iStockPhoto.com # 1036911950
Encouraging exercise and appropriate footwear selection may be key in helping patients maintain healthy activity levels.
By Audris Tien, DPM, Brad Franklin, DNP, RN, FNP-C, FAANP, and Jarrod Shapiro, DPM, FACFAOM, FACFAS

LER is pleased to partner with the American College of Foot & Ankle Orthopedics & Medicine in providing peer-reviewed content for a multidisciplinary audience.
Exercise is recommended for the majority of patients regardless of age, gender, or physical disability. The 2008 Physical Activity Guidelines for Americans1 recommended that all adults perform 150 minutes per week of moderate aerobic physical activity or 75 minutes of intense physical activity per week to achieve a cardiovascular benefit. The World Health Organization corroborates this recommendation for the worldwide adult population.2 Healthcare organizations across the globe support adult exercise recommendations to mitigate the risk of weight-related disease and disability, which is epidemic in the industrialized world. Healthcare providers should be advising patients to exercise.
To ensure patients can exercise safely, practitioners should provide a thorough foot evaluation and evidence-based recommendations on footwear selection. The purpose of this article is to help healthcare providers recognize the components of a proper foot exam, understand the different types of shoes and shoe anatomy, and provide direction to patients in the selection of footwear products.
Literature Review
The rationale for such a broad worldwide consensus on the recommendation for exercise is the need to reduce the incidence of obesity and the diseases that follow. Currently, 34.9% of all US adults are classified as obese (BMI > 30), with another 35 % classified as overweight (BMI 25 – 29).3 Type II diabetes mellitus (T2DM), the disease most often associated with excess weight, is occurring in epidemic proportions with 9% of US adults affected.4 Worse, more than 1 in 3 US adults have prediabetes, a condition caused by excess body weight and lack of exercise. Worse still, the incidence of T2DM among those under 18 is increasing. Once T2DM develops, negative impacts on health include macrovascular (ie, cardiovascular disease) and microvascular (ie, retinopathy, neuropathy) complications. Many consequences of obesity are reduced or preventable with a combination of weight loss and exercise. Despite the benefits of exercise being well known, only 21% of adults report reaching the minimum amount recommended by the 2008 Physical Activity Guidelines—that’s only 1 in 5.5
While the barriers to adequate exercise are multifactorial, convenience, accessibility, and cost play a major factor for many adults.6 Helping patients understand that exercise comes in many forms and tailoring the language to each patient is essential for making exercise recommendations. Generally, exercise recommendations that are simple and easy to complete will improve patient compliance. Walking is a simple exercise that allows nearly all patients to meet the recommended targets. It is an easy way to be physically active and is a normal part of everyday life for most adults. Walking is inexpensive, practical, and generally a convenient form of exercise that can be done in nearly any setting. And importantly, walking is the only aerobic exercise that is considered safe for previously sedentary patients, making it ideal for those patients with comorbidities.7
The benefits of walking have been frequently studied and may surprise many patients and providers alike. Overall, walking improves cardiorespiratory fitness if performed at least 150 minutes per week, typically 30 minutes 5 times a week.8,9 Walking has also been shown to improve lower extremity muscle strength and decrease body weight and body fat in middle-aged obese women.8 Plus, it is associated with a decrease in the decline of bone loss in young and old women, even those with osteopenia.10,11 In men, walking has been associated with a decrease in all-cause mortality, even in those with comorbidities.12 For patients with T2DM, walking up to 150 minutes per week improves fasting blood glucose, hemoglobin A1c (HbA1c), and triglycerides.13 Even standing or walking for as little as 5 minutes after prolonged sitting can reduce post-prandial glucose levels and insulin secretion, which can help with prediabetes.14
Younger patients appear to have additional reductions in total cholesterol and low-density lipoprotein cholesterol (LDL-C) values compared to elderly patients.8,13 Sedentary adults can also show reductions in diastolic blood pressure even if they do not have a history of hypertension. Even patients with chronic musculoskeletal pain show improvement in both pain and activities of daily living with a regular walking routine.7
Although making the recommendation to exercise is straightforward, the actual implementation by the patient can be challenging. Typically, the responsibility for selecting appropriate footwear falls on the patient—often without the benefit of receiving a recommendation from a provider. Most often, patients select athletic footwear based on consumer concerns versus foot form and function. Poor-fitting footwear may lead to injuries that can prevent patients from obtaining the recommended amount of exercise. Healthcare providers, by conducting a foot examination, are in a valuable position to help patients select the appropriate footwear.
