 Despite excellent subjective outcomes following Achilles tendon repair, significant plantar flexion and dorsiflexion strength deficits often persist. However, modern trends in postoperative rehabilitation represent a progression toward a more functional strength recovery.
Despite excellent subjective outcomes following Achilles tendon repair, significant plantar flexion and dorsiflexion strength deficits often persist. However, modern trends in postoperative rehabilitation represent a progression toward a more functional strength recovery.
By David A. Porter, MD, PhD, Kirk Cleland, MD, and Angela M. Rund, MEd, ATC
Achilles tendon injuries are common in the athletic population, both at the recreational and professional levels, and their incidence may be increasing.1,2 Most tendon ruptures occur in individuals aged between 20 and 50 years. Patients with a traumatic rupture can typically be divided into two groups: the “weekend warrior” athletes in their 30s to 50s and active, well-conditioned athletes in their 20s.3
Acute Achilles tendon injuries are seen more frequently in sports that require explosive acceleration or maximal effort, such as basketball, baseball, tennis, softball, and football. Although the optimal treatment for Achilles tendon ruptures remains controversial, a number of studies suggest operative repair in conjunction with an aggressive rehabilitation program commonly results in a quicker return to sports and work, less calf atrophy, decreased occurrences of rerupture, and fewer strength deficits than nonoperative treatment.4-12
Despite these potential advantages of surgery, patients often experience a deficit in plantar flexion strength and varying degrees of dorsiflexion strength after a repair, compared with their uninjured side.13 Thus, though operative repair seems to result in a gastroc-soleus complex that functions more like the preinjury tendon or the uninjured contralateral side, strength and power deficits still exist.
Surgical vs nonsurgical treatment
After treatment of Achilles tendon rupture, the goal of most patients is a full recovery of both preinjury strength and fitness. Early studies evaluating strength found no significant difference between strength achieved by surgical or nonsurgical treatment. Nistor evaluated 105 consecutive patients with a closed acute rupture of the Achilles who were assigned randomly to surgical or nonsurgical treatment.14 Patients were followed for one to five years after injury and evaluated clinically with static and dynamic measurements of plantar flexion strength. In the operative group, strength in the injured leg was 83% of the uninjured leg; in the nonoperative group, the injured limb had 79% of the strength of the contralateral limb.

Figure 1. Setup for dorsiflexion and plantar flexion isokinetic testing used after Achilles tendon rupture treatment. Patient is placed prone with straps over the calf and around the foot to secure the foot to the dynamometer.
In a prospective randomized multicenter study by Moller et al, 59 and 53 patients with Achilles tendon rupture were randomized to either surgical treatment followed by early functional rehabilitation using a brace or to nonsurgical treatment (ie, eight weeks of plaster treatment), respectively.15 Investigators recorded results for each patient of isokinetic muscle strength evaluation for contractions in the concentric and the eccentric mode, plantar flexion and dorsiflexion, two angular velocities, and three different positions. They also administered the heel-raise test for endurance and measured maximum calf circumference and tendon width.
Researchers found a very high rerupture rate of 20.8% in the nonsurgically treated group; the rerupture rate in the surgically treated group was 1.7%. They noted no significant differences between the treatment groups in isokinetic strength measurements or the endurance test among the patients who did not sustain a rerupture, which averaged between 78% and 90% of the strength on the uninjured side. Muscle function, however, was not restored after two years in either group, and at two years the number of single-leg toe raises patients could do using the injured leg was, on average, still less than half the number for the uninjured side in both operative and nonoperative groups. Researchers concluded that, if a rerupture is avoided, both surgical and nonsurgical treatments for Achilles tendon rupture produce good functional outcomes.
Inglis et al presented 79 patients with rupture of the Achilles, 48 of whom were treated surgically and 31 nonsurgically.16 With one exception, all were healthy athletic individuals. The patients treated surgically were more satisfied with results of their treatment. Strength, power, and endurance as measured on the Cybex II dynamometer revealed the patients treated nonsurgically attained only 72% of the strength and 70% of the power and endurance that the surgically treated patients achieved.
