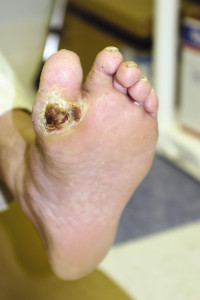
 Patients at risk for diabetic foot ulcers claim to follow practitioner instructions, but the recurrence rates speak for themselves. More favorable outcomes will require a better understanding of why patients don’t comply.
Patients at risk for diabetic foot ulcers claim to follow practitioner instructions, but the recurrence rates speak for themselves. More favorable outcomes will require a better understanding of why patients don’t comply.
By Ryan Crews, MS, CCRP
Diabetes wreaks havoc on a vast number of body systems. Unfortunately the legs and feet act as a retaining pool for a collection of many of these problems, including neurological, vascular and connective tissue maladies.1, 2 Previous work has estimated the lifetime incidence of diabetic foot ulcers to be as high as 25% in individuals with diabetes.3 Not wearing proper footwear is one of the most dangerous things an individual with diabetes can do in regards to their feet as it puts them at risk of developing a foot ulcer and subsequently at risk for amputation.
According to self report in the office, most patients are nearly 100% compliant with their caregiver’s directives, which should help prevent or limit the progression of these complications. And yet the complications persist. If compliance rates are really that high, then it must be just an odd fluke that the one day they happen to treat themselves to some cake and ice cream, miss a dose of insulin, or neglect to wear their prescriptive footwear was the day before their office visit. Sound familiar?
Diabetic foot ulcer formation
In order to appreciate the necessity of utilizing appropriate footwear, one must understand the etiology of the neuropathic diabetic foot ulcer. The lack of tactile sensation in the neuropathic foot effectively shuts down the body’s warning system when damage is being done to the foot. Without the capacity to feel trauma induced pain, repeated cycles of focal pressure (Figure 1) on the plantar surface of the foot result in the formation of diabetic foot ulcers without the individual ever feeling any discomfort.4
The sources of these repetitive traumas are often the ground reaction forces associated with weight bearing. During walking, ground reaction forces push and pull the soft tissue of the foot along the vertical, anteroposterior, and mediolateral axes at forces up to 1.5 times an individual’s body weight.5 During a typical step, these forces generally progress distally from a centralized location below the heel at touchdown until they reach the hallux at push-off.6 The stresses imparted to the feet by the ground reaction forces lead to inflammation and eventually autolysis of the soft tissue beneath bony prominences of the foot.4,7
Offloading
In the presence of sufficient vascular supply, the two primary tenets for healing diabetic foot ulcers are appropriate debridement of all necrotic tissue and pressure dispersion from the ulcer site (offloading).8 Offloading is accomplished by distributing loading forces across the plantar surface of the foot, thereby eliminating isolated pockets of excessive stress. A number of modalities have been developed for offloading the feet, including half shoes, healing sandals, Scotchcast boots, removable cast walkers (RCWs), and total contact casts (TCCs).9
The TCC is commonly recognized as the gold standard in healing ulcers. Although some RCWs have been demonstrated in the gait laboratory to be as effective as the TCC for offloading the foot,10,11 in a clinical trial Armstrong et al12 found the TCC was associated with higher healing rates and a shorter time to healing than an RCW. With similar capacities for offloading wounds, it was hypothesized that the non-removable TCC’s capacity to force compliance was responsible for the difference in healing.
