Clinicians may find the EdUReP theoretical framework provides helpful guidance for exercise prescription and load management for patients with this potentially disabling condition.
By Talysha Reeve, B.App.Sc.(Podiatry), GradCertClinRehab
Despite the substantial gains in knowledge and understanding of lower extremity tendinopathies in recent years, achieving successful treatment outcomes for those suffering posterior tibial tendon dysfunction (PTTD) often remains a challenge for many therapists. A number of histological and mechanical factors unique to the tibialis posterior (TP) tendon exist and an improved understanding of these factors may improve the management strategies we as practitioners implement for our clients.
The literature regarding inclusion of exercise-based therapies in the management of individuals with lower extremity tendinopathies is growing at a rapid pace. For many clients with PTTD the provision of orthomechanical devices and/or passive therapies alone is not sufficient to successfully manage their condition. In this article we will explore how the inclusion of exercise-based therapies can improve pain and function in those with Stages I and II PTTD.
Posterior tibialis tendon dysfunction is a progressive, often disabling condition and is the most common cause of adult acquired flatfoot deformity (AAFD). PTTD can affect both men and women; however, it is most common in women and the incidence increases with age, with an estimated prevalence of between 3.3% and 10%. Women over age 40 are considered to be at the highest risk of developing this condition.1,2,3
A number of inherent problems exist when it comes to the treatment of PTTD.
First, it is reported that PTTD is often misdiagnosed by health care practitioners or remains undiagnosed for several years, during which time a patient may progress through a number of stages of the pathology. Tendonitis, ankle sprains, and arthritis are some of the most common misdiagnoses given to this condition. Second, should a correct diagnosis be made in due course, inadequate or incorrect treatment interventions may be implemented due to a failure to understand the complex structural and functional components unique to this pathology in terms of both etiology and treatment.1,4 Late diagnosis and/or inadequate intervention can significantly limit the efficacy of conservative management and increase the likelihood of requiring surgical intervention.1,4

Republished with permission of MA Healthcare, from Bodill C, Concannon M. Treatments for posterior tibial tendon dysfunction. Practice Nurs. 2012;23(8):389-394; copyright © 2012.; permission conveyed through Copyright Clearance Center, Inc.
Functional Anatomy, Physiology, and Pathomechanics
To understand how we are to improve our management of the pathology in relation to both mechanical intervention and exercise therapies, we first have to understand the structure and function of the muscle-tendon unit in both its healthy and pathological states.
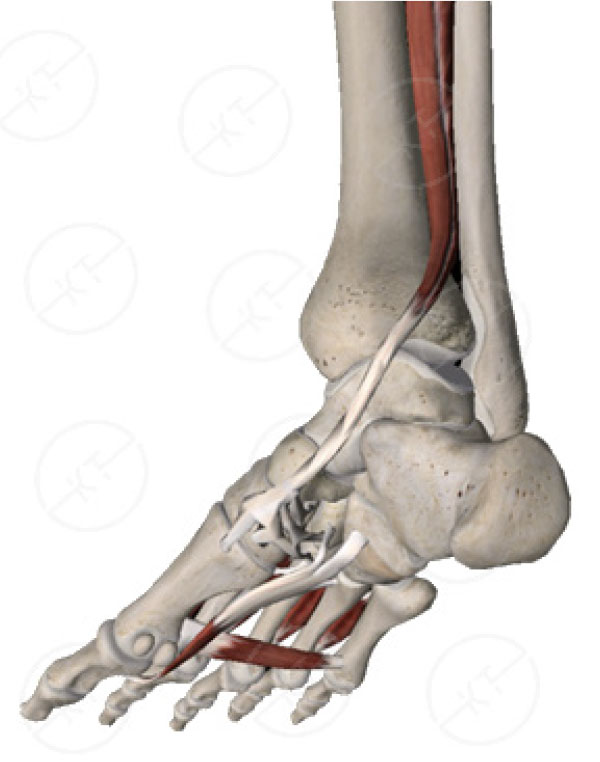
The tibialis posterior originates from the posteromedial surface of the fibula, posterolateral surface of the tibia, and the interosseous membrane. The muscle-tendon junction is located within the distal third of the calf; the 12-15cm long tendon then flattens and courses behind the medial malleolus to a number of insertions located within the foot. Its most superficial insertions are located on the tuberosity of the navicular and the medial cuneiform. The deeper insertions are located on the plantar aspects of metatarsals 2-4 and the intermediate cuneiform. 5
The TP tendon is considered a gliding tendon and variations exist both biomechanically and histologically from traction tendons (eg, Achilles tendon). Unlike traction tendons, gliding tendons change course and are not in line with their associated muscle fibres. When movement of a gliding tendon occurs, high levels of compressive force exist at the interface with the osseous gliding area. For the TP tendon to withstand these loading forces, 2 structural variations exist: the tendon flattens in the retromalleolar region and it contains high level of fibrocartilage. Previously thought to be pathological, this relatively hypovascular region of fibrocartilage is now considered a normal physiological and protective component of the TP tendon.5-9
