By Kirk McCullough, MD
By Kirk McCullough, MD
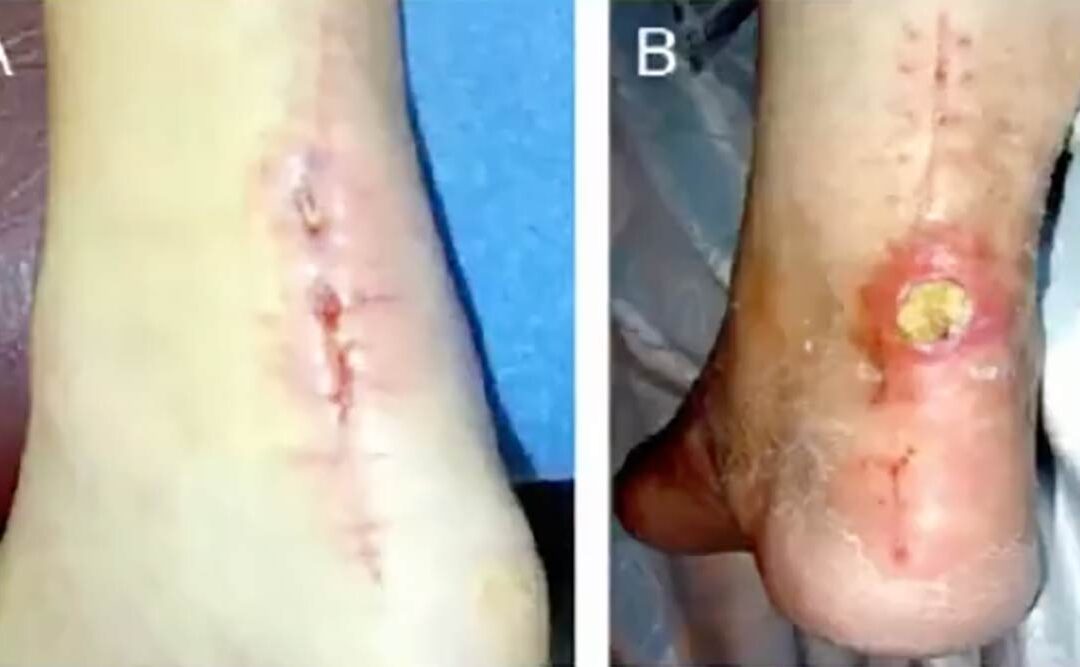
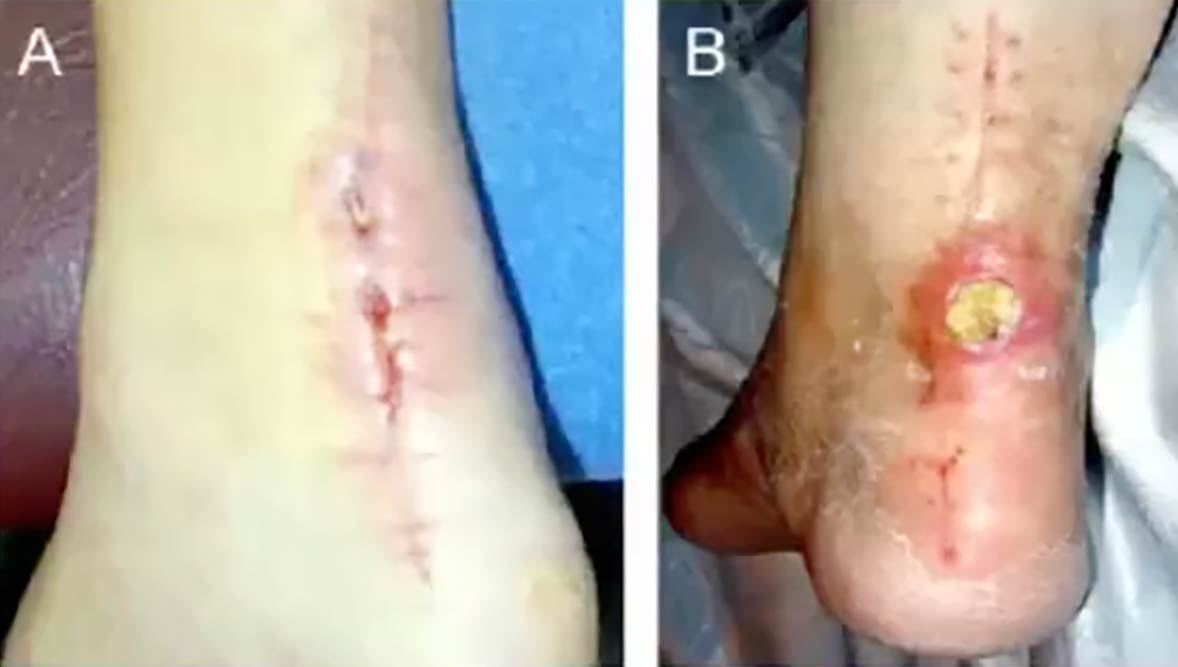
Achilles tendon ruptures are among the most devastating lower extremity injuries an athlete can face. Historically, the medical community has been divided between traditional open surgery and non-operative management. While open surgery effectively lowers the risk of re-rupture, the posterior ankle’s poor blood supply can sometimes lead to severe wound complications that can end careers. High-profile cases, such as NFL player Robert Mathis and MLB star Ryan Howard, highlight how wound-related issues—not the initial injury—can derail a professional trajectory. Conversely, non-operative treatment, though avoiding surgical wounds, carries a 10 times higher risk of re-rupture and often results in persistent calf muscle strength deficits that are still measurable 18 months post-injury.
