istockphoto.com #14464226
Ankle joint laxity can be a complicating factor in patients with acute ankle sprains or chronic instability, and testing for excessive laxity can help practitioners choose an appropriate method of treatment. However, not all tests for ankle joint laxity are created equal.
By Theodore Croy, PhD, PT, OCS, and Jay Hertel, PhD, ATC, FNATA
Clinicians who treat lateral ankle sprains seek to establish and characterize, either qualitatively or quantitatively, any abnormal increase in the amount of ankle joint laxity. Lateral ankle sprain injuries occur when an individual suffers a forced plantar flexion and inversion injury of the ankle; the combined motion may stretch or tear the lateral ankle ligaments. The acute injury results in pain, swelling, and impaired gait and may lead to recurrent injury and symptoms of instability known as “giving way.”
Rationale for clinical assessment of laxity
Both the musculoskeletal practitioner and patient need to understand the severity of ankle laxity to establish a clear diagnosis and prognosis for recovery. Ligament injuries to peripheral joints (including the shoulder and knee as well as the ankle) are known to result in pathological laxity, a condition that may result in further instability and cartilage and bony damage. In addition, chronic ankle laxity and instability have been associated with the onset of posttraumatic ankle osteoarthritis.1 Impaired ankle joint integrity due to ligament damage of the anterior talofibular ligament (ATFL) or calcaneofibular ligament (CFL) can contribute to the syndrome of chronic ankle instability (CAI), which is characterized by joint arthrokinematic changes, proprioceptive and balance deficits, and reductions in self-reported function acutely and over the lifespan of the individual.2
In the case of an acute ankle sprain, clinicians can decide whether a patient may benefit from immobilization or external joint support.3 Protection of the joint from further injury is important in the first six weeks to one year.4 Early functional movement and rehabilitation are also important within the context of healing ligaments, and clinicians may even consider some patients for surgical reconstruction.5
In cases in which CAI is apparent and ankle sprain recurrence is an issue, both mechanical support and rehabilitation for functional impairments are important.6 Balance retraining and restoration of neuromuscular control are key facets of rehabilitation as these impairments play a role in injury recurrence whereas the ligaments act as restraints to end range of motion.7 Functional rehabilitation plans for individuals both with and without ankle laxity treat neuromuscular impairments rather than mechanical joint stability.
Patients with CAI may demonstrate negative or positive clinical ankle laxity tests and clinicians can base treatment decisions on those results. A patient with negative clinical laxity tests may undergo functional ankle rehabilitation and be encouraged to use an ankle support orthosis for protection, whereas a patient with positive tests may also be considered for reconstructive surgery.
Assessment of lateral ankle ligaments
Clinicians test the ankle ligaments by manually applying stress to the ATFL and CFL. The anterior drawer test8 is performed by manually applying an anteriorly directed force at the calcaneus while stabilizing the leg. This test is based on the assumption that the subtalar joint is stable and that the talus and calcaneus move as a unit as the rearfoot is displaced from the tibiofibular mortise. The talar tilt test9 is performed as the clinician passively inverts the rearfoot in relation to the mortise. Excessive motion, or pathologic laxity, on either test may suggest ligament injury requiring further rehabilitation or even surgery.
Positive findings on the anterior drawer or the talar tilt test may alter the clinician’s decision-making process. The clinician will likely suggest potential treatments to the patient—usually rehabilitation, surgery, or both. However, the diagnostic accuracies of the anterior drawer test and talar tilt test have been shown to be problematic. Kerkoffs et al10 demonstrated that clinically important anterior talocrural laxity may be as little as 2.3 mm, a finding that may be difficult to discern using either of the manual tests. Other authors agreed that the anterior drawer and talar tilt tests are problematic with reports of poor intertester reliability in ankles with and without ligament injuries and small changes in anterior laxity after ATFL injury.9 Lahde et al6 found that 28% of ATFL tears and 38% of combined ATFL and CFL tears were not detected using the anterior drawer test; these are findings that should make clinicians pause when interpreting these manual test results.
Instrumented methods
Several studies in the past decade have attempted to quantify talocrural and subtalar joint motion using ankle arthrometers, devices designed to measure joint motion and provide a nonradiographic method of evaluating ankle laxity with more diagnostic accuracy than manual methods.11-15 Ankle arthrometry can quantify increases in anterior and inversion talocrural laxity. However, despite these capabilities, most of these devices are specifically designed for research applications and not widely used in clinical settings, where patients are evaluated and treated. For clinicians to utilize ankle laxity testing to drive treatment decisions, devices and methods must be available, affordable, and provide accurate diagnostic information to the treating clinician.
