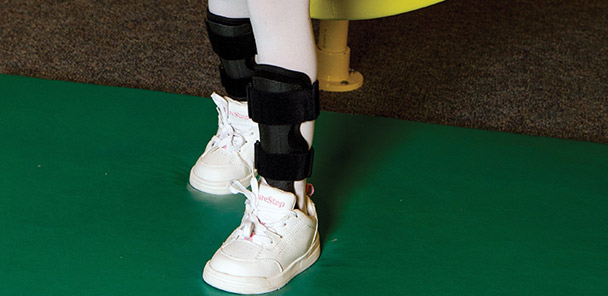
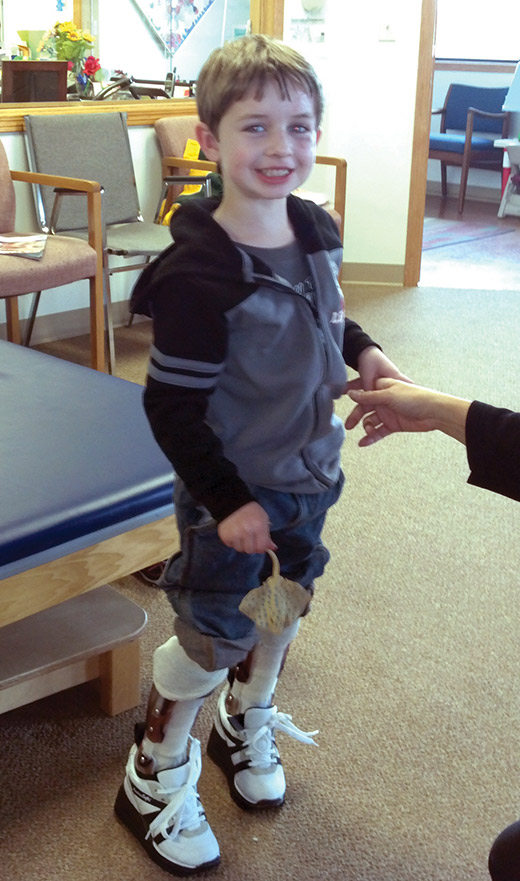
Practitioners and researchers are redefining rocking and rolling as key components of gait, and designing ankle foot orthoses and other orthotic and prosthetic devices to specifically address impairments in the way certain patients rock and roll.
By Cary Groner
This February, two related symposia at the world congress of the International Society for Prosthetics and Orthotics, in Hyderabad, India, addressed the latest thinking about gait biomechanics and the effect of ankle foot orthoses (AFOs).
Presenters discussed research and clinical considerations related to alignment and segment kinematics, provided detailed descriptions of rollover shape—how the ankle and foot create a rocker during standing, swaying, and walking—and how deficient rollover shapes can be aided by AFOs and prosthetic devices. They also discussed the relationship between AFO and prosthetic design, and conferred about device types and designs in the context of individual patients’ needs. Finally, and not insignificantly, they did their best to quiet a stubbornly quacking electronic duck. (More about this later.)
Alignment
“We were partly trying to get across the linkage between orthotics and prosthetics, and the importance of alignment,” said Elaine Owen, MSc, MCSP, a pediatric physical therapist at the Child Development Center in Bangor, North Wales, UK.
Owen specializes in children with neurological diseases, particularly cerebral palsy, and presented in both sessions.
“You have to understand the foot, shank, thigh, pelvis, and trunk to make sense of normal and pathological gait,” she continued. “The symposia were about how all that is important, and about how to put pathological gait right with orthotics and prosthetics.”
This approach includes understanding the nature and function of rockers.
“You have to get the rockers right to produce normal foot and shank kinematics in gait,” said Owen. “You can do that with a fixed ankle—even with a fixed ankle and a fixed MTP [metatarsophalangeal] joint—as long as you use the right alignment of the segments and the joints, and the right shoe profiles.”