The Paradigm Shift: Minimally Invasive “Mini-Open” Repair
To address these challenges, a minimally invasive approach has emerged as a superior middle ground. This technique utilizes a percutaneous Achilles repair system featuring an anatomic jig that allows surgeons to perform locked suture repairs through much smaller incisions.
A key advantage of this method is that the repair is performed deep to the paratenon, which minimizes soft tissue disruption and preserves the skin’s sensitive environment. This “mini-open” approach provides the strength of a traditional open repair while drastically reducing the risk of infection and wound dehiscence. Research into elite populations, specifically NFL players, showed a 100% return-to-play rate, with athletes returning to the field in an average of 5 and a half months. The general public sees similar success in published studies, with 98% of patients returning to their activities significantly faster than those treated with traditional open surgery.
 Technical Nuances: Adhesion Release and Specialized Suturing
Technical Nuances: Adhesion Release and Specialized Suturing
The effectiveness of this procedure often depends on tips and tricks gained from clinical experience. For example, in cases where the presentation is delayed, surgeons can use a traction stitch and a malleable instrument to free up adhesions between the tendon and the paratenon. This allows for the necessary excursion of the muscle-tendon unit proximally, ensuring a more functional repair even in complex, delayed-presentation cases.
Furthermore, surgeons must be meticulous about skin closure. Placing incisions transversely along the Langerhans lines helps the skin come together more naturally during flexion and extension, which creates less shear and promotes better healing. Closing the paratenon as a separate layer from the skin is another critical step in preventing long-term complications.
The “Golden Rule” of Tensioning: Fighting the 50% Elongation
Perhaps the most critical technical realization in modern Achilles repair is the management of tension. A common mistake is to tension the repaired tendon to match the uninjured side at the time of surgery. However, published studies emphasize that 50% of tendon elongation occurs within the first 3 months of recovery, regardless of the rehabilitation protocol used.
Because the tendon inevitably “stretches out” during the healing and early rehabilitation process, surgeons must overtension and excessively plantarflex the foot relative to the opposite limb during the repair. Failing to account for this elongation results in a permanent loss of power, which is considered a clinical complication in itself. By “over-tensioning” initially, surgeons ensure that once the stretching occurs, the patient is left with a muscle-tendon unit that provides optimal power and function.
Beyond Ruptures: Treating Chronic Tendinopathy
The advancements in Achilles care also extend to chronic conditions like insertional and non-insertional tendinopathy. When conservative treatments—such as shockwave therapy, night splints, and stretching—fail to provide relief, surgical debridement of “diseased tissue” may be required.
In these cases, surgeons are now utilizing flowable scaffolds to fill the gaps left by the removal of diseased tissue. This approach treats soft tissue defects much like a surgeon would treat a bone defect: by providing a scaffold that cells can bind to, modulating the healing process from acute inflammation toward regenerative healing rather than just allowing functional scar tissue to fill the void.
 Insertional Disease and the Suture Bridge Technique
Insertional Disease and the Suture Bridge Technique
For insertional issues, particularly calcific changes at the heel, the Suture Bridge technique offers a robust solution. This method creates a strong, knotless construct that often removes the need for an FHL (flexor hallucis longus) transfer, particularly in high-level athletes. It is important to note, however, that the recovery for insertional disease is typically much longer—often 2 and a half times the recovery time of an acute rupture.
A Better Standard of Care for Achilles Rupture
The traditional “long extensile” open repair is increasingly falling out of favor because its risks to the soft tissue are simply too high. By combining minimally invasive techniques with precise tensioning and advanced biological scaffolds, surgeons can achieve the best of both worlds: the structural integrity required for a full return to high-level athletics and the minimized risk of life-altering wound complications. As technology continues to evolve with insertional Achilles tendinopathy management toward arthroscopic and burr-assisted techniques, the focus remains clear: minimize disruption to maximize the body’s native healing potential.
Originally from Kansas City, Dr. McCullough spent his first 2 years of college as a cadet at the US Air Force Academy before completing his Bachelor of Arts degree in Biology from William Jewell College. Following graduation, he earned his medical degree from the University of Kansas School of Medicine in Kansas City. He then completed his residency in Orthopaedic surgery at Vanderbilt University Medical Center Center in Nashville, TN. Following residency, he completed a one-year fellowship in Orthopedic Sports Medicine and Shoulder Surgery at OrthoCarolina in Charlotte, NC, and then completed a second one-year fellowship in Orthopedic Foot and Ankle Surgery at the Cleveland Clinic Foundation in Ohio. Dr. McCullough has served on the NFL Foot/Ankle Committee, as a team physician for the Kansas City Chiefs, KC Ballet, Sporting KC (MLS), and the KC Current (NWSL). Outside of the region, he continues to serve the US Soccer Federation as a team physician for the USMNT and consultant for the USWNT and is the FIFA-appointed Venue Medical Director in Kansas City for the 2026 World Cup.
This article summarizes Dr. McCullough’s presentation, “Minimally Invasive Achilles Tendon Repair and Postop Rehabilitation: How Quick Can We Go,” delivered at the 2025 Lower Extremity Sports Injuries Event (October 25, 2025). To view the full presentation with audience questions and answers–and to see the complete agenda for the program–visit https://sportsmed.lerexpo.com/en/#agenda . Continuing education credits are available for this and many other lerEXPO programs.