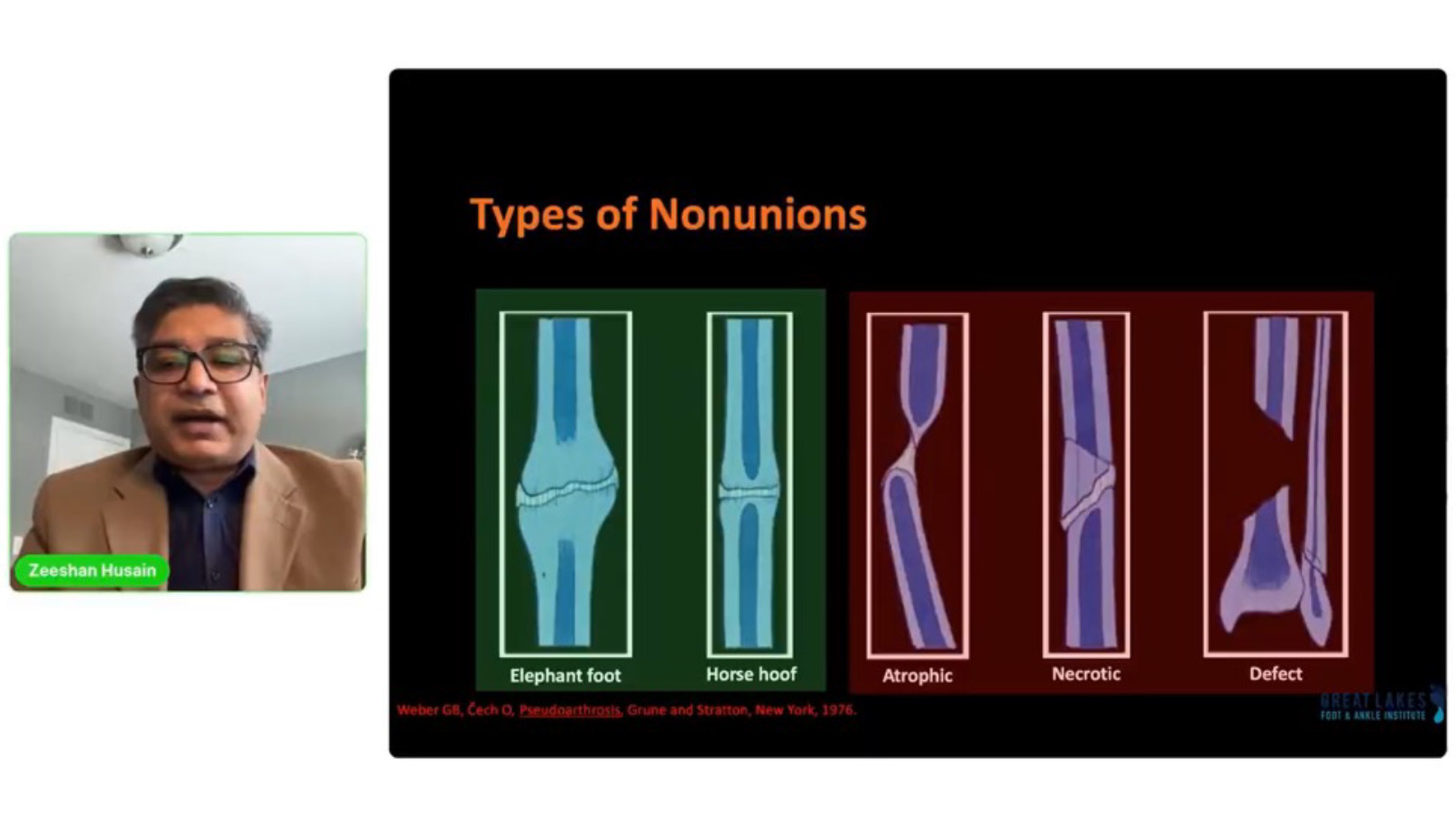
Non-unions occur when a fracture fails to heal within the expected timeframe. Specifically, a fracture is considered a non-union if there is no healing within 9 months or no radiographic improvement over a period of 3 consecutive months. Causes for non-unions include poor vascularity, traumatic injuries, and infections. Often, these factors disrupt the natural bone healing process, making recovery challenging without proper intervention.
Several host factors can increase the risk of non-unions. Patients with vitamin deficiencies, particularly vitamin D, as well as those with poor nutritional status, may face difficulties in bone healing. Smoking and non-compliance with medical advice can also impede recovery. Additionally, diabetic patients, especially those with high hemoglobin A1C levels, are at a greater risk for complications, including infections that may lead to non-unions. Effective management often requires addressing these underlying health concerns through multidisciplinary approaches.
Challenges in Treating Hind Foot Non-Unions
Infection Risks: Infections remain a significant challenge when treating hind foot non-unions. Infection not only contributes to the development of non-unions but also complicates the healing process. Effective treatment necessitates thorough debridement and often involves a multidisciplinary team including surgeons, infectious disease specialists, and clinical pharmacists to manage care and tailor antibiotic therapies.
Weight Bearing Implications: The hind foot’s role in bearing weight complicates the treatment of non-unions. Unlike the forefoot, the hind foot must support significant body weight, which can lead to severe implications for the patient’s quality of life. Non-unions in the hind foot can result in prolonged periods of restricted mobility, increased rehabilitation times, and higher risks of re-injury.
