
Options in subtractive milling materials still outnumber those for additive machines. (Image courtesy of Delcam Healthcare Solutions.)
By Emily Delzell
Practitioners and orthotic laboratory owners at the fourth annual Orthotics Technology Forum (OTF) thinking about switching from traditional design and manufacture methods to digital technology got an up-close look at two distinct systems—additive and subtractive—that promise to deliver quality devices in less time and at lower cost.
Both additive and subtractive machines are highly automated, allowing for rapid orthotic prototyping and manufacture, but their capabilities and compatibility with the needs of individual practitioners and practices are quite different.
OTF presenter and biomechanist Géza F. Kogler, PhD, CO, compared the subtractive process with sculpting marble; to create a 3D structure, the artist begins with a solid marble block, then “subtracts” material to realize his design. Subtractive machines can use either 3D data or 2D CAD data to produce an object.
Additive manufacturing, also called direct digital manufacturing, creates 3D objects by joining, fusing, or solidifying materials layer by layer.
CAD-CAM manufacturer Delcam Healthcare Solutions, a forum sponsor along with Freedom Machine Tool, Stratasys, nora, Acor, Tekscan, Kiwi, JMS Plastics, and Fisher/Unitech, brought in two office-sized systems for attendees to compare and consider.
Subtracting
Subtractive manufacturing in the modern sense has been around since the 1940s, but in recent years engineers have developed smaller, more powerful, and easier-to-use computer numerically controlled (CNC) routers.
 Patrick Bollar, CEO of Diversified Machine Systems (DMS) in Colorado Springs, CO, introduced OTF attendees to one of the newest examples of subtractive technology, a 3-axis machine designed with input from Delcam and first introduced in April at the Pedorthic Association of Canada’s annual PAC symposium.
Patrick Bollar, CEO of Diversified Machine Systems (DMS) in Colorado Springs, CO, introduced OTF attendees to one of the newest examples of subtractive technology, a 3-axis machine designed with input from Delcam and first introduced in April at the Pedorthic Association of Canada’s annual PAC symposium.
The enclosed machine has a 20″ by 16″ workspace and is designed to fit safely into an office environment—and through a standard office door. Its features include a grid fixture-type vacuum table, which Bollar said can cut material of any hardness below that of steel, and an industrial controller instead of the more common PC-based control.
Machines controlled by computer-fed data, said Delcam North America’s Vice President of Sales Maida Koller, who worked with DMS to develop the router, are limited by the rate at which data can be fed into the machine.
“We call it ‘starving for data,’ and the result is that you can’t get as smooth a finish,” she said. “The type of controller on this machine is the kind that’s typically found only on big, far more costly industrial machines, and eliminates that problem.”
Bollar said the machine, which can be used with a large range of materials, can produce about three pairs of foot orthoses every half hour.
Attendees were enthusiastic about subtractive technology, and at least one, Rick Prenger, CPed, who owns Walking Wellness in Ottawa, Canada, has made the move into digital technology since the conference, purchasing a subtractive system, digital scanner, and CAD-CAM software.
Using traditional plaster casts and foam box impressions, two people working in Prenger’s lab can currently turn out 10 to 12 pairs of orthoses a day. Going digital, he said, will eventually push that figure up to 30 pairs a day.
The old way of doing things, he said, is no longer economically viable, and his urgency to make the switch played a role in his purchasing decisions. The software, he ultimately bought, for example, wasn’t his first choice, but his top choice wasn’t available immediately and would have pushed his implementation date from this September to January 2015.
He’s been researching various systems for about a year and attending conferences to glean information. The OTF, particularly the opportunity it provided to talk with other practitioners and sales reps about different systems, helped solidify his plans, he said.
“I really liked the openness [of the OTF],” he said. “At some conferences people are very guarded about their trade secrets; here everything was wide open.”
Although Prenger has chosen subtractive technology for now, he said he plans on bringing in an additive machine in a couple years.
“The technology [additive] isn’t quite there yet—I think there are lots of glitches to be worked out, but the potential to build things into layers, with different areas being harder or softer as needed, is incredible. It will change how we’re looking at people’s feet, how we’re looking into gait pattern, and how we’re going to build the orthotic for the problems that we see.”
Adding
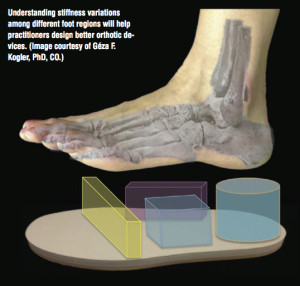
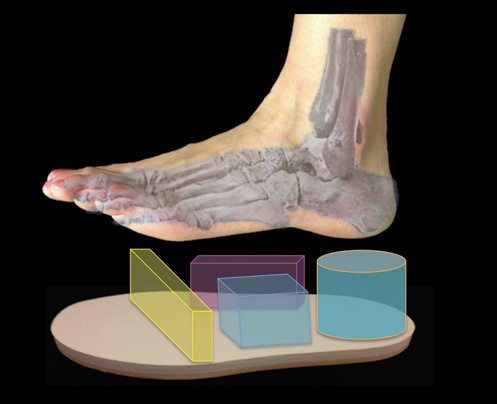
Changing the way practitioners assess patients’ feet and design orthoses was a theme echoed by Kogler, director of the Clinical Biomechanics Laboratory at Georgia Institute of Technology in Atlanta, who presented pilot study data showing that different foot regions vary in stiffness.

Additive machines allow practitioners to design almost any structural feature they can imagine. (Images courtesy of Delcam Healthcare Solutions.)
Kogler and his team measured the loading orientation of 19 foot regions with a 2-axis inclinometer, finding significant variation in initial stiffness and displacement in different regions.
“Most current orthoses have the same stiffness throughout, which is good for production, but we need more—we need to understand these variations to create optimal devices that control stiffness in different regions of the foot,” Kogler said.
Additive technology, with its ability to fuse different materials and create complex shapes of varied density in different areas of a single orthosis, will allow orthotic practitioners to draw on mechanical engineering principles in new ways that take advantage of research like Kogler’s.
The range of materials that can be used in additive machines is still limited compared with subtractive machines, but capabilities are expanding rapidly; the Stratasys 3D printer demoed at the OTF, for example, can use up to 14 different materials at once.
Additive technology appealed to two clinicians working in an orthopedic practice with a strong focus on foot and ankle surgery.
“We have multiple surgeons performing delicate and complicated surgery daily,” said Hannah Dwyer, a pedorthic resident and manager of orthopedic footwear at Midwest Orthopaedic Institute in Sycamore, IL. “Our main use would probably be using MRI-reading software to build surgical practice models. A tool that could potentially cut down on surgery times would allow us to have patients in and out faster, not only boosting productivity of surgeons, but also helping our patients.”
Thomas Dwyer, DPM, who works alongside his daughter at Midwest Orthopaedic, said, “I can see both technologies fitting into our practice. If any of our surgeons want to do templates, we would get the additive technology and use the machine for orthotics as well. If they’re not interested now, I would buy subtractive technology. When the additive technology adds more capabilities, maybe printed shoes, and drops in price, I would switch.”








Trackbacks/Pingbacks