 The increasing utilization of total knee arthroplasty has led to increased efforts to identify variables that can be modified to help improve postoperative functional outcomes. These risk factors include patient weight, smoking, diabetes, infection, and joint range of motion.
The increasing utilization of total knee arthroplasty has led to increased efforts to identify variables that can be modified to help improve postoperative functional outcomes. These risk factors include patient weight, smoking, diabetes, infection, and joint range of motion.
By John Ryan Quinn, MD, and Ran Schwarzkopf, MD, MSc
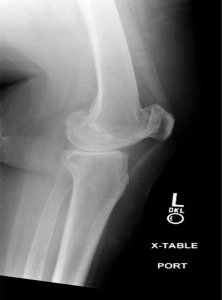
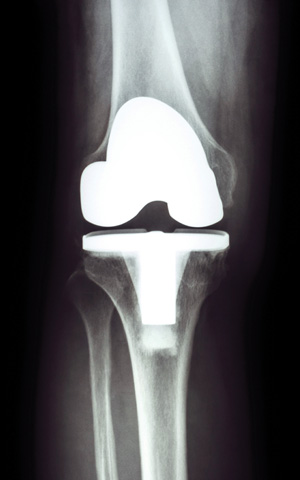
In the last decade, the number of primary total knee arthroplasties (Figures 1-2) performed annually has doubled.1 In 2009, more than 620,000 total knee arthroplasties (TKAs) were performed, and this number continues to increase annually.1 The demand for primary TKA is expected to grow by 673% to 3.48 million procedures by 2030.2,3 One factor contributing to this projection is the increasing number of younger individuals (aged 45-64 years) in need of a primary TKA. In fact, the average age of patients receiving a TKA has decreased over time.1 The increasing demand for TKA in younger people combined with increasing life expectancy suggests that more individuals will need TKA.
Even though primary TKA has a high success rate and a relatively low risk of complication or failure, as more individuals in the US undergo primary TKA, the number of patients at risk by definition will continue to increase.1 For these reasons, it is imperative to identify patient characteristics that predict functional outcomes after TKA. Moreover, we should explore opportunities to implement preoperative, perioperative, and postoperative strategies to maximize functional outcomes and, in turn, patient satisfaction.
Weight
Patient selection based on preoperative characteristics is as important as the technical placement and alignment of the prosthetic implant. One specific patient characteristic that needs to be evaluated is body mass index (BMI). Unfortunately, the obesity epidemic continues to grow within the US. It is estimated that more than 34% of the US population is obese (defined as a BMI higher than 30 kg/m2).4 It is well documented that obesity is associated with knee osteoarthritis, which is a major contributor to TKA (Figures 3-5). In a preoperative risk stratification study, Ng et al identified that one-half of all patients undergoing TKA were obese.5
Nearly all studies demonstrate an increased risk—ranging from fourfold to tenfold—of infection in obese patients undergoing TKA.6-9 A meta-analysis by Kerkhoffs et al found evidence that patients with a BMI of 30 or greater had more infections and a higher revision rate after TKA than patients with a BMI of less than 30.10 It is believed that the excess adipose tissue requires longer incisions and tourniquet times, resulting in more tissue necrosis that may lead to wound complications.11-13
It is important to inform patients of the increased risks and allow them the opportunity to exercise and make dietary modifications and behavioral changes before undergoing TKA. Even if patients fall short of their specific weight-loss goals, they will benefit from optimization of their medical comorbidities, allowing for a safer and an improved outcome after a TKA; the meta-analysis by Kerkhoffs et al concluded that obese patients without comorbidities do not have the same risk as those with comorbidities.10
Diabetes
Obesity is further compounded by diabetes. Approximately 8% to 10% of patients undergoing TKA are affected by diabetes.14 Following a TKA, patients with diabetes have higher risks of pulmonary embolism, postoperative hemorrhage, infection, wound complications, ileus, and even death compared with patients without diabetes.15 In a retrospective study of 4241 TKAs, patients with diabetes had an infection rate of 3.43% (12 of 350 TKAs) while nondiabetic patients had an infection rate of .87% (34 of 3891 TKAs).15
It is important to optimize patients’ diabetic control prior to TKA to reduce the risk of complications; a hemoglobin A1C level below 7 is recommended.16 Preoperative management of diabetes is just as important as postoperative care: a random blood glucose level should consistently be less than 180 mg/dL during hospitalization.16 Again, optimization of patient risk factors prior to TKA is crucial for achieving the best possible outcomes.
