By Barbara Boughton
When I first entered my podiatrist’s office for treatment of a moderately painful case of plantar fasciitis, I never thought that healthcare for my feet could get complicated. I subsequently developed sesamoiditis and my podiatrist prescribed custom orthotics for both my foot conditions. But then came the clincher: one night, I fell down a short flight of stairs and unfortunately landed on my foot.
The next day, my foot was swollen and had turned various shades of purple and black and I learned that I had a broken bone—the fifth metatarsal, a bone that can be difficult to heal.1
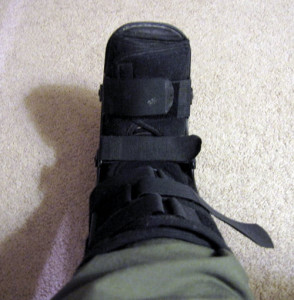
My podiatrist is a fast talker. He provides explanations at every visit, but in a rapid fire manner. So at first I wasn’t sure if he was giving me enough information, particularly when the bone did indeed prove difficult to heal and I was spending months in a walking boot.
Yet as time went on—I spent eight months in that boot and underwent ultrasound bone stimulation therapy—I realized that my podiatrist was providing good explanations of my treatment, with anatomical diagrams that explained the underlying biology of my broken bone and discussion of the pros and cons of various therapies. He also invited me to phone with any follow-up questions, and usually returned these calls within a day.
Since the medical care for my whopping three foot conditions –plantar fasciitis, sesamoiditis, and a broken bone—was so extended, the whole experience made me curious about how other lower extremity clinicians educate their patients. After interviewing practitioners, I’ve found that there are some basic guiding principles for good patient education, although providers may sometimes have different approaches.
Explaining the pain
In my own case, my podiatrist explained that the fifth metatarsal is often difficult to heal, because a strong tendon nearby tends to pull the bone apart. If the bone did not heal, there were other therapies to try such as ultrasound and surgery, he noted. This helped explain why I was in a boot for so long, and the fact that there were other therapies helped reassure me. But at about the six-month point—when my bone was showing signs that healing was not taking place as it should—I was getting exceedingly grumpy about wearing the boot!
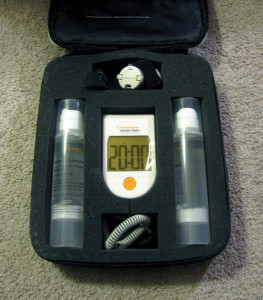
At six months, a computed tomography scan showed that, though there was healing in most of my fifth metatarsal, there was one small section where the bone did not seem to be knitting together again. Thus I was prescribed an ultrasound bone stimulator for use at home.
Before prescribing the therapy, my podiatrist explained the choices open to me: more time in a cast, the bone stimulator, or surgery. I was not exactly enthused about spending more time in a cast or having surgery, and an at-home ultrasound machine seemed a safer bet to me. My podiatrist explained that the bone stimulator had fewer risks than surgery, and though it often worked for patients with broken bones, recovery with it was not a sure thing.2 Surgery was probably more reliable and would work more rapidly to fix my ailing metatarsal, but there were also risks, including the possibility of infection or that the surgery might not be successful.
Luckily the bone stimulator did work, and my poor fifth metatarsal showed enough signs of healing on an x-ray to allow me to walk without my ever-present boot, crutches, or cane at the eight-month point. However, I was still experiencing residual pain.
At that point, I was walking pretty well and the pain was mild. The good news was that I was not troubled by my plantar fasciitis because of the orthotic devices I wore. The mild pain was most likely due to the fact that the tendon near my fifth metatarsal had weakened after months in a cast, my podiatrist said.
However, he warned me that once I returned to regular shoes, I might experience a recurrence of sesamoiditis. He had adjusted my orthoses to cushion the area under the balls of my feet even before I sustained the fracture. Occasionally after I started walking without the boot, I had mild sesamoiditis discomfort, depending on how supportive my shoes were, but this occasional mild pain was easily addressed with additional over-the-counter pads placed under the balls of my feet, as recommended by my podiatrist.