Jacobs et al evaluated maximum static force between operatively and nonoperatively treated Achilles tendon ruptures and noted that strength in the injured versus uninjured limb was 75% in patients with a surgically repaired Achilles compared with 65% in the nonsurgical group; a higher percentage of the surgical group (70%) had an excellent outcome in return-to-activity and motion measures than in the nonsurgical group (56%).17
In a recent study, Willits et al randomized 144 patients with acute Achilles tendon rupture to surgical or nonsurgical treatment (each group had 72 patients).18 Rerupture occurred in two patients in the operative group and in three patients in the nonoperative group. There was no clinically important difference at one and two years after injury between groups in strength, range of motion (ROM), calf circumference, or Leppilahti score, a disease-specific functional outcome measure. It includes patient ratings of pain, stiffness, calf muscle weakness, footwear restrictions, ROM, and satisfaction as well as objective measures of strength to arrive at an overall score on a 100-point scale, in which 100 is the best possible score.19
This study differed from others comparing operative and nonoperative treatment in that the rehabilitation protocol all patients underwent was an accelerated program that featured early weight bearing and early range of motion. This highlights the importance of a structured rehabilitation to maximize strength and functional outcomes in both operative and nonoperatively treated tendon ruptures.
Strength after operative repair
Several case series also have reported plantar flexion and dorsiflexion strength after operative repair. Carter et al evaluated 21 patients treated surgically after Achilles rupture.20 Sixteen patients felt they returned to their preinjury level of activity, and only one was not satisfied with his result. The average plantar flexion and dorsiflexion strength, power, and endurance of the ankles as measured by isokinetic testing revealed no significant differences between the operated leg and the nonoperated side minimum (investigators followed up with patients a minimum of two years after treatment, and average follow-up was 31 months).

Figure 2. Patient performing double heel raise more than one year after right Achilles surgical repair. Note the slightly smaller but well-defined calf size. Note also the repaired Achilles tendon is thicker but functioning well with near equal heel elevation.
Talbot et al have shown the mean plantar flexion strength is slightly increased in the operated leg at the low test speed of 30°/s, and that subsequent deficiencies in the operated leg were then noted at the greater test speeds.21 However, Leppilahti et al have reported a reduced deficiency at higher speeds (ie, 11%, 10%, and 2% muscle strength deficiency on the operated side at test speeds of 30°, 90°, and 240° per second, respectively).19 Several studies also have shown improved plantar flexion and dorsiflexion strength after utilizing an accelerated ROM and physical therapy protocol.6,22 Meaningful meta-analyses are difficult to perform with so many variables and so much heterogeneity among studies.
In most studies, researchers have performed strength assessment and strength return using only a short bout of isokinetic peak torque measurement. It’s not known if this measurement correlates well with return of strength over a prolonged period that occurs during exercise. We recently evaluated the effects of acute exercise and fatigue on strength assessment and strength return after surgical treatment of Achilles tendon injury at least 12 months postrepair.23 We wanted to know if the operatively treated Achilles tendons fatigue at the same rate as the uninjured extremity, if torque return previously reported reflects muscle recruitment that can hold up with prolonged exercise, and if the brain develops a pattern of use to “favor” and “protect” the involved extremity that leads to prolonged deficits and atrophy.
We evaluated strength, endurance, and fatigue for both the involved and uninvolved extremity after 30 minutes of acute exercise at 70% maximum exertion using the Borg Rating of Perceived Exertion Scale. For peak torque, the involved ankle performed significantly worse in plantar flexion and exerted only 85% of the uninvolved ankle’s strength. When looking at the effect of exercise, the involved ankle was significantly weaker in the plantar flexion post-test at 60°/s; the uninvolved ankle was significantly stronger than the involved surgically treated ankle after exercise in the plantar flexion post-test at 180°/s.