Smoking
Smoking, which has detrimental effects on the immune system and on oxygen delivery to the tissues, also needs to be addressed.17,18 Complications after TKA, such as infection, hematoma, and problems with wound healing, are significantly less common in patients who quit smoking six to eight weeks prior to surgery than in persistent smokers.19-21
Intervention consisting of nicotine replacement and intense counseling has been reported to be effective in relieving these patients of a habit that is difficult to break,5 and there is no evidence showing nicotine replacement has an adverse effect on skin healing.20 Again, intervention is imperative; a 2011 meta-analysis found that preoperative smoking cessation was associated with a 41% relative reduction in the risk of postoperative complications after a range of surgical procedures, and each week of smoking cessation increases the positive effects by 19%.22
Pain

Figure 3. Lateral radiograph of right knee showing osteoarthritis: joint space narrow- ing, osteophytes, sclerosis, and subchondral cysts.
Pain control has been researched continuously in an ongoing effort to improve patient satisfaction and outcome. Recent reports have demonstrated only 70% to 88% satisfaction rates following TKA with regard to improvement in function and decrease in pain.23-25 On the other hand, 10% to 30% of patients complain of consistent moderate to severe pain at one to seven years after TKA.26-32
Noiseux et al prospectively analyzed preoperative predictors of pain following TKA in 215 patients. They concluded that characteristics such as marital status, anxiety, depression, and pain catastrophizing were associated with moderate to severe pain following a postoperative TKA range of motion test at six months.33 They also found that patients with severe preoperative knee pain at rest or during a simple knee range of motion test were 10 times more likely to have moderate to severe pain with range of motion six months after TKA than those with less severe preoperative pain.33 These findings are supported by those of Judge et al, who analyzed a prospective cohort of 1991 patients undergoing primary TKA and found those with less pain and better function preoperatively were more likely to achieve better postoperative function and pain control than those who were more symptomatic preoperatively.34
Another study found that preoperative psychological distress was associated with poorer outcomes related to function and quality of life one year after receiving a TKA; however, preoperative psychological distress was not associated with postoperative pain levels.35
Again, the literature suggests that selection of patients preoperatively can have a considerable effect on surgical outcomes and satisfaction. Patients should be examined thoroughly to assess how much postoperative pain they may experience, and they should be educated appropriately. Also, if a patient does suffer from any psychological impairment, it is important to take steps to reduce the patient’s distress prior to surgery so that better postoperative results can be attained. It is essential to identify risk factors for pain and implement a multimodal protocol that will help preempt and control pain and nausea while simultaneously allowing for early ambulation and hospital discharge. Multimodal pain protocols have helped change patient experiences drastically following TKA by encouraging early ambulation and allowing for shorter hospital time.36
Infection
As stated above, by 2030, it is estimated that nearly 3.48 million primary TKAs will be performed annually.2 Approximately 38,000 to 270,000 of those TKAs will be affected by infection.2 Periprosthetic infections occur within the first two years after surgery in 2% of all TKA patients, and roughly 19% of those infections occur within the first 90 days after operation.37 Periprosthetic infection creates a heavy burden for all patients, as quality of life is negatively affected during infection treatment and eradication. Strategies to decrease periprosthetic infection risk are of the utmost importance to all healthcare providers involved in the care of a TKA patient. These can include preoperative, intraoperative, and postoperative measures.
Steps that can be taken preoperatively include detection and management of patients colonized by Staphylococcus aureus, nutritional optimization, and management of medical comorbidities. Medical optimization has been discussed previously.
In 2001, about 33% of the US population was colonized by S. aureus.38 S. aureus colonization can lead to periprosthetic joint infections.39,40 Even though the exact mechanism remains unclear, many studies have shown that implementation of decolonization protocols can decrease the incidence of surgical-site infections in total joint arthoplasty.41-43 Decolonization protocols include a combination of mupirocin nasal ointment application, chlorhexidine mouthwash, and chlorhexidine body wash for up to five days prior to surgery. Rao et al found the combination of mupirocin nasal application and chlorhexidine body wash in patients who tested positive for S. aureus in their nares significantly decreased the risk of postoperative infection in total joint arthroplasty.41 Patients should be screened appropriately and follow the decolonization protocol.
