As obesity and type 2 diabetes continue to be growing public health burdens, clinicians will be faced with increasing numbers of patients who suffer from their complications, in particular, peripheral neuropathy. These authors review the multiple medications available to help.
By Shana Shetty, DPM PGY3, and Marshall G. Solomon, DPM FACPM, FACFAS

A 2015 report published in the Journal of Pain, found that 23.4 million adults (10.3%) in the United Stated experience a lot of pain. But more stunningly, it found that 126 million adults (55.7%) reported some type of pain in the 3 months prior to the survey.1
It will come as no surprise, then, that pain reduction is a major focus for those in the field of podiatric medicine and surgery, and as such, it is important to be well versed in the myriad of potential treatment options. Patients seek help for management of both acute and chronic pain. Most often, our patients are experiencing diabetic neuropathic pain or post-operative surgical pain. This review will focus on treatment options for these conditions.
One of the more common complaints is diabetic neuropathy. Podiatric physicians may treat the pain symptoms or refer to other specialties, such as the patient’s primary care physician, physical medicine and rehabilitation, or a neurologist.
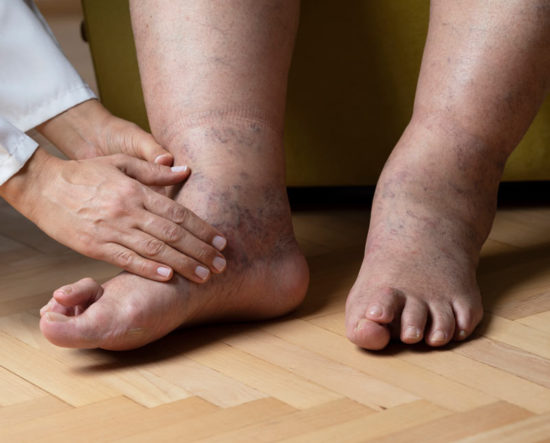
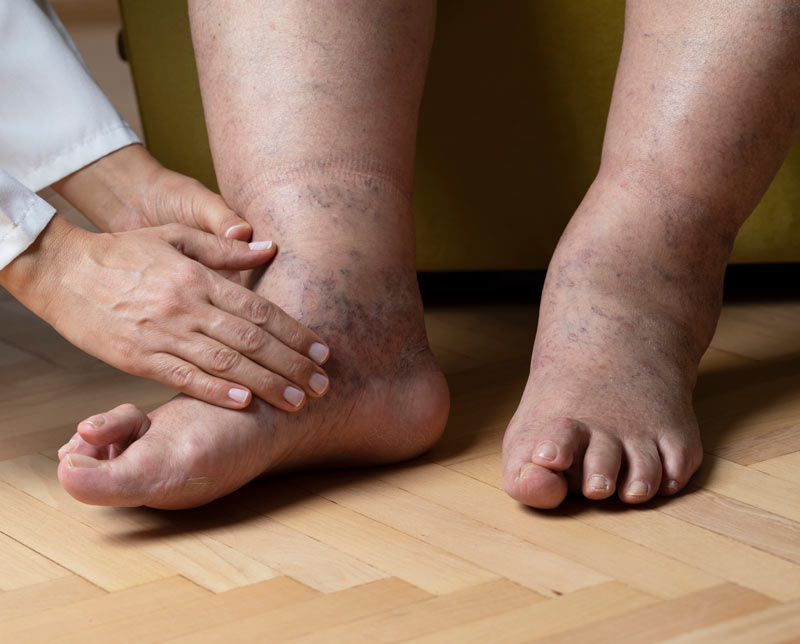
What is Peripheral Neuropathy?