No significant differences existed between the involved and uninvolved ankle in dorsiflexion. For all strength measurements, both the involved and uninvolved ankles fatigued at statistically equivalent rates, despite the differences in raw strength value. Calf circumference decreased by 4.7% (a 1.9-cm difference between limbs), which is similar to the results of Marti et al, who reported an average decrease of 1.5 cm.24 The smaller circumference was not a result of a lengthened Achilles tendon, because dorsiflexion ROM in the involved and uninvolved ankles was similar. Instead, this reduction in size indicated a smaller muscle mass and a decrease in peak muscle torque, which corresponds to a decrease in plantar flexion strength on the involved side.
An under-recognized problem may be weakness in end-range plantar flexion. This impairment would affect descending stairs, running downhill, or landing from a jump. It would increase the demands on the bony structures of the foot as well as the knee joint, and have significant performance implications in sports such as basketball, volleyball, and gymnastics. Mullaney et al looked at plantar flexion strength after Achilles repair.8 Significant weakness was evident on the involved side at 20° and 10° of plantar flexion (34% and 20% deficit, respectively), with no torque deficits evident at other angles (6% at neutral, 3% at 10° of dorsiflexion, 0% at 20° of dorsiflexion). Dorsiflexion ROM was not different between the involved and noninvolved sides, but passive joint stiffness was 34% lower on the involved side. All patients could perform an incline heel rise, but 14 of the 20 patients could not perform a decline heel rise.
Despite excellent subjective outcomes after Achilles repair reported by patients, with American Academy of Orthopaedic Surgeons Foot and Ankle Module (AAOS-FAM) scores nearing 100, and despite increased emphasis in therapy on the use of the operated ankle to promote muscle recruitment and regeneration, significant strength deficits often persist.23 Most patients can return to daily activities without problems, but up to one third do not return to their preinjury activity levels.22,25 The similar amounts of fatigue experienced by both ankles represent equal functionality during sports or daily activities without a greater loss of strength over time.
One explanation for the strength differences is a change in gait kinematics and selective increased use of the uninvolved extremity with all activity. Silbernagel et al reported a case study of a patient who had been in a running analysis study one month before rupturing her Achilles tendon.26 The patient returned for repeat analysis one year after surgical repair. The investigators noted the knee joint in the involved leg accounted for 24.7% more power absorption and 10% more power generation after injury compared with preinjury levels. They also found decreased plantar flexion strength and rearfoot eversion moment in addition to increased dorsiflexion strength, peak rearfoot eversion, and abduction. These alterations suggest a change in gait mechanics for the involved leg, supporting the gait change theory as an explanation for atrophy and strength deficits.
Rehabilitation is key
Although it may be difficult to achieve full recovery of plantar flexion strength after injury to the Achilles tendon, one of the keys to maximizing strength recovery for both the recreational and competitive athlete is a detailed, focused approach to rehabilitation. Multiple studies of ligaments and tendons after injury indicate that exercise and joint motion stimulate healing and influence strength after injury.27-29
Early protected motion and resistance training encourage tendon healing and protect against disuse atrophy. Modern trends in rehabilitation after Achilles tendon repair represent a progression toward a more functional strength recovery. A functional progression, which is usually initiated three to four months after surgery, is a key element in advancing from clinical rehabilitation back into sports for both recreational and high-level athletes. Progression also breaks up the monotony of traditional rehab and allows for the recovery of functional strength in the entire lower extremity. This functional rehabilitation is what allows the body to adjust and compensate for any plantar flexion strength deficits that may exist. Whether this type of compensation is in some ways desirable or potentially prevents plantar flexion strength from returning fully unknown.
