Shutterstock.com #145126192
By Janice T. Radak
When 88-year-old Doris fell getting out of the bathtub late on a Tuesday in the apartment she shared with her 90-year-old husband of 65 years, the ambulance took her to the hospital. As suspected, she had broken her right hip, which was surgically corrected Wednesday morning. Doris was up from bed Thursday and scheduled to transfer to a rehabilitation center that afternoon—but the hospital learned no bed would be available until Friday.
Doris never made it to rehab….
Doris was a close family friend whose story, sadly, is not uncommon. Falls in the elderly are not like falls in the young, who can get up, dust themselves off, and move on. Falls are a frequent and significant challenge for this population, with numerous studies detailing associations with mortality, morbidity, reduced functionality, and premature nursing home admission.1,2
What makes falls so dangerous in this population is the combination of their increased incidence and older adults’ increased susceptibility to injury. Every year, 3 million older adults are treated in the emergency department (ED) for fall-related injuries—most often head trauma or hip fracture.3 Indeed, more than 95% of hip fractures are caused by falling (usually, sideways), with 300,000 older adults hospitalized as a result. Significantly, older adults who visit the ED after a fall face an increased risk of revisiting the ED as well as an increased risk of dying. Some studies show that 25% of those who have a first ED visit for a fall will go on to have at least 1 additional fall-related visit, and 15% of those will die within the first year.4
Troubling trends, burgeoning costs
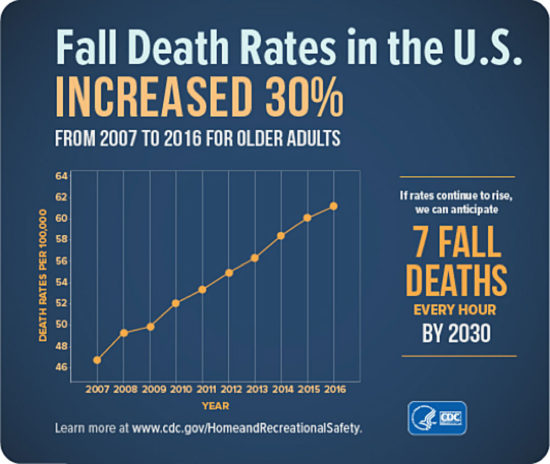
Recent data from the US Centers for Disease Control and Prevention (CDC) reveal an alarming trend: The rate of fall-related deaths among older adults increased 30% between 2007 and 2016.3 At that rate, CDC projects 7 fall-related deaths every hour among older adults by the year 2030.
To the increasing incidence of falls, add the growth of the over-65 crowd. The approaching tidal wave that is the Baby Boom generation—people born between mid-1946 and mid-1964—constitutes one of the largest birth cohorts in US history. In 2012, the 65-and-older population in the United States comprised 43.1 million people. But Baby Boomers, who started turning 65 in 2011, number nearly 77 million. By 2050, the over-65 age group will contain nearly 83 million people (nearly double today’s population) and represent 20% of the US population.5
Now add the cost to treat all these upcoming fall-related injuries and today’s public health alarm makes sense. In today’s dollars, fall-related injuries rank among the 20 most expensive medical conditions, with the average hospital cost more than $30,000 per incident. In 2015, total medical costs for falls totaled more than $50 billion, with Medicare and Medicaid shouldering 75% of costs.6
Risk factors for falls
In 1988, Tinetti and co-workers defined a fall as an event that results in a person coming to rest unintentionally on the ground or other lower level—not as a result of a major intrinsic event or overwhelming hazard.7
Nearly 70% of falls occur from the interaction of multiple risk factors: namely, the combination of acute and chronic risk factors that an individual brings into a particular environment8 (this is an easy feat, as 130 risk factors have been identified). And, it is understood that the risk of falling increases as the number of risk factors increases.7 This represents a double whammy for the elderly: In addition to normal age-related decline, such as decreased flexibility in joints and reduced kidney function, older adults have increasing numbers of chronic conditions for which they may take 5 or more medications (polypharmacy).9 Age-related changes in pharmacokinetics (absorption, distribution, metabolism, and excretion) and pharmacodynamics (the physiologic effects of the drug) can result in potentially serious adverse effects in older adults.10
Recognition of the risk of medication-related adverse events in older adults led to the development, in 1991 (updated in 2015), of the “Beers list,” which identified criteria for potentially inappropriate medication use in older adults.11,12 Yet, despite 25 years of multiple updates, use of the Beers List remains less than optimal in clinical practice, with one recent study finding that 43% of prescriptions for people ≥65 years meet the broad definition of inappropriate, and 30% meet a more qualified definition.13

Falls have consequences: The author’s mother 8 hours after she fell in her Alzheimer’s facility. She hit her head on her dresser at the start of the fall and broke her nose as she hit the floor. While there was no cranial bleed, she was never able to walk again.
