 Ankle-Foot Orthoses (AFOs) play an essential role in the management of various lower extremity conditions. Coding and compliance accuracy and proper documentation can pose a challenge. Providers must accurately explain why the specific AFO is needed. This is not just a box-ticking exercise but a fundamental element to avoid audit failures. Not properly documenting medical necessity is one of most common reasons for audit failure. Providers need to navigate payer-specific rules, where each insurance may have different policies regarding AFO coverage, requiring meticulous attention to detail. Knowing these regulations ensures compliance and facilitates smoother reimbursement processes. Additionally, accurately classifying AFO types–whether custom-fabricated or prefabricated–affects the coding process and ensures proper billing and documentation. By understanding these essential components, providers can significantly enhance their coding accuracy while maintaining compliance.
Ankle-Foot Orthoses (AFOs) play an essential role in the management of various lower extremity conditions. Coding and compliance accuracy and proper documentation can pose a challenge. Providers must accurately explain why the specific AFO is needed. This is not just a box-ticking exercise but a fundamental element to avoid audit failures. Not properly documenting medical necessity is one of most common reasons for audit failure. Providers need to navigate payer-specific rules, where each insurance may have different policies regarding AFO coverage, requiring meticulous attention to detail. Knowing these regulations ensures compliance and facilitates smoother reimbursement processes. Additionally, accurately classifying AFO types–whether custom-fabricated or prefabricated–affects the coding process and ensures proper billing and documentation. By understanding these essential components, providers can significantly enhance their coding accuracy while maintaining compliance.
Importance of Documenting Medical Necessity
Documenting medical necessity is crucial for healthcare providers and necessary for accurate billing and avoiding audit failures. Each instance of medical necessity must tell a complete story to justify why an AFO is necessary for the specific patient. This narrative should clearly explain the patient’s condition and how the AFO will address their unique needs, moving beyond generic templates. Detailed documentation helps auditors quickly understand and validate the necessity of the device, ensuring compliance and proper reimbursement.
Common Pitfalls in Medical Necessity Documentation
 Providers often document vague or insufficient narratives. The story of why must be in the documentation. Common mistakes include failing to tailor the documentation to the individual patient’s condition and inadvertently using boilerplate language. Another frequent error is merely listing the diagnosis or the product name without detailing how the AFO will benefit the patient. This can lead to audit issues. Auditors need specific information to verify medical necessity. To avoid these errors, providers should ensure their documentation is patient-specific and precisely outlines the functional need for the AFO.
Providers often document vague or insufficient narratives. The story of why must be in the documentation. Common mistakes include failing to tailor the documentation to the individual patient’s condition and inadvertently using boilerplate language. Another frequent error is merely listing the diagnosis or the product name without detailing how the AFO will benefit the patient. This can lead to audit issues. Auditors need specific information to verify medical necessity. To avoid these errors, providers should ensure their documentation is patient-specific and precisely outlines the functional need for the AFO.