Offloading compliance and ulcer outcomes

Figure 1. Peak pressure profile for a diabetic foot. A) 2-D depiction of plantar pressure B) 3-D depiction of plantar pressure (note the abnormal spikes along the lateral forefoot)
In order to test whether it was indeed the removable design feature of RCWs that was responsible for the divergence in healing, a trial incorporating forced compliance with an RCW was designed. In this study, the TCC was compared to an RCW that was rendered irremovable by means of a single layer of fiberglass casting material wrapped abound the walker.13 The irremovable RCW was coined an “instant total contact cast” (iTCC). Within 12 weeks of treatment, diabetic foot ulcers had healed in 80% of patients who used the iTCC, in comparison to 74% of patients who wore the TCC. Additional studies have supported the use of non-removable modalities for healing ulcers.14
In addition to treating ulcers, specialized footwear is commonly prescribed to prevent diabetic foot ulcers. Customized and prefabricated orthotics as well as shoes are routinely dispensed to high risk patients. Numerous studies have demonstrated these to be efficacious in offloading the foot.15-17 Additionally, some preliminary studies have shown prescriptive footwear to be effective in preventing ulcer recurrence.14 Chantelau and Haage18 reported in an observational study that individuals who self-reported use of their protective footwear for more than 60% of the day experienced recurrence rates that were more than 50% lower than patients who reported shorter wear times.
State of compliance
Despite the necessity of offloading the foot to allow for ulcer healing, compliance with footwear is far from optimal. An objective means of assessing off-loading compliance has been developed utilizing accelerometer based activity monitors.19 One activity monitor is attached at the subject’s waist per the device’s instructions, and a second monitor for which the internal clock is synchronized with the first monitor is placed (potentially hidden) on the offloader. Daily activity is identified according to the waist mounted monitor. Compliance is then assessed based on the extent to which the waist monitor and the offloader’s monitor recorded activity concurrently (Figure 2).
In an investigation of RCW compliance in individuals with diabetic foot ulcers, this methodology revealed that, on average, patients only wore the RCW during 28% of their total daily activities.20 The subjects did, however, exhibit increased steps per hour while wearing the device (93 vs 46). Anecdotally this makes sense. Patients commonly report to practitioners that they always wear their RCW when leaving the house (the time they are likely to have the highest step rate) but sometimes take it off at home. What this strategy fails to consider is that at home, the step rate may be low, but a large number of steps are accumulated over the course of a day. Poor compliance at home was previously demonstrated when Armstrong et al assessed physical activity in patients at high risk of ulceration.21 In this study, 85% of the patients reported they used their physician-approved shoes while outside the home and only 15% wore their shoes inside the home. As was the case with the RCW compliance, this resulted in subjects wearing their approved footwear during their most active period of the day (5.3 hours outside home), yet accumulating more total steps while walking about their homes without their shoes.
Additional studies have also shown compliance with preventative footwear to be quite poor. In studying prescribed diabetic footwear use in the U.K., Knowles and Boulton found that only 22% of their subjects wore their prescribed footwear all day long.22 This figure was based on face-to-face interviews conducted in the diabetic foot clinic; in truth, the percentage was likely even lower. Patients were likely to inflate their self-reported compliance for a number of reasons. In a face to face interview, patients were particularly likely to have been influenced by their desire to please the practitioner. Poor recall and failure to consider non-compliant steps within the home also may have inflated the self-reported compliance. This low compliance was in spite of the fact that 90% of the subjects felt their shoes helped their feet and 94% reported the shoes were comfortable. Means identified for improving compliance included: providing more style and color options, providing shoes suitable for indoor and outdoor use, and improving patient and clinician education on the importance of proper footwear.
A similar survey-based study in the United States had comparable findings, in that only 28% of patients reported that they wore their diabetic footwear more than 80% of the day.23 Appearance, comfort, and weight were the most common complaints about their shoes. Another noteworthy finding was patients that perceived their diabetic foot condition to be more severe than that of other patients with diabetic foot complications were not any more compliant with their footwear.
The neuropathic absence of pain likely makes it easy for patients to convince themselves that they are not significantly injuring their feet during intermittent times of non-compliance. Lack of education also contributes to non-compliant behavior. For example, many individuals consider calluses to be protective in nature. However, calluses on the feet actually result in increased pressure (similar to walking on any other hard object) and stress on the soft tissue below, thereby contributing to ulcer formation. Another misconception is the idea that carpeting in the home provides adequate protection to the feet. That, coupled with the idea that walking without appropriate footwear is permissible as long as it is only a short distance, is likely the reason compliance within the home is so poor.