As we move superficially away from the gliding area, compressive forces decrease and we observe an increase in tensile forces, with the highest level of tensile force existing at the most superficial aspect of the tendon. It is within the tensile and compressive force transition zone that we see the highest presence of shear stress. Compressive and shear forces have been identified as a potential contributor to degenerative tendon pathology. Despite their low level of vascularization comparative to other connective tissues, tendon vascular supply is considered sufficient to meet metabolic demands in tendon tissue free from pathology. However, due to the combination of potentially increased pathological stress and high concentrations of hypovascular fibrocartilage in this region, we may see a tendon that develops degenerative tendinopathy due to inadequate healing time before damaging forces are reapplied.5-9
Load is a key element in the development of tendon pathology and is further influenced by a range of both intrinsic and extrinsic factors such as age, genetics, body composition, biomechanics, and training characteristics.10,11 Table 1 summarizes the identified causative and risk factors for developing PTTD.
Unlike a number of other lower extremity tendon pathologies TP load is closely linked with the biomechanical function of the foot. Subtalar joint (STJ) axis, low arch height ratio, and increased foot mobility have been identified as factors that may lead to the development of TP tendon pathology.12,13
Tibialis posterior energetics are heavily influenced by the STJ axis, which has implications for both the development and management of PTTD.
The Role of the Subtalar Joint Axis
The TP has the largest supination moment around the STJ and serves a number of mechanical functions during locomotion including: dissipative or elastic energy absorption, contributes to mediolateral stability of the STJ, actively resists STJ pronation during early stance, and actively supinates the STJ during late stance.18, 21
The length of the TP supination moment arm is dependent on the location of the STJ axis (see Figure 2). In a normally located STJ axis, the TP moment arm is approximately 2.0cm on average. Those with a medially deviated STJ axis may have a moment arm <1.0cm. Higher degrees of pronation resulting from a medially deviated axis result in an increase in TP tendon forces, increasing the risk of tendon injury. 12,14-17
Physiologically normal tendons are composed of 95% of collagen type I with very small amounts of types III, IV, and V collagen. In the presence of tendinopathy, we see alterations in collagen synthesis and tendon remodelling. Gonçalves et al performed a histological study on those suffering PTTD compared to controls.18 Although the study had a relatively small sample size, those with PTTD displayed significantly higher proportions of collagen type III (53.6%) and V (26.4%) and a decrease of more than 40% in collagen type 1. Unlike collagen types III and V, the primary function of type I collagen is to tolerate tensile loads. This altered collagen organization and composition may expose the TP tendon to further injury due to the decreased capacity to tolerate and adapt to mechanical load.8,18-20
The continuum model of tendon pathology first proposed by Cook & Purdam in 2008 describes 3 stages of tendon pathology: reactive tendinopathy, tendon disrepair, and degenerative tendinopathy. A tendon may move up and down this continuum through the addition or removal of load. A reactive tendon has an increased likelihood of the tendon structure returning to normal. Tendons in stages of disrepair or degeneration have a limited ability to remodel and return to a normal tendon structure. However, interventions that address load capacity, function, and pain can potentially deliver a pain-free tendon with an acceptable level of function despite the remaining cellular structure deficits.10,21
How a tendon may reach the point of disrepair can be partially understood when we look at Young’s elastic modulus (see Figure 3), which describes the stress-strain curve and its relation to tendon loading.
Stress (compressive, tensile, and shear) refers to the loading force acting on the structure, divided by cross-sectional area.
Strain is the deformation or displacement of the structure as a result of the applied stress.
The stress-strain curve sees 3 primary regions. The elastic region, whereby the structure returns back its original shape upon the removal of load. The plastic region is where the structure has reached its elastic limit and we see an increase in strain (load-deformation) relative to stress, increasing risk of partial tearing or rupture. The final region is the rupture point in which we observe a complete failure of the structure.