Owen draws a distinction between joint alignment and segment alignment; the former is the spatial relationship between the skeletal segments that constitute the joint, whereas the latter is the relationship between the two ends of any given segment (e.g., the foot, shank, or thigh).
“It’s all about how distal segment alignments dictate proximal segment alignments,” she said.
In practical terms, such insight helps researchers and clinicians analyze gait and modify either AFOs or prosthetic devices accordingly.
“The shank is reclined relative to the vertical at initial contact, then moves [through stance phase] to an inclined position,” Owen continued.
She emphasized, however, that the shank doesn’t maintain the same angular velocity throughout stance. Instead, it slows in midstance, where it is typically inclined 10° to 12°.
 “If you’re treating a child who is learning to walk, or an adult with a neurological problem, you have to replicate that normal shank kinematic and reproduce that stable midstance position,” she explained.
“If you’re treating a child who is learning to walk, or an adult with a neurological problem, you have to replicate that normal shank kinematic and reproduce that stable midstance position,” she explained.
According to Owen, many clinicians still teach standing with an aim toward keeping the shank vertical relative to the floor. Unfortunately, this makes balance more difficult. Instead, she said, the goal should be to recreate the slight forward lean that arises naturally during normal walking.
“That ten- or twelve-degree incline puts the knee over the middle of the foot,” she explained. “That makes a stable base for standing because you can easily sway. Then, having created the conditions for stable standing and swaying, you can move to small steps, which is what children do when they’re learning to walk. After that, you can move to full gait cycles, with the first, second, third, and fourth rockers.”
Owen believes the gait cycle is accurately described as comprising four rockers rather than three.1,2 In this view, at the first rocker position, the heel hits the ground and the shank is reclined; at the second, the foot is flat and the shank is angled slightly forward (inclined); at the third, the heel rises and the weight comes to the base of the metatarsals as the ankle remains stiff; and at the fourth, the ankle plantar flexes as the foot is further elevated and pushes off from the metatarsals to propel the walker forward.3
Walking and standing
In presenting her findings, Owen described which alignment factors in an AFO-footwear combination (AFO-FC) help create the most efficient second rocker.
“In the children with CP we’ve studied, the range of shank-to-vertical angles of the AFO-FC is ten to fifteen degrees, with a mean of ten to twelve degrees,” she said. “That’s when the AFO-FCs are considered tuned, when they’re optimal. Patients who walk with insufficiently inclined shanks at temporal midstance normally do well in that ten-to-fifteen degree range.”
Owen noted that patients with stiffness in the knees and hips may need more midstance inclination from the AFO-FC, meaning a shank-to-vertical angle ranging from 15° to 19°.
“That’s a lot, but to get proper shank alignment, you have to get enough inclination that they can get the thigh vertical during stance,” she explained. “If you can do that, and get the trunk vertical, then you can get your center of mass where you need it. These distal alignments you create using AFOs dictate those proximal effects.”
Owen once had an epiphany about such matters while watching a woman learn to tightrope-walk in a park. The woman inclined her shank, put her knee over the middle of her foot, then carefully placed the other foot in front and transferred her weight.
“If you have a child with a neurological problem, one who has never learned to walk, that’s how you have to approach it,” Owen said. “Keep the foot flat on the floor, really stable, have the shank inclined ten to twelve degrees and keep it dead still, then take your step and move. The thigh goes from reclined to inclined so you get the ground reaction force vector in front of the knee and behind the hip, which stabilizes both joints. By aligning the center of mass, you don’t have to use muscles. The most important thing to the body is that the foot and the shank have normal kinematics; the ankle has to adjust to get those right.”
Patients who find standing balance difficult need a stable platform, however, and in such cases the flat part of the shoe’s sole may be 110% of the shoe’s length.
“If you combine that with the right alignment of the shank, you can produce very stable standing, but you won’t be able to walk very far because it’s too stable,” Owen said.
If the children improve, the clinician can create a rocker to help produce heel rise at the right place in the gait cycle.