Peripheral neuropathy (PN) is one of the more frequent pathologies seen in the lower extremities in the podiatric clinical practice. PN has a prevalence of 2.4% in the general population, but soars to 30% to 50% in patients with diabetes, in particular type 2 diabetes.2,3
PN is caused by damage to the peripheral nerves, those that reside outside of the brain and spinal cord. PN can cause weakness, numbness, and pain, usually in the hands and feet. Patients will often present with the concern of neuropathy affecting the feet. Patients will describe a “gloves and stocking” sensation.4
Over time, high blood sugar from poorly controlled diabetes can cause damage to the nerves. Symptoms range from mild numbness to pain that prevents activities of daily living.5,6 Type 1 diabetes and type 2 diabetes differ in symptomatology time frames: Type 1 patients become symptomatic after chronic hyperglycemia, typically after having had insulin-requiring diabetes for 20 years or more. Symptoms of NP occur much earlier in type 2 patients, with onset as early as 5 – 10 years after diagnosis.7 Testing should include peripheral neuropathic testing, vibratory sensation, light touch sensation, and monitoring pulses. Further testing includes glucose levels, Hemoglobin A1c, nerve conduction velocity testing, and Doppler exams.8
Treatment Options
Management for neuropathic pain often presents a challenge to practitioners. Traditional treatments for PN include topical and oral medications. Other options include transcutaneous electrical nerve stimulation (TENS), physical therapy, lasers, focused ultrasound, or referrals to neurology. Combining treatment modalities is also often necessary and can lead to better patient outcomes.
Topical Medications
Topical pain control options include capsaicin cream, lidocaine patches, and compound creams. Topical analgesics provide decreased side effects compared to oral medications.9
Capsaicin Cream: Capsaicin cream is derived from capsaicinoids, the spicy ingredient found chili peppers. When applied to the skin, it causes an initial sensitization followed by prolonged desensitization of nerves that are causing pain.8 There are low concentrations available over-the-counter (OTC), as well as newer higher concentrations, including the capsaicin 8% patch, which is approved by the US Food and Drug Administration (FDA).
A Cochrane systemic review and other studies have reported that a single application of the prescription capsaicin patch with an 8% concentration was shown to provide 3 months of pain relief.10,11 The single application helps avoid noncompliance, though the patch, which supplies about 100 times greater concentration than the OTC versions, must be applied by a healthcare provider under controlled conditions, typically under local anesthetic.
OTC capsaicin creams with concentrations of 0.025 or 0.075% have also shown effective with benefits in pain relief, sleeping, and ability to perform activities of daily living, but must be applied regularly.12,13
Topical Clonidine: Prescription topical clonidine is another option for managing PN. It is also used to treat hypertension as well as attention deficit syndrome. It has been shown to reduce excitability on microvasculature structures, improve blood flow, and reduce cytokine production.14 In a study comparing it to placebo, topical clonidine delivered a 30% reduction in pain intensity, but no better than 50%. This study concluded that it should not be used as a first-line treatment but may be used if other topicals have failed or are contra-indicated.15
Topical Lidocaine: Prescription-strength topical lidocaine has also been shown to reduce neuropathic pain. Lidocaine blocks voltage-gaited sodium channels and reduces the pain transduction. One study compared lidocaine 5% medicated plaster patch directly with an oral standard of care, pregabalin 2x a day. The study concluded that with diabetic PN, the efficacy was comparable between the two. However, the lidocaine plaster patch showed a better safety profile as well as greater patient satisfaction.16
Compound Creams: Prescription compound creams are a combination of 2 or more forms of a topical agent. Compounding creams are an age-old pharmaceutical practice. The purpose of compounding is to provide patients with relief without the side effects of systemic oral medications. Topicals often have less risk of abuse as well.17 Topical compounded medications for managing PN pain provide an anti-inflammatory medication, a tricyclic antidepressant and/or an anticonvulsant. Although they seem to be effective, more studies are needed.18
Cannabidiol Cream/Ointments: As multiple states have moved to legalize medical marijuana, studies with cannabidiol (CBD) oil and creams are ramping up. A recent study published in Current Pharmaceutical Biotechnology examined the effectiveness of topical CBD oil for relief of PN symptoms in the lower extremities. The study used a product containing 250 mg CBD/3 fl oz, and found a reduction in intense pain, sharp pain, and cold and itchy sensations.19 CBD products have been shown to be cost effective and thought to have decreased side effects compared to pharmaceutical treatments. Several clinical trials are already underway in the United States: according to ClinicalTrials.Gov, 13 trials are recruiting and 2 more are preparing to recruit.