 Injured ligaments and tendons that have reached the plastic deformation region will see an increase in cellular strain on the remaining intact tissue, resulting in an increased risk of further deformation and injury. This is one factor that may explain the accelerated progression of PTTD once plastic deformation of the tendon and associated ligamentous structures has occurred. 8,22-24
Injured ligaments and tendons that have reached the plastic deformation region will see an increase in cellular strain on the remaining intact tissue, resulting in an increased risk of further deformation and injury. This is one factor that may explain the accelerated progression of PTTD once plastic deformation of the tendon and associated ligamentous structures has occurred. 8,22-24
A steep slope in relation to stress-strain indicates a higher degree of tissue stiffness and will undergo a lower rate of load-deformation. Inversely, a shallow slope indicates a higher level of compliance and will experience a higher rate of load-deformation. In regard to the tibialis posterior tendon, a more compliant tendon will absorb more energy allowing for greater pronation in comparison to a stiffer tendon and may result in progressive damage to the tendon structure over time.13,22
The TP tendon’s function and pathology are influenced by a complex interrelationship of factors, some of which are unique to this structure alone. Table 2 provides a summary of the structural and mechanical factors that often require attention for the successful conservative management of PTTD.
Conservative Treatment Interventions
Conservative mangement is recommended for those in Stages I and II of PTTD. Often those who have progressed in to Stages III and IV require surgical intervention in addition to orthomechanical and physical therapy to address the numerous structural and functional deficits present.
Davenport et al recommends the EdUReP (Education, Unloading, Reloading, Prevention) theoretical framework for the clinical management of individuals with tendinopathies.25
Education
Client expectations, their treatment compliance, and the engagement of positive behavioral changes are all built upon a foundation of education and understanding. All of these factors are critically important for achieving successful treatment outcomes with those suffering PTTD.
It is recommended that a client has a thorough understanding of: the etiology, pathophysiology, and individual biomechanical factors associated with their condition; importance of load management; importance of treatment compliance; and implications of non-adherence.4,26
Unloading
The goal of unloading is to preserve the structural integrity of the affected structures, allow for adequate healing, and prevent further progression of PTTD. This can be achieved via a number of methods depending on the individual’s needs, including activity limitation, use of foot orthoses (FO)/ankle foot orthoses (AFO), heel lifts, and footwear changes/modifications.
Rest can be as simple as reducing aggravating activities, such as running, through to short-term immobilization when active tenosynovitis or partial tendon tears are present. Periods of immobilization required range from 2-12 weeks depending on the clinical presentation.27
Foot orthoses are considered appropriate when the plantar ligamentous structures – and therefore the foot-leg coupling mechanics – are intact. When we clinically observe a disruption in the coupling mechanics between the foot and the leg, the prescription of an AFO device (eg, Ritchie Brace) over a functional FO is recommended.
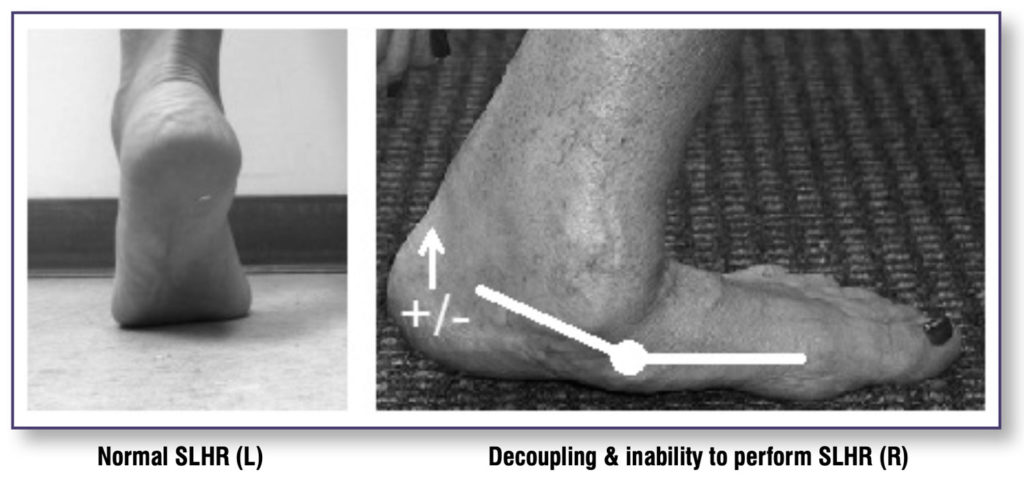
When combined with a thorough subjective history and objective assessment, the single leg heel raise (SLHR) test is an effective functional test that may assist clinicians in selecting the most appropriate orthomechanical device and serve as a starting point for exercise therapy interventions. Depending on the stage of PTTD, clinicians will observe a number of movement variations when the patient is performing this test with or without the presence of pain.

