By Windy Cole, DPM, CWSP, FAPWH
By Windy Cole, DPM, CWSP, FAPWH
Despite advances in wound dressings and best practices, hard-to-heal wounds still remain. Increases in the number of chronic wounds have led to greater antibiotic usage, more hospitalizations, and increased amputations.1 It is therefore necessary to understand the continuum of wound contamination and effectively address bioburden and biofilm. Practicing good wound hygiene and performing regular wound debridement is a key component in achieving better patient outcomes.
Although all chronic wounds exhibit some level of bioburden, most do not need treatment with oral antibiotics. It has been estimated that 80% of chronic wounds contain biofilm.1 What exactly is biofilm? Biofilm consists of a colony of tenacious polymicrobial organisms that form on the wound surface. While these biofilm bacteria are senescent and typically encased in an extra polymeric glycocalyx, the number and complexity of the microbes present can increase the risk for infection.1 The presence of biofilm also contributes to inflammation and wound chronicity.
To support wound healing, biofilm must be removed. Integration of a well-planned and systematic approach to wound hygiene is key. Components of a successful wound hygiene strategy include:2
- Wound Cleansing using antimicrobial washes or surfactants to loosen devitalized tissue, debris, and biofilm.
- Debridement by means of mechanical, sharp, enzymatic, or biologic methods.
- Appropriate wound dressings that manage exudate with or without antimicrobial agents.
The hallmark of good wound hygiene is repetition – Every Wound, Every Visit.
Case Example
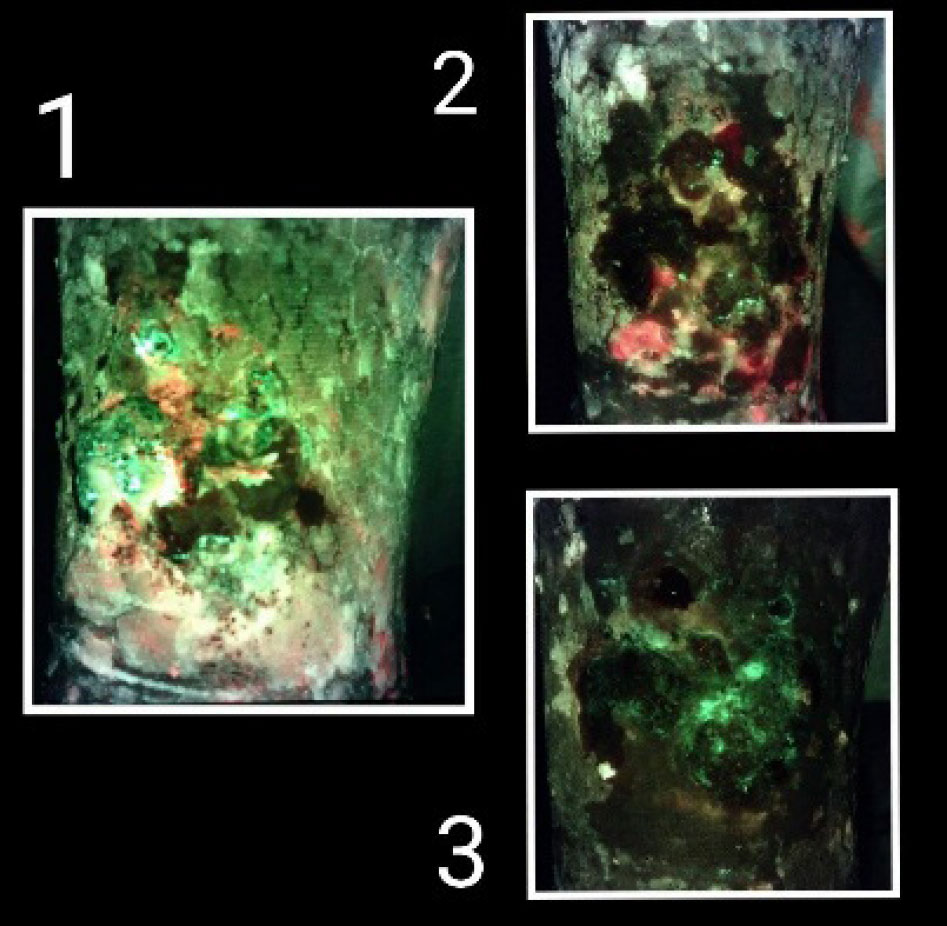
Photo 1 shows a baseline fluorescence image of a chronic wound with an abundance of devitalized tissue and surface bacteria present.
Photo 2 is the same wound after cleaning and debridement. The fluorescent red areas indicate remaining bacterial contamination.
Photo 3 is that same wound after 2 weeks treatment with debridement and collagen matrix containing PHMB. Bacterial contamination has resolved without the use of oral antibiotics. (Polyhexamethylene biguanide [PHMB; polyhexanide] is a broad-spectrum antimicrobial biocide that has been in use for more than 70 years.)
The world is facing a crisis due to the rising rate of bacterial resistance to antimicrobial agents. This resistance is directly related to the increasing utilization of antibiotics.3 Prior treatments with commonly used antibiotics increases a person’s risk for infection, morbidity, length of hospital stay, and overall healthcare costs.3 It has been estimated that 50% of all antibiotic prescriptions are unnecessary or inappropriate.3
Key factors contributing to antimicrobial misuse in patients with wounds include: diagnostic uncertainty, clinical ignorance, clinician fear, and patient demands.3 Possible solutions consist of incorporating rapid point-of-care testing or imaging to detect bacterial contamination and implementing a dedicated antimicrobial stewardship program along with patient education.
Steps to an antimicrobial stewardship program should include the following:
- Avoiding antibiotics when not indicated – wound infections should be diagnosed through clinical signs and symptoms. Uninfected wounds should not be treated with systemic antibiotics.
- Prescribing appropriate antibiotic regimens – use the narrowest spectrum for likely bacteria present initially and then tailor to culture results.
- Ordering antibiotic therapy for the correct duration – treatment should be just long enough to achieve symptom resolution. Consider switching to topical antimicrobial therapy sooner. Typically, 1–2 weeks for soft tissue infections and 6 weeks for bone infection is adequate.
- Always using agents with the least risks and side effects.
Implementing an antimicrobial stewardship program has been associated with a reduction in antimicrobial resistance, better clinical outcomes, and lower costs of care.3
Windy Cole, DPM, CWSP, FAPWH, serves as Adjunct Professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine and Student Rotation Coordinator, UH Richmond Medical Wound Center, both in Cleveland, Ohio. She is a dedicated healthcare advocate with interests focused on medical education, diabetic foot care, wound care, limb salvage, clinical research, and humanitarian efforts. Dr. Cole has published extensively on these topics and is a sought-after speaker both nationally and internationally. Dr. Cole also serves as a member of the Editorial Advisory Board for LER.
- Percival SL, Hill KE, Williams DW, et al. A review of the scientific evidence for biofilms in wounds. Wound Repair Regen. 2012;20(5):647-57.
- Schaper NC, van Netten JJ, Apelqvist J, Bus SA, Hinchliffe RJ, Lipsky BA; IWGDF Editorial Board. Practical Guidelines on the prevention and management of diabetic foot disease (IWGDF 2019 update). Diabetes Metab Res Rev. 2020;36(Suppl 1):e3266.
- Lipsky BA, Dryden M, Gottrup F, Nathwani D, Seaton RA, Stryja J. Antimicrobial stewardship in wound care: a Position Paper from the British Society for Antimicrobial Chemotherapy and European Wound Management Association. J Antimicrob Chemother. 2016;71(11):3026-3035.