Lower extremity injuries due to poor-fitting footwear have been well documented. In a recent study of older adults, Menz et al.15 reported that up to 50% wore shoes that were too narrow or too short, which resulted in corns, toe deformity (hallux valgus), or foot pain. In the Veteran population, patients with diabetic foot wounds were more likely than not to have poor-fitting footwear.16 Even among active US military personnel, one study showed that up to 56% wear shoes that are sized inappropriately.17 That same study reported that up to 70% of runners develop an overuse injury17, making the shoe selection critical, and the foot evaluation even more important. Healthcare providers can help prevent lower extremity injuries by performing a foot evaluation that helps the patient select appropriate footwear for their exercise program.
Foot Examination Components

Figure 1. Footprints indicating three general types of feet. From left to right: the cavus foot type shows minimal arch contact with the ground; rectus foot type shows somewhat more midfoot contact with the ground; and the planus or pronated foot shows a significant amount of arch contact with the ground.
A complete and thorough foot exam has 3 components: the patient history, the physical exam, and patient education.
The history-taking portion of a patient encounter is often the most time-consuming yet most telling portion of the exam. When the chief complaint is related to the patient’s foot, questions regarding onset, duration, provoking and relieving factors, and prior treatment need to be explicitly asked. Information on changes in shoe gear or increased physical activity should also be ascertained. When enough information has been gathered to garner a list of differential diagnoses, the provider may move onto the physical exam to home in on the most likely diagnosis.
Much like a full physical, the components of a complete foot exam can be broken down into various health systems: vascular, dermatology, musculoskeletal, neurological. No matter which systems component is examined first, a systematic order should be followed. Table 1 outlines the essential components of a complete foot exam.
The vascular exam includes palpating for the dorsalis pedis and posterior tibial pulses. The dorsalis pedis pulse can be palpated lateral to the extensor hallucis longus tendon on the dorsal surface of the foot. The posterior tibial pulse can be easily palpated posterior to the medial malleolus. It is also important to check capillary refill of the digits, with normal capillary refill being <3 seconds. The presence or absence of pedal hair growth is also indicative of circulatory status to the lower extremities. Temperature differences between the left and right foot or between ipsilateral calf and foot should be noted too.
The dermatology exam can be done concomitantly with the vascular exam, paying close attention for signs of venous disease which may manifest as varicosities, hemosiderin deposits, or brawny, atrophic skin. Additionally, the location and number of calluses should be documented as calluses are signs of high-pressure areas that may predispose to ulcerative lesions. Increased warmth and edema may also indicate signs of an acute inflammatory response following a musculoskeletal injury. Interdigital spaces should also be checked for any debris or maceration because deeper lesions often go unnoticed due to the folds of the skin. Nails should be inspected for signs of fungal disease, in-growing or elongated toenails.
The musculoskeletal exam should include basic muscle strength testing against resistance in all four quadrants—dorsiflexion, plantarflexion, eversion, and inversion—as well as passive and active range of motion of the ankle joint and subtalar joint. Pain and crepitus with range of motion of joints may indicate symptoms of osteoarthritis. Musculoskeletal deformities, such as hammer toes or bunions, can increase patients’ risk for ulceration and should be charted and monitored.18 Determining foot type is recommended with the patient standing, as natural muscle tone will create the appearance of an inverted foot with high arch in most feet except those with rigid flatfoot, such as patients with osteoarthritis.
Discussion of a complete biomechanical exam is beyond the scope of this review. However, general components of this exam are pertinent to assisting with shoe choices. The general foot type, including pes planus, pes cavus, or rectus appearance (Figure 1), is important when choosing a shoe. More rigid foot types, for example, generally better tolerate cushion shoes, as described below. Next, hammertoes may require a shoe with a deeper or wider toe box to accommodate these deformities. Most significantly, hammertoes with primarily sagittal plane contractures are poorly tolerated by common shoes and may need increased depth or softer materials for the shoe upper. Additionally, the position of the heel in the frontal plane is important for shoe tolerance. An inverted (varus) heel may cause increased friction on the posterosuperior aspect of the calcaneus, potentially causing abrasions.