Figure 5. Exercises for managing posterior tibialis tendon dysfunction: A) Calf isometric; B) Calf raise with tibialis posterior activation; C) Isolated loading tibialis posterior.
In the early stages, a client will be able to perform the SLHR, and we will observe a diminished or the absence of calcaneal inversion, indicating TP insufficiency (see Figure 4). As the pathology progresses a decrease in heel raise height will occur, further progressing to decoupling of the foot-leg and eventual inability to perform the SLHR.
When the plantar ligamentous structures are intact, we will observe the relative maintenance of the medial longitudinal arch and plantarflexion of the entire foot. In those with disrupted plantar ligaments we observe the rearfoot plantarflex relative to the forefoot.5,28
The use of FO or AFO can be enhanced by selecting the appropriate footwear. Motion-control shoes that include medial posting, reinforced heel cups, and a stiff shank are generally considered appropriate footwear for those with PTTD. When managing more athletic clients, cross-training shoes may be beneficial over other sports shoes due to the improved hindfoot control.30
Should standard retail shoes be insufficient, orthopedic footwear allows for a high degree of customization and additional areas of support, including: medial flares, medial posting, extended Thomas heel, navicular supports, and reinforcement of the medial heel counter.27
Reloading
The evidence supporting exercise therapies for tendon pathologies has risen significantly in recent years with a small number of studies relating to PTTD specifically. We know that various exercises can facilitate collagen repair and increase tendon stiffness or compliance. Exercise selection should be based on the individual’s presentation, their individual goals, and the desired physiological response. As with the management of all tendinopathies, there will be significant variation regarding exercise selection, therapeutic dosage, and the treatment response among clients.
For a tendon to positively adapt, we are required to load the tendon within its anabolic range. Too much or too little load and we may further increase the catabolic changes occurring within the tendon structure.23 Further to tendon loading, the repeated long-term exposure time to load has a profound impact on collagen synthesis. It is theorized that the initial stages of training increases collagen type I turnover to allow for reorganization of the tissue. When the tissue is exposed to more prolonged, repeated bouts of training greater than 4 weeks, we begin to see changes in the strength and cross-sectional area of the tendon structure.29 The 2008 systematic review conducted by Ross et al found small-to-moderate improvements across outcome measures at 6 weeks.3 However, a greater number of outcome measures achieved significant improvements when reviewed again at 12 weeks. Previously, Alvarez et al had reported 89% of participants achieved significant improvements in pain and function after participating in the daily exercise loading program after 4 months.31 Understanding and communicating to your client that the rehabilitation of tendons can take months is important when devising and implementing your treatment plan.
Exercise Therapies for Conservative Management
Despite the small number of studies in relation to exercise therapies for the conservative management of PTTD, we are able to see that those who participate in exercise-based therapies improve across a range of outcome measures. Overall, eccentric exercises appear to create the biggest improvements across the range of outcome measures, however concentric exercises and stretching exercises all appear to have a positive impact when compared to no exercise intervention at all.
The confounding factor for many clinicians is the selection and dosage of exercises as there are no established protocols. Due to the unique presentation of each client, exercise selection and the overall management plan should be based upon their individual needs and the results of their individual assessment.
Strength and functional deficits have been identified in the gastroc-soleus complex, tibialis posterior, tibialis anterior, peroneals, gluteals, and lateral hip stabilizers in those individuals with PTTD. Targeted strengthening of these muscles in addition to functional strengthening, balance, and proprioceptive exercises have been shown to have positive impacts on pain and function for the management of PTTD.3,4,26,27,31,32
As discussed previously, in order for positive adaptation to occur we must load the target structure within its anabolic range. Limiting exercises to non-weight bearing or to low-load resistance band exercises may leave the client ‘under-dosed’. As the foot is subject to loads up to 1.5 x body weight during walking, exercise dosing must aim to progressively restore the structures to a point where they are able to tolerate the required loading demands.23 To facilitate an increased activation of the TP, have a client perform their rehabilitation exercises wearing their prescribed foot orthoses; use of supportive shoes may assist.26
A range of both bilateral and unilateral weight-bearing exercises can be incorporated into the rehabilitation of PTTD. Figure 5 provides examples of exercises that may benefit an individual with this condition.