Pharmaceutical Medications: Over-the-Counter Medications
OTC oral medications include acetaminophen and several other well-known non-steroidal anti-inflammatory drugs (NSAIDS). NSAIDS reduce pain through decreasing the body’s production of prostaglandin, an enzyme that sends pain messages to the brain. These are often used as a first-line option in patients with painful neuropathy. Acetaminophen is used for mild to moderate pain relief and to reduce inflammation. Common NSAIDS include aspirin, ibuprofen, and naproxen sodium.
Pharmaceutical Medications: Prescription Strength Medications
When OTC medications fail, prescription-strength medications may be used. FDA-approved treatments include duloxetine and pregabalin. Other prescribed medications include tricyclic medications, gabapentin, and tramadol.
Duloxetine: This antidepressant is FDA-approved for diabetic neuropathy. Research shows that it is effective in short-term studies (up to 8 weeks). It has been shown that 60 mg a day is both safe and effective. However, it should be avoided in patients with hepatic and renal impairment.20 Several authors acknowledge that long-term evaluation is still needed.21
Gabapentin and Pregabalin: Gabapentin and pregabalin are antiseizure medications. Gabapentin may be taken with tricyclic antidepressants or duloxetine. In a head-to-head randomized controlled study that compared gabapentin and duloxetine, both were shown to be equally effective. While duloxetine had fewer side effects, gabapentin users reported pain relief was faster.22
Tricyclic Antidepressants: This class includes amitriptyline, nortriptyline, and desipramine. These have been shown to be superior to placebo. However, further studies are needed to compare efficacy. Amitriptyline and desipramine are commonly used.23
Other: Metanx® (Pamlab LLC, Covington, LA), a prescription medical food product/supplement, is specially formulated to meet the distinctive nutritional requirements for diabetic peripheral neuropathy and can only be used under the supervision of a physician for the clinical dietary management of this condition.24 In a 24-week randomized trial of 214 patients with type 2 diabetes and neuropathy, the product was shown to alleviate peripheral neuropathic pain.25 Metanx is a capsule made up of L-methyl folate calcium and other B vitamins that allows the body to address the symptoms of diabetic nerve damage by improving blood flow to help with nerve repair. Although shown to be effective in short-term treatment, long-term studies are still necessary.
Other Treatment Modalities
Many of today’s patients are open to alternative pain-relief options. These can include focused ultrasound, TENS, lasers, and physical therapy.
Focused ultrasound therapy is an emerging therapeutic modality for a host of neurologic diseases. This non-invasive therapy is FDA-approved for unilateral treatment of essential tremor and clinical studies are underway in Parkinson’s and chronic pain. Studies have shown that it temporarily blocks conduction of in vitro sural nerves and thereby modulates diabetic blood vessels, improves pain symptoms, and decreases neuropathic progression.26
TENS is used for pain control for both acute and chronic pain caused by myriad conditions. A TENS unit is a small device that delivers electrical pulses to stimulate nerve fibers at the point where pain is perceived and works by dampening the pain signals to the brain. A randomized controlled trial involving 31 participants showed that 15 of 18 (83%) patients receiving TENS had significantly improved pain scores (reduction from 3.17 to 1.44 on a 5-point scale; P < 0.01) versus 5 of 13 (38%) patients receiving sham treatments (reduction from 2.98 to 2.38). Although research is still not definitive, it has been shown to provide some relief in neuropathic pain.27
Laser therapy provides a non-invasive treatment. In this treatment, a low-level laser is used to irradiate the plantar and dorsal aspect of the foot. In one study of 19 patients with DPN, laser therapy demonstrated a significant decrease in the Visual Analogue Scale (VAS) pain scale—6.47 ± 0.84 to 1.21 ± 0.78 (P <0.001).28 The authors hypothesized that the decrease in pain was due to an increase in microcirculation in the periphery or the release of cytokines which cause vasodilation and new capillaries.