The neurological exam consists of testing the Achilles tendon reflex and light touch sensation, as well as protective sensation using the 5.07 Semmes-Weinstein monofilament (SWMF) in those at risk for peripheral neuropathy, such as patients with diabetes. There are 10 points to examine using the SWMF with the patient’s eyes closed, as depicted in Figure 2; inability to feel at least 7 of the 10 spots indicates loss of protective 102 sensation (LOPS). The Ipswich Touch Test (IpTT) is a simple alternative neurologic test that requires only the provider’s index finger. During the IpTT, the patient is instructed to close his/her eyes while the provider lightly rests his or her index finger on the patient’s first, third, and fifth toes for a few seconds. Patients are instructed to respond “yes” every time they feel the provider’s light touch. Two or more insensate areas are indicative of peripheral neuropathy based on this test. In a trial conducted in 2011, the IpTT was found to be equally sensitive and specific to the SWMF test.19
Patient education is a critical component of the office visit as it serves to inform the patient about their diagnosis, manifestations of the disease process, and allows them to take an active role with the treatment team; engaged patients often are more adherent to recommendations and treatment options. This part of the visit gives healthcare professionals the opportunity to equip patients with the knowledge needed to allow them to take control of their foot care and report any new findings of pain, swelling, lesions, or discoloration.
Foot Type and Shoe Selection
All patients who begin a new exercise program should consider the importance of appropriate shoes. In many cases, incorrectly chosen or worn out shoes may be the cause of considerable injury. Improper shoe wear has been implicated in a host of lower extremity complaints including hallux valgus (bunions), hammertoes, plantar fasciitis, and hindfoot pain, in both children and adults.20-23 Because of the important contribution shoes have on foot health, it behooves healthcare providers to understand shoe anatomy.
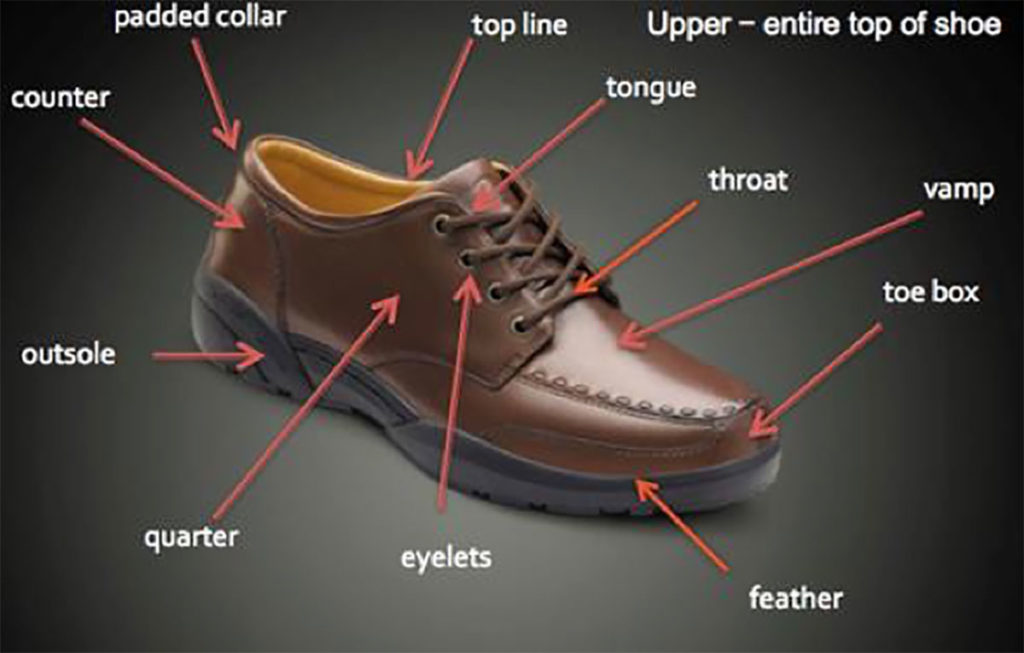
Basic shoe anatomy may be best described in terms of the Oxford dress shoe (Figure 3). The standard shoe consists of the top portion of the shoe, called the upper, and the bottom of the shoe, called the sole, which is generally broken into three parts: the outsole, midsole, and inner sole. The outsole is the part of the shoe touching the ground, while the midsole is sandwiched between the outsole and the upper. The innersole is generally the inside part of the shoe touching the foot. Many shoes will also have a “sock liner” or removable insert.
