Perfect compliance is probably too much to hope for. But patient education, diligent follow-up, empathy and a little imagination can go a long way toward improving device wear rates and clinical outcomes.
By L.W. Barnes
Despite decades of research, innovations and refinements that have helped orthotics and prosthetics evolve from their progenitors into far more refined applications, one axiom still holds true: patient compliance is hard fought.
That’s because patients, no matter their affliction, wrestle with a host of conflicts from vanity (think: I don’t want kids in school to see me in this brace) to restricted mobility and discomfort, all of which make it easy to abandon prescribed treatments and leave compliance to “the other guy.”
Physicians, O&P clinicians and physical therapists rely on every weapon in the therapeutic arsenal— from cajoling to cartoon characters— to overcome those obstacles. The challenges are many.
Interviews with practitioners, even those who say their patients dutifully follow medical directives, suggest that patients seldom achieve perfect compliance.
“I don’t put my dish away every night,” said Ken Gavin, CO, with Audubon Orthotic & Prosthetic Services in Colorado Springs, CO. “No one is going to give you 100 percent,” he said, unless the patient buys in completely.
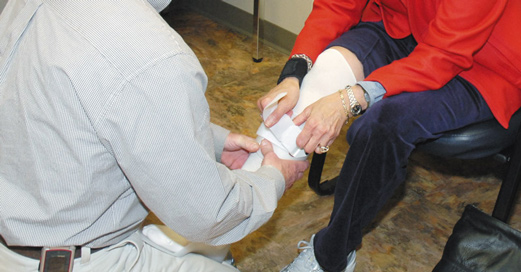
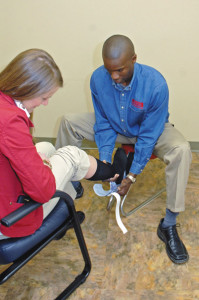
Why? Comfort plays a big role. If a device does not fit correctly – if it’s too loose, too tight, or not aligned properly, particularly in people with a lot of edema— a patient may decide it’s not worth the pain. If the device is too heavy or the material doesn’t breathe, or if it’s difficult to put on (a recurrent problem for those who’ve had strokes or suffer from arthritis, obesity and other conditions), they may also score low in compliance.
Fear is also a factor, especially among athletes who worry that a brace will slow them down or signal weakness to an opponent, even if the device is likely to help their performance.
Vanity is a stumbling block most often encountered by women who may find it hard to cosmetically disguise a brace. Although this is less of an issue in lower extremity O&P than in scoliosis bracing – where resistance on the part of teenage girls is such that some practitioners resort to negotiating reduced wear time, when appropriate, in exchange for a commitment to the treatment plan– an AFO is not what most women would consider a fashionable footwear accessory.
And without strong parental guidance, children can suffer from forgetfulness, as can the elderly, who also need monitoring and may have the most trouble adapting to change. Slow recoveries, lack of mobility and inappropriate expectations all can play a role in compliance.
But perhaps the biggest hurdle faced by clinicians in the compliance game, they say, is simply patients’ ignorance of the consequences.
That’s why many practitioners say it’s their job, first and foremost, to embolden patients to understand their treatment and do the work it takes to make the brace do its work.
“Education is central to compliance. It’s huge,” said Larry Lerman, CO, vice president of Lerman & Sons Orthotics & Prosthetics in Beverly Hills, CA. “In the beginning I talk [with patients] about what we’re doing, what we’re trying accomplish, why we’re here. I try to make people knowledgeable about what they’re getting into. Similarly, I let them know we’re available if they get off track.”
That because, as Lerman puts it, “the device is just a tool. How you use it makes all the difference.” While some patients may think that their fate rests in the hands of a surgeon, even a surgical outcome, clinicians say, is equally incumbent on patient participation.
Gavin likens his work to that of a coach, explaining the positives and negatives, setting goals and making sure that there are realistic expectations and lots of communication, which he says is key to patient “buy-in.” What’s the patient’s comfort level? What kind of discomfort is likely? What kind of lifestyle accommodations will be necessary? How will O&P treatment be a key component of a safe and cost effective outcome?
“All of these things need to fit together in order to reach a
common goal,” Gavin said. To make it work, “you have to have buy- in from the patient that they accept both the complications as well as the functional positives of the device.”
Shane Coltrain, CPO, president of Orthotics and Prosthetics East in Greenville, NC, deals mostly with amputees on a day-to-day basis. He says it’s his heavy reliance on patient follow-up that helps boost his compliance rate.
Because prosthetic devices must be comfortable not only when a patient is walking, but also sitting, or riding in a car or airplane, Coltrain said he schedules appointments with his patients at two- week intervals until they’ve had the device for a month. Then he follows up at three months, and again every four to five months. All to be sure the fit is right and the comfort level is appropriate.
“The patient needs to be educated on the device and on how to wear it,” Coltrain said. “That takes consistent follow-up to make adjustments. If they’re happy, they’re more likely to wear it. That goes for orthotics too.”
As with any type of device, orthotic or prosthetic, clinicians say the device must also provide enough advantages that the patient is willing to put up with the inherent disadvantages.
Scott Hosie, CPO, who works at Shriner’s Hospital for Children in Salt Lake City, UT and has been in O&P for 25 years, says a large part of successful compliance is making sure the brace is appropriate for the patient’s needs.
“If you put a brace on a patient who doesn’t need it, they won’t wear it,” said Hosie, who deals exclusively with lower-extremity cases. “If you put one on a patient who’s unstable, falling and tripping, and now they can walk and won’t fall as much, they’ll wear it.”
