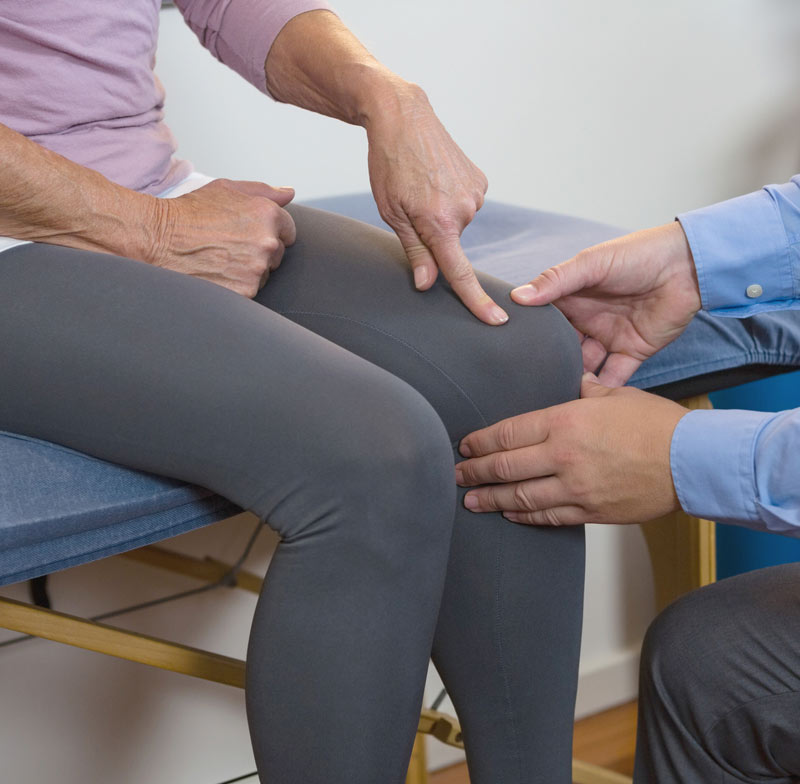
iStock #837638416
Conventional diagnostic tools may miss the hallmark features of this painful condition
By Donald C. Pompan, MD
With an aging population that is increasingly overweight, a growing number of patients present to providers with a chief complaint of “knee pain.” Successful treatment of these individuals depends on making the correct diagnosis. Conventional thinking is that knee pain in middle-aged or older patients is due to the degeneration of the articular cartilage and/or the tearing of the menisci. When such patients are referred to the orthopedist, there is generally a diagnosis of “osteoarthritis” (OA) or “meniscus tear,” with the expectation of a curative procedure based on a radiographic finding.
However, scientific evidence suggests that knee pain in middle-aged and older patients without an obvious traumatic etiology may not be in relation to intra-articular pathology. There are studies that call into question the relationship between the degree of radiographic OA and the level of knee pain.1,2 In the case of MRI, a number of studies show that degenerative meniscal tears are seen on MRI examination with increasing frequency in asymptomatic knees as individuals age and are thus not necessarily the cause of the pain.3,4
Studies have also shown that arthroscopic debridement of arthritic knees does not decrease knee pain, and this procedure is not recommended for the treatment of OA by the American Academy of Orthopedic Surgeons.5,6,7 Moreover, partial meniscectomy has been shown not to be an effective treatment in middle-aged and older patients even in the absence of OA.8,9 One study showed that patients with degenerative medial meniscal tears who underwent arthroscopic partial meniscectomy did no better than those treated with a sham operation.8 Indeed, the title of a recent JAMA article calls arthroscopic partial meniscectomy a measure of “low-value care” in older patients.9 Moreover, studies are showing that patients who do undergo partial meniscectomy are placed at increased risk of developing OA−so these procedures have the potential to be detrimental.10,11
Thus, MRI could suggest a diagnosis (“meniscal tear”) that leads to a surgical procedure that not only fails to alleviate knee pain, but may have subsequent adverse effects. How then can we identify the source of knee pain in the middle-aged or older patient who presents without a clear acute mechanism of injury without relying on potentially misleading radiographic findings?
Examine the Patient!
As one of my favorite mentors in training instructed the residents, “when in doubt, examine the patient!” It is the author’s experience that the source of knee pain in most cases can be identified by a thorough physical examination, especially in regards to palpation.
There is a subset of patients who will present with a specific injury (eg, work or sports injury) with joint pain, mechanical symptoms such as locking, possibly knee swelling, and who demonstrate specific joint line tenderness. These patients may have a clinically relevant meniscal tear and ultimately benefit from surgery.
However, most middle-aged and older patients will present with non-acute, more insidious pain suggestive of a degenerative, chronic process. In the experience of this author, these patients will commonly present with two features:
- They almost invariably have quadriceps weakness.