In addition to polypharmacy and age itself, key risk factors associated with an increased risk of falling include:1,7
- Arthritis/joint pain
- Cardiovascular disease
- Depression
- History of falls
- Foot deformities/foot pain
- Reduced muscle strength and endurance
- Vision problems
- Nutritional deficiencies
- Cognitive incidents
- Chronic obstructive pulmonary disease
- Imbalance and gait deficits
- Peripheral neuropathy (numbness in the feet)
- Poorly fitting shoes
- Reduced response time
- Voiding problems
- Being female
Studies have shown that, among community-dwelling adults, 30% to 50% of falls that occur outdoors have an environmental cause (uneven surfaces, slippery walkways, poor lighting); 20% are due to causes that would make anyone fall.1 What makes it so dangerous for the elderly is the loss of all righting mechanisms—that is, the ability to stop one’s self from falling.
Perhaps this is part of the fear of falling that afflicts so many elderly. Indeed, 70% of those who have fallen, and nearly 40% of those who have not fallen, report a fear of falling. This fear is known to prevent people from participating in physical, functional, and social activities. Poor posture, low-speed walking, muscle weakness, and reduced quality of life have all been linked to this fear.1,4,7
How do falls happen?
For years, the popular belief was that falls were the result of slips, trips, or stumbles—reasons that were based on the recall of the faller, which was often incomplete.
Video evidence used to determine causation. Robinovitch and colleagues, to learn what precipitated falls, conducted a study that used real-world video footage of nursing home residents to examine how falls actually happen.14 Video captured 227 falls among 130 residents; researchers analyzed the recordings from a biomechanical perspective, with a focus on 2 aspects of fall initiation: cause of imbalance and activity just prior to the fall. Robinovitch’s team used 7 categories to identify the cause of the fall:
 incorrect transfer or shifting of body weight
incorrect transfer or shifting of body weight- trip or stumble
- hit or bump
- loss of support with external object
- collapse or loss of consciousness
- slip
- cause not discernible.
“Incorrect transfer or shifting of body weight” was defined as an apparent self-induced shift in body weight; i.e., moving the center of gravity outside the base of support.14 The key difference of this cause, as opposed to the others, is its internal, rather than external, genesis of the perturbation. Examples of these kinds of body weight shifts, Robinovitch reported, include “leaning too far from the base of support during walking or standing; failure to establish a stable final position during transferring or gait termination; excessive trunk sway; an improperly placed step during walking, with no obvious trip or stumble; or freezing during walking as is common in Parkinson’s disease.” Many falls in this category appeared to be overcorrections that occurred while transferring from one stance to another—sitting to standing, walker to chair, etc.
What Robinovitch found dispelled several myths:14
- A mere 3% of falls were caused by slipping
- Only 20% of falls were caused by “tripping” (eg, over an uneven surface or getting a foot caught in a chair leg or another walker)
- “Incorrect transfer or shifting of body weight” was identified as the cause of nearly 41% of falls among 51% of fallers
- Activities preceding the fall were ordinary moves of everyday life: The 4 most common activities just prior to the fall were walking forward (24%), standing quietly (13%), sitting down or lowering (13%), and initiation of walking (11%).
Other researchers are looking for underlying mechanisms that disrupt dynamic stability and might play a role in those disruptive overcorrections.
