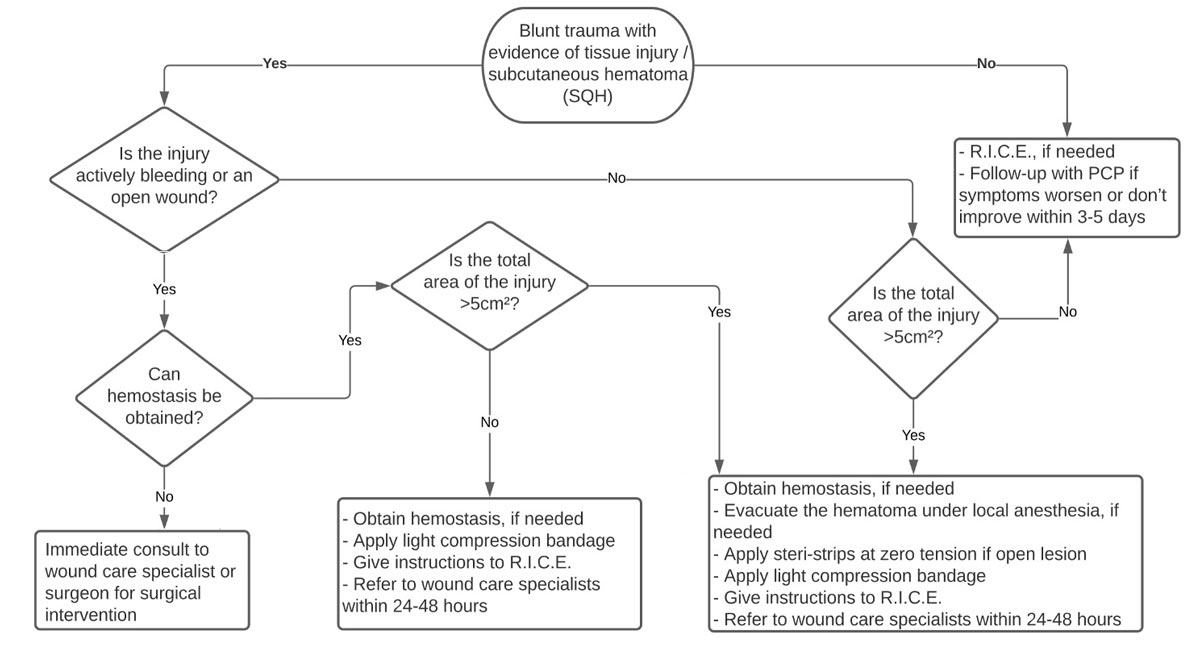
Figure 1. Authors developed this algorithm for use by providers to help appropriately treat and refer patients who experience blunt trauma to the lower extremity that results in soft tissue injury.
Researchers at the Kent State University College of Podiatric Medicine observed a specific subset of patients was frequently coming to their clinic with complications after mismanagement or misdiagnosis of initial blunt trauma soft tissue injuries to the lower extremity:
- Elderly (at greater risk for trauma or falls with resulting soft tissue injury)
- Multiple comorbidities (eg, diabetes or peripheral vascular disease) that contribute to thinning of the skin in the lower extremity
- Use of bloodthinners such as aspirin, warfarin, or Novel Oral Anticoagulants
- Sequelae such as infection, skin loss, chronic non-healing wounds, and a need for surgical intervention after developing deep dissecting hematomas (DDH)
In response to what they were seeing in their own clinic, these researchers sought to develop an evidence-based algorithm to help decrease mismanagement and/or misdiagnosis of initial injury by improving early detection, proper treatment, and proper referral of lower extremity blunt trauma soft tissue injuries to prevent serious complications.
After examining recent clinical cases of lower extremity blunt trauma soft tissue injuries that came to their wound clinic after having progressed to deep dissecting hematomas (DDH), they conducted a literature search and reviewed 25 articles focused on hematoma in lower extremities.
Then, they applied the algorithm to the case of an 85-year-old male with a left lower extremity skin tear laceration secondary to blunt trauma from a fall from a ladder (see Case Example, page 18). Using the algorithm, they found key differences from what happened and what the evidence base supported:
- Steri-strips at zero tension would have been used instead of Prolene stitches
- Referrals for follow up would have been for 24 to 48 hours after being seen, not 10 days.
The authors concluded that proper management of the initial injury may have prevented an additional ED visit, use of a second antibiotic, unnecessary patient pain, and surgery.
Patient outcomes can be improved through prompt recognition and appropriate treatment that can decrease the extent of tissue loss and associated wound defects and minimize the need for surgical intervention. The algorithm also streamlines the logistics of coordinating ongoing care for these at-risk patients by providing for proper referrals in appropriate timeframes.

Figure 2: Patient taken to OR, Interrupted Prolene stitches were removed. Figure 3: DDH surgically evacuated. Figure 4: Wound extended deep to the level of muscle and measured 8.2 cm x 6.4 cm x, 1.0 cm post-operatively. Figure 5: With aggressive wound care, patient healed in 11 weeks with minimal scarring
Case Example: History
85 YO male with LLE skin tear laceration secondary to blunt trauma from fall from ladder
- Seen in local ED 3 hours S/P initial injury
- No labs collected; negative x-ray of LLE
- Irrigation of injured tissue; re-approximation of traumatically avulsed tissue flap with interrupted Prolene stitches; dry dressing
- Discharged with oral antibiotics and instructions to follow- up with PCP in 10 days for stitch removal
5 days post-trauma returned to ED with continued pain, swelling, and redness at injury site
- WBC 4.6, blood cultures negative
- Duplex ultrasound negative for worsening DVT
- Discharged with additional antibiotics due to patient history of MRSA and again referred to PCP for stitch removal
9 days post-trauma presented to wound care clinic with persistent and worsening pain, edema and discoloration
- Diagnosed with DDH requiring surgical evacuation
Source: Cole W, Coe S, Chmielewski S. Implementation of the Dedicated Lower Extremity Hematoma Algorithm (LEHA) Will Improve Trauma Patient Outcomes. Poster presented at Symposium on Advanced Wound Care (SAWC) Fall Virtual. Sept. 18-20, 2020.