
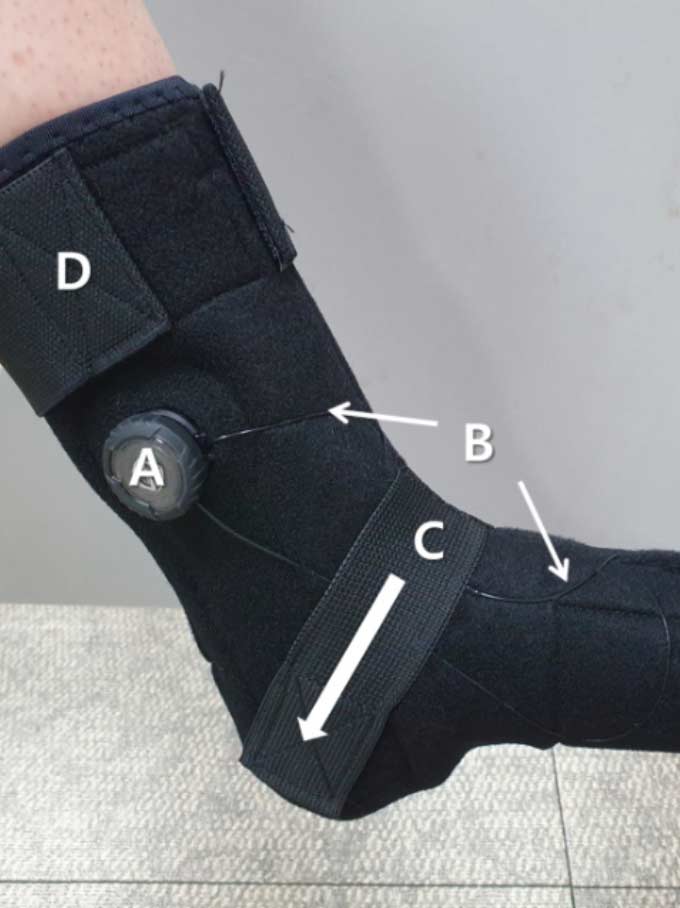
Figure 1. Lateral view of the ankle–foot orthosis using wire. A: wire adjustor; B: wire; C: talus posterior gliding Velcro; D: Velcro for ankle fixation; E: metatarsal joint stabilization strap.
Figure 2. Lateral view of induction of passive ankle dorsiflexion. A: wire adjustor; B: passive ankle dorsiflexion.
Researchers from Korea have developed a new type of AFO that uses neoprene and a novel wire configuration for use with foot drop after stroke.
By Jung-Hoon Lee, Im-Rak Choi, and Hyun-Su Choi
Foot drop can be a sequela of stroke. An ankle–foot orthosis (AFO) is the most widely used method to prevent foot drop in patients with stroke, and is used during weight-bearing training of the limb on the affected side or when there is ankle spasticity or deformity. AFO use has been reported to improve abnormal gait caused by mediolateral instability of the ankle in patients with stroke and enhance balance in these patients. However, AFOs passively fix the ankle to restrict ankle joint movement, thus limiting mobility of the joint; and they have been reported to cause contracture of the ankle joint and reduce muscle activity of the lower extremity. They also limit ankle range of motion (ROM), which makes standing from a seated posture difficult; thus, the neuromuscular system cannot be stimulated. However, despite these shortcomings, plastic AFOs are widely used for foot drop in patients with stroke.
Thus, the aim of this cross-over study was to investigate the immediate static balance effects of bare foot, plastic UD-Flex AFO, and a newly developed AFO using wire (AOW) in stroke patients with foot drop.
The AOW Orthosis
The AOW (Okmeditech Co., Ltd, Changwon, Korea) is a newly developed AFO designed by the first author. It is made of a flexible material consisting of neoprene and spandex and has a polyvinyl chloride (PVC) wire to induce passive ankle dorsiflexion (Figure 1). The device was designed such that turning the wire adjustor above the lateral and medial malleoli (A in Figures 1 and 2) triggers the wire crossed above the dorsum of the foot (B in Figure 1), inducing passive ankle dorsiflexion and preventing plantarflexion (B in Figure 2). Further, to assist ankle dorsiflexion, a talus strap made of polyester with rubber is stretched and attached from the front of the ankle joint toward the inferior posterior direction on both sides (C in Figure 1) to induce talus posterior gliding (Arrow of Figure 1). A Velcro strap on the top of the ankle secures the AOW from sliding down the ankle (D in Figure 1). Another Velcro strap is used to fix the front part of the orthosis above the intermetatarsal joints (E in Figure 1).
The UD-Flex AFO
The UD-Flex AFO used in this study was a type of plastic AFO that compensates for the shortcomings of the posterior AFO, which is widely used in hospitals to prevent foot drop in patients with stroke (Figure 3).