Applying virtual reality tools. In a series of recently published studies,15,16,17 Franz and other researchers from the University of North Carolina and North Carolina State University State Joint Department of Biomedical Engineering sought to understand how aging impacts neuromechanical strategies needed to accommodate balance perturbations while walking. The studies use virtual reality and optical flow balance perturbations that give people the visual perception that they are experiencing a fall.
In the first of these 3 studies,15 Qiao and colleagues collected leg-joint kinematics in young and older adults with and without varying degrees of perturbations, with the goal of looking at the effects of age on kinematic variability. Two findings seem relevant here:
- Kinematic variability, indicative of corrective motor adjustments, occurred primarily during push-off and early swing
- Older adults seemed unable to proportionately scale their response to even minor perturbations. Specifically, compared to young adults, post-hoc comparisons showed that, in response to smaller, 20-cm perturbations, older adults “increased sagittal plane hip, knee, and ankle joint variabilities by an average of 211%, 140%, and 94% more, respectively, and coronal plane hip joint variability by an average of 68% more” across the gait cycle.
In the second study,16 which looked at trunk kinematics in young adults, older non-fallers, and older fallers, participants in all three groups were found to be susceptible to perturbations during walking tests. However, researchers found age-related differences in local dynamic stability that had not been apparent during unperturbed walking, with more pervasive responses to perturbations in older fallers (i.e., a history of ≥1 fall) than older non-fallers while walking. Furthermore, the researchers were least able to predict the response of older fallers to balance perturbations from measurements during unperturbed walking.
In the most recent of the 3 studies,17 Allen and Franz used motor-module analyses to identify changes in the neuromuscular recruitment of leg muscles by older adults during walking trials. Their findings demonstrate that older adults with a history of falls, despite having no apparent neurologic deficits, have a reduced peripheral motor repertoire while walking, which might explain their disproportionate response to balance perturbations.
“Changes are happening that are negatively affecting balance,” Franz explained in a subsequent interview with LER. “We don’t know what. We don’t know when. But we know neural changes are all happening in tandem and building over time.” These 3 studies, he said, are trying to tease apart the deficits—first at the joint level, then in the dynamics of the trunk, and, third, at the neuromuscular level—in an effort to “find the critical threshold that once someone crosses, they fall.”
Although current screening tools for falls risk often use non-perturbed walking as the baseline, Franz notes that what the UNC–NC State research shows is that assessment most likely needs to be performed while the patient is walking—preferably, during challenged walking. Franz’s group is working with virtual reality tools in the hope of creating measures that can be used in clinicians’ offices on an everyday basis for such assessments.
Do falls interventions work?
Although falls do occur, they are not inevitable. Various types of falls prevention programs have been developed and deployed across countless settings. And there is evidence that they are succeeding in keeping older adults safe.
In the CDC’s STEADI (“Stopping Elderly Accidents, Deaths & Injuries”) initiative,18 the agency developed an algorithm to aid the implementation of the American Geriatrics Society/British Geriatrics Society clinical practice guideline for the prevention of falls in older persons. The algorithm recommends assessment and multifactorial intervention for those who have had 2 or more falls or 1 fall-related injury. Multifactorial interventions should include exercise—in particular, balance, strength, and gait training; vitamin D supplementation, with or without calcium; management of medications, especially psychoactive medications; home environment modifications; and management of postural hypotension, vision problems, foot problems, and footwear. These interventions have been shown to decrease falls in community settings, hospitals, and nursing homes.
A 2012 Cochrane Review19 examined 159 trials of various falls prevention interventions including tai chi (see “Evidence Building for Tai Chi as Falls Prevention Intervention,” page 2720-24) with nearly 80,000 participants overall; exercise as a single intervention and multifactorial programs were the most common interventions tested. Researchers used a rate ratio (RaR) to compare the rate of falls (i.e., falls/person/year) between the intervention and control groups; for risk of falling, they used a risk ratio (RR) based on the number of people falling (fallers) in each group.
