Like other common multifactorial conditions, patellofemoral pain syndrome (PFPS) can be frustrating to treat. Contributing factors may include overuse, malalignment, muscular dysfunction, microtrauma, or a combination; multimodal treatment regimens are popular for relieving immediate symptoms. Unfortunately, up to 70% of patients (primarily athletes, more often than not runners) experience relapses five to 20 years after the first occurrence.
Anecdotal and epidemiological evidence has led researchers to suspect that chronic PFPS may be a predictor for developing patellofemoral osteoarthritis (PFOA), which has been reported in 24% of female individuals and 15.4% of male individuals over the age of 55 (see “Is PFPS a precursor to patellofemoral osteoarthritis?.”)
Researchers from the University of the Sciences in Philadelphia have studied kinematics and kinetics during sit-to-stand in patients with PFOA and found similarities to previously reported characteristics of patients with PFPS. In one study, presented in April 2009 at the first international PFPS research retreat in Baltimore, they found significantly greater tibial abduction in patients with PFOA than in controls. And in a second study, presented in October 2009 at the annual meeting of the American College of Rheumatology, they found increased hip abduction and external rotation moments in the PFOA patients compared with the controls.
“We found that increased joint moments were likely due to increased muscle force at the hips and/or knees,” said lead study author Lisa Hoglund, PT, PhD, OCS, an orthopedic physical therapist and assistant professor in the department of physical therapy at the university.
If a relationship between PFPS and PFOA can be identified, clinical interventions that address the former could potentially delay progression of the latter.
“Theoretically, if we figure out a way to minimize PFPS, it may have long-term ramifications down the road,” said Christopher M. Powers, PT, PhD, an associate professor of biokinesiology and physical therapy at the University of Southern California and a co-organizer of the research retreat.
But investigation into the causative link between anterior knee pain and PFOA has been limited. A 2005 study from the U.K. showed 22% of patellofemoral arthroplasty patients reported having anterior knee pain in adolescence compared with 6% of patients with medial unicompartmental arthroplasty.
However, a recent literature review in the September issue of BMC Musculoskeletal Disorders disputed that finding. In addition to the 2005 study, the investigators looked at six small, uncontrolled, observational follow-up studies that were not specifically designed to determine the relationship between anterior knee pain and PFOA. From those six studies, they estimated an annual risk of PFOA ranging from 0% to 3.4% in individuals who had previously experienced anterior knee pain. With so little quality evidence available, the researchers were unable to confirm a link between the two conditions.
Until more comprehensive prospective studies clarify the association between early PFPS and later PFOA, practitioners can benefit from new research to improve diagnoses and treatment protocols.
At the PFPS research retreat, most presentations focused on the mechanisms causing patellofemoral abnormalities, such as pronated foot posture and abnormal increases in hip internal rotation, and treatment interventions. The efficacy of popular multifaceted therapeutic approaches—combining balance, coordination, flexibility, strength training, proprioceptive training, and gait retraining, as well as taping, bracing, tracking, and foot orthoses—is another area of active research.
Investigators and practitioners are also starting to identify PFPS subgroups for whom treatment can be tailored.
“There is a need for a classification system for different subclasses of PFPS —whether the etiology is thought to come from local, proximal, or distal factors,” Hoglund said. “I don’t think a ‘shotgun’ approach is appropriate for every patient. The best approach is to perform a good exam, identify a patient’s impairments, and treat those.”
Powers agreed.
“We have to a) ID the mechanism (and there’s probably more than one), and b) come up with interventions that address them to bring about long-term change,” he said.
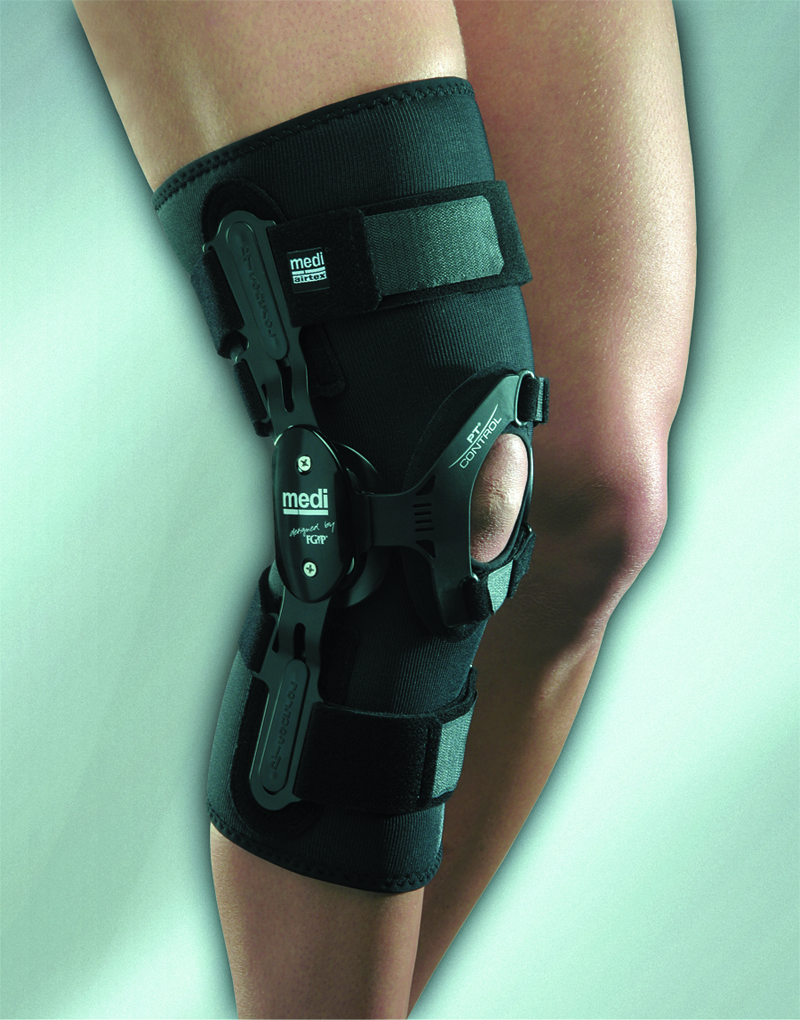
Sponsored by an educational grant from MediUSA