Identifying and Verifying Third-Party Payer Policies
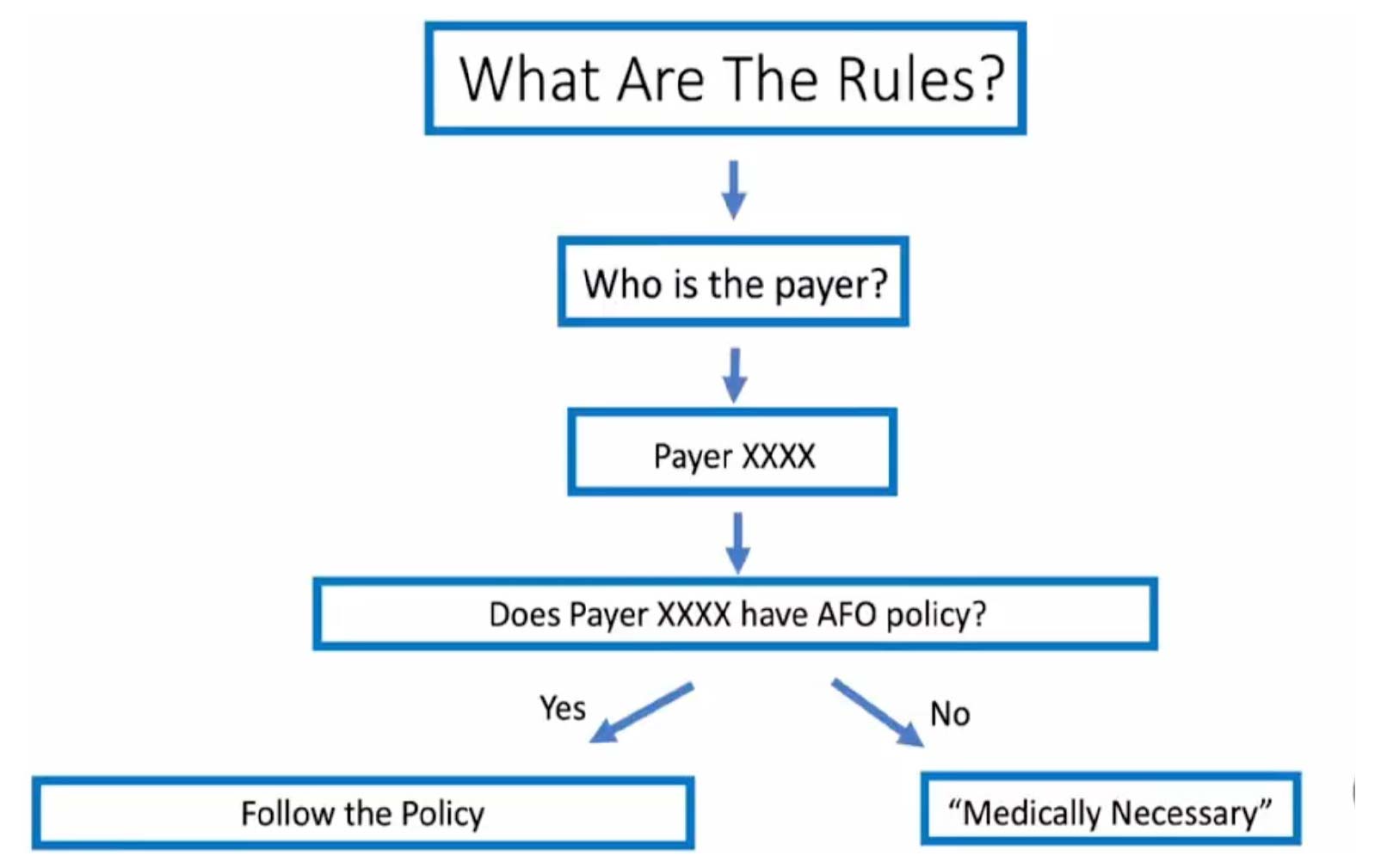
Navigating payer-specific rules requires healthcare providers to understand that while many insurance policies are similar when it comes to AFO coverage, they should not all be treated the same. Identifying and verifying each third-party payer’s policies is essential. Providers should regularly check payer websites for specific AFO policies, which often include detailed documentation and coverage requirements. In the absence of a specific policy, coverage hinges on demonstrating medical necessity–a task that demands comprehensive evidence and justification.