Nutritional optimization in patients undergoing TKA can help decrease the risk of superficial infection, as well as periprosthetic infection. Studies have shown that a lymphocyte count higher than 1500 cells/μL, albumin level higher than 3.5 g/dL, a zinc level higher than 5 μg/dL, and a transferrin level higher than 200 mg/dL are associated with not only a reduced risk of infection among patients, but also a decreased risk of delayed wound healing.44-47
Postoperative measures to prevent infection begin with perioperative antibiotics. Among the recommended antibiotics are the cephalosporins cefazolin and cefuroxime and, if allergy to these antibiotics is present, clindamycin, levofloxacin, or vancomycin can be used.48 If a preoperative nasal screen reveals MRSA (methicillin resistant S. aureus), adding vancomycin is recommended. The antibiotic timeframe should not exceed 24 hours after total joint arthroplasty because of increased risk of resistance and toxicity and a lack of evidence that prolonged antibiotic use decreases risk of infection.48 It is well documented that the use of antibiotics perioperatively decreases the risk of periprosthetic infection in all joint replacements.49-52
Another postoperative measure to decrease risk of infection is to minimize blood product transfusion perioperatively. TKA patients who receive a blood transfusion are 2.1 times more likely to develop an infection than those who do not, and the risk of infection increases with each unit transfused.53,54
Length of hospital stay is also associated with risk of infection and perioperative complications. Fortunately, the mean length of a hospital stay following a total joint arthroplasty has decreased dramatically, from 9.3 days in 1990 to 3.7 days in 2008.55,56 Patients after TKA now have hospital stays averaging from one to four days in length.57
Infection must be avoided in TKA, and a multispecialty approach should be used to help control all possible factors leading to infection. Multiple measures taken perioperatively help assure that the best possible functional outcome is achieved.
Motion
The functional variable that is most often assessed after TKA is postoperative knee range of motion, an important clinical outcome that affects everyday life activities.58 Many factors influence postoperative knee range of motion, but the primary factor is preoperative range of motion.48,57-59 Ritter et al evaluated multiple potential predictive variables in 4727 TKA patients and found that preoperative flexion was the best predictor of postoperative knee flexion.48
Another valuable aid in increasing postoperative motion is extensive early physiotherapy.57 The importance of early postoperative mobility is paramount considering the decreasing hospital stay after TKA surgery, which limits the extent to which therapy can be done while the patient is in the hospital.57 The decreasing time spent in the hospital warrants continued physiotherapy at an outpatient facility or at home where further treatment and education can take place. Patients should be provided with a home physical therapy rehabilitation regimen to continue increasing their postoperative range of motion.
The decreased hospital time also emphasizes the importance of maximizing patients’ range of motion preoperatively. Practitioners should educate patients about the importance of perioperative activity as well as physiotherapy to achieve the best possible outcomes.
Contralateral knee
Another factor contributing to improving outcome and satisfaction is identifying how contralateral knee function affects TKA outcome. Few studies have addressed the effects of the contralateral knee on the operated TKA knee. Nevertheless, Kahn et al revealed a significant relationship between severity of symptoms in the contralateral knee and eventual TKA outcome.60 They reported that lower preoperative WOMAC (Western Ontario and McMaster Universities Osteoarthritis Index) scores in the contralateral knee were associated with poorer short-term outcomes in the operated TKA knee.60 Moreover, postoperative WOMAC score for the contralateral knee was correlated with postoperative WOMAC scores for the operated knee, revealing that poor contralateral knee function negatively affects overall function of the operated knee after TKA.60
Other studies have reported an association between contralateral knee pain and TKA function. Farquhar et al proved that contralateral knee pain and quadriceps strength following TKA were significant predictors of function for up to three years.61 Zeni et al confirmed these results by showing that poor contralateral quadriceps strength led to worse TKA outcomes at one- and two-year marks.62 These relationships are crucial in determining functional outcomes in patients considering TKA. It is important to consider the function and pain levels of the contralateral knee and, if appropriate, to consider the possibility of changing the definitive treatment to a closely staged bilateral TKA or simultaneous TKAs (Figure 5).60
Conclusion
The rapid growth in TKA popularity has led to increased efforts to identify protocols that will lead to an excellent functional outcome. Risk factors for infection—a serious risk in patients undergoing TKA—should be optimized to the greatest extent possible. It is important that preoperative, perioperative, and postoperative strategies be utilized to maximize functional outcomes and patient satisfaction.