- They are routinely maximally tender in a specific area in the pes anserine region, which seems to be the source of the pain.
If the pes anserine area is not examined, the diagnosis may be missed. The patient may then be subject to a procedure that may not be addressing the cause of the pain. Therefore, the key is making the correct diagnosis, which begins by understanding the anatomy.
Pes Anserinus
The pes anserinus (“goose foot”) consists of the tendinous attachments of the semitendinosus, gracilis, and sartorius muscles. A bursa exists underneath these tendons, and its location has been well-described in an anatomical study.12 Pes anserine bursitis, also known as pes anserine tendino-bursitis (PATB) is a condition in which this entire area becomes inflamed.13,14 A few studies have shown that injection into the pes anserine bursa can be an effective treatment of PATB, even in the presence of OA.15,16 The challenge in making the diagnosis is knowing precisely where to palpate.
While the pes anserine bursa has been shown to occupy the bulk of the proximal medial tibia, the area of maximal tenderness is palpable with the tip of the index finger in the same specific location − slightly posterior to the middle of a line drawn between the apex of the knee flexion crease and the tibial tubercle (Figure 1). This site appears to correspond to where the gracilis and sartorius tendons converge as they begin their attachment to the tibia, as seen in the anatomical study by Lee et al.12 By locating the landmarks of the tibial tubercle and the knee flexion crease and then using deep palpation (which requires significant manual pressure in morbidly obese patients), one can reliably diagnose PATB.
In addition, all patients are checked for quadriceps weakness by manually testing the strength against resistance and assessing the ability of the patient to perform straight leg raises. All patients are instructed on a self-directed straight-leg-raising exercise program (done seated or supine) and are encouraged to do it as much as possible throughout the day (eg, when sitting at a desk working or watching television). Many patients’ pain will improve with quadriceps strengthening, which is consistent with studies that show the positive effects of quadriceps strengthening on knee pain in patients with OA.17 For those patients who do not respond to exercises and anti-inflammatory medication, injection with corticosteroid is an effective way to reduce pain.
In terms of the injection technique, the goal is to inject the bony periosteum in the area of maximal tenderness, which is consistently found in the same location, as described above. The injection is done using a 1 1/2-inch-long 22-gauge needle with an entry angle of approximately 45 degrees to the coronal plane of the tibia angling from anteromedial to posterolateral (Figure 2). Lidocaine (5cc of 1% lidocaine) in one syringe is injected into the subcutaneous and deeper layers all the way to bone (Figure 2). Then, without removing the needle, steroid (80 mg Kenalog) from a second syringe is injected around the bone (Figure 3). It should be noted that in cases in which the patient is morbidly obese, “puckering” of the tissues may be required to reach the bone (Figure 4).

iStock #948440058
Quadriceps Strengthening Prevents Recurrence
The results of this author have been in line with studies that have shown injection with corticosteroid to be an effective treatment of PATB, including patients with OA.15,16 While the problem may recur, the frequency of recurrence seems to be decreased by increasing and then maintaining quadriceps strength. There are patients, especially those with more advanced arthritis, who may require periodic injections. Those who experience only short-lived pain relief with the injection (ie, recurrence in one month or less) are considered to have failed the regimen, and other treatments are considered.
There will be a minority of patients that either do not have maximal tenderness in the specific area in the pes anserine region or do not respond to the pes anserine periosteal injections. These patients are then considered for other diagnoses and treated accordingly.
In my opinion, dependence on radiologic studies may lead a provider to misdiagnose or underdiagnose PATB. MRI identified pes bursitis in only 2.5% of patients with knee pain without OA in one study, while another showed just a 17% incidence of PATB in those with knee OA.18,19 Two studies in which ultrasonography was utilized on patients with painful knee OA found incidences of pes anserine bursitis of 8% and 20%, respectively.16,20
In contrast, one study in the literature that utilized palpation on physical examination to diagnose PATB in patients with knee OA found 46% as having PATB.21 In this author’s experience, the incidence of PATB in this patient demographic is even higher and is more common in overweight patients, especially women.22
By closely examining the pes region in all middle-aged and older patients with knee pain, this author has substantially reduced the number of arthroscopies and knee replacements. Moreover, by focusing on quadriceps strengthening, the patient becomes an active participant rather than a passive bystander in their treatment.
In conclusion, pes anserine tendino-bursitis (PATB) should be placed at the top of the differential diagnosis in middle-aged and older patients who present with knee pain without a clear, traumatic etiology. Radiological studies may identify pathology that is not the source of the pain and should not be the basis of a diagnosis. Rather, the source of pain can be identified by a physical examination that seeks to find the area of maximum tenderness, which is often found in a specific location in the pes anserine region. PATB is invariably accompanied by quadriceps weakness. The majority of patients can be successfully treated by correcting the quadriceps weakness with self-directed exercises, but some cases require a periosteal injection into the location of maximal tenderness in the pes anserine region.