Imaging and surgical evaluation
Graded stress radiography has been used in evaluation of ankle instability and has shown clinical utility in identification of joint injuries; it can also aid in clinical decisions regarding immobilization, rehabilitation, or surgery to repair or reconstruct injured ligaments.16,17 Using radiography, tibiotalar displacement is measured bilaterally during an anterior drawer stress and talar inversion test; an increase in displacement on the affected side may correlate with an increase in the severity of ligament injury. An anterior tibiotalar displacement of 3 mm relative to the uninvolved side or an increase in the tibiotalar angle is usually accepted as a sign of anterior talocrural instability.17 However, this test can be difficult to perform in the acute phase of injury due to patient discomfort and can expose the patient to unnecessary radiation.
Hubbard et al18 also utilized stress radiography and ankle arthrometry in individuals reporting unilateral functional ankle instability (FAI). The null hypothesis was that individuals with FAI who do not demonstrate mechanical laxity would not demonstrate mechanical laxity using arthrometry and stress radiography. When measured with arthrometry or stress radiography, the researchers observed significantly greater anteroposterior tibiotalar displacement in ankles with FAI than in uninvolved ankles. This suggests that “functional ankle instability” may include subclinical laxity that is not detected using manual stress examination techniques.
Investigators have used stress radiography to determine the need for surgical treatments well as a method of assessing surgical outcomes.19 In an interesting case series of 14 individuals with FAI, Takao et al conducted stress radiography and magnetic resonance imaging (MRI) before and two years after ligament reconstruction. Reductions in anterior and talar tilt laxity were observed at two-year follow up. Stress radiography alone, however, may not be sufficient to identify ankle instability as it is not capable of identifying both ligament status and talar motion.20 In a systematic review, stress radiography was not reliable enough to diagnose ankle instability in six of seven studies of acute ankle instability and one study of chronic ankle instability.21
MRI of the ankle provides a standardized protocol for imaging ankle joint anatomy. Kirby et al22 report that lateral ankle injuries can result in a constellation of injuries, including ATFL avulsions, fibrotic scar tissue in the lateral gutter, talar dome lesions, retinacular tears, CFL tears, and other injuries that are readily assessed with a comprehensive exam such as an MRI. Clinicians can use MRI to evaluate stretching of the ATFL (grade 1 using the O’Donoghue classification23), partial tears (grade 2) and complete ruptures (grade 3). A normal ATFL appears as a thin band from the lateral malleolus to the talar neck and failure to visualize this structure, the presence of fluid in the lateral gutter, or both may suggest a tear of the ATFL.
Researchers have attempted in vivo assessment of ankle ligament changes during motion using newer methods such as computed tomography reconstruction and MRI modeling. De Asla et al23 evaluated four healthy ankles from two men using computerized reconstruction of the ankle joint complex with dual orthogonal fluoroscopy and MRI. These authors measured the apparent ATFL length between the centroids of origin and insertion of the ATFL on the fibula and the talus. Their results indicated a nonsignificant increase in apparent ATFL length from 16.3 ± 3.0 mm in neutral to 20.8 ± 2.7 mm in full plantar flexion and inversion, a 28% increase in length. Gould et al24 indicated that any ATFL elongated by more than 4 mm, approximately 20% of its length, would result in failure of the ligament. These biomechanical factors have guided development of autograft surgical reconstruction constructs to mimic the ATFL, and the elongation to failure of these constructs ranges from 19% to 33%.25
Caputo et al26 used similar ankle joint complex reconstructive techniques to evaluate the kinematics of the ankle joint in nine individuals with unilateral ATFL deficiency while they performed a step-down task. The researchers observed significant increases in anterior talar translation of 0.9 ± 0.5 mm and an increase of 5.7 ± 3.6° of internal talar rotation in the ATFL-deficient ankle compared with the uninvolved ankle. The advantage of MRI is that a comprehensive examination in multiple planes and echo sequences can be performed, however, MRI cannot depict the ATFL during movement, like fluoroscopy or ultrasound, or assess the contralateral side. MRI also requires a physician referral to a radiology center.
Hintermann et al27 reported findings of arthroscopic examination of ankle laxity in 148 ankles with a history of ankle injury; 69% of study participants were asymptomatic and 31% had chronic pain and symptoms of giving way. Hintermann and colleagues categorized ankles as “moderately unstable” if the talus could be translated via anterior drawer a distance of 5 mm out of the ankle mortise (allowing for passage of the 5-mm arthroscope into the lateral tibiotalar space), but not more than 5 mm. If the talus translated more than 5 mm, allowing for easy passage out of the mortise and a free view of the posterior aspect of the ankle, it was considered “severely unstable.” These investigators found that 86% of ankles demonstrated a ruptured (64%) or elongated ATFL (22%); in addition, they observed cartilage damage in 66% of all ankles that also demonstrated ligament injuries. These measurements taken during anesthetized conditions ought to give a frame of reference for measurements of anterior instability taken during normal clinical conditions.