The various parts of the shoe upper include:
- the toe box (the front aspect of the shoe where the toes sit),
- the throat (the portion that rises onto the top of the foot, generally where the laces are located),
- the vamp (the section between the throat and the toe box),
- the quarter (essentially, the sides of the shoe), and
- the heel counter (the curving aspect at the back of the shoe that holds the heel).
The shoe may additionally contain padding and decorations for comfort or style. Shoes are generally manufactured from a pre-made mold, or last, which determines the shape of the shoe. Shoes are generally available as straight- or curved-lasted (Figure 4). The shape of the shoe will have significant effects on fit and function and may affect some patients’ pre-existing pathology.
When educating patients about shoes it is helpful to simplify the many available choices into the following three options:
- Neutral shoe – midrange stiffness and cushion with few additional components built into the shoe. A neutral shoe may be recommended for patients with a rectus foot type—those who do not overpronate (roll too far inward) or supinate (roll outward). The neutral shoe has equal amounts of cushioning and stability to help absorb shock.
- Motion control shoe – also called “anti-pronation” shoes, has additional components, such as internal stiffeners and heel wedges, to prevent excessive foot pronation during walking. These shoes are most appropriate for patients with planus foot types because built-in components, such as stiffer heels, counter the excessive motion seen in over-pronation.
- Cushion shoe – provides extra shock absorption for walking and tends to be more flexible throughout the shoe upper and sole. Cushioned shoes are recommended for those with cavus feet to compensate for the poor shock absorption of a high-arched foot.24
It is important to understand, though, that the foot is a highly complicated anatomical structure that does not always conform to these general rules and we recommend consultation with a podiatric foot and ankle physician whenever patients present with foot pain.
Characteristics of Good Footwear

Figure 4. Example of a straight lasted shoe. Note the lack of curvature or “C” shape in the outsole of this athletic shoe.
The choice of appropriate footwear is a highly subjective process. However, some objective characteristics of quality shoes may be made. Shoes should be sized correctly, with a snug, but not too tight fit. The shoe should be made from quality materials to prevent premature breakdown. A quality shoe typically has a removable insert that is not glued to the insole. Determination of shoe stability is also essential prior to wear. We recommend three simple tests to assess the quality of the shoes and appropriate foot support provided. Figures 5A-C demonstrate these tests and show examples of a poor-quality shoe (page 48).
Recommendations on Buying Shoes
When purchasing new shoes, various factors should be considered to optimize fit and decrease the chance of foot, leg, back pain, or injury. We make the following recommendations to patients to find the “right fit” (see Table 2).
Implications for Practice
Implementing a walking program clearly has many benefits for overall patient health. Making the appropriate footwear choice will contribute to preventing shoe-related foot problems and keep patients healthy. Healthcare providers are ideally suited to provide a thorough foot examination and make appropriate footwear recommendations for their patients who start walking exercise programs.

Figure 5. Tests to determine shoe stability. A. Shoe counter test. Squeeze the lower portion of the shoe counter. A quality shoe will not allow the counter to collapse inward. B. Shoe torsion test. Holding the heel counter and toe box, attempt to twist the shoe. A quality shoe will not allow significant twist. C. Flex test. Attempt to compress the anterior aspect of the shoe with the posterior part. A quality shoe should allow the vamp to bend only at the same location the toes would normally bend and nowhere else. Additionally, further compression of the shoe should not occur.
- US Department of Health and Human Services. Physical Activity Guidelines. 2nd Ed. Washington, DC: Office of Disease Prevention and Health Promotion; 2008. Last update: 2019. Available at http://health.gov/paguidelines/guidelines/adults.aspx. Accessed Aug. 1, 2019.
- World Health Organization. Physical Activity and Adults. In: World Health Organization. Global Strategy on Diet, Physical Activity and Health. New York, NY; 2015. Last update: 2019. Available at http://www.who.int/dietphysicalactivity/factsheet_adults/en/
- Centers for Disease Control and Prevention. Adult Obesity Facts, 2015. Available at http://www.cdc.gov/obesity/data/adult.html. Accessed Aug. 1, 2019.