But two months after the bone stimulation, the pain had not resolved and seemed to be escalating with increased activity. At that point, my podiatrist ordered magnetic resonance imaging (MRI). He was concerned about the possibility of damage to the tendon near the broken bone—perhaps a tear—or that the bone’s healing was delayed. The MRI revealed a small central area in the bone that
hadn’t healed, as well as injuries to a nearby tendon. After a consultation with my doctor, I decided to schedule surgery for my fifth metatarsal bone. It will involve placing a screw in the area that hasn’t healed, strengthening the bone.
The MRI also revealed damage to a tendon nearby, so I’m now undergoing physical therapy, which has helped lessen the pain. And I’m actually looking forward to my surgery! That may seem odd, but surgery is my best chance of strengthening the bone for good, as my podiatrist explained. I’ll wear a surgical shoe for two weeks, and then a removable cast/boot for six weeks. But after that, I will be able to throw that cast to the back of my closet–I hope, for good.
Educational initiative
My patient experience has been long and sometimes frustrating for me. I’m sure other patients have similar lengthy and sometimes complex medical care, but, according to the clinicians I interviewed, good patient education can make the experience a lot easier.
Yet patient education is often a highly individual process that can depend on the patient’s medical condition and the prescribed treatment, according to Judith Baumhauer, MD, professor and associate chair of orthopedic surgery at the University of Rochester School of Medicine and Dentistry in Rochester, NY. Baumhauer is also the past president of the American Orthopaedic Foot and Ankle Society.
There are some diagnoses for which exercise at home can be critical to patient recovery, for instance.
“For plantar fasciitis, there are stretching exercises that have been shown to be between 80 and 90 percent effective,” she said.
In a 2006 study published by Baumhauer and colleagues in the Journal of Bone and Joint Surgery, 77% of 66 patients who went through a plantar fascia stretching program for eight weeks in a prospective randomized clinical trial reported no limitation in physical activities two years later. Likewise, 94% of the patients showed a significant decrease in pain compared with symptoms they experienced before the stretching program began.3
“[In our practice] we have a plantar fascia stretching sheet that shows a stretch shown to be effective in clinical trials. We have a description of the stretch on the University of Rochester Medical Center foot and ankle home page and patients can download it as a PDF,” Baumhauer said.
When considering more aggressive interventions (such as surgery), Baumhauer always discusses with the patient the extent to which they have not responded to nonoperative treatments, such as foot orthoses and exercise, and their level of pain during exercise and daily activities.
“For someone who has failed other treatments and has daily walking pain, surgery might be a good choice. But for someone who can walk comfortably but has exercise-induced pain, surgery might not be always be the best option, because surgery may not get you back to your previous exercise ability anyway. For a patient who only has exercise-induced pain, I tend to focus on nonoperative options,” she said.
When a patient has a fracture, the alignment of the bones and the stability of the fracture are two important guidelines in deciding whether to perform an operation, Baumhauer said.
There is important information for practitioners to share with patients when surgery is being considered, she noted. It’s crucial to tell a patient what the outcome of surgery is likely to be—whether that’s pain relief, greater mobility, or healing of a fractured bone. The risks of surgery should always be discussed with a patient, including outcomes such as nerve injury, wound healing problems, and infection risk, she added.
A clinician should also advise a patient about what the postoperative recovery will be like, including how long immobility might last, so they can plan to recruit relatives or friends for assistance with daily tasks or hire someone to help if needed. The question of physical therapy also needs to be addressed, Baumhauer noted. Before surgery, her patients undergo assessment by a physical therapist to determine what kind of assistive device (such as walkers, crutches, or even a wheelchair) they may need to keep load off their foot following surgery.
For podiatrist Larry Huppin, DPM, of the Foot and Ankle Center of Washington in Seattle, good patient education also means making enough time during a patient visit to answer questions. He also refers patients to handouts on his practice’s website.
“We’ve been referring patients to our website since 1996, and today, since so many patients are Internet savvy, a majority of them do use information from our website,” he said.
It’s important that the doctor-patient visit not be rushed, Huppin says. To ensure that, he makes sure his staff is well-trained so that they can usher patients in and out of the office in a timely manner. Yet he also makes sure he and his staff provide patients with enough time and information for a thorough discussion of any treatment plan. The clinician also has to make time for and encourage questions concerning the pros and cons of various therapies or surgeries, including their benefits and risks, he noted.
When a patient is not responding to treatment, of course, then medical management can become more complicated.