Ultrasound imaging
Recent advances in ultrasound imaging and techniques have allowed researchers to use this imaging technique at the ankle. Campbell described dynamic ultrasound imaging as a means of detecting ATFL injury using qualitative appearances of the ligament.28 Mei-Dan et al29 described ultrasound methods combined with ankle motion to quantitatively identify syndesmosis injuries.
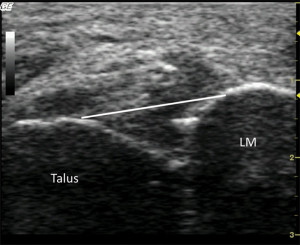
More recently, Croy et al30,31 also used ultrasound imaging combined with ankle joint stress tests (stress ultrasonography) to reliably identify laxity changes of the talocrural joint in ankle sprain copers and patients with chronic ankle instability, as well as uninjured controls. ATFL elongation due to anterior drawer and inversion stress was 15% to 25% in CAI patients and significantly greater than uninjured controls. Anterior talar translation of 2.3 mm to 2.8 mm with anterior drawer force was observed in copers and CAI patients, but only 0.2 mm in uninjured controls when translation was measured directly over the origin and insertion of the ATFL. Thus, the increase in talocrural laxity is large in magnitude, but small enough to make it difficult to differentiate from normal talocrural laxity present using manual anterior drawer testing. Further work into the diagnostic accuracy of these methods is ongoing.
Ultrasound affords a real-time evaluation of the site of injury and is tolerated well by patients with both acute and chronic injuries. This type of modality has been described as being “operator dependent,” and unfamiliarity with the capabilities and techniques is one of the main limiting factors precluding its usage in the foot and ankle. Ultrasound is a rapid examination that can be performed inexpensively and does not expose the patient to ionizing radiation as in standard or stress radiographs or during fluoroscopy.
The added benefits of imaging, with and without stress applied, as well as the ability to measure changes between bony landmarks, could potentially help clinicians understand the laxity that results from injury. Moreover, this method allows for bilateral analysis, repeated imaging sessions, and visualization of the ligaments from origin to insertion.25 These characteristics and early positive results in ankle injury patients suggest that the use of ultrasound to determine talocrural movement is promising, but further work must be done to continue to improve upon these methods.
Conclusion
In summary, clinicians and researchers have used manual tests, arthrometric devices, imaging, and arthroscopic methods, as well as combinations of imaging and arthrometric methods, to better understand the pathologic laxity resulting from lateral ankle sprains. This injury is so prevalent that diagnostic tests must be available, affordable, reliable, safe, and accurate for the quantification of the injury severity. When musculoskeletal practitioners can employ ankle laxity tests with these characteristics, our ability to treat lateral ankle sprains will continue to improve.
Theodore Croy, PhD, PT, OCS, is an assistant professor at the US Army-Baylor University Doctoral Program in Physical Therapy at Fort Sam Houston, TX. Jay Hertel, PhD, ATC, FNATA, is a Joe Gieck Professor of Sports Medicine in the Curry School of Education at the University of Virginia in Charlottesville.
1. Valderrabano V, Hintermann B, Horisberger M, Fung TS. Ligamentous posttraumatic ankle osteoarthritis. Am J Sports Med 2006;34(4):612-620.
2. Hertel J. Functional anatomy, pathomechanics, and pathophysiology of lateral ankle instability. J Athl Train 2002;37(4):364-375.
3. Cooke MW, Marsh JL, Clark M, et al. Treatment of severe ankle sprain: a pragmatic randomised controlled trial comparing the clinical effectiveness and cost-effectiveness of three types of mechanical ankle support with tubular bandage. The CAST trial. Health Technol Assess 2009;13(13):iii, ix-x, 1-121.
4. Hubbard TJ, Cordova M. Mechanical instability after an acute lateral ankle sprain. Arch Phys Med Rehabil 2009;90(7):1142-1146.
5. Kerkhoffs GM, Handoll HH, de Bie R, et al. Surgical versus conservative treatment for acute injuries of the lateral ligament complex of the ankle in adults. Cochrane Database Systematic Rev 2007;(2):CD000380.
6. Hubbard TJ, Kramer LC, Denegar CR, Hertel J. Contributing factors to chronic ankle instability. Foot Ankle Int 2007;28(3):343-354.
7. Hiller CE, Kilbreath SL, Refshauge KM. Chronic ankle instability: evolution of the model. J Athl Train 2011;46(2):133-141.
8. Frost HM, Hanson CA. Technique for testing the drawer sign in the ankle. Clin Orthop Relat Res 1977(123):49-51.
9. Fujii T, Luo ZP, Kitaoka HB, An KN. The manual stress test may not be sufficient to differentiate ankle ligament injuries. Clin Biomech 2000;15(8):619-623.
