 Preliminary research suggests the use of a kinetic return ankle foot orthosis is associated with small but significant short-term increases in calf circumference, which in turn suggests this type of device might reduce or protect against the risk of disuse muscle atrophy.
Preliminary research suggests the use of a kinetic return ankle foot orthosis is associated with small but significant short-term increases in calf circumference, which in turn suggests this type of device might reduce or protect against the risk of disuse muscle atrophy.
By Robert H. Meier, CO, BOCO; David C. Ruthsatz, CO, CPA; and Daniel Cipriani, PT, PhD
Atrophy of the calf muscle group in patients with neuromuscular involvement has been seen clinically. Evidence clearly demonstrates the contribution of the neuromuscular condition for calf muscle atrophy, yet only a single case study demonstrated the contribution of a molded ankle foot orthosis (MAFO) to calf circumference. It is not known if a more dynamic AFO would have any influence on calf circumference. The objective of this study was to determine the influence of a dynamic AFO on calf circumference and, potentially, the risk of calf muscle atrophy.
Calf group atrophy in patients with neuromuscular involvement is a common clinical observation and may be the result of a combination of factors, including the neuromuscular condition as well as the use of a MAFO to manage foot drop. A literature search (via PubMed), which we conducted using numerous key words and phrases (eg, AFO calf atrophy, CVA calf atrophy, neuro-deficit calf atrophy), yielded results indicating calf muscle group atrophy can occur secondary to cerebrovascular accident1 but only one case study2 specifically linked calf atrophy to MAFO usage, in this case in a patient with a diagnosis of clubfoot. Several studies identified significant reduction in muscle activity of the tibialis anterior while wearing an AFO, which, with prolonged usage, could lead to muscle atrophy.3-5
The search also revealed numerous studies6-8 suggesting that immobilization may be a causative factor leading to disuse atrophy of muscle mass and strength. While custom-molded AFOs do not induce 100% immobilization because they are fit on soft tissue, these rigid structures provide functional immobilization. Even articulating ankle MAFOs immobilize foot complex inversion and eversion, abduction and adduction, and plantar flexion, while allowing only dorsiflexion. It is likely that MAFOs may contribute to the development of disuse atrophy in neuromuscular deficit patients.
Review of the calf group function
Before studying atrophy of the calf group in neuro-involved patients, a review of the normal closed chain function of the gastrocsoleus complex was completed.9 Both the gastrocnemius and soleus muscles are activated at initial contact during gait secondary to synergistic firing of the anterior tibialis muscle, and this results in deceleration of the forefoot to the ground. At the same time, calcaneal eversion triggers a stretch reflex to both the gastroc and soleus muscles. The gastrocsoleus complex, along with the posterior tibialis muscle, eccentrically decelerates frontal plane calcaneal eversion, which is a component of pronation. This helps to control frontal plane ankle eversion and transverse plane internal rotation of the tibia.
Transitioning into the second rocker of gait, the muscle group continues to work eccentrically in midstance. The soleus decelerates the progression of the tibia over the fixed foot (ankle dorsiflexion motion), allowing proximal inertial forces to create knee extension. The gastrocnemius, which originates above the knee, works to modulate the rate of knee extension being created by the soleus and by inertia. In late midstance the gastroc and soleus muscles work to facilitate inversion of the calcaneus, supinating the foot so it can be a more efficient lever arm for propulsion.
In the third rocker, or the propulsive phase, of gait, the gastrocsoleus complex works concentrically to lift the heel off the ground, taking advantage of proximal inertial forces, and then to concentrically plantar flex the ankle (creating 39% to 47% of propulsion10), propelling the foot off the ground and advancing the limb though space. In the process, the muscle complex helps maintain a more rigid supinated foot to create a more efficient propulsive lever arm, and facilitates external tibial rotation and ankle inversion. The complex turns off as the toes leave the ground and stays off until the next initial contact made by that limb.