“To start walking, you reduce the stable base to perhaps eighty-five percent of the shoe length, with a small rocker at the front; that lets you produce stable steps with a little bit of heel rise. It’s all about manipulating heel and toe levers, and how they link, to prevent or promote heel rise.”
Owen noted that this is one realm in which her work with AFOs differs from that of prosthetists, in that the latter often use rounded, rocker sole shapes.
“Those are fine if you’re able-bodied and you know how to walk—say, if you’ve had an amputation,” she said. “But if you’re a child with a neurological condition and have never learned to walk, or if you’re an adult who has had a neurological event such as a stroke, then those rounded rocker shapes aren’t stable enough.”
Rocking out
Studying and achieving such rocker effects was the subject of a presentation by Andrew H. Hansen, PhD, who is director of the Minneapolis VA Rehabilitation Engineering Research Program and associate professor of physical medicine and rehabilitation at the University of Minnesota.
“In the symposium, we discussed how able-bodied people walk, and focused on the effective rocker shapes we make when we walk,” Hansen said.
Hansen explained that an effective rocker involves the whole lower-limb system; the foot, ankle, and knee are subsystems examined for clinical and research purposes, but they all work together.
“We’ve seen that able-bodied people make a very nearly circular rocker shape when we walk, and what’s interesting is that it doesn’t change if we walk faster or slower, or if we carry weight,” Hansen said.4,5 “When we play around with the rocker radius on the shoe, ankle motion changes dramatically so that the overall rocker shape remains the same.”6,7
Hansen explained that the primary rollover shapes—foot, ankle-foot, and knee-ankle-foot—are described by transforming data about center of pressure of the ground reaction force (GRF) into coordinate systems for the foot, shank, and leg, respectively. For example, researchers can place markers on the shank to establish coordinates that rotate sagittally with leg movement, to determine the ankle-foot rollover shape.8
When individuals are walking, the radius of the shape is about a third of leg length, according to Hansen. But when people stand and sway, the rollover shape is flatter, with a radius roughly equal to the person’s height. The center of mass remains at the waist in either case, of course, so standing is inherently more stable.
“We’ve been able to use this information about rollover shape to make low-cost prosthetic feet that closely mimic the rolling properties of the natural foot and ankle,” Hansen said. “We hope to be able to design a prosthesis that can switch modes between walking and standing, because it needs to be a little stiffer for standing and swaying.”
Hansen’s examination of subsystems has clinical implications for the amputee population. For example, a patient with a below-knee amputation would require a prosthesis consisting of the ankle, foot, and shoe, so the clinician would focus on ankle-foot rollover shapes. In those with an above-knee amputation, the clinician should consider how the prosthetic knee will affect rollover shapes.
“We’re looking at these shapes and trying to use them to help us design better prostheses, to try and mimic those [natural rollover] shapes,” he said. “We can also use them to evaluate current components, to see how well they mimic the natural shapes.
Synthesis
Researchers have also used rollover shape to study the effectiveness of AFOs.9,10 The author of several such studies—and a collaborator of Hansen’s—is Stefania Fatone, PhD, BPO(Hons), a research associate professor of physical medicine and rehabilitation at Northwestern University’s Feinberg School of Medicine in Evanston, IL. At the ISPO conference, Fatone helped tie together the work by Owen and Hansen in addition to discussing her own.
“Andrew’s done a lot of work establishing what rockers look like in normal, able-bodied people, so we can use that as a basis for design evaluation of prosthetic feet,” she said. “Elaine often uses solid AFOs on her patients, which create stability and better alignment, and protect the foot from damage. But they also remove the ability of the ankle and foot to contribute to creating the rocker needed for forward progression during walking, so you have to replace that in some way. That’s typically done with an AFO-footwear combination—an AFO-FC—so we can make specific and deliberate modifications to the footwear to enhance the function the child gets from the overall system.”