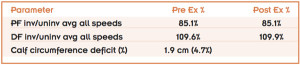
Table 1. Plantar flexion (PF) and dorsiflexion (DF) percent deficit in involved extremity compared with uninvolved extremity (inv/uninv) as measured by isokinetic dynamometer more than one year after repair of acute Achilles tendon rupture. Assessments were performed before a 30-minute bout of exercise (Pre Ex %) and after the 30-minute bout of exercise (Post Ex %) averaged over speeds of 60°/s, 120°/s, and 80°/s. (Data reported by Porter et al in reference 23.)
Return of strength is of great importance to all types of athletes. Even after recovery from Achilles tendon rupture, some runners have described their gait as similar to “running on a flat tire.” This description of a lack of spring in one’s step leads us to believe patients experience excessive dorsiflexion force upon striking the ground with a restrained amount of plantar flexion at push-off. Isokinetic testing, while not difficult to perform, may not be the optimal method for assessing return of strength, as the gastroc-soleus complex does not function at isokinetic speeds during activities of daily living or athletic activities.
Ankle fatigue during exercise, therefore, may be a more accurate assessment of functional outcome than plantar flexion strength or dorsiflexion strength alone. While more research is needed on gait mechanics and fatigue after Achilles repair, validated surveys and outcome measures indicate that persistent changes in gait mechanics and mild decreases in plantar flexion strength are not debilitating if compensated for with an aggressive functional rehabilitation program.
Key points:
- Subjective and functional recovery after an Achilles tendon repair is possible in the recreational athlete but, even with successful healing, high-level athletes can be subject to decreased performance after a tear.
- Calf size and peak plantar flexion torque is mildly decreased even after a successful repair and restoration of the normal musculotendinous length.
- Aggressive and accelerated rehabilitation supports a quicker and more robust return of plantar flexion strength after operative or nonoperative treatment.
- Calf size is on average about 5% smaller in the involved extremity than the uninvolved extremity even after successful treatment.
- An altered gait that results in high impact at heel strike and diminished push-off may be the cause of decreased plantar flexion strength after Achilles rupture treatment with normal dorsiflexion ROM.
- Care must be taken during rehabilitation to avoid over-lengthening of the Achilles muscle-tendon unit.
- Functional rehabilitation can be beneficial after complete tendon healing and allow a more normal daily activity and sports participation.
- Achilles reruptures typically occur within three months of operative treatment.
- “Primary” repair to restore normal Achilles musculotendinous length and continuity can still be achieved up to four to eight weeks after rupture with meticulous attention to proximal release, careful repair, and gradual return to normal dorsiflexion ROM.29
Future investigation
Researchers need to undertake further evaluation of the relationship between gait alterations after Achilles rupture treatment and strength deficits, loss of muscle mass, and impaired sports performance. Now that practitioners are encouraging improved surgical techniques, accelerated rehabilitation, less immobilization time, and earlier ROM, we need to develop a better understanding of the limitations of a healed tendon compared with its uninjured counterpart.
There continues to be investigation into making smaller and less complicated incisions to reduce the potential for neurologic and skin coverage and healing complications. Normal strength, safe uncomplicated healing with minimal to no risk of rerupture, and 100% functional recovery for all athletes, remains our stated but still somewhat elusive goal. Progress continues to be made, but this is an area that will continue to challenge us to work harder for our patients and the field of sports medicine.
David A. Porter, MD, PhD, is the orthopedic foot and ankle consultant to the Indianapolis Colts as well as to athletes at Indiana University in Indianapolis and Purdue University in West Lafayette, IN. He is also volunteer associate professor of orthopaedic surgery at Indiana University. Kirk Cleland, MD, is an orthopedic sports medicine fellow at Methodist Sports Medicine/The Orthopedic Specialist in Indianapolis. Angela Rund, MEd, ATC, is a clinical research assistant at Methodist Sports Medicine/The Orthopedic Specialist.
- Kujala UM, Sarna S, Kaprio J. Cumulative incidence of achilles tendon rupture and tendinopathy in male former elite athletes. Clin J Sport Med 2005;15(3):133-135.