Physical therapy modalities have also been shown to be effective, as strength training can improve muscle function leading to decreased pain. Regular exercise can help to better control blood sugar and delay progression of neuropathic pain as well. However, some diabetic patients may have limitations in performing physical exercise, which is why multiple alternative treatments are necessary.29,30
Conclusion
Peripheral neuropathy is an all-too-common long-term complication of diabetes. Improving blood glucose control is a first line of defense, but long-standing diabetes is notoriously difficult to control. While long-term studies are still needed to determine which treatments are most efficacious, today’s patients have a multitude of treatment options for pain reduction. Clinicians are advised to understand each patient’s pain experience and offer appropriately customized therapy options.
Shana Shetty, DPM, is a third-year resident at the Beaumont Health Farmington Hills PMRS/RRA residency program in Farmington Hills, Michigan, specializing in foot and ankle surgery.
Marshall G. Solomon, DPM, FACPM, FACFAS, FFPM RCPS (Glasg) is a foot and ankle surgeon at the Foot Care Institute of Michigan and the Beaumont Hospital Podiatry Clinic and is the podiatry residency program director at the Beaumont Hospital, Farmington Hills, all in Farmington Hills, Michigan.
LER is proud to partner with the American College of Podiatric Medicine to present clinically relevant peer-reviewed content, curated by Jarrod Shapiro, DPM, FACFAS, FACPM, FFPM RCPS (Glasg).
- Nahin RL. Estimates of pain prevalence and severity in adults: United States, 2012. J Pain. 2015;16(8):769-780.
- Watson J Dyck P. 2020. Peripheral neuropathy: a practical approach to diagnosis and symptom management. Mayo Clin Proc. 2015;90(7):940-951.
- Tesfaye S. Neuropathy in diabetes. Medicine. 2010;38(12):649-655.
- Azhary H, Farooq MU, Bhanushali M, Majid A, Kassab MY. Peripheral neuropathy: differential diagnosis and management. Am Fam Physician. 2010;81(7):887-892.
- Pop-Busui R, Boulton AJ, Feldman EL, et al. Diabetic neuropathy: a position statement by the American Diabetes Association. Diabetes Care. 2017;40(1):136–154.
- Izenberg A, Perkins BA, Bril V. Diabetic neuropathies. Semin Neurol. 2015;35(4):424–430.
- White NH. Type 2 diabetes in youth: a 21st century disorder. Lower Extremity Review. 2019;10(2):32-41.
- Quan, D. Diabetic neuropathy. Medscape. Available at https://emedicine.medscape.com/article/1170337-overview. Published July 28, 2020. Accessed Oct. 2, 2020.
- Peppin JF, Pappagallo M. Capsaicinoids in the treatment of neuropathic pain: a review. Ther Adv Neurol Disord. 2013;7(1):22-32.
- Derry S, Sven-Rice, A, Cole P, Tan T, Moore RA. Topical capsaicin (high concentration) for chronic neuropathic pain in adults. Cochrane Database Syst Rev. 2013;(2):CD007393. Update in: Cochrane Database Syst Rev. 2017;1:CD007393.
- Rosenberg CJ, Watson JC. Treatment of painful diabetic peripheral neuropathy. Prosthet Orthot Int. 2015;39(1):17-28.
- Treatment of painful diabetic neuropathy with topical capsaicin. A multicenter, double-blind, vehicle-controlled study. The Capsaicin Study Group. Arch Intern Med. 1991;151(11):2225-2229.
- Effect of treatment with capsaicin on daily activities of patients with painful diabetic neuropathy. Capsaicin Study Group. Diabetes Care. 1992;15(2):159-165.