The researchers found that multiple-component group exercise significantly reduced the rate of falls and risk of falling (RaR = 0.71 [confidence interval (CI), 0.63 to 0.82]; RR = 0.85 [CI, 0.76 to 0.96]), as did multiple-component home-based exercise (RaR = 0.68 [CI, 0.58 to 0.80]; RR = 0.78 [CI, 0.64 to 0.94]). Although the rate of falls for tai chi bordered on statistical significance (RaR = 0.72; CI, 0.52 to 1.00), tai chi did significantly reduce risk of falling (RR = 0.71; CI, 0.57 to 0.87).
The Cochrane Review authors compared other interventions as well and found that:
- Multifactorial interventions, which had to include individual risk assessment as part of inclusion, reduced the rate of falls (RaR = 0.76; CI, 0.67 to 0.86), but not risk of falling (RR = 0.93; CI, 0.86 to 1.02)
- Vitamin D did not reduce the rate of falls (RaR = 1.00; CI, 0.90 to 1.11) or risk of falling (RR = 0.96; CI, 0.89 to 1.03)
- Home safety assessment and modification interventions were effective for reducing the rate of falls (RaR = 0.81; CI, 0.68 to 0.97) and the risk of falling (RR = 0.88; CI, 0.80 to 0.96).
The National Council on Aging offers a detailed listing of select evidence-based falls prevention programs at www.ncoa.org/healthy-aging/falls-prevention/.
What can providers do?

iStockphoto.com 626641908
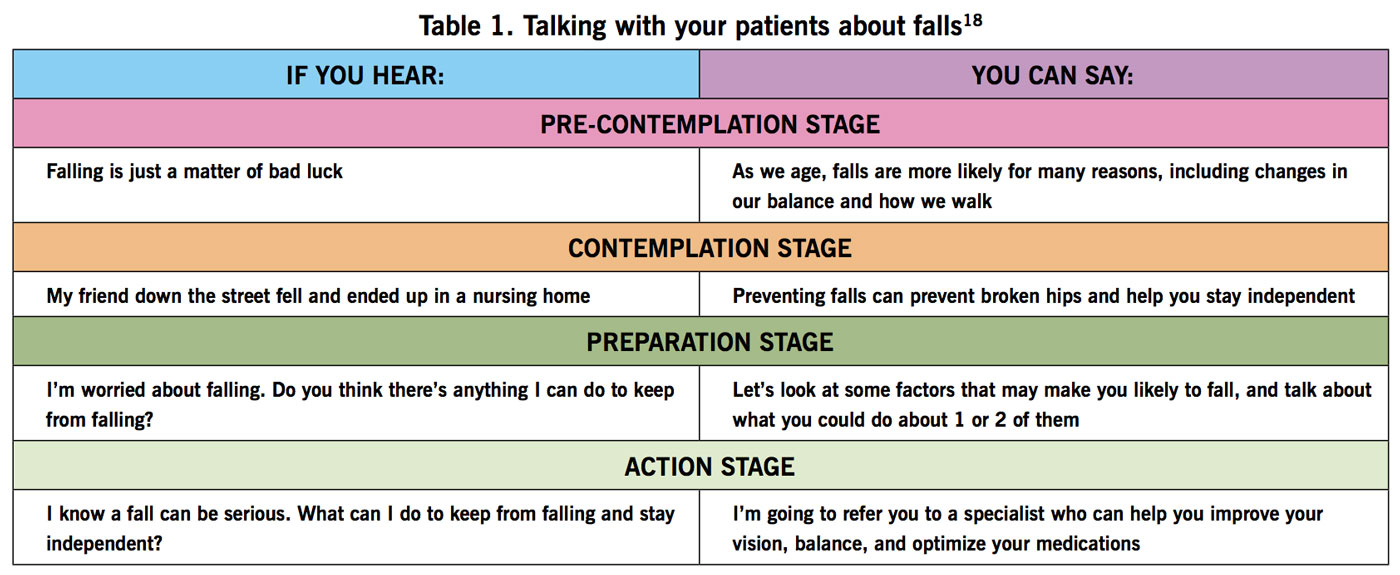
Have a conversation. Talking with patients about falls is a first step. Table 118 offers dialogue starters from the CDC’s STEADI initiative, which recommends clinicians be proactive and screen all patients ≥65 years with the following questions:18
- Have you fallen in the past year?