Differences in Medicare and Non-Medicare Policies
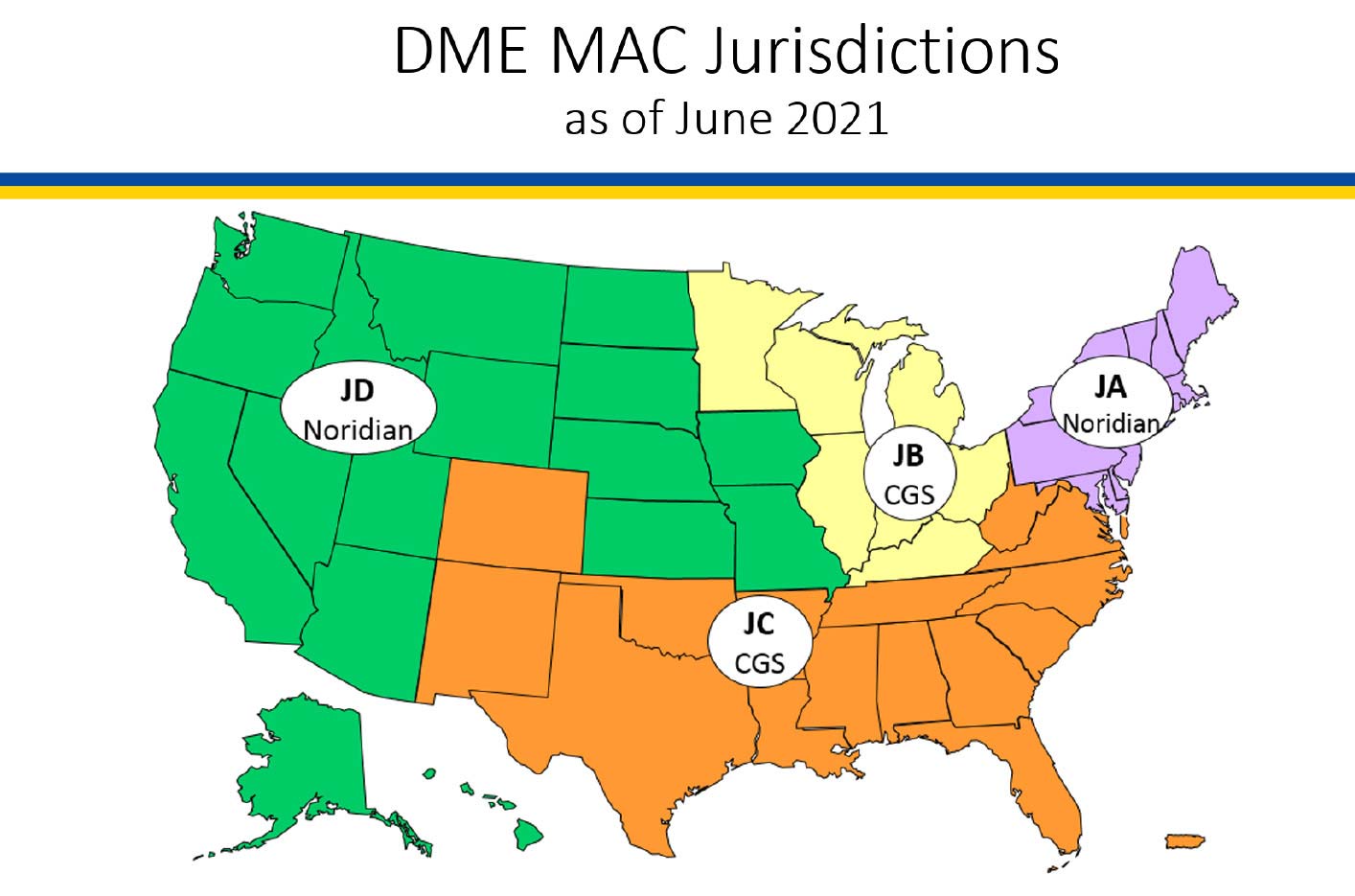
Medicare beneficiaries benefit from a single, nationwide AFO policy, encompassing uniform guidelines governed by Durable Medical Equipment (DME) Medicare Administrative Contractors (MACs) across the country. However, it is crucial not to assume these rules apply to non-Medicare patients as well. Although many non-Medicare insurers might align their policies with Medicare, variations do exist, necessitating careful verification of payer guidelines. Providers must verify individual payer policies to ensure compliance when serving patients under different plans.
Utilizing DME MAC Policies for Compliance
DME MAC policies provide a direct guide for ensuring AFO coding compliance. These policies, available for free online, offer detailed coverage criteria and documentation requirements. By aligning with DME MAC guidelines, healthcare professionals can reduce errors and streamline the compliance process, ultimately safeguarding against potential audit failures while ensuring appropriate reimbursement for their services.