Results
Seventeen patients with foot drop resulting from stroke (8 men and 9 women) were randomized to three conditions (bare foot, UD-Flex AFO, or AOW made with a flexible material). Static balance was assessed using the Zebris (Zebris GmbH, Isny, Germany) and BioRescue (RM Ingenierie, Rodez, France) pressure platform by a single examiner, following a random order.
The center of pressure path length (mm) measured using Zebris showed significant differences among the three conditions (bare foot, 484.47 ± 208.42; UD-Flex AFO, 414.59 ± 144.43; AOW, 318.29 ± 157.60) (P < 0.05). The bare-foot condition was not significantly different from the UD-Flex AFO condition (P > 0.05), but was significantly different from the AOW condition (P < 0.05). The surface area ellipse (mm2) measured using BioRescue showed significant differences among the three conditions (bare foot, 241.35 ± 153.76; UD-Flex AFO, 277.41 ± 381.83; AOW, 68.06 ± 48.98) (P < 0.05). The bare-foot condition was not significantly different from the UD-Flex AFO condition (P > 0.05), but the AOW condition was significantly different from the bare-foot (P < 0.05) and from the UD-Flex AFO conditions (P < 0.05).
Discussion
The static balance of the UD-Flex AFO condition was not significantly increased in the BioRescue and Zebris measurements compared to the bare-foot condition. The BioRescue measurements showed significantly improved static balance when using AOW compared with the bare-foot and UD-Flex AFO conditions and the Zebris measurements showed significantly increased static balance when using the AOW compared with the bare-foot condition. AFO made with plastic limits the ROM of the ankle and decreases its control, therefore, AFO aggravates mobility and balance. Although the study of Kim et al. [2015] did not focus specifically on the use of AOW, their use of an elastic band-type AFO led to improved balance compared to when a plastic AFO or bare foot was used. The reason for this was suggested to be the ability of the elastic band-type AFO to promote even weight distribution between the affected and nonaffected limbs. The AOW used in this study seemed to improve static balance, with the polyvinyl chloride (PVC) wire attached to the mediolateral side of the ankle potentially inducing passive ankle dorsiflexion and preventing plantarflexion, as well as promoting even distribution of pressure while decreasing COP displacement. Furthermore, the flexible material consisting of neoprene and spandex permitted minimal movement required to control the position of the ankle joint, possibly helping to improve static balance.
Patients with stroke have trouble controlling their ankles due to the weakening of tibialis anterior, spasticity of gastrocnemius, and asymmetry of the anterior talofibular ligament, with further difficulty regarding posterior gliding of the talus below the tibia during dorsiflexion. The lack of posterior gliding of the talus limits ankle dorsiflexion, which alters the alignment of the foot in turn, thereby leading to abnormal ankle movement and increased risk of ankle injury. In a previous study, patients with chronic stroke who wore a flexible AFO made of elastic bands demonstrated increased balance due to the elastic band providing lesser limitation of dorsiflexion than the plastic AFO. Lee et al. [2017] reported that talus posterior gliding in a weight-bearing posture improved static balance in patients with stroke by increasing afferent stimulation of the ankle joint. Talus posterior gliding stimulates the afferent pathway of the mechanical receptors around the ankle joint, which enhances talocrural articulation and afferent information in the surrounding tissues. Applying taping in the inferior posterior direction for talus posterior gliding increased ankle dorsiflexion in patients with limited dorsiflexion and improved static balance in patients with chronic stroke. The talus-stabilizing strap attached to the dorsal part of the AOW developed in this study probably functioned similarly to the taping used in previous studies, as inferior posterior gliding of the talus in a weight-bearing posture may assist ankle dorsiflexion.
Conclusions
Our results showed that the use of AOW led to immediate effects on static balance in patients with stroke compared to those with bare feet. The use of UD-Flex AFO did not show any immediate effects on static balance in comparison with the bare-foot condition. However, further studies on the effects of dynamic balance and gait should be conducted to clinically suggest the use of AOW for stroke patients with foot drop.
Jung-Hoon Lee is a researcher in the Department of Physical Therapy of the College of Nursing, Healthcare Sciences and Human Ecology at Dong-Eui University in Busan, Korea.
Im-Rak Choi is a researcher in the Department of Rehabilitation Therapy in the Sports Exercise Therapy Center of Good Samsun Hospital in Busan, Korea.
Hyun-Su Choi is a researcher in the Department of Biomedical Health Science in the Graduate School of Dong-Eui University in Busan, Korea.
This article is excerpted from “Immediate Effects of Ankle–Foot Orthosis Using Wire on Static Balance of Patients with Stroke with Foot Drop: A Cross-Over Study,” by the same authors which appeared in Healthcare 2020;8:116; doi:10.3390/healthcare8020116. Its use is per the Creative Commons License 4.0; editing has occurred, and references have been deleted for length considerations.








How do you get one