By Patrick DeHeer, DPM
By Patrick DeHeer, DPM
The COVID-19 pandemic’s profound effect on the healthcare system will produce a ripple across all healthcare industry sectors, including podiatric medicine and surgery. Some of these changes are obvious and currently taking place, and many are still to be determined.
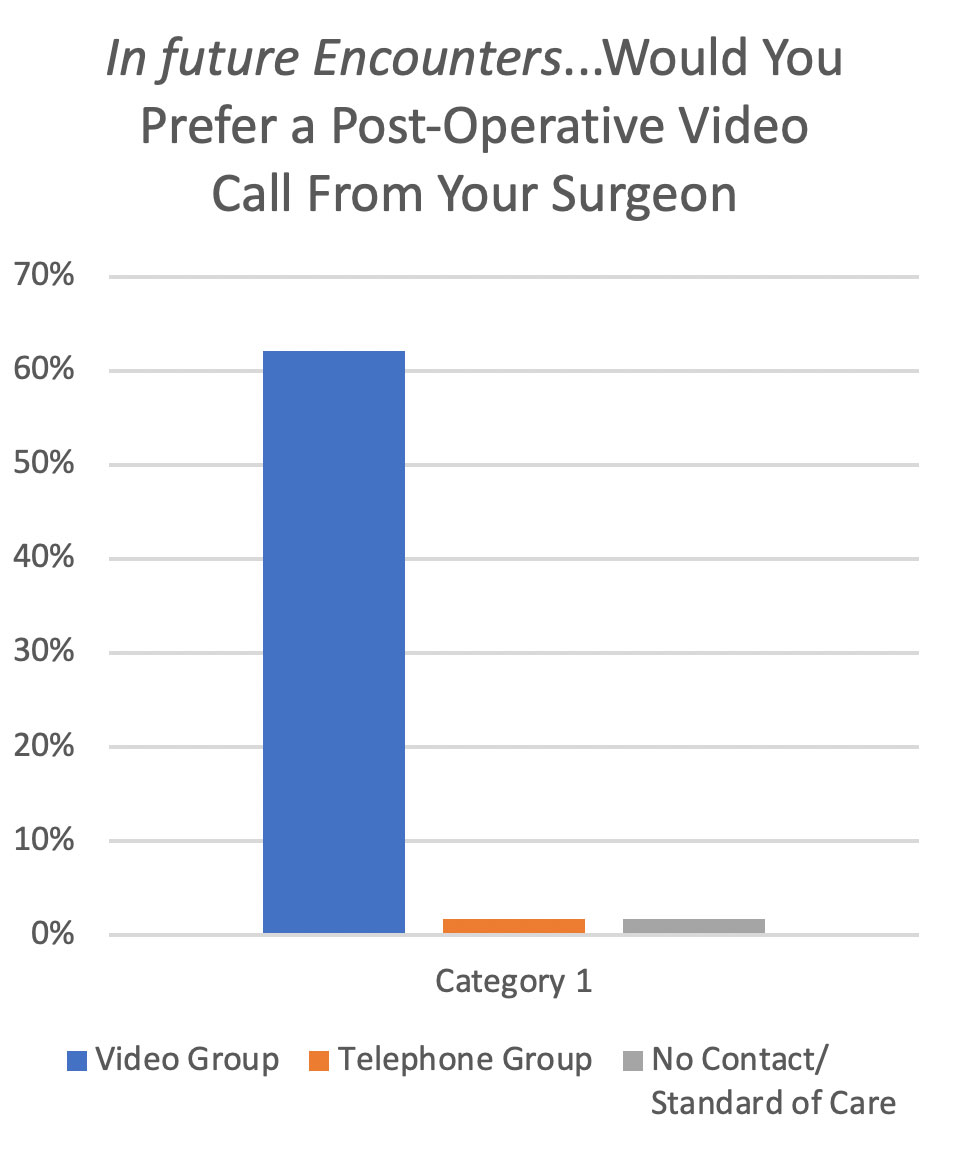
Patients and physicians are both comfortable with telemedicine for multiple types of encounters. A recent study in The Journal of Bone and Joint Surgery by Kingery and colleagues demonstrated the power of postoperative telemedicine appointments.1 Patient satisfaction rates were significantly higher with virtual visits. I incorporated postoperative telemedicine visits the day after surgery in my practice, and I will never go back to phone calls. Although telemedicine has limitations in podiatric medicine, opportunities exist to increase the use of this technology for patient convenience and provider productivity.
Another area in healthcare that will be forever changed post-pandemic is continuing education for practicing physicians and post-graduate medical education for podiatric residents. Numerous potential benefits exist for educational opportunities, including access to many previously not routinely accessible speakers at lower costs and more convenience. I participated as a speaker for numerous virtual conferences during the pandemic, and the virtual platform allowed me to participate without missing days from the office. As the Continuing Education Chair for the Indiana Podiatric Medical Association, I invited speakers to participate who would not have been able to otherwise. Their virtual participation helps reduce conference expenses, especially critical for smaller organizations (like state associations) trying to put on top-tier conferences on a limited budget.
A glaring negative resulting from the pandemic was the microscope placed on the disparities in healthcare access for underserved populations. A bold strategy for a national initiative to address these inequities consisting of collaboration between healthcare providers, politicians, and insurers must occur. Podiatric physicians can and should be part of the conversation.
The pandemic reinforced my desire to be a physician, not a business owner. I was in the process of selling my practice to Upperline Health during the pandemic. The sale closed in October 2020, relieving me of numerous administrative tasks and worries. Instead, I now concentrate on what I do best, patient care and educating both residents and students. Solo practice or small group practice models continue to decline, but the pandemic expedited the transition, in my opinion.
As a small business entrepreneur, the impact of the COVID-19 pandemic on our company, IQ Med, was significant. The sales of The Equinus Brace™ took approximately a year to rebound to pre-pandemic sales. I am sure the effect on medical supply companies was like our experience, with the noted exception of personal protective equipment sales.
Collateral damage from the pandemic was a pause on high-level research. The ramifications from the disruption of research will affect all of medicine. It is important for residencies, fellowships, and podiatric medical schools to prioritize high-level research to keep the field up-to-date and to be able to attract new recruits.
There is no doubt that the pandemic created a paradigm shift in healthcare. The opportunities coming out of the pandemic to reimagine healthcare are abundant. The time is now to use the lessons learned to change healthcare to reach our highest ideals.
Patrick DeHeer, DPM, is now Medical Director at Upperline – Indiana and Podiatric Residency Director at Ascension St. Vincent Hospital in Indianapolis.
- Kingery MT, Hoberman A, Baron SL, et al. Day-of-surgery video calls and phone calls increase patient satisfaction with outpatient surgery experience: a randomized controlled trial of postoperative communication modalities. J Bone Joint Surg Am. 2021;103(3):243-250.