- Moller A, Astron M, Westlin N. Increasing incidence of Achilles tendon rupture. Acta Orthop Scand 1996;67(5):479-481.
- Dugan DH, Hobler CK. Progressive management of open surgical repair of achilles tendon rupture. J Athl Train 1994;29(4):349-351.
- Henriquez H, Munoz R, Carcuro G, Bastias C. Is percutaneous repair better than open repair in acute Achilles tendon rupture? Clin Orthop Relat Res 2012;470(4):998-1003.
- Kangas J, Pajala A, Siira P, et al. Early functional treatment versus early immobilization in tension of the musculotendinous unit after Achilles rupture repair: a prospective, randomized, clinical study. J Trauma 2003;54(6):1171-1180; discussion 1180-1181.
- Maffulli N, Tallon C, Wong J, et al. Early weightbearing and ankle mobilization after open repair of acute midsubstance tears of the achilles tendon. Am J Sports Med 2003;31(5):692-700.
- McCoy BW, Haddad SL. The strength of achilles tendon repair: a comparison of three suture techniques in human cadaver tendons. Foot Ankle Int 2010;31(8):701-705.
- Mullaney MJ, McHugh MP, Tyler TF, et al. Weakness in end-range plantar flexion after Achilles tendon repair. Am J Sports Med 2006;34(7):1120-1125.
- Ozkaya U, Parmaksizoglu AS, Kabukcuoglu Y, et al. Open minimally invasive Achilles tendon repair with early rehabilitation: functional results of 25 consecutive patients. Injury 2009;40(6):669-672.
- Rettig AC, Liotta FJ, Klootwyk TE, et al. Potential risk of rerupture in primary achilles tendon repair in athletes younger than 30 years of age. Am J Sports Med 2005;33(1):119-123.
- Speck M, Klaue K. Early full weightbearing and functional treatment after surgical repair of acute achilles tendon rupture. Am J Sports Med 1998;26(6):789-793.
- Thompson J, Baravarian B. Acute and chronic Achilles tendon ruptures in athletes. Clin Podiatr Med Surg 2011;28(1):117-135.
- Bruggeman NB, Turner NS, Dahm DL, et al. Wound complications after open Achilles tendon repair: an analysis of risk factors. Clin Orthop Relat Res 2004;(427):63-66.
- Nistor L. Surgical and non-surgical treatment of Achilles tendon rupture. A prospective randomized study. J Bone Joint Surg Am 1981;63(3):394-399.
- Moller M, Lind K, Movin T, Karlsson J. Calf muscle function after Achilles tendon rupture. A prospective, randomised study comparing surgical and non-surgical treatment. Scand J Med Sci Sports 2002;12(1):9-16.
- Inglis AE, Scott WN, Sculco TP, Patterson AH. Ruptures of the tendo achillis. An objective assessment of surgical and non-surgical treatment. J Bone Joint Surg Am 1976;58(7):990-993.
- Jacobs D, Martens M, Van Audekercke R, et al. Comparison of conservative and operative treatment of Achilles tendon rupture. Am J Sports Med 1978;6(3):107-111.
- Willits K, Amendola A, Bryant D, et al. Operative versus nonoperative treatment of acute Achilles tendon ruptures: a multicenter randomized trial using accelerated functional rehabilitation. J Bone Joint Surg Am 2010;92(17):2767-2775.
- Leppilahti J, Forsman K, Puranen J, Orava S. Outcome and prognostic factors of achilles rupture repair using a new scoring method. Clin Orthop Relat Res 1998;(346):152-161.
- Carter TR, Fowler PJ, Blokker C. Functional postoperative treatment of Achilles tendon repair. Am J Sports Med 1992;20(4):459-462.
- Talbot JC, Williams GT, Bismil Q, et al. Results of accelerated postoperative rehabilitation using novel “suture frame” repair of Achilles tendon rupture. J Foot Ankle Surg 2012;51(2):147-151.