- Do you feel unsteady when standing or walking?
- Do you worry about falling?
“Simply reminding older patients of the importance of maintaining healthy leg muscles through regular movement, low-intensity resistance exercise, and adequate protein intake provides a tremendous public health service,” Robert Creighton, DPM, who is also a podiatry blogger and personal trainer, told LER.
Assess risk. Podiatrists should be offering falls risk assessment to all their Medicare patients. “It’s a service that podiatrists are thoroughly trained to provide, and it applies to the Medicare Physician Quarterly Reporting System (PQRS) Measure #154,” Creighton said. “When a patient has a documented fall history, defined as 2 or more falls in the past year or any fall with injury in the past year, then [PQRS Measure] #155 can be added for the subsequent care plan.”
Prescribe exercise and lifestyle modifications. Creighton has 3 evidence-based falls prevention recommendations for his patients:
- Proprioception, balance, and strength training. Lower-limb strength training has been shown to improve falls-related gait kinematics for older adults, he said. Indeed, conclusions from a randomized controlled trial by Persch and colleagues showed that strength training effectively reversed age-related changes in gait speed, stride length, cadence, and toe clearance, bringing the elderly close to reference values for healthy young women.25
- Exercise. Ideally, both resistance exercise and aerobic exercise are needed to keep older adults healthy—preferably, at least twice a week. The evidence comes from a German study, which found that a regimen of mixed, intense aerobic, resistance, and balance training for 18 months among women ≥65 years had a substantial effect.26 The researchers divided the group of 162 into low-intensity and high-intensity exercise, depending on how often they participated. Whereas there were no differences between the 2 groups in 10-year risk of coronary heart disease and in the number of falls, there were significant improvements observed for lumbar-spine bone mineral density and proximal femur bone mineral density, lean body mass, and appendicular skeletal muscle mass. Based on their findings, the authors concluded that exercising at least 2 sessions a week may be crucial for improving bone and muscle mass of elderly people.
- Nutrition. Often overlooked, good nutrition is critical for maintaining leg strength and avoiding frailty, said Creighton. There is some controversy over whether the recommended daily allowance for protein for elderly women is appropriate; Creighton pointed to a study of 65 older adults (60 to 74 years of age) who used a combination of exercise and protein supplements for 12 weeks found improved muscle strength and body composition with reduced body weight and increased strength.27
With aging, keep the focus on balance and strength
As the wave of Baby Boomers moves from middle age and to elderly years, maintaining balance and strength will be critical to keeping them safe and out of the hospital. Screening every patient older than 65 years and properly referring them to falls prevention programs will help clinicians ensure better outcomes—no matter the age of the patient.
Janice T. Radak, former Editor-in-Chief of the journal Geriatrics, is Editor of Lower Extremity Review.
- Dionyssiotis Y. Analyzing the problem of falls among older people. Int J Gen Med. 2012;5:805-813.
- Mangram A, Dzandu J, Harootunian G, et al. Why elderly patients with ground level falls die within 30 days and beyond? J Gerontol Geriatr Res. 2016;5:289.
- Burns E, Kakara R. Deaths from falls among persons aged ≥65 Years – United States, 2007–2016. MMWR Morb Mortal Wkly Rep 2018;67(18):509–514.
- Lesser A, Israni J, Kent T, Ko KJ. Association between physical therapy in the emergency department and emergency department revisits for older adult fallers: a nationally representative analysis. J Am Geriatr Soc. 2018 August 21. [Epub ahead of print]
- US Census Bureau. Fueled by aging Baby Boomers, nation’s older population to nearly double in the next 20 years, Census Bureau reports. Release Number: CB14-84. May 6, 2018. www.census.gov/newsroom/press-releases/2014/cb14-84.html. Accessed September 17, 2018.
- Centers for Disease Control and Prevention. Costs of falls among older adults. www.cdc.gov/homeandrecreationalsafety/falls/fallcost.html. Accessed September 17, 2018.
- Tinetti ME, Speechley M, Ginter SF. Risk factors for falls among elderly persons living in the community. N Engl J Med. 1988;319(26):1701–1707.