10. Kerkhoffs GM, Blankevoort L, van Poll D, et al. Anterior lateral ankle ligament damage and anterior talocrural-joint laxity: an overview of the in vitro reports in literature. Clin Biomech 2001;16(8):635-643.
11. Kovaleski JE, Hollis J, Heitman RJ, et al. Assessment of ankle-subtalar-joint-complex laxity using an instrumented ankle arthrometer: an experimental cadaveric investigation. J Athl Train 2002;37(4):467-474.
12. Kovaleski JE, Gurchiek LR, Heitman RJ, et al. Instrumented measurement of anteroposterior and inversion-eversion laxity of the normal ankle joint complex. Foot Ankle Int 1999;20(12):808-814.
13. Liu W, Siegler S, Techner L. Quantitative measurement of ankle passive flexibility using an arthrometer on sprained ankles. Clin Biomech 2001;16(3):237-244.
14. Kerkhoffs GM, Blankevoort L, van Dijk CN. A measurement device for anterior laxity of the ankle joint complex. Clin Biomech 2005;20(2):218-222.
15. Nauck T, Lohrer H, Gollhofer A. Evaluation of arthrometer for ankle instability: a cadaveric study. Foot Ankle Int 2010;31(7):612-618.
16. van Dijk CN, Mol BW, Lim LS, et al. Diagnosis of ligament rupture of the ankle joint. Physical examination, arthrography, stress radiography and sonography compared in 160 patients after inversion trauma. Acta Orthop Scand 1996;67(6):566-570.
17. Oae K, Takao M, Uchio Y, Ochi M. Evaluation of anterior talofibular ligament injury with stress radiography, ultrasonography and MR imaging. Skeletal Radiol 2009;39(1):41-47.
18. Hubbard TJ, Kaminski TW, Vander Griend RA, Kovaleski JE. Quantitative assessment of mechanical laxity in the functionally unstable ankle. Med Sci Sports Exerc 2004;36(5):760-766.
19. Takao M, Innami K, Matsushita T, et al. Arthroscopic and magnetic resonance image appearance and reconstruction of the anterior talofibular ligament in cases of apparent functional ankle instability. Am J Sports Med 2008;36(8):1542-1547.
20. Hashimoto T, Inokuchi S, Kokubo T. Clinical study of chronic lateral ankle instability: injured ligaments compared with stress X-ray examination. J Orthop Sci 2009;14(6):699-703.
21. Frost SC, Amendola A. Is stress radiography necessary in the diagnosis of acute or chronic ankle instability? Clin J Sport Med 1999;9(1):40-45.
22. Kirby AB, Beall DP, Murphy MP, et al. Magnetic resonance imaging findings of chronic lateral ankle instability. Curr Probl Diagn Radiol 2005;34(5):196-203.
23. de Asla RJ, Kozánek M, Wan L, et al. Function of anterior talofibular and calcaneofibular ligaments during in-vivo motion of the ankle joint complex. J Orthop Surg Res 2009;4(7):1-6.
24. Gould N, Seligson D, Gassman J. Early and late repair of lateral ligament of the ankle. Foot Ankle 1980;1(2):84-89.
25. Jeys L, Korrosis S, Stewart T, Harris NJ. Bone anchors or interference screws?: A biomechanical evaluation for autograft ankle stabilization. Am J Sports Med 2004;32(7):1651-1659.
26. Caputo AM, Lee JY, Spritzer CE, et al. In vivo kinematics of the tibiotalar joint after lateral ankle instability. Am J Sports Med 2009;37(11):2241-2248.
27. Hintermann B, Boss A, Schäfer D. Arthroscopic findings in patients with chronic ankle instability. Am J Sports Med 2002;30(3):402-409.
28. Campbell DG, Menz A, Isaacs J. Dynamic ankle ultrasonography: a new imaging technique for acute ankle ligament injuries. Am J Sports Med 1994;22(6):855-858.
29. Mei-Dan O, Kots E, Barchilon V, et al. A dynamic ultrasound examination for the diagnosis of ankle syndesmotic injury in professional athletes: a preliminary study. Am J Sports Med 2009;37(5):1009-1016.
30. Croy T, Saliba SA, Saliba E, et al. Differences in lateral ankle laxity measured via stress ultrasonography in individuals with chronic ankle instability, ankle sprain copers, and healthy individuals. J Orthop Sports Phys Ther 2012;42(7):593-600.
31. Sisson L, Croy T, Saliba S, Hertel J. Comparison of ankle arthrometry and stress ultrasound imaging in the assessment of ankle laxity in healthy adults. Int J Sports Phys Ther 2011;6(4):297-305.