- Mandelbaum BR, Myerson MS, Forster R. Achilles tendon ruptures. A new method of repair, early range of motion, and functional rehabilitation. Am J Sports Med 1995;23(4):392-395.
- Porter DA, Barnes AF, Rund AM, et al. Acute achilles tendon repair: strength outcomes after an acute bout of exercise in recreational athletes. Foot Ankle Int 2014;35(2):123-130.
- Marti RK, van der Werken C, Schutte PR, Bast TJ. Operative repair of ruptured achilles tendon and functional after-treatment–I. Acute rupture. Neth J Surg 1983;35(2):61-64.
- Parekh SG, Wray WH 3rd, Brimmo O, et al. Epidemiology and outcomes of Achilles tendon ruptures in the National Football League. Foot Ankle Spec 2009;2(6):283-286.
- Silbernagel KG, Willy R, Davis I. Preinjury and postinjury running analysis along with measurements of strength and tendon length in a patient with a surgically repaired Achilles tendon rupture. J Orthop Sports Phys Ther 2012;42(6):521-529.
- Buckwalter JA. Activity vs. rest in the treatment of bone, soft tissue and joint injuries. Iowa Orthop J1995;15:29-42.
- Buckwalter JA. Effects of early motion on healing of musculoskeletal tissues. Hand Clin 1996;12(1):13-24.
- Burroughs P, Dahners LE. The effect of enforced exercise on the healing of ligament injuries. Am J Sports Med 1990;18(4):376-378.
- Porter DA, Mannarino FP, Snead D, et al. Primary repair without augmentation for the neglected Achilles tendon rupture. Foot Ankle Int 1997;18(9):557-564.










Excellent article. I had percutaneous Achilles repair surgery by Dr. D. Thornbury in Montgomery, AL. I am very active in sports, gym, running & basketball. At 2 wks. I was doing upper body, at 6 months I was doing a lot more already & running. At 7-1/2 (yesterday) I was released to play basketball. Thank you for this article!
hi ,i just had my achilles ankle tendon surgery ,today makes it 25 days ,to my surprise after the surgery my foot did not get swelling and i didnot fell any pains ,but to my greatest surprise was after the 14 days of my surgery my stitches was removed , and the wound was dry up with no blood but i normally had popping sounds from me foot i operated so i want to know if it is normal sometime i do heard pops sound from my operated ankle foot ,all of a sudden my foot is swollen now and i dont know if it is lack of mobilization of my foot that causes the swollen or lack of blood circulation? also it is normal after remover of stitches the operated foot will be swollen?
thanks
sunday josh
Sir,
I have Achilles tendon surgery before 6weeks.but when I ll recovery 100%
And can I run after recovery..pls reply to me sir
After 2 years I can only say “still painful” . I ruptured my Achilles playing basketball at the age of 56 it was 3.5cm separation and I required surgery. I did 9months rehab through my doctors office and have been active walking and exercising on my leg ever since. What I experience daily is extreme burning and pain in my foot and lower leg. I stretch it before, during and after my walks and exercise no improvement after 2 years. Question: How long will it take before I am minimum 90% again?
I am an 80 year old male and keep very active . Recently I suffered a bad tear . My specialist said he would not repair it because of my age saying that I could have major healing problems, that could possibly lead to an ampution .I was shocked as I do not have any history of any healing difficulties in my life.I am in a cast five days .Will my tear treatments be successful.I don’t’ want to have to give up my activities. Billy.
Achilles surgery (ruptured) was 7 days ago. Cast was installed today. Surgery went well. We hope i can bare weight and start rehab in 8 weeks from today.
I’m 65, retired, in good shape. Ruptured it while playing tennis…classic example.
Advise to all in my stage of life…stretch and strengthen before and after sports. Listen to your Dr or trainer. Don’t screw around with pain, its a sign and tells you to slow down.
As I lay here in my rented hospital bed, take my advise and then enjoy your retirement.