By Windy Cole, DPM, CWSP
Surgical site dehiscence is one of the most commonly reported complications seen post-operatively. Surgical wound dehiscence (SWD) is defined as the separation of the margins of a closed surgical incision that has been made in skin, with or without exposure or protrusion of underlying tissue, organs, or implants.1 In essence, a wound dehiscence is a result of breakdown of the surgical site. Defined as either partial, with only the superficial layers of tissue exposed, or complete, with all wound layers separated. Since the inherent durability of a newly formed skin incision is essentially zero, the skin edges are typically coapted with some form of temporary closure such as sutures or staples. At one week after the surgery, the tensile strength across an incision is only 3% of that of uninterrupted skin. This figure increases to 20% by the third week when remodeling begins and to 80% after three months.2 Skin fixation allows for the disrupted tissue to heal and reestablish structural and functional integrity during this time period. It is most common to see a dehiscence occur within 4 to 14 days after surgery.2 It has been well-established that SWD contributes to increased patient morbidity and mortality as well as overall increases in health care costs.3 Prolonged clinical courses have been associated psychosocial stressors on individuals and their families.3
A variety of factors can increase a patient’s risk for developing a post-op dehiscence. Patients 65 years or older have an increased risk of developing a wound dehiscence due to the compromised tissue repair mechanisms seen in aging skin.4 Patients who are malnourished or have weakened immune systems due to chronic disease states such as diabetes, AIDs, renal disease, PAD, obesity, hypertension and cancer are at increased risks for complication in wound healing.4 Gender also has been shown to influence the rate of SWD, with men experiencing a higher higher rate of dehiscence than women.4 Patient behaviors can also contribute to the

Figure 2. Radiographs show middle phalanx is fragmented with extensive soft tissue swelling of the second toe, no air in tissues, and distal tip of the distal phalanx not well visualized, findings consistent with osteomyelitis.
occurrence of SWD. Patients who smoke or abuse alcohol have a higher rate of SWD.4 Local stress to the wound site as seen with strenuous exercise, heavy lifting, and ambulation can also play a role in SWD development. Poor surgical technique, surgeon experience, emergency surgical procedures, prolonged OR time, over-tightening of sutures, or inappropriate fixation cannot be overlooked.4 Infection is one of the largest factors contributing in SWD.4 Many foot and ankle amputations are a direct result of severe infection or necrosis. It only stands to reason that these patients would be at an increased risk for developing post-amputation SWD.
Despite increases in knowledge relative to the process of wound healing, SWD is still a major contributing factor to increased hospital stays, prolonged healing, and re-operation rates which result in higher healthcare costs and resource utilization. Patients are inconvenienced and quality of life is also disrupted due to delays in return to employment, limitations in activities of daily living, and social isolation. Given the vast number of potential sequelae related to SWD, an ounce of prevention may indeed be worth a pound of cure. Herein the author presents a case of a toe amputation where a novel adhesive suture retention device (HEMIGARD ARS; SUTUREGARD Medical, Inc.; Corvallis, OR) was used to augment surgical incision closure.