- Meyer G, Ayalon M. Biomechanical aspects of dynamic stability. Eur Rev Aging Phys Act. 2006;3:29-33.
- Kaufman DW, Kelly JP, Rosenberg L, Anderson TE, Mitchell AA. Recent patterns of medication use in the ambulatory adult population of the United States: the Slone survey. JAMA. 2002;287(3):337-344.
- Ruscin JM, Linnebur SA, Pharmacokinetics in the elderly. Merck Manual Professional Edition. Kenilworth, NJ: Merck Sharpe & Dohme Corp; June 2014. www.merckmanuals.com/professional/geriatrics/drug-therapy-in-the-elderly/pharmacokinetics-in-the-elderly. Accessed September 17, 2018.
- Beers MH, Ouslander JG, Rollingher I, Reuben DB, Brooks J, Beck JC. Explicit criteria for determining inappropriate medication use in nursing home residents. Arch Intern Med. 1991;151(9):1825-1832.
- American Geriatrics Society 2015 Beers Criteria Update Expert Panel. American Geriatrics Society 2015 Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults. J Am Geriatr Soc. 2015 Nov;63(11):2227-2246.
- Davidoff AJ, Miller GE, Sarpong EM, Yang E, Brandt N, Fick DM. Prevalence of potentially inappropriate medication use in older adults using the 2012 Beers criteria. J Am Geriatr Soc. 2015;63(3):486-500.
- Robinovitch S, Feldman F, Yang Y, et al. Video capture of the circumstances of falls in elderly people residing in long-term care: an observational study. The Lancet. 2013;381(9860):47-54.
- Qiao M, Feld JA, Franz JR. Aging effects on leg joint variability during walking with balance perturbations. Gait Posture. 2018;62:27–33.
- Qiao M, Kinh TN, Franz JR. Does local dynamic stability during unperturbed walking predict the response to balance perturbations? An examination across age and falls history. Gait & Posture. 2018;62:80–85.
- Allen JL, Franz JR. The motor repertoire of older adult fallers may constrain their response to balance perturbations. J Neurophysiol. 2018 August 22. [Epub ahead of print]
- Centers for Disease Control and Prevention. STEADI—Stopping elderly accidents, deaths & injuries. Available at https://www.cdc.gov/steadi/. Accessed September 17, 2018.
- Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2012(9):CD007146.
- Statista: The Statistics Portal. Number of yoga participants in the United States from 2012 to 2020 (in millions). www.statista.com/statistics/605355/us-yoga-participation. Accessed September 17, 2018.
- Lomas-Vega R, Obrero-Gaitán E, Molina-Ortega FJ, Del-Pino-Casado R. Tai chi for risk of falls. A meta-analysis. J Am Geriatr Soc. 2017;65(9):2037–2043.
- Zou L, Han J, Li C, Yeung A, et al. The effects of tai chi on lower limb proprioception in adults aged over 55: a systematic review and meta-analysis. Arch Phys Med Rehabil. 2018 August 17. pii: S0003-9993(18)30932-8. [Epub ahead of print]
- Han J, Anson J, Waddington G, Adams R. Proprioceptive performance of bilateral upper and lower limb joints: side-general and site-specific effects. Exp Brain Res 2013; 226(3):313-323.
- PEDro: Physiotherapy Evidence Database. PEDro statistics. September 3, 2018. www.pedro.org.au/
english/downloads/pedro-statistics. Accessed September 17, 2018. - Persch LN, Ugrinowitsch C, Pereira G, Rodacki AL. Strength training improves fall-related gait kinematics in the elderly: a randomized controlled trial. Clin Biomech (Bristol, Avon). 2009;24(10):819-825.
- Kemmler W, von Stengel S. Exercise frequency, health risk factors, and diseases of the elderly. Arch Phys Med Rehabil. 2013;94(11):2046-2053.
- Shahar S, Kamaruddin NS, Badrasawi M, et al. Effectiveness of exercise and protein supplementation intervention on body composition, functional fitness, and oxidative stress among elderly Malays with sarcopenia. Clin Interv Aging. 2013;8:1365-1375.