By Windy Cole, DPM, CWSP
Use of an antimicrobial moisture management dressing paired with a gellable fiber technology under a two-layer compression system in the treatment of heavily exudating VLUs improves clinical outcomes and cost savings.
 Chronic venous insufficiency is the 7th most common chronic disease and is the underlying cause of 95% of leg ulcers.¹ Venous leg ulcers (VLUs) are difficult to treat, often taking a minimum of 12 weeks to heal.² VLUs are notoriously heavily draining wounds. This drainage contributes to the formation of excessive bioburden, devitalized tissue, and microorganisms, all of which prolong wound healing. To effectively manage VLU exudate, dressing changes 3 or more times weekly are not uncommon. More frequent dressing changes increase the overall cost of care and may contribute to delayed wound healing via disruption of the wound and exposure to external contaminates.
Chronic venous insufficiency is the 7th most common chronic disease and is the underlying cause of 95% of leg ulcers.¹ Venous leg ulcers (VLUs) are difficult to treat, often taking a minimum of 12 weeks to heal.² VLUs are notoriously heavily draining wounds. This drainage contributes to the formation of excessive bioburden, devitalized tissue, and microorganisms, all of which prolong wound healing. To effectively manage VLU exudate, dressing changes 3 or more times weekly are not uncommon. More frequent dressing changes increase the overall cost of care and may contribute to delayed wound healing via disruption of the wound and exposure to external contaminates.
Methods
This single-center retrospective analysis examined the impact on clinical outcomes and cost savings of a dressing combination newly available to our outpatient wound clinic. Standard-of-Care (SOC) dressings consisted of Non-adherent+Silver Alginate+Hydroconductive Dressing+Compression. The new treatment combination consisted of an antimicrobial moisture-management dressing (TRITEC™ Silver Dressing, Milliken Healthcare Products, LLC, Spartanburg, SC) , an innovative gellable fiber dressing (AGILE, Milliken Healthcare Products, LLC), and a two-layer compression system (CoFlex® TLC, Milliken Healthcare Products, LLC).
 Medical records of 6 patients who received the same SOC treatment were reviewed for the 4 weeks prior and the 4 weeks after converting to the new treatment combination. Analyzed data consisted of frequency of bandage changes, cost of wound dressings, wound size, wound tissue appearance, exudate amount, and quality of the peri-wound skin.
Medical records of 6 patients who received the same SOC treatment were reviewed for the 4 weeks prior and the 4 weeks after converting to the new treatment combination. Analyzed data consisted of frequency of bandage changes, cost of wound dressings, wound size, wound tissue appearance, exudate amount, and quality of the peri-wound skin.
Product Details
The antimicrobial moisture-management dressing is two-layered and combined into one dressing by means of a micro-knit process. The dressing pulls away excess exudate while still preserving optimal moisture at the wound bed. Moisture wicks from protection layer (wound facing) to transfer layer (outward facing) reducing the risk for peri-wound maceration. A secondary dressing is required to capture the moisture being wicked through. This primary dressing can be left in place for up to 7 days while secondary dressings and other treatments are replaced as needed
The gellable fiber dressing provides the optimal balance between absorption capacity and structural integrity. While many dressings classified as alginate dressings will burst upon reaching their fibers capacity, this dressing will remain intact. One dressing is capable of absorbing 296% of its own weight. The micro-fibril gelling fibers work to absorb, transport, and disperse fluid in all directions of the dressings. The gellable fiber dressing can be used as either a primary or secondary dressing based on the clinician’s needs.

