
Istockphoto.com # 15213116
Researchers from New York University have found that wearing high heels increases muscle activation, which can have painful ramifications throughout the kinetic chain. Some individuals, however, seem to adapt to high heels more effectively than others.
By Smita Rao, PT, PhD, and Renata Ripa, MA
High-heeled shoes (2 in/5 cm or higher) are worn by 57% to 62% of women and have been linked to the development of foot pain.1,2 Footwear choices and their role in the development of foot pain are a growing concern, particularly given that recent epidemiological studies have found that foot pain affects 10% to 28% of adults and has a substantial negative impact on health-related quality of life.3-6
High-heeled shoes may contribute to the development of foot pain by adversely affecting joint motion and consequent joint loading.7 Previous studies have shown that high-heeled shoe use is accompanied by increased medial forefoot plantar loading.8,9 In recent work, we found elevated plantar loading in individuals with foot pain, supporting the role of mechanical overloading in the development of foot pain.10 In addition to walking, individuals with foot pain report activities such as stair descent or descending from a curb as being particularly painful.11 While most studies have assessed lower extremity motion and joint loading during walking, few studies have assessed more challenging activities such as a single-limb step descent.

shutterstock.com # 29411662
Single-limb step descent mimics stepping off a curb and other weight-bearing activities of daily living, and is challenging because it requires increased joint motion and loading. When performed in high-heeled shoes, we expected to find that the combined effects of footwear and activity would results in increased demands on lower extremity musculature, reflected as increased activation. While previous studies have assessed the effects of high-heeled shoe use on muscles such as the gastrocnemius and rectus femoris,7,12 limited data are available related to the peroneus longus and gluteus medius. Recent reports indicate that the latter two muscles may play in important role in sagittal and frontal plane function at the ankle, knee, and hip joints.13 By comparison, the chief role of the gastrocnemius muscle is power generation at push-off phase of gait, while the chief role of the rectus femoris is to control swing phase knee flexion. We conducted a study to assess the effect of footwear (low versus high heels) and activity (walking versus step down) on activation of the gluteus medius, rectus femoris, peroneus longus, and medial gastrocnemius muscles.
Heel height study
Thirty-one women who were not habitual wearers of high-heeled shoes participated in this study. None of the participants reported any lower extremity or other musculoskeletal pain or conditions affecting walking. They performed two activities: walking along a 15-foot walkway and stepping down from an 8-inch (20.32 cm) step. The latter activity was designed to simulate stepping off a curb or single-limb step descent.11

Istockphoto.com # 17424298
Each activity was performed while the subject wore standardized, lab-issued, low-heeled and high-heeled footwear, sized to their feet. Because our main goal was to evaluate the effect of heel height, we picked shoes that were devoid of special features such as arch support, toe rings, or heel cups. A secondary consideration was shoe design that allowed the placement of markers in both low-heeled and high-heeled footwear conditions. Consequently, shoes with significant design features on the upper (e.g., huaraches, water shoes) were not suitable. Subjects were allowed as many practice trials as they needed to feel comfortable with the footwear and activity. A minimum of five trials were collected for each activity and footwear condition as the subjects walked at a self-selected walking speed, monitored to ±5% using an infrared timing device.
Muscle activation was assessed using electromyography (EMG). Bipolar surface electrodes were placed over the gluteus medius, rectus femoris, peroneus longus, and medial gastrocnemius muscles. A single tester prepared the subjects’ skin by cleaning with alcohol and gentle abrasion. Linear envelopes of EMG data were created and muscle activation was quantified as EMG amplitude, expressed as a percentage of peak activation noted during walking with low-heeled shoes. All EMG data were time-normalized to the stance phase.
Peak muscle activation in the stance phase of gait was calculated for each muscle during each activity and footwear condition, and served as the chief dependent variable of interest. The effect of activity and footwear on peak muscle activation was examined using two-way repeated measures ANOVA. Interaction effects were assessed first, followed by simple or main effects as appropriate (p=.05). Exploratory data analysis using bivariate correlation (Pearson’s r) and k-means cluster analysis was also done.
Significant interaction between activity and footwear type was found for both proximal muscles (p<.01 and p=0.04 for gluteus medius and rectus femoris). Significant effects of activity and footwear were found for gluteus medius (p<.01 and p<.01) and rectus femoris (p<.01 and p<.01, Figure 2). No interaction effect was found for medial gastrocnemius (p=.74), but significant effects of activity (p<.01) and footwear (p<.01) were found. Significant interaction was found for peroneus longus (p<.01). Subsequently, significant simple effects of footwear (p=.03) and activity (p<.01) were noted (Figure 3).