This review reinforced the concept that the calf group functions in all three planes during the stance phase of gait, which led to the hypothesis that simply immobilizing the calcaneus in a subtalar neutral position would diminish the functional capacity of the calf muscle group and increase the risk of disuse atrophy.
Study design
The study was designed to measure calf circumference in patients who had worn MAFOs and were being transitioned into a more dynamic AFO design, a kinetic return AFO (KRAFO). Patient selection included all consecutive patients presenting for new AFOs at a single O&P facility. A single orthotist measured calf circumference in all patients to minimize intrarater variability, measuring at maximum calf circumference and 2.54 cm above and 2.54 cm below that mark.
A subjective patient survey was administered to determine the patient’s level of satisfaction and level of function while wearing their MAFOs. The survey (Figure 1) asked for patient estimates of total device wear time, device wear time leading to fatigue, and distance capacity; it also asked patients to use a 1-to-10 rating scale for seven different criteria related to patient satisfaction and perceptions of their ability to function in the devices. Gait speed was also measured in seconds with a stopwatch while patients walked 10-meter timed tests both in their existing device and after fitting of the KRAFOs. All of the data were locked after acquisition to avoid influencing the follow-up tests.
During the test period, patients were instructed to wear the KRAFO during waking hours or to tolerance. After eight weeks, the patient’s calf circumference and walking speed were reassessed by the same rater following the same protocols to detect any differences in circumference measurements occurring secondary to the switch to a KRAFO. At the same time, the subjective patient survey was administered again to determine the patient’s level of satisfaction and level of function while in the KRAFO. This second set of data was compared with the first set and analyzed using a paired samples T-test.
Objective study results

Figure 2. Solid ankle molded ankle foot orthosis.
All study participants presented to a single orthotist in a privately owned O&P clinical setting over a 14-month period with prescriptions from various physicians for replacement AFOs. Although 38 patients were initially enrolled in the study, only 19 patients were available for the eight-week (plus or minus two days) follow-up assessment. Patients had worn MAFOs an average of 17.44 months (range, 1-24 months) prior to the start of the study, and presented with foot drop resulting from 12 different neuromuscular diagnoses. The right side was involved in seven patients, the left side was involved in nine patients, and three patients were affected bilaterally. MAFO design included solid ankle (n = 6) (Figure 2), posterior leaf spring (n = 10), and articulating ankle/plantar flexion stop (n = 3) AFOs. These patients were switched to one of three KRAFOs (Figure 3) that provided different levels of support; patient body type and proximal deficits determined the level of support needed. All KRAFOs were customized, including, at a minimum, the addition of a firm, prefabricated foot orthotic shell on top of the AFO footplate.
Calf circumference. In the 19 patients, mean calf circumference was 324.35 mm (minimum = 266.7 mm, maximum = 419.1 mm) at the start of the study and 328.95 mm (minimum = 279.4 mm, maximum = 425.45 mm) after eight weeks in KRAFOs. The difference between measurements was statistically significant.
Walking speed. Patients tended to walk more slowly while wearing the MAFOs, completing the 10-m walking distance in 14.99 seconds (range, 10.8-18.8), compared with 14.58 seconds (range, 12.5-17.8) while wearing the KRAFOs (p < .001).
Subjective study results
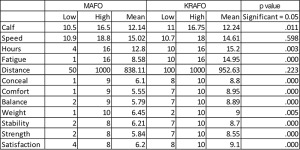
Subjective study results are reported in Table 1.
Device use. The self-reported mean number of hours per day (h/d) that patients wore the AFOs was 13.26 h/d for the MAFOs (range, 8-16 h/d, with eight patients at 16 h/d) compared with 15.16 h/d (range, 10-16 h/d, with 16 patients at 16 h/d) for the KRAFOs. This difference was statistically significant (p < .001). (A patient response of “waking hours” was calculated as 16 h/d.)