As ankle equinus resulting from shortening of the Achilles tendon is a common finding in those with PTTD, stretches that aim to improve ankle dorsiflexion range of motion (ROM) are routinely prescribed. The inclusion of gastrocnemius and soleus stretching exercises that place the ankle in maximal dorsiflexion ROM may be counterproductive to the treatment goals in some cases. Understanding that the PT tendon experiences high degrees of compressive load as it courses behind the medial malleolus, the prescription of maximal range calf stretches may flare symptoms and/or lead to further damage of the tendon by the additional compressive loading. The addition of calf stretches may be included once acute symptoms have subsided.3,27
In summary, we can identify a number of factors that highlight the need for the combination of load management and exercise-based therapies for the successful management of Stage I and II PTTD. As tendon structures require repetitive exposure to high loads within their anabolic threshold in order to positively adapt, the application of orthomechanical devices and/or passive therapies alone will unlikely be sufficient to significantly improve pain and function in those individuals with PTTD.
Exercise rehabilitation plans should be devised based upon individual assessment, client treatment goals, and functional requirements. It is important for clinicians and their clients to understand that the conservative management of PTTD can take months and requires a high level of adherence to treatment interventions to achieve a successful outcome. However, should an individual adhere to their management plan, the chance of successful pain reduction and functional improvement is high.
Talysha Reeve, B.App.Sc.(Podiatry), GradCertClinRehab, is a podiatrist and former private clinic owner in Adelaide, South Australia. She has a special interest in the management of complex biomechanical and musculoskeletal conditions, with particular focus on their treatment via movement-based therapies and load management. Currently she divides her time between private clinical practice and delivering continuing professional development courses via Kinetic Therapies.
- Kohls-Gatzoulis J, Angel J, Singh D, Haddad F, Livingstone J, Berry G. Tibialis posterior dysfunction: a common and treatable cause of adult acquired flatfoot. BMJ. 2004;329(7478):1328-1333.
- Ling S, Lui T. Posterior tibial tendon dysfunction: an overview. Open Orthop J. 2017;11(1):714-723.
- Ross M, Smith M, Mellor R, Vicenzino B. (2018). Exercise for posterior tibial tendon dysfunction: a systematic review of randomised clinical trials and clinical guidelines. BMJ Open Sport Exer Med. 2018;4(1):e000430.
- Bodill C, Concannon M. Treatments for posterior tibial tendon dysfunction. Practice Nurs. 2012;23(8):389-394.
- Guelfi M, Pantalone A, Mirapeix RM, et al. Anatomy, pathophysiology and classification of posterior tibial tendon dysfunction. Eur Rev Med Pharmacol Sci. 2017;21(1);13-19.
- Pufe T, Petersen W, Mentlein R, Tillmann B. The role of vasculature and angiogenesis for the pathogenesis of degenerative tendons disease. Scand J Med Sc Sports. 2005;15(4):211-222.
- Semple R, Murley G, Woodburn J, Turner D. Tibialis posterior in health and disease: a review of structure and function with specific reference to electromyographic studies. J Foot Ankle Res. 2009;2(1):24.
- Snedeker J, Foolen J. Tendon injury and repair – a perspective on the basic mechanisms of tendon disease and future clinical therapy. Acta Biomater. 2017;63:18-36.
- Tempfer H, Traweger A. Tendon vasculature in health and disease. Front Physiol. 2015;6:30.
- Cook J, Purdam C. Is tendon pathology a continuum? A pathology model to explain the clinical presentation of load-induced tendinopathy. Br J Sports Med. 2008;43(6):409-416.
- Nielsen R, Buist I, Sorensen H, Lind M, Rasmussen S. Training errors and running related injuries: a systematic review. Int J Sports Phys Ther. 2012;7(1):58-75.
- Kirby K. Posterior Tibial Tendon Supination Moment Arm Decreases with Medial Deviation of Subtalar Joint Axis. Facebook. Available at https://www.facebook.com/kevinakirbydpm/ photos/a.554861454611102/ 1095208100576432/?tyty=1&theater. Published Nov. 29, 2016. Accessed Mar. 28, 2020.
- Maharaj J, Cresswell A, Lichtwark G. Subtalar joint pronation and energy absorption requirements during walking are related to tibialis posterior tendinous tissue strain. Sci Rep. 2017;7(1);17958.
- Maharaj J, Cresswell A, Lichtwark G. Foot structure is significantly associated to subtalar joint kinetics and mechanical energetics. Gait Posture, 2017;58:159-165.