Donald C. Pompan, MD, is a board-certified orthopedic surgeon, fellowship-trained in sports medicine. He has published articles on the appropriate use of MRI in assessing musculoskeletal conditions. He practices in Salinas, California.
- Hannan MT, Felson DT, Pincus T. Analysis of the discordance between radiographic changes and knee pain in osteoarthritis of the knee. J Rheumatol. 2000;27(6):1513-7.
- Bedson J, Croft PR. The discordance between clinical and radiographic knee osteoarthritis: A systematic search and summary of the literature. BMC Musculoskelet Disord. 2008;9:116.
- Englund M, Guermazi A, Gale D, et al. Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Engl J Med. 2008;359(11):1108-1115.
- Boks SS, Vroegindeweij D, Koes BW, et al. Magnetic resonance imaging abnormalities in symptomatic and contralateral knees: prevalence and association with traumatic history in general practice. Am J Sports Medicine. 2006:34(12):1984-1991.
- Kirkley A, Birmingham TB, Giffen JR, et al. A randomized trial of arthroscopic surgery for osteoarthritis of the knee. N Engl J Med. 2008;359(11):1097-107.
- Thorland JB, Juhl CB, Roos EM, et. al. Arthroscopic surgery for degenerative knee: systematic review and meta-analysis of benefits and harms. BMJ. 2015;350:h2747.
- Jevsevar DS. Treatment of osteoarthritis of the knee: evidence-based guideline, 2ndedition. J Am Acad Orthop Surg. 2013;21(9):571-576.
- Sihvonen R, Paavola M, Maimivaara A, et al. Arthroscopic partial meniscectomy versus sham surgery for degenerative meniscal tear. N Engl J Med. 2013;369(26):2515-24.
- Stahel PF, Wang W, Hutfless S, et al. Surgeon practice patterns of arthroscopic partial meniscectomy for degenerative disease in the United States: A measure of low-value care. JAMA Surg. 2018;153(5):494-496.
- Englund M, Lohmander LS. Risk factors for symptomatic knee osteoarthritis fifteen to twenty-two years after meniscectomy. Arth & Rheum. 2004;50(9):2811-2819.
- Papalia R, Del Buono A, Osti L, et al. Menisectomy as a risk factor for knee osteoarthritis: a systematic review. British Med Bull. 2011;99(1):89-106.
- Lee JH, Kim JK, Jeong YG, et al. Pes anserinus and anserine bursa: anatomical study. Anat Cell Biol. 2014;47(2):127-131.
- Moshkowitz E. Bursitis of sartorius bursa: An undescribed malady stimulating chronic arthritis. JAMA. 1937;109(17):1362-1366.
- Larsson LG, Baum J. The syndrome of anserina bursitis: an overlooked diagnosis. Arthritis Rheum. 1985:28(9):1062-1065.
- Sarifakioglu B, Afsar SI, Yalbuzdag SA, Ustaömer K, Bayramoğlu M. Comparison of the efficacy of physical therapy and corticosteroid injection in the treatment of pes anserine tendino-bursitis. J Phys Ther Sci. 2016:28(7):1993-1997.
- Yoon HS, Kim SE, Suh YR, et al. Correlation between ultrasonographic findings and the response to corticosteroid injection in pes anserinus tendino-bursitis syndrome in knee osteoarthritic patients. J Korean Med Sci. 2005;20(1):109-112.
- Imoto AM, Peccin MS, Trevisani VFM. Quadriceps strengthening exercises are effective in improving pain, function, and quality of life in patients with osteoarthritis of the knee. Acta Ortop Bras. 2012;20(3):174-9.
- Rennie WJ, Saifuddin A. Pes anserine bursitis: incidence in symptomatic knees and clinical presentation. Skeletal Radiol. 2005;34(7):395-398.
- Kim IJ, Kim DH, Song YW, et al. The prevalence of periarticular lesions detected on magnetic resonance imaging in middle-aged and elderly persons: a cross-sectional study. BMC Musculoskelet Disord. 2016;17:186.
- Uysal F, Akbal A, Gokmen, et al. Prevalence of pes anserine bursitis in symptomatic osteoarthritis patients: An ultrasonographic prospective study. Clin Rheum. 2015;34(3):529-33.
- Kang I, Han SW. Anserine bursitis in patients with osteoarthritis of the knee. South Med J. 2000;93:207-9.
- Pompan DC. Pes anserine bursitis: An underdiagnosed cause of knee pain in overweight women. Am Fam Phys. 2016;93(3):170.