Balance intervention programs improve postural stability, which reduces ankle sprain risk. By reducing injury recurrence, balance training reduces the risk of chronic ankle instability, and in turn the risk of ankle osteoarthritis.
by Erik A. Wikstrom, PhD, ATC, and Mitchell L. Cordova, PhD, ATC
Lateral ankle sprains are generally caused by forces acting on the ankle/foot complex whereby sudden foot inversion is coupled with ankle plantar flexion,1 causing the maximum load to failure of the anterior talofibular and calcaneofibular ligaments to be exceeded.1 In addition to being the most common injury suffered by both high school and collegiate athletes,2, 3 lateral ankle sprains are also extremely common in military training and various occupational settings.4,5 Indeed, it is estimated that between 23,000 and 27,000 lateral ankle sprains occur daily in the United States alone.6,7 However, as many as 55% of individuals suffering a lateral ankle sprain may not seek treatment from a healthcare professional;8 thus, the actual incidence of ankle injuries could be vastly underestimated.
As the epidemiological data clearly indicate, lateral ankle sprains are a major healthcare issue and continue to represent a financial burden on the healthcare system. Unfortunately, lateral ankle sprains are often erroneously believed to be minor and inconsequential when the reality is that the recurrence rate is greater than 70%;9 moreover, the sequela associated with the lateral ankle sprain, commonly referred to as chronic ankle instability (CAI), has been shown to occur in up to 75% of individuals in an athletic population who sprain an ankle.9 CAI is characterized by residual symptoms,10 recurrent injury,11 and decreased physical activity.12 More importantly, the development of CAI compromises the articular surface of the talus13 and recently has been identified as a leading cause of post-traumatic ankle osteoarthritis.14
Sensorimotor function after lateral ankle injury
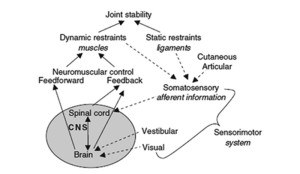
Unfortunately, the mechanisms underlying CAI are not completely understood, but it is becoming more apparent that the cause is due to alterations in the sensorimotor system.15,16 The sensorimotor system maintains joint stability through a complex integration of afferent information within the central nervous system, which emanates from the static (ligaments, skin) and dynamic (muscles) restraints and ultimately determines the neural drive for the muscles that stabilize the joint (Figure 1). Optimization of the sensorimotor system is therefore dependent on the success of feedback (reflex pathways that continuously adjust to coordinate muscle activity) and feed-forward (pre-programmed muscle activation patterns based on previous experience) neuromuscular control.17
Impairments in peripheral sensory feedback have long been proposed as the principal mechanism of CAI;18,19 however, recent research has indicated that centrally mediated changes in sensorimotor function are present following acute lateral ankle sprains and the development of CAI.20,21 For example, bilateral balance impairments (involved and uninvolved limb) are present during a single-leg stance in patients with acute lateral ankle sprains. Additionally, bilateral alterations have been reported at proximal joints in patients with acute lateral ankle sprains22,23 and with CAI.24,25 Both bilateral and proximal impairments suggest centrally mediated changes to motor control patterns (i.e. feed-forward neuromuscular control) have occurred. These changes would affect the way that these individuals move and the loads placed on the ankle joint. Specifically, recent research has demonstrated that subjects with CAI have a decreased ability to modulate presynaptic inhibition of the soleus in a single-leg stance and demonstrate higher levels of postsynaptic inhibition (indicative of a more depressed motor neuron pool) when compared to healthy subjects.16,21 These findings suggest that both sudden environmental changes (presynaptic inhibition) and longer lasting modulation (postsynaptic inhibition) of motor neuron output are altered in those who suffer from CAI. Furthermore, these data are beginning to provide evidence that not only does CAI negatively influence traditional measures of sensorimotor function (e.g. static and dynamic balance, peroneus longus reflex response), but also that a central mechanism does exist which modifies spinal reflexes in controlling joint function. It is also believed that descending supraspinal control of spinal reflexes may also be altered with CAI,15 however this has yet to be shown empirically.
Clinically, these findings strongly suggest that: 1) lateral ankle sprains are not an innocuous injury, and 2) lateral ankle sprains should be treated as a global and not a local injury. Indeed, the presence of alterations in the modulation of spinal reflexes and deficits in sensorimotor function clearly indicate that previously established rehabilitation protocols, which focused exclusively on the ankle joint, are insufficient for restoring proper neuromuscular control and preventing recurrent injury. Therefore, global coordination/balance training programs have been recommended for both the involved and uninvolved limbs of patients suffering from acute lateral ankle sprains and CAI.26,27 Balance training is often recommended and a common component of rehabilitation programs because impaired postural control is associated with an increased risk of ankle injury28,29 and has been shown to be impaired in subjects with acute lateral ankle sprains,30,31 CAI,30,32,33 and post-traumatic ankle osteoarthritis.34 But is balance training effective?
