 Research supports the use of balance training to improve physiological and clinical outcome measures in patients with chronic ankle instability. Now researchers and clinicians must use that knowledge to optimize the incorporation of balance training into CAI rehabilitation protocols.
Research supports the use of balance training to improve physiological and clinical outcome measures in patients with chronic ankle instability. Now researchers and clinicians must use that knowledge to optimize the incorporation of balance training into CAI rehabilitation protocols.
By JoEllen M. Sefton, PhD, ATC, CMT, and Kenneth E. Games, MEd, ATC
Chronic ankle instability is a common condition affecting thousands of individuals. Researchers have learned a great deal about this multifaceted injury; however, we still do not fully understand the condition or its causes. Likewise, we continue to lack a true understanding of how common rehabilitation procedures like balance training influence this condition. While there is much still to learn, clinicians can take advantage of current knowledge to insure they are achieving the best possible outcomes for their patients.
Introduction
Lateral ankle sprains are thought to be the most common injury incurred in active populations.1 Contributing to this high rate of injury is the tendency among those who sustain an initial sprain to develop chronic ankle instability (CAI). This condition affects 40% to 70% of those experiencing a lateral ankle sprain,2,3 and is defined as a tendency toward repeated ankle sprains and recurring symptoms (i.e., weakness, giving way, and instability).4 Although a wealth of literature has been devoted to better understanding of this disability, the cause of CAI has yet to be determined and likely includes multiple contributing factors.5-7
Rehabilitation protocols for CAI are fairly uniform, designed to address suspected deficits, and typically include some form of strength, balance, and range-of-motion exercises. Balance training (called balance, proprioception, or neuromuscular training) is almost universally included and is easy for patients to perform even without equipment.8,9 Multiple studies have suggested that individuals with CAI have balance deficits;6,7,10,11 and several indicate that balance training in different populations produces improvements in measures of postural control.12-14 Given the extent to which balance training is included in rehabilitation protocols for CAI, it is important for clinicians to better understand balance, balance deficits, and the protocols used to address this issue.
Balance is critical not only in executing difficult athletic maneuvers, but also in quiet standing, climbing stairs, walking on uneven terrain, and bending to pick up a child. Balance and maintenance of postural control is a multisystem process requiring critical input from the vestibular, visual, and proprioceptive systems (Figures 1-4). Information regarding body position, gravity, musculosekeletal activity, tactile and visual feedback, and other input provides the nervous system with the information required to maintain balance during daily activities taking place in an ever-changing environment.
The human body has a remarkable ability to adapt and overcome deficits to perform as required. If CAI produces deficits in sensorimotor function, muscular strength, or joint motion, this may result in a decreased ability to maintain posture. Adaptations in gait that may occur as a result put additional stresses on joints, tendons, ligaments, and muscles up the kinetic chain. We as practitioners often see these accommodations resulting in pain or discomfort in the knees, hips and low back. Thus, CAI is a concern, not because of the pain and disability it produces at the ankle, but also because of the potential resulting pathologies that can occur in other areas of the body.
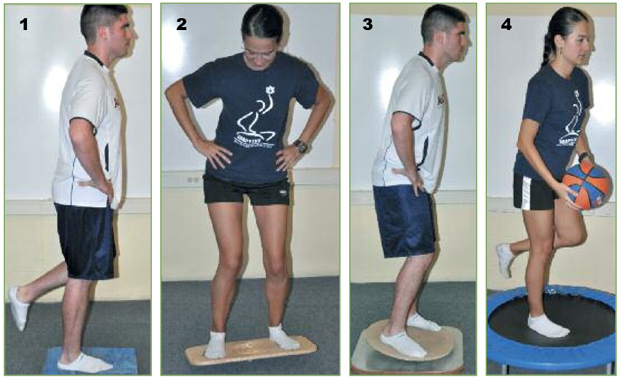
Figure 1. Foam pad, single leg stance. Figure 2. Adjustable level balance board with marble maze skill task. Figure 3. Instrumented balance board with computer tracking. Figure 4. Mini-trampoline with functional task
Clearly this condition and how we go about rehabilitating it warrants our attention. A review of the literature on balance training brings to light several questions:
1) What are the physiological effects of balance training?
2) What are the known clinical effects of balance training in in individuals with CAI?
3) How is balance training best utilized?
4) If we are able to improve an individual’s ability to maintain balance and postural control through rehabilitation, will we see a resulting decrease in maladaptations?