Future of compliance
The lack of compliance with RCWs has led a number of companies to develop lockable versions of their devices. While this is likely to aid in the healing of diabetic foot ulcers, forced compliance for prevention is not a likely option. Enhanced and more effective education is needed to improve off-loading compliance. Individuals with diabetic neuropathy need to appreciate that each step they take without their protective footwear is hazardous. Unprotected steps may result in a new ulcer by allowing a foreign object to pierce the skin or by acting as the final cumulative stressor needed to form a break in the skin. For individuals with ulcers already present, a few unprotected steps can negate the day’s healing that occurred while the foot was off-loaded. While busy clinicians may not have the time to fully educate patients on the principles and necessity of off-loading, adequate means of education must be found. Both medical assistants and multi-media presentations may be able to improve patients’ knowledge.
Monitoring of compliance will continue to grow in popularity. In any clinical trial in which compliance is unaccounted for, there is a fair possibility that any potential therapeutic benefit of the test article/device will lack statistical significance due to non-compliant study subjects. The dual activity monitor method of measuring compliance is currently in use in a number of industry and grant funded investigations for which compliance will be considered a potential confounding variable. However, it is likely that in the future, currently available technologies such as Bluetooth communication will be utilized to develop more functional and user-friendly monitoring devices. These technologies could make it easy for caregivers to track patients’ offloading compliance. They could also be used to send alarm or reminder signals to patients via a watch or phone when the system identifies that the patient is walking without their offloading footwear, something that could be particularly helpful for elderly patients with dementia.
In summary
Off-loading is critical to the healing process of diabetic foot ulcers. Total contact casting typically results in healing of diabetic foot ulcers due to the forced compliance of pressure relief for the ulcer, however, the successful healing of ulcers with other off-loading modalities is dependent upon the patients’ adherence to the devices.24 Likewise, therapeutic shoes can only prevent diabetic foot ulcers if they are worn. At present patient compliance with offloading devices is very poor. Utilizing patient feedback in the design of offloaders and better educating patients will help improve compliance. Compliance monitoring is presently used on a relatively small scale typically in conjunction with clinical trials; however, in the future it is likely to become more widespread, with applications for both care providers and patients.
Ryan Crews, MS, CCRP, is a clinical research scientist and operations manager in Scholl College of Podiatric Medicine’s Center for Lower Extremity Ambulatory Research (CLEAR), at Rosalind Franklin University of Medicine and Science in Chicago, IL.
Figure 1. Peak pressure profile for a diabetic foot. A) 2-D depiction of plantar pressure B) 3-D depiction of plantar pressure (note the abnormal spikes along the lateral forefoot)
Figure 2. Compliance assessment via dual activity monitors.
References
1. Bennett PJ, Stocks AE, Whittam DJ. Analysis of risk factors for neuropathic foot ulceration in diabetes mellitus. J Am Podiatr Med Assoc 1996;86(3):112-116.
2. Frykberg RG, Zgonis T, Armstrong DG, et al. Diabetic foot disorders. A clinical practice guideline (2006 revision). J Foot Ankle Surg 2006;45(5 Suppl):S1-S66.
3. Singh N, Armstrong DG, Lipsky BA. Preventing foot ulcers in patients with diabetes. JAMA 2005;293(2):217-228.
4. Brand PW. The diabetic foot. In: Ellenberg M, Rifkin H, ed. Diabetes mellitus, theory and practice. 3rd ed. New York: Medical Examination Publishing; 1983:803-828.
5. Hamill J, Hardin, EC. Special topics in biomechanics. In: Kamen G, ed. Foundations of exercise science. Baltimore: Lippincott Williams & Wilkins; 2001:177-189.