John Ryan Quinn, MD, is an orthopedic surgery resident training at the University of California, Irvine. Ran Schwarzkopf, MD, MSc, is an assistant clinical professor of orthopaedic surgery at University of California, Irvine, who specializes in hip and knee joint replacement.
- Weinstein AM, Rome BN, Reichmann WM, et al. Estimating the burden of total knee replacement in the United States. J Bone Joint Surg Am 2013;95(5):385-392.
- Kurtz S, Ong K, Lau E, et al. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J Bone Joint Surg Am 2007;89(4):780-785.
- Kurtz S, Ong K, Lau E, Bozic K. Impact of the economic downturn on total joint replacement demand in the United States: updated projections to 2021. J Bone Joint Surg Am 2014; 96(8):624-630.
- Vincent HK, Vincent KR, Lee LW, Alfano AP. Effect of obesity on inpatient rehabilitation outcomes following total knee arthroplasty. Clin Rehabil 2007;21(2):182-190.
- Ng VY, Lustenberger D, Hoang K, et al. Preoperative risk stratification and risk reduction for total joint reconstruction. J Bone Joint Surg Am 2013;95(e19):1-15.
- Namba RS, Paxton L, Fithian DC, Stone ML. Obesity and perioperative morbidity in total hip and total knee arthroplasty patients. J Arthroplasty 2005;20(7 Suppl 3):46-50.
- Samson AJ, Mercer GE, Campbell DG. Total knee replacement in the morbidly obese: a literature review. ANZ J Surg 2010;80(9):595-599.
- Malinzak RA, Ritter MA, Berend ME, et al. Morbidly obese, diabetic, younger, and unilateral joint arthroplasty patients have elevated total joint arthroplasty infection rates. J Arthroplasty. 2009;24(6 Suppl):84-88.
- Winiarsky R, Barth P, Lotke P. Total knee arthroplasty in morbidly obese patients. J Bone Joint Surg Am 1998;80(12):1770-1774.
- Kerkhoffs GM, Servien E, Dunn W, et al. The influence of obesity on the complication rate and outcome of total knee arthroplasty. J Bone Joint Surg Am 2012;94(20):1839-1844.
- Samson AJ, Mercer GE, Campbell DG. Total knee replacement in the morbidly obese: a literaturereview. ANZ J Surg 2010;80(9):595-599.
- Booth RE Jr. Total knee arthroplasty in the obese patient: tips and quips. J Arthroplasty 2002;17 (4Suppl 1):69-70.
- Christensen CP, Jacobs C. Morbidly obese TKA patients require lengthier operative procedure and hospital stay. J Arthroplasty 2009;24(2):e69.
- Marchant MH Jr, Viens NA, Cook C, et al. The impact of glycemic control and diabetes mellitus on perioperative outcomes after total joint arthroplasty. J Bone Joint Surg Am 2009;91(7):1621-1629.
- Illingworth KD, Mihalko WM, Parvizi J, et al. How to minimize infection and thereby maximize patient outcomes in total joint arthroplasty: a multicenter approach. J Bone Joint Surg Am 2013;95(e50):1-13.
- Moghissi ES, Korytkowski MT, DiNardo M, et al. American Association of Clinical Endocrinologists and American Diabetes Association consensus statement on inpatient glycemic control. Endocr Pract 2009;15(4): 353-369.
- Sopori ML, Kozak W. Immunomodulatory effects of cigarette smoke. J Neuroimmunol 1998;83(1-2):148-156.
- Jensen JA, Goodson WH, Hopf HW, Hunt TK. Cigarette smoking decreases tissue oxygen. Arch Surg 1991;126(9):1131-1134.
- Møller AM, Villebro N, Pedersen T, Tønnesen H. Effect of preoperative smoking intervention on postoperative complications: a randomised clinical trial. Lancet 2002;359(9301):114-117.