In attempting to answer these important questions, we realize we still have much to learn.
Physiological effects of balance training
While this seems like the logical question to answer first, this may be the area in which we have the least knowledge. Researchers are trying to determine why some individuals develop CAI after a lateral ankle sprain (non-copers) while others do not (copers). Initial studies have revealed differences in postural control10 and foot position during gait15,16 between these groups. Individuals that develop CAI are thought to have deficits in sensorimotor function,7,17,18 supraspinal motor control mechanisms,19 joint position sense,20,22 muscle strength,23 neuromuscular control,23 postural control,11,24 and joint kinematics.25 Little research has been completed that directly assesses how balance training influences these deficits in individuals with CAI, as research to date has focused primarily on changes in clinical outcomes such as strength and postural control.
Research on physiological measures has focused on the sensorimotor system. This system integrates sensory input to produce appropriate motor output. Sensorimotor deficits are thought to be instrumental in CAI. Deficiencies in joint kinesthesia have received much attention, as their consequence may be incorrect placement of the foot/ankle complex during gait,26 landing from a jump, or with other activities that may result in tripping and potential reinjury. Several studies have indicated possible deficits in joint kinesthesia in individuals with CAI.21,22,27
Investigations evaluating changes in joint position sense after balance training have been equivocal. Work in our neuromechanics research lab at Auburn University, for example, found no differences in inversion joint position sense in individuals with CAI, possibly because of the small changes produced and the difficulty in assessing this measure accurately.23,28,29
Reflex activity
Another area of sensorimotor focus has been the role of spinal reflexes and motoneuron pool excitability in CAI. Deficits in this system would influence all areas of motor control and response. Research has suggested reflex inhibition after injury as a possible physiological mechanism responsible for strength deficits in the ankle invertors.30,31 Decreased forces from the musculature surrounding the ankle are thought to serve as a protective mechanism, reducing forces that would further damage injured tissues.23 While decreases in muscular strength resulting from motoneuron pool inhibition may serve as a protective adaptation during acute stages of injury; failure to resolve this inhibition may be involved in producing the chronic deficits found with CAI.
Inhibition of the motoneuron pool may also influence muscle activation patterns. Alteration of feedback from the lateral ankle ligaments has been shown to influence muscle activation of the dynamic ankle stabilizers.32 Moreover, inhibition of muscles that act on joints proximal to the ankle has been shown to occur in participants with CAI.33 Taken together, this work suggests changes in timing and strength of muscle activation may be involved in the clinical deficits seen in individuals with CAI.
Several studies have utilized a balance board as a way to demonstrate functional adaptation of the spinal reflexes in healthy and elderly populations.34,35 In one study36 this central nervous system adaptation was correlated with the clinical outcome of improved static balance, providing a direct connection between the sensorimotor system and measures of postural control. Studies with CAI participants indicate that six weeks of balance/coordination training resulted in improved peroneal reaction times,37 inversion joint position sense, and motoneuron pool excitability (specifically recurrent inhibition).29 Research suggests that ankle bracing facilitates peroneus longus stretch reflex activity during sudden ankle inversion,38 suggesting that use of a brace during rehabilitation may improve results. Work in our lab indicated that modulation of the motoneuron pool excitability does not occur if the CAI ankle is braced during rehabilitation.39 This may suggest that movement at the ankle during rehabilitation is important in producing the desired training adaptations. These studies measure slightly different aspects of the sensorimotor system, and clearly, more work needs to be done in this area for clinicians to understand the physiological mechanisms involved in the changes that occur with balance training.
Together, these studies suggest that the sensorimotor system is involved to some degree in the deficits found with CAI, and that balance training can be utilized to address some of these issues. As we begin to understand these mechanisms more completely, we may be able to advance our rehabilitation protocols to improve clinical outcomes.