Functional improvement. The self-reported mean time to fatigue was nine hours in the MAFOs (range, 4-16 h, with one patient at 16 h) compared with 15.11 h (range, 10-16 h, with 16 patients at 16 h) in the KRAFO, a statistically significant difference (p < .001). Mean distance capacity reported for the MAFOs was 882.35 yards (range, 500 to 1000 yards, with 15 patients at 1000 yards) compared with 1000 yards (all 19 at 1000 yards) in the KRAFOs, a statistically significant difference (p = .041).
Ease of use. Patients gave the KRAFOs significantly higher ratings than the MAFOs for ability to conceal the device, comfort, and satisfaction with the device’s weight (p < .001). Mean rating for ability to conceal the device was 6.32 (range, 1-9) for the MAFOs and 8.79 (range, 8-10) for the KRAFOs. Mean rating for comfort was 5.89 for the MAFOs (range, 1-9) and 9 for the KRAFOs (range, 7-10). Mean satisfaction with the weight of the device was rated at 6.37 (range, 1-10) for the MAFOs and 9 (range, 2-10) for the KRAFOs.
Patient perceptions. Patients gave the KRAFOs significantly higher ratings than the MAFOs for perceived balance, perceived stability during gait, and perceived strength (p < .001). Perceived balance was given a mean rating of 5.89 (range, 2-9) for the MAFOs and 8.94 (range, 7-10) for the KRAFOs. The mean rating for perceived stability during gait was 6.39 (range, 5-9) for the MAFOs and 8.74 (range, 7-10) for the KRAFOs. Perception of strength was given a mean rating of 6 (range, 2-8) for the MAFOs and 8.58 (range, 7-10) for the KRAFOs.
Finally, the mean rating for overall satisfaction with the device was 6.32 (range, 5-8) for the MAFOs compared with 9.16 (range, 7-10) for the KRAFOs. This difference was statistically significant (p < .001).
Discussion

Figure 3. Kinetic return ankle foot orthosis.
This study attempted to determine if KRAFOs could influence calf circumference in patients who had habitually worn MAFOs. In addition, it examined walking speed and subjective perceptions of the patients when wearing KRAFOs and MAFOs.
The data suggest that use of a KRAFO may engage the calf muscles during physical activity. The slight but statistically significant increase in mean calf size observed over the eight-week period is very encouraging, especially considering that muscle hypertrophy does not begin until at least three to four weeks of muscle overload or resistance.11 Any additional calf muscle activity associated with KRAFO use is likely related to two primary design differences between MAFOs and KRAFOs: KRAFOs allow normal biomechanical function in the talocalcaneal and talotarsal joints, while the rearfoot is relatively immobilized in MAFOs, and KRAFOs are designed to return energy during the third rocker to assist with propulsion, while MAFOs are not.
Patients also walked slightly but significantly faster when wearing the KRAFOs than while wearing the MAFOs, even though they were less familiar with the KRAFOs, a finding that suggests improved function. This is consistent with the subjective ratings of perceived stability during gait, which were significantly higher for the KRAFOs than the MAFOs. In addition, there was less variability between patients with regard to gait speed for the KRAFOs than the MAFOs, suggesting a more consistent gait with the KRAFOs.
Other subjective ratings were also significantly higher for the KRAFOs than the MAFOs. This suggests the KRAFOs’ light weight and low profile are associated with an improved sense of balance, strength, and gait stability. Higher levels of overall satisfaction for the KRAFOs than the MAFOs also are consistent with the improved gait speeds and improved sense of comfort and mobility.
Study limitations
The study does not identify causative factors leading to calf hypertrophy. The authors assume it is a result of the functional design of the KRAFO, but it could also be secondary to the patient’s perception of comfort, leading to longer wearing times and greater walking distances in the KRAFO. And it may be all of these factors.