- Thomsen T, Tønnesen H, Møller AM. Effect of preoperative smoking cessation interventions on postoperative complications and smoking cessation. Br J Surg 2009;96(5):451-461.
- Lindstrom D, Sadr Azodi O, Wladis A, et al. Effects of a perioperative smoking cessation intervention on postoperative complications: a randomized trial. Ann Surg. 2008;248(5):739-745.
- Mills E, Eyawo O, Lockhart I, et al. Smoking cessation reduces postoperative complications: a systematic review and meta-analysis. Am J Med 2011;124(2):144-154.
- Bourne RB, Chesworth BM, Davis AM, et al. Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res 2010;468(1):57-63.
- Anderson JG, Wixson RL, Tsai D, et al. Functional outcome and patient satisfaction in total knee patients over the age of 75. J Arthroplasty 1996;11(7):831-840.
- Heck DA, Robinson RL, Partridge CM, et al. Patient outcomes after knee replacement. Clin Orthop Relat Res 1998;(356):93-110.
- Williams O, Fitzpatrick R, Hajat S et al. Mortality, morbidity, and 1-year outcomes of primary elective total hip arthroplasty. J Arthroplasty 2002;17(2):165-171.
- Nilsdotter AK, Petersson IF, Roos EM et al. Predictors of patient relevant outcome after total hip replacement for osteoarthritis: a prospective study. Ann Rheum Dis 2003;62(10):923-930.
- MacWilliam CH, Yood MU, Verner JJ, et al. Patient-related risk factors that predict poor outcome after total hip replacement. Health Serv Res 1996;31(5):623-638.
- Jones CA, Voaklander DC, Suarez-Almazor ME. Determinants of function after total knee arthroplasty. Phys Ther 2003;83(8):696-706.
- Judge A, Cooper C, Williams S, et al. Patient-reported outcomes one year after primary hip replacement in a European collaborative cohort. Arthritis Care Res 2010;62(4):480-488.
- Heck DA, Robinson RL, Partridge CM, et al. Patient outcomes after knee replacement. J Arthroplasty 1998;(356):93-110.
- Kennedy LG, Newman JH, Ackroyd CE, et al. When should we do knee replacements? Knee 2003;10(2):161-166.
- Noiseux NO, Callaghan JJ, Clark CR, et al. Preoperative predictors of pain following total knee arthroplasty. J Arthroplasty 2014;29(7):1383-1387.
- Judge A, Arden NK, Copper C, et al. Predictors of outcomes of total knee replacement surgery. Rheumatology 2012;51(10):1804-1813.
- Utrillas-Compaired A, De la Torre-Escuerdo BJ, Martinez AJ, Barco AA. Does preoperative psychological distress influence pain, function, and quality of life after TKA? Clin Orthop Relat Res 2014;472(8):2457-2465.
- Deirmengian C, Lonner JH. What’s new in adult reconstructive knee surgery. J Bone Joint Surg Am 2014;96(2):169-174.
- Berbari EF, Hanssen AD, Duffy MC, et al. Risk factors for prosthetic joint infection: case-control study. Clin Infect Dis 1998;27(5):1247-1254.
- Kuehnert MJ, Kruszon-Moran D, Hill HA, et al. Prevalence of Staphylococcus aureus nasal colonization in the United States, 2001-2002. J Infect Dis 2006;193(2):172-179.
- Yano K, Minoda Y, Sakawa A, et al. Positive nasal culture of methicillin-resistant Staphylococcus aureus (MRSA) is a risk factor for surgical site infection in orthopedics. Acta Orthop. 2009;80(4):486-490.
- Kalmeijer MD, van Nieuwland-Bollen E, Bogaers-Hofman D, de Baere GA. Nasal carriage of Staphylococcus aureus is a major risk factor for surgical-site infections in orthopedic surgery. Infect Control Hosp Epidemiol 2000;21(5):319-323.
- Rao N, Cannella BA, Crossett LS, et al. Preoperative screening/decolonization for Staphylococcus aureus to prevent orthopedic surgical site infection: prospective cohort study with 2-year follow-up. J Arthroplasty 2011;26(8):1501-1507.