Clinical effects of balance training
Multiple studies have looked at the clinical effects of balance training alone or in conjunction with other rehabilitation protocols in individuals with CAI. Modulation of postural control is the most consistently reported effect. However, comparing studies is difficult as researchers often use different measures of postural control in both static and dynamic assessments. A 2008 review13 found balance training may decrease the risk of acute injury or reinjury, but that the effects on CAI were as yet undetermined. A review of functional rehabilitation (using a balance/wobble board) and functional assessment studies indicates that most patients with CAI reported improved postural control and self-reported function.40
A 2008 study utilizing four weeks of balance training in individuals with CAI revealed improved static balance (time-to-boundary measures), and dynamic balance (Star Excursion Balance Test).41 Six weeks of balance board training with stochastic resonance stimulation was found to improve postural control measures in participants with functional ankle instability.42 However, a balance board with a marble maze resulted in improved dynamic balance in the anterior-posterior directions, but not the medial-lateral directions,29 and this raises the question of the importance of directionally specific rehabilitation for the inversion-eversion weakness that may be associated with CAI. Improved balance measures in functionally unstable ankles were also found after six weeks of rehabilitation incorporating balance and coordination training,28 as well as after Dura Disc and mini-trampoline training.12 Moreover, one day of intense balance training was shown to have immediate effects on balance measures in individuals with CAI.43
With regard to the effect of balance training on other clinical measures, one study found that four weeks of balance training did not influence joint laxity but did alter the relationship between shank rotation and rearfoot inversion-eversion, which could potentially have a direct effect on gait.44 Few studies have assessed strength changes resulting from rehabilitation programs that contained only balance training. One study found that 10 weeks of disc training improved isokinetic pronator strength as well as postural control measures, but more than 10 weeks of training was not beneficial.45
A recent review, however, found that evidence of pronator weakness in CAI is lacking, suggesting that if strength deficits exist, they are in the ankle invertors.23 Another study found that combining strength and proprioceptive training did not produce changes in strength.46 It is possible that balance training could have a direct or indirect influence on strength of the musculature surrounding the ankle, and future research should help answer these questions.
How is balance training best utilized?
As we begin to understand the physiological and clinical benefits of balance training, the question becomes: how do we best design rehabilitation protocols utilizing this knowledge, and will we see a resulting decrease in maladaptations or reinjury? To date, little work has been done to optimize balance/proprioception/neuromuscular training protocols. Most researchers have utilized conventional clinical rehabilitation protocols to determine the potential changes these procedures produce. Studies of changes in physiological or clinical measures over time typically assess changes before and after a four- to six-week training intervention,12,29,44,47 with training occurring three to five times per week and lasting 10 to 30 minutes per session.
Rehabilitation may include only balance training13,23,29,41,44 or balance, strength, and other neuromuscular training.37,40,42,48,49 Training protocols have included a variety of techniques, including mini-trampolines and Dura Discs,12 wobble/balance boards,29,34,40,50 and Tai Chi,51 with all producing similar improvements in balance. One study has also demonstrated that a single day of intense short-term balance training produced improvements in CAI patients with regard to the static balance measures of medial-lateral center of pressure displacement and velocity and dynamic balance measures in the medial and posterior medial directions.43 While additional work needs to be completed, this initial study suggests that balance training may yield immediate results enabling it to be utilized for specific events or to reduce frequency and length of rehabilitation protocols.
Summary
Taken together, these studies encourage the continued use of balance training for individuals with CAI. However, much remains to be done to fully understand this common method of rehabilitation.
Future research should further explore the physiological changes resulting from these protocols; determine a dose-response relationship to optimize the frequency and duration of training; further explore the differences between methods of balance training (e.g., inclusion of a skill task or directional training); explore how balance training results vary when combined with other types of rehabilitation, such as strength and range of motion; and determine if balance training reduces maladaptations and risk of reinjury in those with CAI.
With this new knowledge, clinicians will be able to better utilize this common rehabilitation protocol to optimize patient outcomes.
JoEllen Sefton, PhD, ATC, CMT, is the director of the Warrior Athletic Training Program, Warrior Research Center, and the Neuromechanics Research Laboratory at Auburn University in Alabama. Kenneth Games, MEd, ATC, is a doctoral fellow in the Neuromechanics Research Laboratory at Auburn.
References
1. Hootman JM, Dick R, Agel M. Epidemiology of collegiate injuries for 15 sports: summary and recommendations for injury prevention initiatives. J Athl Train 2007;42(2):311-319.
2. Gerber JP, Williams GN, Scoville CR, et al. Persistent disability associated with ankle sprains: a prospective examination of an athletic population. Foot Ankle Int 1998;19(10):653-660.
3. McKay GD, Goldie PA, Payne WR, Oakes BW. Ankle injuries in basketball: injury rate and risk factors. Br J Sports Med 2001;35(2):103-108.
4. Hertel J. Functional anatomy, pathomechanics, and pathophysiology of lateral ankle instability. J Athl Train 2002;37(4):364-375.