6. van Deursen R. Mechanical loading and off-loading of the plantar surface of the diabetic foot. Clin Infect Dis 2004;39 Suppl 2:S87-S91.
7. Brand PW. The insensitive foot (including leprosy). In: Jahss M, ed. Disorders of the foot and ankle. 2nd ed. Philadelphia: Saunders; 1991:2170-2175.
8. Armstrong DG, Wu SC, Crews RT. Practical strategies for debridement, off-loading and healing the diabetic foot wound. In: Pearce WH MJ, Yao JST, ed. Trends in vascular surgery. Evanston, IL: Greenwood Academic; 2006:461-472.
9. Wu SC, Crews RT, Armstrong DG. The pivotal role of offloading in the management of neuropathic foot ulceration. Curr Diab Rep 2005;5(6):423-429.
10. Baumhauer JF, Wervey R, McWilliams J, et al. A comparison study of plantar foot pressure in a standardized shoe, total contact cast, and prefabricated pneumatic walking brace. Foot Ankle Int 1997;18(1):26-33.
11. Lavery LA, Vela SA, Lavery DC, Quebedeaux TL. Reducing dynamic foot pressures in high-risk diabetic subjects with foot ulcerations. A comparison of treatments. Diabetes Care 1996;19(8):818-821.
12. Armstrong DG, Nguyen HC, Lavery LA, et al. Off-loading the diabetic foot wound: a randomized clinical trial. Diabetes Care 2001;24(6):1019-1022.
13. Katz IA, Harlan A, Miranda-Palma B, et al. A randomized trial of two irremovable off-loading devices in the management of plantar neuropathic diabetic foot ulcers. Diabetes Care 2005;28(3):555-559.
14. Bus SA, Valk GD, van Deursen RW, et al. The effectiveness of footwear and offloading interventions to prevent and heal foot ulcers and reduce plantar pressure in diabetes: a systematic review. Diabetes Metab Res Rev 2008;24 Suppl 1:S162-S180.
15. Owings TM, Woerner JL, Frampton JD, et al. Custom therapeutic insoles based on both foot shape and plantar pressure measurement provide enhanced pressure relief. Diabetes Care 2008;31(5):839-844.
16. Tsung BY, Zhang M, Mak AF, Wong MW. Effectiveness of insoles on plantar pressure redistribution. J Rehabil Res Dev 2004;41(6A):767-774.
17. Schaff PS, Cavanagh PR. Shoes for the insensitive foot: the effect of a “rocker bottom” shoe modification on plantar pressure distribution. Foot Ankle 1990;11(3):129-140.
18. Chantelau E, Haage P. An audit of cushioned diabetic footwear: relation to patient compliance. Diabet Med 1994;11(1):114-116.
19. Crews RT, Armstrong DG, Boulton AJ. A method for assessing off-loading compliance. J Am Podiatr Med Assoc 2009;99(2):100-103.
20. Armstrong DG, Lavery LA, Kimbriel HR, et al. Activity patterns of patients with diabetic foot ulceration: patients with active ulceration may not adhere to a standard pressure off-loading regimen. Diabetes Care 2003;26(9):2595-2597.
21. Armstrong DG, Abu-Rumman PL, Nixon BP, Boulton AJ. Continuous activity monitoring in persons at high risk for diabetes-related lower-extremity amputation. J Am Podiatr Med Assoc 2001;91(9):451-455.
22. Knowles EA, Boulton AJ. Do people with diabetes wear their prescribed footwear? Diabet Med 1996;13(12):1064-1068.
23. Macfarlane DJ, Jensen JL. Factors in diabetic footwear compliance. J Am Podiatr Med Assoc 2003;93(6):485-491.
24. Rathur HM, Boulton AJ. The neuropathic diabetic foot. Nat Clin Pract Endocrinol Metab 2007;3(1):14-25.









Trackbacks/Pingbacks