In her own research, Fatone is examining the rollover shapes exhibited by patients with pathologies such as stroke and CP, and how orthotic devices affect them.
“In my presentation, I wanted to show how you could take Andy’s rollover shape analysis and apply it to quantify the techniques Elaine uses, to show how her clinical methods may be achieving similar goals,” Fatone said. “I showed a little bit about what AFOs do to the rollover shape in stroke patients, and some preliminary analysis of data from a child with CP.”9,11
She noted that in stroke patients, neuromuscular impairment often leads to an equinovarus foot posture, so that the patients make contact with the ground either with the foot flat or with the forefoot.
“They’re not getting a heel-toe gait, and you really need that if you’re going to create a good rocker for forward movement,” she explained. “That equinovarus foot posture leads to a reverse thrust in the lower limb; it’s actually pushing you backward. But when you put an AFO on those patients, you do a pretty good job of restoring heel-toe gait and reducing the reverse thrust.”
In her research, Fatone used articulated AFOs with a 90° plantar flexion stop to make sure the heel was the first part of the foot to contact the floor.9
“That moves the center of pressure back behind the ankle at initial contact, which allows improved forward progression,” Fatone continued. “We do a pretty good job of improving rollover shape with that kind of AFO, but we don’t fully restore it, because we’re not doing anything to correct the terminal part of stance at the third and fourth rockers.”
According to Fatone, Elaine Owen is determining how to affect those third and fourth rockers, as noted above, via her sole shapes.
“With the CP child we saw quite a lot of improvement in the rollover shape when we used the tuned AFO-FC, compared to the untuned, nonarticulated AFOs the children had at the beginning of the study,” Fatone said.11
The AFO-FC approach has as its fundamental biomechanical goal the control of segment kinematics.
“Instead of just trying to control ankle movement or position, I’m really interested in what the body is doing above the foot. What’s the tibia doing? What’s the thigh doing? We’re trying to create a foundation about which those two segments can move more normally,” she said. “Ideally, you look at the ankle angle as one unique component, and the shank angle as a separate component, and tune the segment kinematics using a dynamic alignment process. The footwear becomes an integral part of that system, and we need to get better at harnessing it.”
One problem with the analyses performed so far, she noted, is that they haven’t been adequately systematic. Researchers haven’t taken one AFO and modified it incrementally; rather, they’ve changed the whole system.
“It’s hard to know if the improvements we’re getting are because the rigidity of the system has improved, or if it has to do with alignment of the orthosis, or if it’s due to the shoe, or if it’s from a combination of all these,” she said. “We need to conduct studies that allow us to tease out what the relative contribution of all the different design elements might be.”
Another issue is how well the research in children with CP will translate into patients with other conditions such as poststroke impairment.
“Although CP and stroke are different, there’s a lot of similarity in the fundamental biomechanics of standing and walking,” she said. “Again, though, all of these devices are custom. If you build twenty AFO-FCs, they’ll all be different. We’re trying to develop an understanding of basic biomechanical principles, but the orthotist has to pull all the components together in the right way for that individual patient.”
The treatment goals are the same, in any case—better gait biomechanics and safer, more efficient ambulation with lower risk of falls.
“The diagnosis isn’t the thing that gets you there; it’s what impairments you want the orthosis to address,” she said.
New designs
Researchers are developing other AFO designs to address issues related to rocker function. For example, at the second ISPO symposium, Sumiko Yamamoto, PhD, of the International University of Health and Welfare in Tokyo, discussed first rocker and presented information about an oil damper AFO that was developed in 2006 and is now used by more than 20,000 Japanese patients.12
“The AFO with an oil damper [AFO-OD] controls heel and foot contact,” she told LER via email. “It facilitates smooth weight shift to the paretic limb and changes the ankle joint angle at the beginning of the second rocker function. In stroke patients, the activation of the dorsiflexors is difficult, so the AFO-OD assists with that. It generates resistive force to prevent rapid plantar flexion in loading response. The resistance of the oil damper shows the largest value just after initial contact and decreases during loading response, a resistance pattern that’s similar to the activity of the dorsiflexors.”