Venous leg ulcers are a known result of chronic venous insufficiency and venous hypertension. VLUs are already a worldwide problem and are expected to worsen as the population ages. Annual estimated costs for a VLU in the United States range from $13,653 to $18,986 per episode; annual burden is estimated at $14.9 billion.3
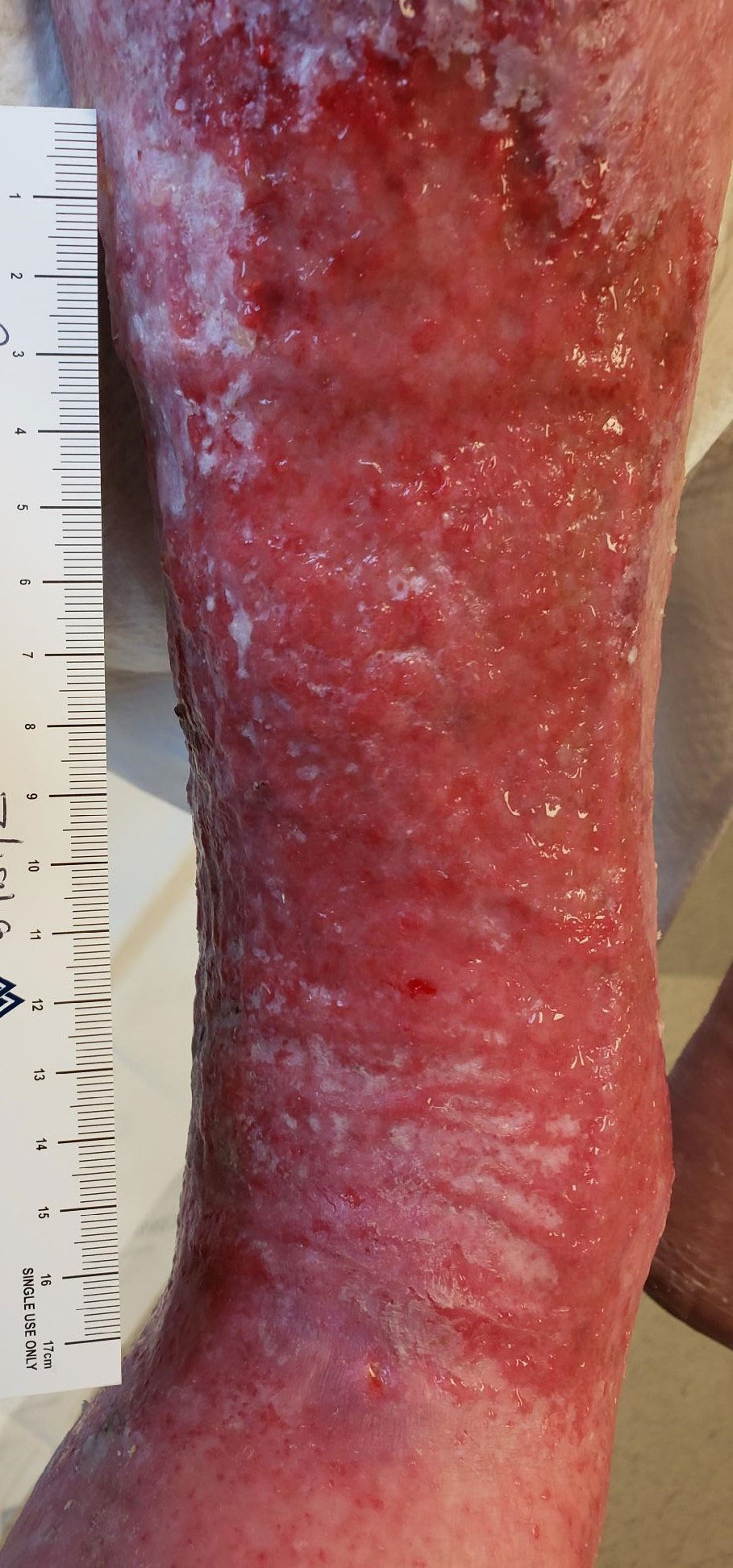
Photo courtesy of Windy Cole, DPM
The two-layer compression system gives patients more freedom and mobility. This system is a short stretch performance designed for active patients with edema. Odor and itch control properties are embedded within the foam first layer. Visual indicators within the second layer guide restorative compression application and ease of application. This system provides non-slip support while still being low profile, lightweight, comfortable, and breathable.
Results
Figure 1 shows that the new dressing combination resulted in an almost 40% reduction in overall dressing change frequency as compared to SOC.
Cost per bandage change decreased by 46% with use of the new dressing combination versus SOC, as seen in Figure 2.
Conclusions
Adoption of the new dressing regimen resulted in several notable outcomes:
- Improved management of exudate resulted in a near 40% decrease in weekly bandage changes
- Per bandage cost decreased by almost half
- Overall average dressing cost savings of $506.64 per patient during the 4-week new bandage adoption period, versus the 4-week SOC treatment period.
- Decreased patient visits required less clinical staff time.
- Wound area continued to progress in a positive direction.
- No treatment related adverse events.
- No patient complaint
Windy Cole, DPM, CWSP, serves as Adjunct Professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine and Student Rotation Coordinator, UH Richmond Medical Wound Center, both in Cleveland, Ohio. She is a dedicated healthcare advocate with interests focused on medical education, diabetic foot care, wound care, limb salvage, clinical research, and humanitarian efforts. Dr. Cole has published extensively on these topics and is a sought-after speaker both nationally and internationally. Dr. Cole also serves as a member of the Editorial Advisory Board for LER.
- Eberhardt R, Raffetto J. Chronic Venous Insufficiency. Circulation. 2014;130(4):333–346.
- Nelson EA, Adderley U. Venous leg ulcers. BMJ Clin Evid. 2016:1902.
- Rice JB, Desai U, Cummings AK, Birnbaum HG, Skornicki M, Parsons N. Burden of venous leg ulcers in the United States. J Med Econ. 2014 May;17(5):347-56.







I appreciated this post’s focus on vascular health. I recently visited a vein restoration clinic and was surprised how comprehensive their diagnostic tools were. They went beyond just surface-level treatment to address deeper vein issues I didn’t even know existed