Where it becomes a more challenging endeavor, Hosie says, is in trying to prevent degradation – as is often the case with knee and spinal bracing.
Hosie deals a lot with kids who don’t necessarily need a brace for improved function but rather for positional support, such as with children with cerebral palsy who need bracing to prevent ankle contractures.
“We don’t provide any function,” Hosie said. “That’s when the parents’ involvement becomes very important. They’re the ones who have to enforce brace wear.”
Parents, of course, play a major role when it comes to compliance, at least until their children become rebellious teens. Then, as Hosie puts it, “there’s only so much you can do.”
Until that time, clinicians say they’re strong believers in braces constructed with funky colors and adorned with cartoon characters to inspire compliance. And it works.

istockphoto.com 11853069
“It’s amazing how the kids enjoy that,” Hosie said. “They’re no longer the kid that has to wear the brace but the kid that gets to wear the cool brace.”
By the same token, he’s not above suggesting a reluctant adult consider a brace featuring the logo of a favorite sports team. Flesh- colored devices are also available for those interested in a more subtle look.
Comfort issues can be address easily by trying different materials – foam cushioning, mesh, wicking materials and Velcro are all used. New material concepts like bamboo have allowed practitioners a wider range of choices to enhance patient comfort. Lerman is currently working with industry manufacturers to enhance the design criteria needed with graphite in the construction of AFOs to make them stronger and lighter.
Structural changes are also easy to tweak, such as trimming the edge of a device so that it doesn’t rub. Coltrain, for example, has seen problems with socket-fit for transfemoral amputees. To solve the issue during a refit, he’ll heat the gel liner and form it directly to the positive model of the patient, then fabricate the socket over that, creating a more comfortable liner and a more comfortable fit.
Combating a child’s feelings of emotional distress, however, can be a more difficult fix.
In some cases, Hosie said, he will send a care coordinator or social worker to a child’s school to explain why a classmate has an artificial leg and how it works.
“It can really break the ice,” Hosie said, but warned that when entering the school environment, clinicians must tread carefully to create positive attention rather than negative.
The same technique can be used for orthotic cases as well, but the method goes from helpful to totally counterproductive when kids approach their teen years.
“When they get older of course they don’t want any attention,” Hosie said.
Once a child is not longer largely under the influence of a parent, compromise and bargaining become a big factor for clinicians.
Gavin, who been in the profession for 18 years, said his adolescent patients are consistent: two out of 10 kids will not use their braces as instructed. Most, he said, overcome their issues with proper guidance. While you can’t predict the future, outcomes can be improved, he said. “Once their function is increased, they acclimate to the use of the braces and prosthetics very well,” Gavin said. “They are able to relate with the device.”
Adults, particularly those in denial about their conditions, pose the biggest challenges. They’re extreme cases, patients who ultimately will need counseling. It’s a touchy subject, he said, and one that the profession needs to develop better guidelines and instruction for.
“I’ve had other clinicians tell me they never encounter negative people,” Gavin said with incredulity. “’Oh really?’ I tell them. ‘You must be practicing on a beach in Hawaii.’”
For those patients, who have not accepted their condition and simply will not follow the prescribed treatment, he recommends a visit with a psychologist or counselor. It’s a technique, he said, that’s prone to make some patients even more upset, but one that he feels is appropriate.
The problem is less extreme, he said, the less bracing someone has to cope with. Some are so hobbled by their disabilities that they give up on compliance. Even for others, Gavin said, little things can become “a mountain.”
“Some [of the issues that surround compliance] have to do with fear,” Gavin said. “Not the fear of hurting yourself but the fear of losing your public identity and your physical abilities. As we all know, fear prevents a lot of people – not just those who are physically challenged –from doing a lot of things.”
It’s not fear, but largely vanity, clinicians say, that causes some patients with diabetes to struggle with compliance (see “Diabetes: Improving foot care compliance,” October, page 25).
Clinicians say they see it all the time – patients who are noncompliant because they want to wear shoes that are more attractive than those approved by Medicare, or, hard as it may be to fathom, patient with gaping ulcers in the soles of their feet who don’t want to wear a boot or walker. Researchers have used accelerometers embedded in offloading devices to confirm that patients’ reported compliance often far exceeds their actual compliance, but those assessment tools have yet to become a part of daily clinical practice.
It’s not that patients are self-destructive, practitioners say. It’s that in addition to all of the aforementioned factors that contribute to noncompliance, patients with diabetic neuropathy lack the sensation to know an ulcer has developed unless they see it—and aren’t likely to be motivated by the idea of relieving pain they’re not experiencing. These patients are generally referred for a total contact cast (TCC) or a so-called “instant TCC,” a removable walker rendered irremovable with fiberglass casting material.
Sometimes, Coltrain says, there’s too much compromise in the mix, particularly when it comes to the new styles of diabetic shoes on the market.
“We’re staring to lose the actual function of the shoe in order to improve compliance, making them more appealing so that patients will wear them,” he said. “On the back side, they may not function as well, causing further problems.”
“There’s a very fine line you have to tread with patients,” Coltrain said. “Always.”
Gavin weighs in on the side of practicality, saying that in his book compliance is largely about compromise, assuming it doesn’t put the patient at risk.
“If you’re willing to accept 70 percent of compliance and/or what the device will provide,” Gavin said, “Then I say, ‘Let’s do it.’”
L.W. Barnes is a freelance writer and editor based in Alexandria, VA.