- Maharaj J. The mechanical function of the subtalar joint and tibialis posterior muscle and tendon during walking. J Science Med Sport. 2017;20(Supp 3):6.
- Maharaj J, Cresswell A, Lichtwark G. The mechanical function of the tibialis posterior muscle and its tendon during locomotion. J Biomechan. 2016;49(14):3238-3243.
- Kirby K. Conservative treatment of posterior tibial dysfunction [Ebook]. Bryn Mawr, PA:Podiatry Management; 200:73-82.
- Gonçalves-Neto J, Witzel S, Teodoro W, Carvalho-Junior A, Fernandes T, Yoshinari H. Changes in collagen matrix composition in human posterior tibial tendon dysfunction. Joint Bone Spine. 2002;69(2):189-194.
- Satomi É, Teodoro W, Parra E, et al. Changes in histoanatomical distribution of types I, III and V collagen promote adaptative remodeling in posterior tibial tendon rupture. Clinics (Sao Paulo). 2008;63(1);9-14.
- Sandhu SV. Gupta S, Bansal H, Singla, K. Collagen in health and disease. J Orofacial Res. 2012;2(3):153-159.
- Cook, J., Rio, E., Purdam, C., & Docking, S. Revisiting the continuum model of tendon pathology: what is its merit in clinical practice and research? Br J Sports Med. 2016;50(19):1187-1191.
- Kirby, K. Basic Biomechanics Terminology and Concepts: Stress-Strain Curves, Part 2. Facebook. Available at https://www.facebook.com/kevinakirbydpm/ photos/a.554861454611102/1842037945893440/ ?type=3&theater. Published Oct. 25, 2018. Accessed Mar. 28, 2020.
- Pizzolato C, Lloyd D, Zheng M, et al. Finding the sweet spot via personalised Achilles tendon training: the future is within reach. Br J Sports Med. 2018;53(1);11-12.
- Kirby K. Basic Biomechanics Terminology and Concepts: Stress-Strain Curves, Part 1. Facebook. Available at https://www.facebook.com/kevinakirbydpm/posts/basic-biomechanics-terminology-and-concepts-stress-strain-curves-part-iin-my-las/1841470949283473/. Published Oct. 25, 2018. Accessed Mar. 28, 2020.
- Davenport T, Kulig, K, Matharu Y, Blanco C. The EdUReP model for nonsurgical management of tendinopathy. Phys Ther. 2005;85(10).
- Kulig K, Lederhaus E, Reischl S, Arya S, Bashford G. Effect of eccentric exercise program for early tibialis posterior tendinopathy. Foot Ankle Int. 2009;30(9):877-885.
- Bowring B, Chockalingam N. Conservative treatment of tibialis posterior tendon dysfunction—a review. Foot. 2010;20(1):18-26.
- Ritchie D. Keys to the biomechanical evaluation of the symptomatic adult-acquired flatfoot. Podiatry Today. 2012;25(4);48-60.
- Kjaer M, Langberg H, Miller B, et al. (2005). Metabolic activity and collagen turnover in human tendon in response to physical activity. J Musculoskelet Neuronal Interact. 2005;5(1);41-52.
- Espinosa N, Maurer M. Stage I and II posterior tibial tendon dysfunction. Cli Sports Med. 2015;34(4):761-768.
- Alvarez R, Marini A, Schmitt C, Saltzman C. Stage I and II posterior tibial tendon dysfunction treated by a structured nonoperative management protocol: an orthosis and exercise program. Foot Ankle Int. 2006;27(1):2-8.
- Houck J, Neville C, Tome J, Flemister A. Randomized controlled trial comparing orthosis augmented by either stretching or stretching and strengthening for stage II tibialis posterior tendon dysfunction. Foot Ankle Int. 2015;36(9):1006-1016.










Hi,
I treat a lot of individuals with posterior tibial tendonitis.They are not an easy group to contend with.My recommendations is to place these individuals in a high stability shoes with an orthotic that is medially posted and is elevated 3mm plus in the hind foot to decrease eccentric loading on the posterior tibial tendon.My exercise program is initially non weight bearing utilizing therabands emphasizing plantarflexion,inversion and toe flexion.I eventually move toward weight bearing exercises.Great results.
Understanding how each part of the foot works together makes a big difference when it comes to mobility and balance. Learning more about toe anatomy helps explain why even small issues in alignment or movement can affect overall comfort and create strain that travels up the foot and leg over time.