The study did not document patient weight during either test session. It is possible that patient weight loss due to an increase in activity in the KRAFO might have had a negative effect on calf circumference, potentially offsetting increases related to muscle development. No clinically relevant changes in edema status were noted between the two testing sessions. An increase in walking would tend to decrease edema, so if that occurred, that also would have had a negative impact on gains shown in calf circumference.
The subjective assessment of distance capacity may not have offered enough choices to reflect patients’ actual activity levels. Fourteen of the 19 patients rated their capacity at 1000 yards or more in the MAFOs, while all 19 rated their distance capacity at 1000 yards or more in the KRAFOs. Future study designs should include options such as longer measures of distance capacity.
The study was designed with a very narrow window for follow-up, at eight weeks plus or minus two days, and data were not acquired if the follow-up was outside the four-day window. A slightly wider window of plus or minus five days would have increased participation rates at follow-up.
Conclusions
Some design features commonly used in MAFOs to create stability lead to areas of immobilization that may increase a patient’s risk of disuse atrophy in the calf muscles. This study found that use of a kinetic return AFO is associated with small but significant short-term increases in calf circumference, which suggests this type of device might reduce or protect against the risk of disuse atrophy. Subjective ratings of patient perceptions also suggest this device may make the patient more functionally stable.
Robert H Meier, CO, BOCO, is president of Kassel Group, an orthotic education company based in Adrian, MI. David C. Ruthsatz, CO, CPA, is practice manager at Advanced Prosthetics in Columbia, SC. Daniel Cipriani, PT, PhD, is an associate professor of physical therapy at Chapman University in Orange, CA.
Disclosures: Institutional Review Board approval was not required for this study. Principles of the Declaration of Helsinki were followed. No funding was provided for this study. Devices used in this study are US Food and Drug Administration class 1 devices.
- Dattola R, Girlanda P, Vita G, et al. Muscle rearrangement in patients with hemiparesis after stroke: an electrophysiological and morphological study. Eur Neurol 1993;33(2):109-114.
- Chan KT, Hurley RA, Dural A, Hayman LA. Improving the clinical assessment of leg muscle in adult clubfoot using magnetic resonance imaging: a case report. J Clin Neuromuscul Dis 2002;4(1):23-26.
- Crabtree CA, Higginson JS. Modeling neuromuscular effects of ankle foot orthoses (AFOs) in computer simulations of gait. Gait Posture 2009;29(1):65-70.
- Hesse S, Konrad M, Uhlenbrock D. Treadmill walking with partial body weight support versus floor walking in hemiparetic subjects. Arch Phys Med Rehabil 1999;80(4):421-427.
- Geboers JF, Drost MR, Spaans F, et al. Immediate and Long-term effects of ankle-foot orthosis on muscle activity during walking: a randomized study of patients with unilateral foot drop. Arch Phys Med Rehabil 2002;83(2):240-245.
- Urso ML. Regulation of muscle atrophy: wasting away from the outside in: an introduction. Med Sci Sports Exerc 2009;41(10):1856-1859.
- Khalid M, Brannigan A, Burke T. Calf muscle wasting after tibial shaft fracture. Br J Sports Med 2006;40(6): 552-553.
- Jackman RW, Kandarian SC. The molecular basis of skeletal muscle atrophy. Am J Physiol Cell Physiol 2004;287(4):C834-C843.
- Neumann DA. Kinesiology of the Musculoskeletal System. St. Louis, MO; Mosby; 2002.
- Farris DJ, Sawicki GS. The mechanics and energetics of human walking and running: a joint level perspective. J R Soc Interface 2012;9(66):110-118.
- Blazevich AJ,Gill ND,Bronks R, Newton RU. Training-specific muscle architecture adaptation after 5-wk training in athletes. Med Sci Sports Exerc 2003;35(12):2013-2022.










I am in my 40s recovering from a Traumatic by Injury for years ago. The AFO eyewear seems to be affecting my calf circumference and decreasing it. What should I do? Contact the person at the clinic I survive my AFO or just suck it up? Thank you