Costs and Patient Satisfaction: Addressing hind foot non-unions can be costly, with expenditures encompassing medical procedures, prolonged treatments, and potential litigation from dissatisfied patients. The complexities of these conditions can lead to lower patient satisfaction, as individuals endure lengthy recovery processes that demand compliance and lifestyle adjustments. Managing these factors is critical to improving outcomes and reducing the financial burden associated with non-unions.
Risk Factors and Diagnostics
 Poor Vascularity and Trauma: Hind foot non-unions often occur due to several underlying factors, including poor vascularity and trauma. Trauma, particularly high-impact injuries or fractures, can significantly impair blood flow to the affected area, leading to delayed or incomplete bone healing. Moreover, poorly vascularized bone tissue struggles to receive the necessary nutrients and oxygen crucial for bone regeneration, thereby increasing the risk of non-union.
Poor Vascularity and Trauma: Hind foot non-unions often occur due to several underlying factors, including poor vascularity and trauma. Trauma, particularly high-impact injuries or fractures, can significantly impair blood flow to the affected area, leading to delayed or incomplete bone healing. Moreover, poorly vascularized bone tissue struggles to receive the necessary nutrients and oxygen crucial for bone regeneration, thereby increasing the risk of non-union.
Compliance and Lifestyle Factors: Patient compliance and lifestyle choices also play a pivotal role in the development of non-unions in the hind foot. Non-compliance with post-operative care, such as failure to adhere to weight-bearing restrictions, can compromise healing. Lifestyle factors, such as smoking and poor nutrition, further exacerbate the risk, as they can impair the body’s ability to repair itself effectively. A high hemoglobin A1C level, especially above 7.7%, can increase susceptibility to infections and complications, further complicating the healing process.
Collaborative Care: Infections are a significant contributor to non-unions and can lead to bone resorption. Accurate diagnosis requires a comprehensive approach, utilizing thorough imaging and microbiological testing. A multidisciplinary team consisting of surgeons, infectious disease specialists, and clinical pharmacists can ensure appropriate management. This team collaborates to design targeted antibiotic therapies and effective intervention plans, often involving surgical debridement and extended follow-up care.
Management Strategies for Non-Unions
Non-Surgical Approaches: Managing non-unions of the hind foot often begins with conservative strategies. These include nutritional optimization and lifestyle modifications to bolster the patient’s overall health and enhance bone healing potential. Addressing vitamin deficiencies, particularly vitamin D, plays a critical role in supporting bone health. Use of bone stimulators, such as ultrasound or electromagnetic devices, can promote healing by stimulating the bone’s natural regenerative processes.
Surgical Techniques and Grafting: When non-surgical efforts prove insufficient, surgical intervention becomes necessary. Techniques often involve stabilization with rigid fixation using plates, screws, or intramedullary nails. Bone grafting is another cornerstone treatment, using autografts or allografts to provide osteogenic, osteoinductive, and osteoconductive properties to the healing site. Meticulous surgical planning and execution are paramount to improving outcomes and minimizing complications.
Supplements and Bone Stimulators: Supplementation with calcium, vitamin D, and vitamin K can enhance bone formation and density, thus aiding recovery. Additionally, bone stimulators are valuable adjuncts in the management of non-unions. These devices generate electrical or electromagnetic fields to augment bone healing processes. By integrating these therapeutic strategies, healthcare professionals can effectively address hind foot non-unions, optimizing patient recovery and long-term foot health.
Conclusion
In conclusion, understanding and addressing non-unions of the hind foot require a comprehensive approach that encompasses the identification of underlying causes, informed diagnosis, and a multidisciplinary treatment plan. Factors such as poor vascularity, infection, vitamin deficiencies, and patient non-compliance must be carefully managed to improve bone healing outcomes. Surgical interventions may include stabilization with various fixation techniques and bone grafting, while non-surgical therapies such as nutritional supplementation and lifestyle modifications play crucial roles. Collaborative care with infectious disease specialists and clinical pharmacists can ensure accurate diagnosis and effective treatment pathways, ultimately enhancing patient outcomes and quality of life. Properly addressing these complex cases requires not only technical expertise but also an awareness of patient-specific factors that may influence healing and recovery.
Zeeshan Husain, DPM, FACFAS, FASPS, is a board-certified foot and ankle surgeon at Great Lakes Foot and Ankle Institute located in Rochester, Chesterfield, Clinton Township, Fort Gratiot, East China Township, and Shelby Township, Michigan. His expertise is in foot and ankle reconstruction, trauma, sports medicine, and diabetic limb salvage and wound care. Dr. Husain is certified by the American Board of Foot and Ankle Surgery in foot and rearfoot reconstruction and ankle surgery, and he’s also a fellow of the American College of Foot and Ankle Surgeons and American Society of Podiatric Surgeons. He is President-Elect of the Michigan Podiatric Medical Association.
This article is a summary of Dr. Husain’s presentation titled, “None of the Joints I Fused healed, Now What?,” from the APMA Surgical Complications Virtual Seminar, January 18, 2025 hosted by lerEXPO.com. To view the slide presentation which includes 2 complex case studies with questions and answers, visit https://apmasurgical.lerexpo.com/. Continuing education credits are available for many lerEXPO.com programs