- Centers for Disease Control and Prevention. Diabetes report card, 2014. Available at Retrieved http://www.cdc.gov/diabetes/pdfs/library/diabetesreportcard2014.pdf. Accessed Aug. 1, 2019.
- Centers for Disease Control and Prevention. Facts about physical activity, 2014. Available at http://www.cdc.gov/physicalactivity/data/facts.htm Accessed Aug. 1, 2019.
- Roller M. Motivators and barriers to exercise adherence. Nursing and Residential Care. 2012;14(9):482-485.
- O’Connor S, Tully M, Ryan B, et al. Walking exercise for chronic musculoskeletal pain: Systematic review and meta-analysis. Arch Phys Med Rehabil. 2015;96(4):724-734.
- Lee S, Seo B, Chung S. The effects of walking exercise on physical fitness and serum lipids in obese middle-aged women: Pilot study. J Phys Therap Sci. 2013;25(12):1533-1536.
- Murphy M, Nevill A, Murtagh E, Holder R. The effects of walking on fitness, fatness and resting blood pressure: A meta-analysis of randomized, controlled trials. Prev Med. 2007;44(5):377-385.
- Habibzadeh N. The effect of walking exercise on bone mass density in young thin women with osteopenia. Bone. 2011;48(S2):269.
- Ikeda H, Ishizaki F, Shiokawa M, et al. Correlations between walking exercise and each of bone density, muscle volume, fluctuations of the center of gravity, and dementia in middle-aged and elderly women. Internat Med J. 2012;19(2):154-157.
- Zhao W, Ukawa S, Kawamura T, et al. Health benefits of daily walking on mortality among younger-elderly men with or without major critical diseases in the new integrated seniority investigation project: a prospective cohort study. J Epidemiol. 2015;25(10):609-616.
- Sung K, Bae S. Effects of a regular walking exercise program on behavioral and biochemical aspects in elderly people with type II diabetes. Nurs Health Sci. 2012;14(4):438-445.
- Henson J, Davies M, Bodicoat D, et al. Breaking up prolonged sitting with standing or walking attenuates the postprandial metabolic response in postmenopausal women: a randomized acute study. Diabetes Care 2016;39(1):130-138.
- Menz H, Auhl S, Ristevski S, et al. Evaluation of the accuracy of shoe fitting in older people using three-dimensional foot scanning. J Foot Ankle Res. 2014;7(3):1-9.
- Nixon B, Armstrong D, Wendell C, et al. Do US veterans wear appropriately sized shoes: The Veterans Affairs shoe size election study. J Amer Podiatr Med Assoc. 2005;96(4):290-292.
- Teyhen D, Thomas R, Roberts C, et al. Awareness and compliance with recommended shoe guidelines among US Army soldiers. Mil Med. 2010;175(11):847-854.
- Lavery L, Armstrong D, Vela S, et al. Practical criteria for screening patients at high risk for diabetic foot ulceration. Arch Intern Med. 1998;158(2):157-162.
- Rayman G, Vas P, Baker N, et al. The Ipswich Touch Test: a simple and novel method to identify inpatients with diabetes at risk of foot ulceration. Diabetes Care. 2011;34(7):1517-1518.
- Dufour A, Broe K, Nguyen US, et al. Foot pain: Is current or past shoewear a factor? Arthritis Rheum. 2009; 61(10):1352-1358.
- Menz H, Roddy E, Marshall M, et al. Epidemiology of shoe wearing patterns over time in older women: associations with foot pain and hallux valgus. J Gerontol A Med Sci. 2016;71(12):1682-1687.
- McRitchie M, Branthwaite H, Chockalingham N. Footwear choices for painful feet—an observational study exploring footwear and foot problems in women. J Foot Ankle Res. 2018;11(23):1-7.
- Wegener C, Hunt A, Vanwanseele B, et al. Effect of children’s shoes on gait: a systematic review and meta-analysis. J Foot Ankle Res. 2011;4(3):1-13.
- American Podiatric Medical Association. Which running shoe is right for you? Available at https://www.apma.org/Patients/HealthyFeetTips.cfm?ItemNumber=9865. Accessed Aug. 1, 2019.