5. Hertel J. Functional instability following lateral ankle sprain. Sports Med 2000;29(5):361-371.
6. Hubbard TJ, Kramer LC, Denegar CR, Hertel J. Contributing factors to chronic ankle instability. Foot Ankle Int 2007;28(3):343-354.
7. Sefton JM, Hicks-Little CA, Hubbard TJ, et al. Sensorimotor function as a predictor of chronic ankle instability. Clin Biomech 2009;24(5):451-458.
8. Arnold BL, Docherty CL. Low-load eversion force sense, self-reported ankle instability, and frequency of giving way. J Athl Train 2006;41(3):233-238.
9. Wang HK, Chen CH, Shiang TY, et al. Risk-factor analysis of high school basketball-player ankle injuries: a prospective controlled cohort study evaluating postural sway, ankle strength, and flexibility. Arch Phys Med Rehabil 2006;87(6):821-825.
10. Wikstrom EA, Fournier KA, McKeon PO. Postural control differs between those with and without chronic ankle instability. Gait Posture 2010;32(1):82-86.
11. Brown CN, Mynark R. Balance deficits in recreational athletes with chronic ankle instability. J Athl Train 2007;42(3):367-373.
12. Kidgell DJ, Horvath DM, Jackson BM, Seymour PJ. Effect of six weeks of dura disc and mini-trampoline balance training on postural sway in athletes with functional ankle instability. J Strength Cond Res 2007;21(2):466-469.
13. McKeon PO, Hertel J. Systematic review of postural control and lateral ankle instability, part II: is balance training clinically effective? J Athl Train 2008;43(3):305-315.
14. Yaggie JA, Campbell BM. Effects of balance training on selected skills. J Strength Cond Res 2006;20(2):422-428.
15. Brown C. Foot clearance in walking and running in individuals with ankle instability. Am J Sports Med 2011;39(8):1769-1776.
16. Brown C, Padua D, Marshall SW, Guskiewicz K. Individuals with mechanical ankle instability exhibit different motion patterns than those with functional ankle instability and ankle sprain copers. Clin Biomech 2008;23(6):822-831.
17. Sefton JM, Hicks-Little CA, Koceja DM, et al. Discriminant analysis of sensorimotor measures in chronically unstable and healthy ankles. J Athl Train 2007;42(suppl 2):S-28.
18. Hertel J. Sensorimotor deficits with ankle sprains and chronic ankle instability. Clin Sports Med 2008;27(3):353-370, vii.
19. Hass CJ, Bishop MD, Doidge D, Wikstrom EA. Chronic ankle instability alters central organization of movement. Am J Sports Med 2010;38(4):829-834.
20. Boyle J, Negus V. Joint position sense in the recurrently sprained ankle. Aust J Physiother 1998;44(3):159-163.
21. Konradsen L. Factors contributing to chronic ankle instability: kinesthesia and joint position sense. J Athl Train 2002;37(4):381-385.
22. Nakasa T, Fukuhara K, Adachi N, Ochi M. The deficit of joint position sense in the chronic unstable ankle as measured by inversion angle replication error. Arch Orthop Trauma Surg 2008;128(5):445-449.
23. Holmes A, Delahunt E. Treatment of common deficits associated with chronic ankle instability. Sports Med 2009;39(3):207-224.
24. Riemann BL. Is there a link between chronic ankle instability and postural instability? J Athl Train 2002;37(4):386-393.
25. Denegar CR, Hertel J, Fonseca J. The effect of lateral ankle sprain on dorsiflexion range of motion, posterior talar glide, and joint laxity. J Orthop Sports Phys Ther 2002;32(4):166-173.
26. Tropp H. Commentary: functional ankle instability revisited. J Athl Train 2002;37(4):512-515.
27. Brown C, Ross S, Mynark RG, Guskiewicz K. Assessing functional ankle instability with joint position sense, time to stabilization, and electromyography. J Sport Rehabil 2004;13(2):122-134.
28. Bernier JN, Perrin DH. Effect of coordination training on proprioception of the functionally unstable ankle. J Orthop Sports Phys Ther 1998;27(4):264-275.
29. Sefton JM, Yarar C, Hicks-Little CA, et al. Six weeks of balance training improves sensorimotor function in individuals with chronic ankle instability. J Orthop Sports Phys Ther 2011;41(2):81-89.