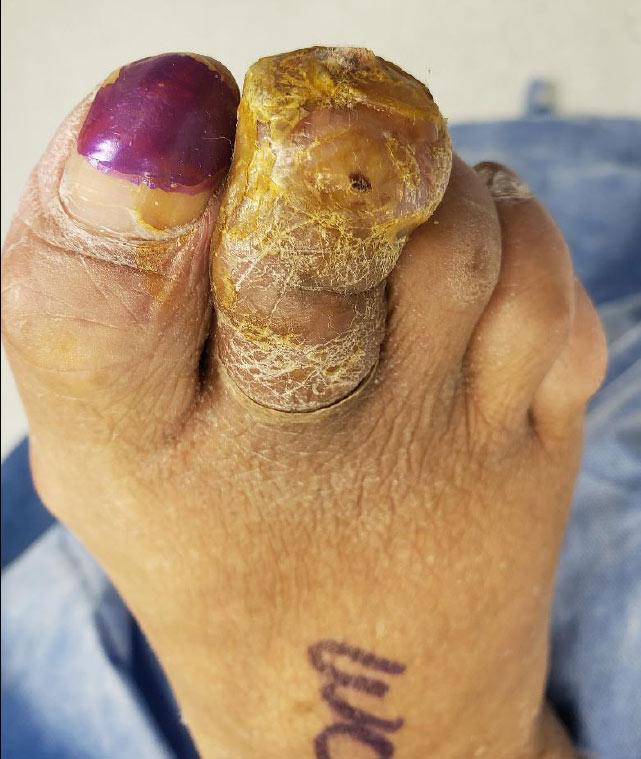
Case Report
A 60-year-old female, with a 7-year history of type 2 diabetes mellitus presented to the wound care center seeking a second opinion for a non-healing right second toe wound. Her complete past medical history includes peripheral neuropathy, osteoarthritis, non-Hodgkin’s lymphoma, hypertension (HTN), and peripheral vascular disease (PVD). She had been seen by another clinic where she was instructed to paint the wound with betadine. She had also completed 3 rounds of different oral antibiotics within the 6 weeks the wound had been present. The patient was concerned that the wound was not progressing, and her toe was extremely swollen (Figure 1). Upon initial exam there was scant drainage noted on the bandage, no malodor present, the toe was warm to the touch, significant edema, there was fluctuance of the tissues with palpation, no pain was elicited due to advance peripheral neuropathy. ABI was 1.02 on the limb. Radiographs were ordered with the results showing that the middle phalanx is fragmented with extensive soft tissue swelling of the second toe. No air in tissues. The distal tip of the distal phalanx is not well visualized. Findings are consistent with osteomyelitis (Figure 2). Due to the extent of the boney destruction caused by the osteomyelitis, surgical intervention with amputation of the second toe was determined to be the best option.
Patient was taken to the operating room and placed on the table in a supine position. A pneumatic ankle tourniquet was applied around the right ankle, but not yet inflated. After monitored anesthesia care was established, a local block of 2% lidocaine plain and 0.5% Marcaine plain in a 50/50 mix was used to perform a traditional digital block. The foot was prepped and draped in the usual sterile manner. The pneumatic ankle tourniquet was elevated to 250mmHg. At this time, a skin marker was used to plan the double-elliptical skin incision at the level of the base of the second toe. The incision was carried through to bone with a 15-blade. Moderate purulent drainage was expressed from the surgical site. All bleeders were cauterized as needed. The toe was disarticulated at the metatarsophalangeal joint and the digit was passed to the surgical table to be sent for gross pathologic examination. The pulse lavage system was used to copiously flush the surgical site with normal sterile saline. Tissues were examined and felt to be free of infection or contaminants. A post-lavage tissue culture was then obtained.
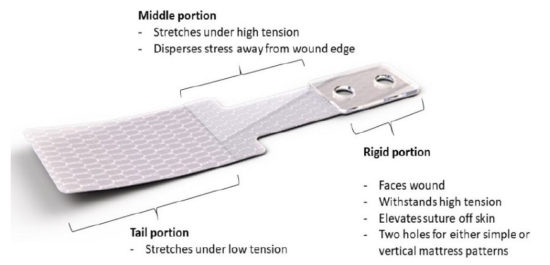
Considering the patient’s pertinent past medical history (type 2 diabetes, cancer, PVD, and HTN) she is historically at an increased risk for post-operative dehiscence. When coupled with the diagnosis of infection with underlying osteomyelitis and extensive edema, it was determined that the use of the HEMIGARD retention device would be beneficial. The HEMIGARD device is made up of 3 zones5 (Figure 3). Zone A is the water-resistant rigid, elevated wound end zone with 2 holes to accept and withstand forces of high-tension nonabsorbable simple interrupted or vertical mattress suture.5 This zone elevates the suture above the skin surface. Zone B is the less rigid, non-elevated, water-resistant middle zone that transmits force of wound closure away from the wound edge.5 Zone C is the least rigid zone with monolayer of stretchy nonwoven polyester that allows for reduction of shear forces from high-tension wound closures.5

Figure 4. At post-op visit #1, 4 days after surgery, surgical site was well coapted without evidence of dehiscence or infection. The HEMIGARD remains in place.