Balance training interventions for lateral ankle injury
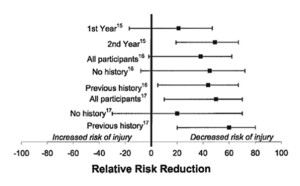
In short, the answer is yes. Balance training is effective! A recent meta-analysis by Wikstrom et al30 indicated that balance scores improved in patients who had sustained an acute lateral ankle sprain and in those who suffered from CAI. Not only is balance training effective in improving various balance measures in acute ankle sprains and in those who suffer from CAI, but balance training has been shown to reduce the risk of sustaining a lateral ankle sprain.26,35,36 Specifically, these preventive effects (Figure 2) are most apparent for individuals with a history of lateral ankle sprains (60% reduction of risk) and in individuals who have completed two consecutive years of balance training (49% reduction of risk).37 Thus, it appears that improving balance may be the primary mechanism for reducing recurrent ankle injuries after the completion of a balance-training program.
Although balance training is quite effective, what still remains unknown is the exact dosage necessary during rehabilitation programs that will yield optimal recovery of postural control and, more importantly, induce a reduction in the incidence of recurrent injuries.37 For example, just three days of balance training after an acute lateral ankle sprain resulted in postural control improvements.38,39 On the other hand, some investigations have demonstrated that subjects with CAI did not develop postural control improvements until after four40 or six41 weeks of global coordination/balance training. More importantly, Bahr et al26 reported that the longer a balance training program is implemented, the greater the preventive effects accrued from the program (Figure 2). Thus, the rapid improvements observed after acute ankle injury38,39 are extremely exciting, but it remains unclear how much of the improvement was due to the natural course of recovery following lateral ankle sprains. Evans et al42 indicated that the complete resolution of postural impairments did not occur until at least four weeks after injury; therefore, an early (albeit incomplete) improvement may be responsible for the significant improvements reported after just three days of balance training.38,39 It should also be noted that most of the existing balance training investigations utilized prospective, cohort designs where the baseline measures reported represent postural control deficits that existed prior to the intervention and not pre-injury postural control values. Although we can say with a large degree of confidence that balance training improves overall balance and postural control, it is not clear if these intervention programs restore postural control to pre-injury balance values.
While balance training is effective in restoring postural control following acute lateral ankle sprains and CAI, recent investigations have identified several adjunctive treatments/constructs that may optimize balance training. Two of the more interesting approaches include stochastic resonance and the direction of a patient’s attention. Stochastic resonance (SR) is a form of stimulation that is thought to enhance the effectiveness of traditional balance training protocols by subjecting the nervous system to low levels of sub-sensory or mechanical noise, to enhance the detection of sensorimotor signals related to postural control.43-46 There is also some evidence that indicates SR enhances monosynaptic stretch reflex responses generated by muscle spindles.47 Thus, SR stimulation functions to enhance the sensitivity of afferent input, which then positively affects efferent neural drive and ultimately joint system function, both of which are critical for the maintenance of upright postural control. Stochastic resonance stimulation therapy has been useful for improving postural stability in healthy young and elderly individuals when compared to postural stability tests without stimulation.43-46 Further, balance/coordination training combined with SR stimulation has been reported to improve both static and dynamic postural stability earlier and with greater efficacy than balance coordination training alone in both stable and unstable ankles.48,49
The direction of a patient’s attention has also gained a great deal of consideration, primarily in the field of motor control, in an effort to optimize the learning of new motor skills. During balance training programs, especially when working with a patient who has never completed a balance training program, many clinicians will instruct the patient to “stand as still as possible.” This commonly used technique directs the patient’s attention towards themselves or emphasizes an internal attentional focus (IAF). However, research on uninjured subjects indicates that motor skills, including balance, may be learned more effectively if an individual’s focus is directed outside their body [i.e., an external attentional focus (EAF)] or on the effect of their movement.50-52 Similar findings were reported in patients with acute lateral ankle sprains38,39 where EAF facilitated greater acquisition, retention, and transfer of postural control skills than an IAF technique after just three days of balance training. To date, no published investigations have compared the effects of an IAF program to that of an EAF program in subjects with CAI. Researchers hypothesize that an EAF facilitates more efficient movement patterns during a variety of motor skills by allowing the sensorimotor system to self-organize and become a more automated process.51 Furthermore, instructions directing a patient’s focus towards themselves may actually degrade the execution of automated skills (e.g., balance) compared to when no instructions are given.53
Clinical recommendations
Researchers and clinicians may never know the “best” parameters for a balance training intervention program. The exact dosage, type of exercise, and level of intensity needed to improve various indices of postural control and reduce recurrent injury are most likely multi-factorial in nature and influenced by injury severity, concomitant injuries, demands of the activity/sport and position played, experience with balance training, motor ability levels, and physical conditioning. Although this may be concerning, given the ongoing paradigm shift towards evidenced-based practice, current research indicates that balance training intervention programs are effective, regardless of the specific parameters employed. Further, research suggests that the longer a patient is enrolled in a balance training program, the greater the effects regardless of the parameters.