30. Ryan L. Mechanical stability, muscle strength, and proprioception in the functionally unstable ankle. Austr J Physiother 1994;40:41-47.
31. Wilkerson GB, Nitz AJ. Dynamic ankle stability: mechanical and neuromuscular interrelationships. J Sports Rehabil 1994;3(1):43-57.
32. Myers JB, Riemann BL, Hwang JH, et al. Effect of peripheral afferent alteration of the lateral ankle ligaments on dynamic stability. Am J Sports Med 2003;31(4):498-506.
33. Sedory EJ, McVey ED, Cross KM, et al. Arthrogenic muscle response of the quadriceps and hamstrings with chronic ankle Modulation of the triceps surae H-reflex with training instability. J Athl Train 2007;42(3):355-360.
34. Trimble MH, Koceja DM. Modulation of the triceps surae H-reflex with training. Int J Neurosci 1994;76(3-4):293-303.
35. Trimble MH, Koceja DM. Effect of a reduced base of support in standing and balance training on the soleus H-reflex. Int J Neurosci 2001;106(1-2):1-20.
36. Mynark RG, Koceja DM. Down training of the elderly soleus H reflex with the use of a spinally induced balance perturbation. J Appl Physiol 2002;93(1):127-133.
37. Schmidt R, Benesch S, Bender A, et al. The potential for training of proprioceptive and coordinative parameters in patients with chronic ankle instability. Z Orthop Ihre Grenzgeb 2005;143(2):227-232.
38. Cordova ML, Ingersoll CD. Peroneus longus stretch reflex amplitude increases after ankle brace application. Br J Sports Med 2003;37(3):258-262.
39. Yarar C, Plueger M, Sefton JM. The effects of ankle bracing during a 6-week rehabilitation protocol on spinal reflex modulation during double and single legged stance. Presented at the 40th annual meeting of the Society for Neuroscience, San Diego, CA, November 2010.
40. Webster KA, Gribble PA. Functional rehabilitation interventions for chronic ankle instability: a systematic review. J Sport Rehabil 2010;19(1):98-114.
41. McKeon PO, Ingersoll CD, Kerrigan DC, et al. Balance training improves function and postural control in those with chronic ankle instability. Med Sci Sports Exerc 2008;40(10):1810-1819.
42. Ross SE, Arnold BL, Blackburn JT, et al. Enhanced balance associated with coordination training with stochastic resonance stimulation in subjects with functional ankle instability: an experimental trial. J Neuroeng Rehabil 2007;4(7):47.
43. Sefton JM, Hicks-Little CA, Hubbard TJ, et al. The effects of short-term intense balance training on sensorimotor function in individuals with chronically ankle instability. J Athl Train 2008;43(3):S-65.
44. McKeon PO, Paolini G, Ingersoll CD, et al. Effects of balance training on gait parameters in patients with chronic ankle instability: a randomized controlled trial. Clin Rehabil 2009;23(7):609-621.
45. Tropp H, Askling C. Effects of ankle disc training on muscular strength and postural control. Clin Biomech 1988;3(2):88-91.
46. Kaminski TW, Buckley BD, Powers ME, et al. Effect of strength and proprioception training on eversion to inversion strength ratios in subjects with unilateral functional ankle instability. Br J Sports Med 2003;37(5):410-415.
47. Rozzi SL, Lephart SM, Sterner R, Kuligowski L. Balance training for persons with functionally unstable ankles. J Orthop Sports Phys Ther 1999;29(8):478-486.
48. Ross SE, Guskiewicz KM. Effect of coordination training with and without stochastic resonance stimulation on dynamic postural stability of subjects with functional ankle instability and subjects with stable ankles. Clin J Sport Med 2006;16(4):323-328.
49. McLeod TC, Armstrong T, Miller M, Sauers JL. Balance improvements in female high school basketball players after a 6-week neuromuscular-training program. J Sport Rehabil 2009;18(4):465-481.
50. Hupperets MD, Verhagen EA, van Mechelen W. The 2BFit study: is an unsupervised proprioceptive balance board training programme, given in addition to usual care, effective in preventing ankle sprain recurrences? Design of a randomized controlled trial. BMC Musculoskelet Disord 2008;9:71.
51. Fong SM, Ng GY. The effects on sensorimotor performance and balance with Tai Chi training. Arch Phys Med Rehabil 2006;87(1):82-87.