“Sometimes generalized difficulty with medical issues such as a healing of a broken bone may require a further work-up, perhaps a test for osteoporosis,” Baumhauer said. “Or if a bone isn’t healing we have to ask: Is it a metabolic bone issue or a stability problem?”
In cases in which the bone doesn’t heal, a bone graft surgery can be performed, she said. But it is quite common for patients to experience delayed healing in the fifth metatarsal, as I did, she added.
Although I spent eight months in a cast, I’m told the fifth metatarsal actually doesn’t heal completely for a year. And certainly spending that many months in a cast has its price—not only in terms of the activities you can’t participate in during that time, but also the pain that can occur with walking once the cast is removed if nearby tendons or muscles have weakened.
And so, as I begin my physical therapy and exercise program, I’ll certainly remember that breaking the fifth metatarsal is not an experience one wants to repeat. My podiatrist has emphasized that once a bone breaks, it’s easier to break it again, particularly before it has fully healed.
After surgery, there’s likely to be more physical therapy and an exercise program for me. Yet I’m actually looking forward to the chance to exercise again after surgery, to walk without pain, and to be able to walk the trails of Lake Merritt in north Oakland, CA, where I live.
Finally, no more dress pumps for me! Although they didn’t contribute to my accident, the fashionable heels that I used to enjoy are just too likely to result in a fall that could mean another painful broken bone. Instead, I’m aiming for a pair of low-heeled strappy sandals, with a firm sole, or ones in which my orthoses will slide right in. Who says patients never learn?
Advising patients about orthoses and dress shoes
For most patients, custom dress shoe inserts can be costly. Although foot orthoses designed for walking shoes or athletic shoes are usually covered by insurance, many dress orthotics are not.
Yet patients do need and want to wear dress shoes, but many can’t afford the out-of-pocket cost for a custom dress orthosis. What’s the solution? Many dress orthoses sold in drugstores provide little pain relief, but there are other over-the-counter dress orthoses that can help prevent foot pain, according to lower extremity clinicians interviewed by LER.
First, it’s important to counsel patients about the importance of selecting a dress shoe that provides good support for the feet and has some cushioning in the insole, according to Judith Baumhauer, MD, professor and associate chair of orthopedic surgery at the University Rochester School of Medicine and Dentistry in Rochester, NY. Baumhauer is also the past president of the American Orthopaedic Foot and Ankle Society.
“For some women’s dress shoes, particularly those with a heel, it’s very difficult to fit in an orthotic that will cure the patient’s problem. If a patient has a shoe that is wide enough and has no pitch, as well as a cushioned insole, he or she might not even need an orthotic. What we often do is glue pads [such as metatarsal pads or arch supports] into a dress shoe because it’s hard to fit in anything else,” Baumhauer said.
Baumhauer also cautions people against foot inserts created by machines in drugstores, based on pressure points in the foot.
“The pressurized mats on those machines only capture a moment in time, not the pain that can result after waking or exercising. Inserts created this way are not really customized for a patient’s individual diagnosis,” she said.
One option for summer dress shoes are sandals in which the insoles can be removed and orthotics put in their place, she said. Other good dress shoes are Mary Jane-style clogs with good arch support.
High-end shoe stores also sell quality over-the-counter inserts that can be used for dress shoes, according to Larry Huppin, DPM, a podiatrist at the Foot and Ankle Center of Washington in Seattle and medical director of Prolab Orthotics.
“I tell patients that a good prefab orthotic is fairly rigid and not too soft. Patients with a high arch also need arch support, as well as a good heel cup,” Huppin said.
Barbara Boughton is a freelance health and medical writer based in the San Francisco Bay Area.
- Darabos N, Obrovak K, Knez N, et al. Combined surgical therapy and orthotic management of stress and tuberosity avulsion fractures of the fifth metatarsal bone: A case report. J Am Podiatr Med Assoc 2009;99(6):529-535.
- Hemery X, Ohl X, Saddiki R, et al. Low-intensity pulsed ultrasound for non-union treatment: a 14-case series evaluation. Orthop Traumatol Surg Res 2011;97(1):51-57.
- Digiovanni BF, Nawoczenski DA, Malay DP, et al. Plantar fascia-specific stretching exercise improves outcomes in patients with chronic plantar fasciitis. A prospective clinical trial with two-year follow-up. J Bone Joint Surg Am 2006;88(8):1775-1781.