The deep tissues were reapproximated with 3-0 vicryl. The HEMIGARD was placed centrally across the amputation site and paired with a 4-0 prolene retention stitch. Interrupted 4-0 prolene stitches were used to coapt the remaining skin edges along the incision. In this case, the addition of the HEMIGARD to the post-amputation tissues helped to transfer tension away from the vulnerable incision site and offset the extensive edema present in order to help prevent a SWD. A dry sterile surgical bandage was applied to the foot. Patient was given a surgical shoe to aid in ambulation. She was instructed to keep the bandage on and intact and follow-up at the wound center in 4 days.
At post-op visit #1, it was noted that the bandage was on and intact. Upon removal there was slight serosanginous drainage on the bandage. No active drainage from surgical site and no malodor; there was minimal edema and slight dried sanginous drainage at skin incision. Surgical site was well coapted without evidence of dehiscence. No signs of infection noted (Figure 4). The surgical site was cleansed with normal saline solution and rebandaged with a dry bulky dressing. Patient was instructed to leave bandage intact and clean. She was reappointed for 2 weeks for follow-up. Patient was seen in clinic 17 days after the surgical amputation. The HEMIGARD and stitches were removed. The wound edges were noted to be healed with no evidence of SWD or any complications (Figure 5). Patient was transitioned into normal shoes and was able to ambulate and return to daily activities without restriction.
Conclusion

Figure 5. At post-op visit #2, 17 days after surgical amputation, the HEMIGARD and stitches were removed, and the wound edges were noted to be healed with no evidence of surgical wound dehiscence.
In summary, postoperative wound complications can be very challenging to both clinicians and patients alike. Surgical wound dehiscence typically occurs as a result of a combination of pre, intra, and postoperative factors. The management of dehisced surgical wounds requires extensive treatments such as advanced wound care dressings, antibiotic therapy, debridement, and even additional surgery. Minor SWD may be effectively treated in outpatient settings, but cases of severe SWD can require hospital admission. Given the severity of the potential sequela of SWD, surgeons should take reasonable steps to reduce the risk of these complications. The HEMIGARD adhesive suture retention device is an easy to use and effective device that can be incorporated into current surgical wound closure algorithms to prevent SWD in an at-risk patient population as demonstrated with this case report.
Windy Cole, DPM, serves as Adjunct Professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine and Student Rotation Coordinator, UH Richmond Medical Wound Center, both in Cleveland, Ohio. She is a dedicated healthcare advocate with interests focused on medical education, diabetic foot care, wound care, limb salvage, clinical research, and humanitarian efforts. Dr. Cole has published extensively on these topics and is a sought-after speaker both nationally and internationally. Dr. Cole also serves as a member of the Editorial Advisory Board for LER.
- World Union of Wound Healing Societies (WUWHS) Consensus Document. Surgical wound dehiscence: improving prevention and outcomes. Wounds Int. Feb. 20, 2018.
- Son D, Harijan A. Overview of surgical scar prevention and management. J Korean Med Sci. 2014;29(6):751-757.
- Sandy-Hodgetts K, Carville K, Leslie GD. Determining risk factors for surgical wound dehiscence: a literature review. Int Wound J. 2015 Jun;12(3):265-75.
- Chun JC, Yoon SM, Song WJ, Jeong HG, Choi CY, Wee SY. Causes of surgical wound dehiscence: a multicenter study. J Wound Manag Res. 2018;14(2):74-79.
- Roybal LL, Blattner CM, Young J, Lear W. A novel adhesive suture retention device for the closure of fragile skin under tension. JAAD Case Rep. 2020;6(2):109-114.