Figure 1. High-heeled (3 in/7.62 cm) footwear, top, and low-heeled (0.75 in/1.91 cm) footwear, bottom, used in study.
A modest negative correlation was noted between gluteus medius and peroneus longus activation during the step-down task in high-heel shoes (r=-0.41, p<0.01)
Using k-means cluster analysis, we assessed whether there were subgroups of individuals in our study population who used different activation strategies. After we normalized activation in high heels to activation in low heels, we found that participants could be assigned to one of two clusters (Figure 4). Activation in high heels relative to activation in low heels during walking was higher across the four muscles for individuals in Cluster 1 (n=10, green circles) compared to Cluster 2 (n=20, orange squares). Further analyses are underway to determine predictors of cluster membership.
Proximal implications
Overall, these results indicate that high-heeled shoes affect not only distal lower extremity muscles (gastrocnemius and peroneus longus) but also proximal muscles (rectus femoris and gluteus medius). Muscle activation in high heels was consistently higher than muscle activation in low heels; notably, these differences in activation were greater for the proximal muscles than the distal muscles. The higher levels of muscle activation may predispose wearers of high-heeled shoes to fatigue and the development of pain, although previous work in this area has not examined the proximal muscles.14
Long-term use of high-heeled footwear may not only have implications for the development of foot pain but may also negatively influence the strength and endurance of proximal muscles. Specifically, endurance in the proximal muscles may be negatively affected due to fatigue and pain. Decreased proximal muscle strength resulting from high-heeled shoe wear could also affect knee loading, which could in turn lead to knee pain. Consistent with this theory, previous studies have found that the use of high-heeled shoes has been accompanied by increased knee loading.15,16 These findings have tremendous public health relevance because increased knee loading is a marker of knee osteoarthritis severity and progression.17,18
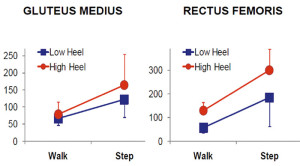
Figure 2. The effect of footwear on gluteus medius and rectus femoris peak activation was influenced by activity performed (interaction p<.01 and p=0.04 for gluteus medius and rectus femoris, respectively). For both muscles, peak activation was higher in high-heeled shoes and in the step down task.
Although evidence indicates that the use of high-heeled footwear significantly increases the odds of foot pain,19 foot pain in habitual wearers is not universal. There may be a subgroup of high-heeled shoe users who are able to adapt to the demands on proximal musculature or decrease the “dosage” (reduce length of time or distance walked in high-heeled shoes) to reduce the overall stress on the lower extremity.
Consistent with previous authors, we found an increase in rectus femoris activation and a decrease in gastrocnemius muscle activation in high-heeled shoe walking.7,14 We agree with previous authors in that habitual high-heeled shoe use increases the loads sustained at the knee and may have detrimental long-term effects on the strength and endurance of the gastrocnemius muscle.
Step descent surprise
Overall, higher muscle activation during the step down task compared to the walking task was seen for all muscles except the medial gastrocnemius. Gastrocnemius muscle activation being lower during step down than during walking is a thought-provoking finding. We were expecting that the gastrocnemius would have to work harder in the high-heeled shoe step down condition compared to the high-heeled shoe walking condition because of the additional ankle dorsiflexion associated with step descent. We expected the gastrocnemius to work eccentrically and control the forward progression of the tibia during the step down.

Figure 3. No significant interaction between activity and footwear type was found for medial gastrocnemius (p=.74) while a significant interaction was found for peroneus longus (p<.01). For both muscles, peak activation was higher in high-heeled shoes and lower in the step down task.
In contrast to our hypothesis, our data showed that the rectus femoris increases its activation to control knee flexion. The lower activation in the gastrocnemius may indicate that we use proximal muscles preferentially during the step down task. The relationship between the peroneus longus and gluteus medius may suggest that the two muscles work together to provide frontal plane stability.
A unique finding of our study is that we were able to discern a high-activation subgroup and a low-activation subgroup. Individuals in the high-activation subgroup showed a greater increase in activation compared to the low-activation group (in the high-heeled condition relative to the low-heeled condition). Previous footwear use may have played a role in group membership. Most of the data were collected between November and March in New York City, so most participants at that time were accustomed to wearing winter footwear rather than either of the more summery styles tested. Additional studies are indicated to determine the consequences of being in the high-activation group versus the low-activation group, particularly for individuals with foot pain who habitually wear high-heeled shoes.
Conclusion