- Sawynok J. Topical analgesics for neuropathic pain: preclinical exploration, clinical validation, future development. Eur J Pain. 2014;18(4):465-481.
- Wrzosek A, Woron J, Dobrogowski J, Jakowicka-Wordliczek J, Wordliczek J. Topical clonidine for neuropathic pain. Cochrane Database Syst Rev. 2015;8(9):CD010967.
- Baron R, Mayoral V, Leijon, et al. 5% lidocaine medicated plaster versus pregabalin in post-herpetic neuralgia and diabetic polyneuropathy: an open-label, non-inferiority two-stage RCT study. Curr Med Res Opin. 2009;25(7):1663-1676.
- National Academies of Sciences, Engineering, and Medicine; Health and Medicine Division; Board on Health Sciences Policy; Committee on the Assessment of the Available Scientific Data Regarding the Safety and Effectiveness of Ingredients Used in Compounded Topical Pain Creams; Jackson LM, Schwinn DA, editors. Compounded Topical Pain Creams: Review of Select Ingredients for Safety, Effectiveness, and Use. Washington (DC): National Academies Press (US); 2020 May 13.
- Ormseth MJ, Scholz BA, Boomershine CS. Duloxetine in the management of diabetic peripheral neuropathic pain. Patient Prefer Adherence. 2011;5:343-356.
- Xu DH, Cullen BD, Tang M, Fang Y. The effectiveness of topical cannabidiol oil in symptomatic relief of peripheral neuropathy of the lower extremities. Curr Pharma Biotechnol. 2020;21(5):390–402.
- Feldman E. Diabetic neuropathy (Beyond the basics). UpToDate. www.uptodate.com. Published September 2020. Available at www.uptodate.com/contents/diabetic-neuropathy-beyond-the-basics. Accessed Oct. 2, 2020.
- Majdinasab N, Kaveyani H, Azizi M. A comparative double-blind randomized study on the effectiveness of duloxetine and gabapentin on painful diabetic peripheral polyneuropathy. Drug Des Devel Ther. 2019;13:1985-1992.
- Lesser, U. Sharma, L. LaMoreaux, R. M. Poole. Pregabalin relieves symptoms of painful diabetic neuropathy a randomized controlled trial. Neurology. 2004:63(11):2104-2110.
- Joss JD. Tricyclic antidepressant use in diabetic neuropathy. Ann Pharmacother. 1999;33(9):996-1000.
- Metanx [package insert]. Covington, LA: Alfasignma USA, Inc. 2017.
- Fonseca VA, Lavery LA, Thethi TK, et al. Metanx in type 2 diabetes with peripheral neuropathy: a randomized trial. Am J Med. 2013;126(2):141-149.
- Tan JS, Lin CC, Chen GS. (2020). Vasomodulation of peripheral blood flow by focused ultrasound potentiates improvement of diabetic neuropathy. BMJ Open Diabetes Res Care. 2020;8(1):e001004.
- Snyder MJ, Gibbs LM, Lindsay TJ. Treating painful diabetic neuropathy: an update. Am Fam Physician. 2016;95(33):2227-2234.
- Cg SK, Maiya AG, Hande H, et al. Efficacy of low level laser therapy on painful diabetic peripheral neuropathy. Laser Ther. 2015;24(3), 195–200.
- American Physical Therapy Association. Guide to Physical Therapist Practice. 2nd Ed. American Physical Therapy Association. Phys Ther. 2001;81(1):9-746.
- Kluding PM, Bareiss SK, Hastings M, et al. Physical Training and activity in people with diabetic peripheral neuropathy: paradigm shift. Phys Ther. 2017;97(1):31-43.








I have diabetes, and diabetic nerve pain need to know something that I can do from home.
Readers are encouraged to consult a medical professional or healthcare provider if they seek medical advice, diagnoses, or treatment.
Please send the Pain Reduction Methods for Peripheral Neuropathy diseases medicine in aauyrvedic