Patients with a history of lateral ankle sprains should complete a balance/coordination intervention program for three evidence-based reasons. First, balance training improves postural control, a measure associated with an increased risk of sustaining a lateral ankle sprain.28,29,35 Second, balance training reduces the recurrence of ankle injuries,35,54-56 which is the primary symptom of CAI. And, finally, reducing the occurrence of CAI ultimately reduces the incidence of post-traumatic ankle osteoarthritis.14
Erik A. Wikstrom, PhD, ATC, is an assistant professor, and Mitchell L. Cordova, PhD, ATC, is professor and chairperson, in the Biodynamics Research Laboratory, Department of Kinesiology; and Center for Biomedical Engineering Systems at the University of North Carolina at Charlotte, Charlotte, NC.
References
1. Fallat L, Grimm DJ, Saracco JA. Sprained ankle syndrome: prevalence and analysis of 639 acute injuries. J Foot Ankle Surg 1998;37(4):280-285.
2. Fernandez WG, Yard EE, Comstock RD. Epidemiology of lower extremity injuries among U.S. high school athletes. Acad Emerg Med 2007;14(7):641-645.
3. Hootman JM, Dick R, Agel J. Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives. J Athl Train 2007;42(2):311-319.
4. Grimm DJ, Fallat L. Injuries of the foot and ankle in occupational medicine: a 1-year study. J Foot Ankle Surg 1999;38(2):102-108.
5. McGaughey I, Sullivan P. The epidemiology of knee and ankle injuries on Macquarie Island. Injury 2003;34(11):842-846.
6. Baumhauer JM, Alosa DM, Renstrom AF, et al. A prospective study of ankle injury risk factors. Am J Sports Med 1995;23(5):564-570.
7. Kannus P, Renstrom P. Treatment for acute tears of the lateral ligaments of the ankle. Operation, cast, or early controlled mobilization. J Bone Joint Surg Am 1991;73(2):305-312.
8. McKay GD, Goldie PA, Payne WR, Oakes BW. Ankle injuries in basketball: injury rate and risk factors. Br J Sports Med 2001;35(2):103-108.
9. Gerber JP, Williams GN, Scoville CR, et al. Persistent disability associated with ankle sprains: a prospective examination of an athletic population. Foot Ankle Int 1998;19(10):653-660.
10. Anandacoomarasamy A, Barnsley L. Long term outcomes of inversion ankle injuries. Br J Sports Med 2005;39(3):e14.
11. Yeung MS, Chan KM, So CH, Yuan WY. An epidemiological survey on ankle sprain. Br J Sports Med 1994;28(2):112-116.
12. Verhagen RA, de Keizer G, Van Dijk CN. Long-term follow-up of inversion trauma of the ankle. Arch Orthop Trauma Surg 1995;114(2):92-96.
13. Marsh JL, Buckwalter J, Gelberman R, et al. Articular fractures: does an anatomic reduction really change the result? J Bone Joint Surg Am 2002;84(7):1259-1271.
14. Valderrabano V, Hintermann B, Horisberger M, Fung TS. Ligamentous posttraumatic ankle osteoarthritis. Am J Sports Med 2006;34(4):612-620.
15. Hertel J. Sensorimotor deficits with ankle sprains and chronic ankle instability. Clin Sports Med 2008;27(3):353-370.
16. Sefton JM, Hicks-Little CA, Hubbard TJ, et al. Sensorimotor function as a predictor of chronic ankle instability. Clin Biomech 2009;24(5):451-458.