Distinction Between Custom Fabricated and Prefabricated AFOs
 When it comes to Ankle-Foot Orthoses (AFOs), it’s crucial to correctly classify them to ensure proper coding and compliance in order for them to be covered. The first distinction is how the device is constructed.
When it comes to Ankle-Foot Orthoses (AFOs), it’s crucial to correctly classify them to ensure proper coding and compliance in order for them to be covered. The first distinction is how the device is constructed.
- Custom Fabricated AFOs are made specifically for individual patients, often using a mold or digital rendering.
- Prefabricated AFOs are mass-produced and not tailored to any specific patient from the outset.
Understanding this distinction is essential to avoid the common error of misclassification.
Understanding the Differences in Off-the-Shelf and Custom Fitted
Prefabricated AFOs are further categorized based on the fitting procedure.
- Prefabricated Off-the-Shelf: Manufactured en masse and can be fitted by patients themselves and does not require specialized expertise.
- Prefabricated Custom Fitted: Do require someone with specialized training to modify them, such as adjusting angles or reshaping components, indicating a higher level of expertise in fitting the device.
Documentation Requirements for Each AFO Type
Each AFO type requires specific documentation. For custom fabricated AFOs, it’s crucial to explain why such a level of customization was necessary; such as severe deformity. For prefabricated custom fitted AFOs, the documentation should detail why the expert fitting was necessary.
Ensuring Correct Code Selection and Documentation Specifics
 Correct code selection is paramount. AFOs are coded using Healthcare Common Procedure Coding System (HCPCS) codes, not CPT codes. Each code has precise descriptors. The device must align with these specifications, and the documentation should adopt language from these descriptors, not just mention the brand name.
Correct code selection is paramount. AFOs are coded using Healthcare Common Procedure Coding System (HCPCS) codes, not CPT codes. Each code has precise descriptors. The device must align with these specifications, and the documentation should adopt language from these descriptors, not just mention the brand name.
Providers must also verify device specifications themselves rather than relying on manufacturer claims. Manufacturers may suggest codes, but these should be cross-referenced with official descriptions to ensure accuracy in billing and compliance.
Understanding Advance Beneficiary Notices (ABNs)
ABNs are exclusive to Medicare and should only be used when the service being provided is not reasonable and necessary. They should not be issued routinely or as a precaution for high-cost items. Proper documentation and adherence to specified coverage rules mitigate the need for ABNs.
Conclusion
In conclusion, ensuring coding accuracy and compliance when dispensing Ankle-Foot Orthoses (AFOs) is crucial for healthcare providers, particularly in avoiding audit failures. The cornerstone of success is meticulous documentation of medical necessity, tailored specifically to each patient. This narrative should be a detailed story that explains why the AFO is needed and how it benefits the patient’s condition.
To navigate the complex landscape of payer policies, it is essential to verify each payer’s specific rules and requirements, as there is no single rule applicable to all situations. Providers must distinguish clearly between custom-fabricated, prefabricated off-the-shelf, and prefabricated custom-fitted AFOs, as these classifications directly impact coding choices and documentation requirements.
Moreover, documenting the specific technical specifications of the AFO using the language from code descriptors is vital to compliance and accurate billing. Utilizing resources like the DME MAC policies available online can further aid in understanding and meeting Medicare requirements, while remaining mindful of payer-specific nuances.
By adopting these comprehensive documentation strategies, providers can ensure accurate coding, maintain compliance with varying payer policies, and ultimately secure the necessary reimbursement for AFO services provided to their patients.
This article is an AI-generated summary of Dr. Lehrman’s presentation, “PTTD Ankle-Foot Orthoses Coding, Compliance, and Documentation,” from lerExpo’s Conservative Approach to PTTD Seminar. To view the full presentation with questions and answers–and see the agenda for the program, visit https://pttd.lerexpo.com/. Continuing education credits are available for this and many of the lerEXPO programs.
- Who are the MACS. Centers for Medicare & Medicaid Services. 2021. Accessed June 3, 2025. https://www.cms.gov/medicare/coding-billing/medicare-administrative-contractors-macs/who-are-macs