- Kim DH, Spencer M, Davidson SM, Li L, et al. Institutional prescreening for detection and eradication of methicillin-resistant Staphylococcus aureus in patients undergoing elective orthopaedic surgery. J Bone Joint Surg Am 2010;92(9):1820-1826.
- Buehlmann M, Frei R, Fenner L, et al. Highly effective regimen for decolonization of methicillin-resistant Staphylococcus aureus carriers. Infect Control Hosp Epidemiol 2008;29(6):510-516.
- Zorrilla P, Salido JA, Lopez-Alonso A, Silva A. Serum zinc as a prognostic tool for wound healing in hip hemiarthroplasty. Clin Orthop Relat Res 2004;(420):304-308.
- Greene KA, Wilde AH, Stulberg BN. Preoperative nutritional status of total joint patients. Relationship to postoperative wound complications. J Arthroplasty 1991;6(4):321-325.
- Jensen JE, Jensen TG, Smith TK, et al. Nutrition in orthopaedic surgery. J Bone Joint Surg Am 1982;64(9):1263-1272.
- Marın LA, Salido JA, Lopez A, Silva A. Preoperative nutritional evaluation as a prognostic tool for wound healing. Acta Orthop Scand 2002;73(1):2-5.
- Ritter MA, Harty LD, Davis KE, et al. Predicting range of motion after total knee arthroplasty: clustering, log-linear regression, and regression tree analysis. J Bone Joint Surg Am 2003;85(7):1278-1285.
- Doyon F, Evrard J, Mazas F. [Evaluation of therapeutic trials published apropos of antibiotic prophylaxis in orthopedic surgery]. Rev Chir Orthop Reparatrice Appar Mot 1989;75(2):72-76.
- Dellinger EP, Gross PA, Barrett TL, et al. Quality standard for antimicrobial prophylaxis in surgical procedures. The Infectious Diseases Society of America. Infect Control Hosp Epidemiol 1994;15(3):182-188.
- Heath AF. Antimicrobial prophylaxis for arthroplasty and total joint replacement: discussion and review of published clinical trials. Pharmacotherapy 1991;11(2):157-163.
- Nelson CL. The prevention of infection in total joint replacement surgery. Rev Infect Dis 1987;9(3):613-618.
- Garvin KL, Konigsberg BS. Infection following total knee arthroplasty: prevention and management. J Bone Joint Surg Am 2011;93(12):1167-1175.
- Raghavan M, Marik PE. Anemia, allogenic blood transfusion, and immunomodulation in the critically ill. Chest 2005;127(1):295-307.
- Cram P, Lu X, Kaboli PJ, et al. Clinical characteristics and outcomes of Medicare patients undergoing total hip arthroplasty, 1991-2008. JAMA 2011;305(15):1560-1567.
- Rana AJ, Iorio R, Healy WL. Hospital economics of primary THA decreasing reimbursement and increasing cost, 1990 to 2008. Clin Orthop Relat Res 2011;469(2):355-361.
- Dennis DA, Komistek RD, Scuderi GR, Zingde S. Factors affecting flexion after total knee arthroplasty. Clin Orthop Relat Res 2007;464:53-60.
- Kotani A, Yonekura A, Bourne RB. Factors influencing range of motion after contemporary total knee arthroplasty. J Arthroplasty 2005;20(7):850-856.
- Brosseau L, Milne S, Wells G, et al. Continuous passive motion improves active knee flexion and shortens hospital stay but does not affect other functional outcomes after knee arthroplasty. J Bone Joint Surg Am 2005;87(11):2594.
- Kahn TL, Soheili AC, Schwarzkopf R. Poor WOMAC scores in contralateral knee negatively impact TKA outcomes: Data from the Osteoarthritis Initiative. J Arthroplasty 2014;29(8):1580-1585.
- Farquhar S, Snyder-Mackler L. The Chitranjan Ranawat award: the nonoperated knee predicts function 3 years after unilateral total knee arthroplasty. Clin Orthop Relat Res 2010;468(1):37-44.
- Zeni JA, Snyder-Mackler L. Early postoperative measures predict 1- and 2-year outcomes after unilateral total knee arthroplasty: importance of contralateral limb strength. Phys Ther 2010;90(1):43-54.