17. Riemann BL, Lephart SM. The sensorimotor system, part I: The physiologic basis of functional joint stability. J Athl Train 2002;37(1):71-79.
18. Freeman MA. Instability of the foot after injuries to the lateral ligament of the ankle. J Bone Joint Surg Br 1965;47(4):669-677.
19. Freeman MA, Dean MR, Hanham IW. The etiology and prevention of functional instability of the foot. J Bone Joint Surg Br 1965;47(4):678-685.
20. McVey ED, Palmieri RM, Docherty CL, et al. Arthrogenic muscle inhibition in the leg muscles of subjects exhibiting functional ankle instability. Foot Ankle Int 2005;26(12):1055-1061.
21. Sefton JM, Hicks-Little CA, Hubbard TJ, et al. Segmental spinal reflex adaptations associated with chronic ankle instability. Arch Phys Med Rehabil 2008;89(10):1991-1995.
22. Bullock-Saxton JE. Local sensation changes and altered hip muscle function following severe ankle sprain. Phys Ther 1994;74(1):17-28.
23. Bullock-Saxton JE, Janda V, Bullock MI. The influence of ankle sprain injury on muscle activation during hip extension. Int J Sports Med 1994;15(6):330-334.
24. Gribble PA, Hertel J, Denegar CR. Chronic ankle instability and fatigue create proximal joint alterations during performance of the Star Excursion Balance Test. Int J Sports Med 2007;28(3):236-242.
25. Sedory EJ, McVey ED, Cross KM, et al. Arthrogenic muscle response of the quadriceps and hamstrings with chronic ankle instability. J Athl Train 2007;42(3):355-360.
26. Bahr R, Lian O, Bahr IA. A twofold reduction in the incidence of acute ankle sprains in volleyball after the introduction of an injury prevention program: a prospective cohort study Scand J Med Sci Sports 1997;7(3):172-177.
27. Rozzi SL, Lephart SM, Sterner R, Kuligowski L. Balance training for persons with functionally unstable ankles. J Orthop Sports Phys Ther 1999;29(8):478-486.
28. Tropp H, Ekstrand J, Gillquist J. Stabilometry in functional instability of the ankle and its value in predicting injury. Medicine and science in sports and exercise 1984;16(1):64-66.
29. Wang HK, Chen CH, Shiang TY, et al. Risk-factor analysis of high school basketball-player ankle injuries: a prospective controlled cohort study evaluating postural sway, ankle strength, and flexibility. Arch Phys Med Rehabil 2006;87(6):821-825.
30. Wikstrom EA, Naik S, Lodha N, Cauraugh JH. Balance capabilities after lateral ankle trauma and intervention: a meta-analysis. Med Sci Sports Exerc 2009;41(6):1287-1295.
31. McKeon PO, Hertel J. Systematic review of postural control and lateral ankle instability, Part I: Can deficits be detected with instrumented testing? J Athl Train 2008;43(3):293-304.
32. Munn J, Sullivan SJ, Schneiders AG. Evidence of sensorimotor deficits in functional ankle instability: A systematic review with meta-analysis. J Sci Med Sport 2009 May 11 [Epub ahead of print]
33. Arnold BL, De La Motte S, Linens S, Ross SE. Ankle instability is associated with balance impairments: a meta-analysis. Med Sci Sports Exerc 2009;41(5):1048-1062.
34. Hubbard TJ, Hicks-Little C, Cordova M. Mechanical and sensorimotor implications with ankle osteoarthritis. Arch Phys Med Rehabil 2009;90(7):1136-1141.
35. McGuine TA, Keene JS. The effect of a balance training program on the risk of ankle sprains in high school athletes. Am J Sports Med 2006;34(7):1103-1111.
36. Verhagen E, van der Beek A, Twisk J, et al. The effect of a proprioceptive balance board training program for the prevention of ankle sprains: a prospective controlled trial. Am J Sports Med 2004;32(6):1385-1393.
37. McKeon PO, Hertel J. Systematic review of postural control and lateral ankle instability, Part II: Is balance training clinically effective? J Athl Train 2008;43(3):305-315.
38. Laufer Y, Rotem-Lehrer N, Ronen Z, et al. Effect of attention focus on acquisition and retention of postural control following ankle sprain. Arch Phys Med Rehabil 2007;88(1):105-108.
39. Rotem-Lehrer N, Laufer Y. Effect of focus of attention on transfer of a postural control task following an ankle sprain. J Orthop Sports Phys Ther 2007;37(9):564-569.