Figure 4. Cluster 1 (n=10, green circles) showed higher activation across the four muscles compared to cluster 2 (n=20, orange squares)
Our study builds on previous evidence showing that increased plantar loading and foot motion noted with high-heeled shoe use may be important pathways in the development of pain. Additionally, we found preferential increases in proximal muscles, particularly in the step down task, with high-heeled shoe use. The unique findings of our study indicate that proximal and distal muscle activation may also be a key pathway in the development of musculoskeletal foot pain.
Smita Rao, PT, PhD, is a physical therapist and biomechanist whose research examines mechanisms underlying the evolution of foot pain and an assistant professor in the Department of Physical Therapy at New York University. Renata Ripa, MA, is a physical therapist and certified pilates instructor and was a graduate student in the Department of Physical Therapy at New York University at the time this study was conducted.
References:
1. Cho NH, Kim S, Kwon DJ, Kim HA. The prevalence of hallux valgus and its association with foot pain and function in a rural Korean community. J Bone Joint Surg Br 2009;91(4):494-498.
2. Nguyen US, Hillstrom HJ, Li W, et al. Factors associated with hallux valgus in a population-based study of older women and men: the MOBILIZE Boston Study. Osteoarthritis Cartilage 2010;18(1):41-46.
3. Greenberg L, Davis H. Foot problems in the US. The 1990 National Health Interview Survey. J Am Podiatr Med Assoc 1993;83(8):475-483.
4. Garrow AP, Silman AJ, Macfarlane GJ. The Cheshire Foot Pain and Disability Survey: a population survey assessing prevalence and associations. Pain 2004;110(1-2):378-384.
5. Hannan MT, McLennan CE, Rivinus MC, et al. Population-based study of foot disorders in men and women from the Framingham Study. Arthritis Rheum 2006;54(Suppl):S497.
6. Hill CL, Gill TK, Menz HB, Taylor AW. Prevalence and correlates of foot pain in a population-based study: the North West Adelaide health study. J Foot Ankle Res 2008;1(1):2.
7. Stefanyshyn DJ, Nigg BM, Fisher V, Liu W. The influence of high heeled shoes on kinematics, kinetics, and muscle EMG of normal female gait. J Appl Biomech 2000;16(3):309-319.
8. Yu J, Cheung JT, Fan Y, et al. Development of a finite element model of female foot for high-heeled shoe design. Clin Biomech 2008;23(Suppl 1):S31-S38.
9. Yung-Hui L, Wei-Hsien H. Effects of shoe inserts and heel height on foot pressure, impact force, and perceived comfort during walking. Appl Ergon 2005;36(3):355-362.
10. Rao S, Baumhauer JF, Nawoczenski DA. Is barefoot regional plantar loading related to self-reported foot pain in patients with midfoot osteoarthritis. Osteoarthritis Cartilage 2011;19(8):1019-1025.
11. Rao S, Baumhauer JF, Tome J, Nawoczenski DA. Comparison of in vivo segmental foot motion during walking and step descent in patients with midfoot arthritis and matched asymptomatic control subjects. J Biomech 2009;42(8):1054-1060.
12. Simonsen EB, Svendsen MB, Norreslet A, et al. Walking on high heels changes muscle activity and the dynamics of human walking significantly. J Appl Biomech 2011 Aug 26. [Epub ahead of print.]
13. Powers CM. The influence of abnormal hip mechanics on knee injury: a biomechanical perspective. J Orthop Sports Phys Ther 2010;40(2):42-51.
14. Gefen A, Megido-Ravid M, Itzchak Y, Arcan M. Analysis of muscular fatigue and foot stability during high-heeled gait. Gait Posture 2002;15(1):56-63.
15. Kerrigan DC, Todd MK, Riley PO. Knee osteoarthritis and high-heeled shoes. Lancet 1998;351(9113):1399-1401.
16. Kerrigan DC, Johansson JL, Bryant MG, et al. Moderate-heeled shoes and knee joint torques relevant to the development and progression of knee osteoarthritis. Arch Phys Med Rehabil 2005;86(5):871-875.
17. Hurwitz DE, Ryals AR, Block JA, et al. Knee pain and joint loading in subjects with osteoarthritis of the knee. J Orthop Res 2000;18(4):572-579.
18. Sharma L, Hurwitz DE, Thonar EJ, et al. Knee adduction moment, serum hyaluronan level, and disease severity in medial tibiofemoral osteoarthritis. Arthritis Rheum 1998;41(7):1233-1240.
19. Dufour AB, Broe KE, Nguyen US, et al. Foot pain: is current or past shoewear a factor? Arthritis Rheum 2009;61(10):1352-1358.









The most obvious component missing from this study are the dimensions of the contact surface of the heels. I cannot assess from the pictures nor from the article if the heel dimensions of the low heel and high heel shoe were the same. My best guess is that the contact area on the low heel shoe was much greater than the high heel shoe. If the heel dimensions are indeed different, that would change the outcomes of this study. Maybe the authors could clarify the heel dimensions of the 2 shoes used. I would be interested in outcomes of high heel shoes with heels that have a much larger contact area vs. the extremely narrow heels used in this study.