Yamamoto and her colleagues have used the AFO in clinical applications, research, and gait training of stroke patients.
“The ankle joint of the AFO-OD moves to plantar flexion gradually in loading response, thus it does not push the shank excessively forward,” she wrote. “Physical therapists and orthotists can adjust the amount of resistance during gait training. This is important, because with excessive resistance, patients show instability at the knee joint, and with insufficient resistance, they show hyperextension of the knee joint.”
Yamamoto noted that the new AFO has limitations; it doesn’t work well in patients with very limited walking ability, for example, so in those cases she and her colleagues use knee-ankle-foot orthoses (KAFOs) for gait training. On the other hand, the AFO-OD appears to have a wide range of clinical applications.
“It was developed for stroke patients, but we’ve found that it improves the gait of patients with other diseases such as incomplete spinal cord injury, spina bifida, and peripheral nerve paralysis,” she wrote.
Is there a quack in the house?
During the second symposium, Elain Owen set an alarm on her iPad to let her know when she had a minute left to speak. The alarm, as suggested earlier, emitted the sound of a loudly quacking duck.
The quacking startled everyone when it began, but Owen quickly discovered that she couldn’t turn it off. People in the audience began to laugh, and the laughter spread. Owen, flustered, put the iPad in the corner, but it kept quacking, and by then everyone, including the presenter, was laughing so hard it was impossible to go on.
In this match, ultimately, Australia defeated Wales: Stefania Fatone (originally from Melbourne) strode forward, grabbed the iPad, and escorted the unruly duck out into the hall.
Cary Groner is a freelance writer in the San Francisco Bay Area.
1. Perry J. Normal and pathologic gait. In: Hsu J, Michael J, Fisk J, eds. AAOS Atlas of Orthoses and Assistive Devices. 4th ed. Philadelphia: Mosby Elsevier; 2008.
2. Owen E. The importance of being earnest about shank and thigh kinematics, especially when using AFOs. Prosthet Orthot Int 2010; 34(3):254-269.
3. Owen E. From stable standing to rock and roll walking. Presented at International Society of Prosthetics and Orthotics 2013 World Congress, Hyderabad, India, February 2013.
4. Hansen A, Childress D, Knox E. Rollover shapes of human locomotor systems: effects of walking speed. Clin Biomech 2004;19(4):407-414.
5. Hansen A, Childress D. Effects of adding weight to the torso on rollover characteristics of walking. J Rehabil Res Dev 2005; 42(3):381-390.
6. Hansen A, Childress D. Effects of shoe heel height on biological rollover characteristics during walking. J Rehabil Res Dev 2004; 41(4):547-554.
7. Wang C, Hansen A. Responses of able bodied persons to changes in shoe rocker radius during walking: changes in ankle kinematics to maintain a consistent rollover shape. J Biomech 2010; 43(12):2288-2293.
8. Hansen A. The quest to improve rocker effects in O&P. LER 2010;2(4):35-39.
9. Fatone S, Hansen A. Effect of ankle-foot orthosis on rollover shape in adults with hemiplegia. J Rehabil Res Dev 2007;44(1):11-20.
10. Fatone S, Sorci E, Hansen A. Effects of clinically prescribed ankle-foot orthoses on ankle foot rollover shapes: a case series. J Prosthet Orthot 2009;21(4):196-203.
11. Fatone S. “Rocking with Orthotics.” Presented at International Society of Prosthetics and Orthotics 2013 World Congress, Hyderabad, India, February 2013.
12. Yamamoto S, Masako F, Tadashi Y. Change of rocker function in the gait of stroke patients using an ankle foot orthosis with an oil damper: immediate changes and the short-term effects. Presented at International Society of Prosthetics and Orthotics 2013 World Congress, Hyderabad, India, February 2013.