40. Hale SA, Hertel J, Olmsted-Kramer LC. The effect of a 4-week comprehensive rehabilitation program on postural control and lower extremity function in individuals with chronic ankle instability. J Orthop Sports Phys Ther 2007;37(6):303-311.
41. Tropp H, Askling C. Effects of ankle disk training on muscular strength and postural control. Clin Biomech 1988;3(2):88-91.
42. Evans T, Hertel J, Sebastianelli W. Bilateral deficits in postural control following lateral ankle sprain. Foot Ankle Int 2004;25(11):833-839.
43. Collins JJ, Priplata AA, Gravelle DC, et al. Noise-enhanced human sensorimotor function. IEEE Eng Med Biol Mag 2003;22(2):76-83.
44. Gravelle DC, Laughton CA, Dhruv NT, et al. Noise-enhanced balance control in older adults. Neuroreport 2002;13(1):1853-1856.
45. Priplata AA, Niemi JB, Harry JD, et al. Vibrating insoles and balance control in elderly people. Lancet 2003;362(9390):1123-1124.
46. Priplata A, Niemi J, Salen M, et al. Noise-enhanced human balance control. Phys Rev Lett 2002;89(23):238101-238104.
47. Martinez L, Perez T, Mirasso CR, Manjarrez E. Stochastic resonance in the motor system: effects of noise on the monosynaptic reflex pathway of the cat spinal cord. J Neurophysiol 2007;97(6):4007-4016.
48. Ross SE, Guskiewicz KM. Examination of static and dynamic postural stability in individuals with functionally stable and unstable ankles. Clin J Sports Med 2004;14(6):332-338.
49. Ross SE, Guskiewicz KM. Effect of coordination training with and without stochastic resonance stimulation on dynamic postural stability of subjects with functional ankle instability and subjects with stable ankles. Clin J Sport Med 2006;16(4):323-328.
50. Wulf G, Weigelt, M, Poulter D, McNevin N. Attentional focus on suprapostural tasks affects balance learning. Q J Exp Psychol A 2003;56(7):1191-1211.
51. Wulf G, McNevin N, Shea CH. The automaticity of complex motor skill learning as a function of attentional focus. Q J Exp Psychol A 2001;54(4):1143-1154.
52. Vuillerme N, Nafati G. How attentional focus on body sway affects postural control during quiet standing. Psychol Res 2007;71(2):192-200.
53. Wulf G, Weigelt C. Instructions about physical principles in learning a complex motor skill: to tell or not to tell. Res Q Exerc Sport 1997;68(4):362-367.
54. Emery CA, Rose MS, McAllister JR, Meeuwisse WH. A prevention strategy to reduce the incidence of injury in high school basketball: a cluster randomized controlled trial. Clin J Sports Med 2007;17(1):17-24.
55. Holme E, Magnusson SP, Becher K, et al. The effect of supervised rehabilitation on strength, postural sway, position sense and re-injury risk after acute ankle ligament sprain. Scand J Med Sci Sports 1999;9(2):104-109.
56. McHugh MP, Tyler TF, Mirabella MR, et al. The effectiveness of a balance training intervention in reducing the incidence of noncontact ankle sprains in high school football players. Am J Sports Med 2007;35(8):1289-1294.
Figure Legends
Figure 1: Joint stability is the cumulative result of the sensorimotor system working effectively. More specifically, joint stability is the result of the afferent information (dotted lines) from the somatosensory system (peripheral feedback), integration of feedback from the somatosensory (and other sensorimotor system components) and the efferent response (solid lines) regulated by an individual’s neuromuscular control. Reprinted with permission from: Wikstrom EA, Tillman MD, Chmielewski TL, Borsa PA. Measurement and evaluation of dynamic joint stability of the knee and ankle after injury. Sports Med 2006;36(5):393-410.
Figure 2: The relative risk reduction (RRR) and 95% confidence intervals (CI) which indicate that balance training is effective for reducing the risk of sustaining a recurrent lateral ankle sprain. The RRR estimates the percentage of injury risk that is reduced for individuals who participate in an intervention program versus individuals in a control group. When the lower boundary (left side) of an RRR CI crosses zero, no risk reduction is present, but when the lower boundary is greater than zero, a reduction in injury risk is present. Reprinted with permission from: McKeon PO, Hertel J. Systematic review of postural control and lateral ankle instability, Part II: Is balance training clinically effective? J Athl Train 2008;43(3):305-315.37 Figure reference key: #15 refers to Bahr et al,26 #16 refers to McGuine and Keene,35 and #17 refers to Verhagen et al.36