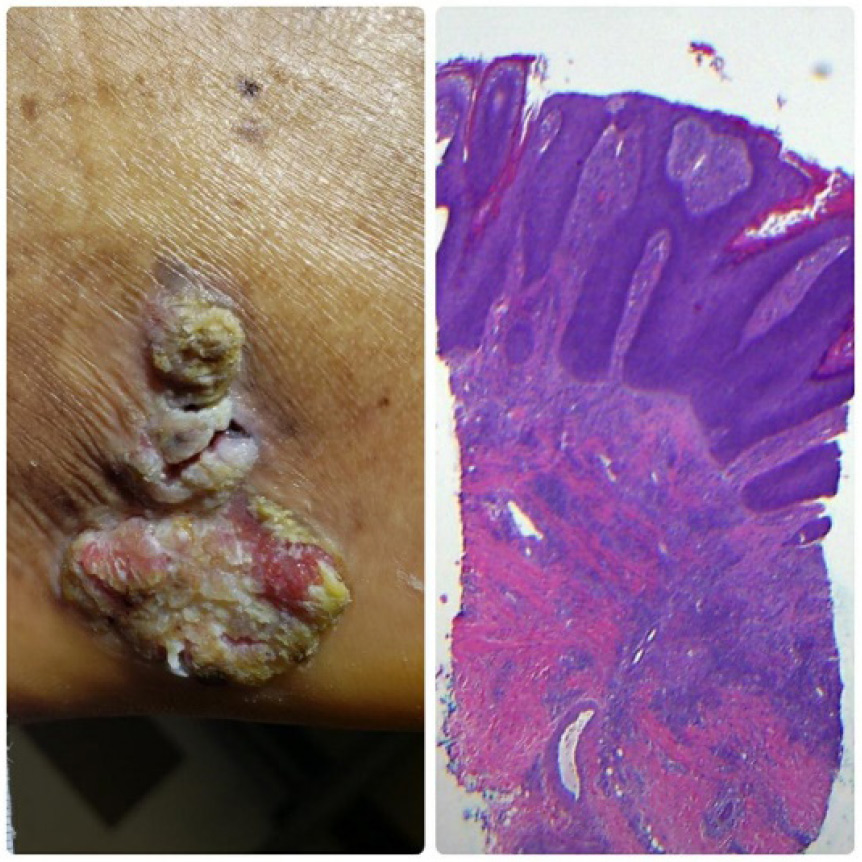
Figure 1. A) Wound of 18 months duration. B) Punch biopsy exhibits nests of large squamous epithelial cells with abundant eosinophilic cytoplasm arising from the epidermis and extending into the dermis.
By Windy Cole, DPM, CWSP
Neoplasm should be high on the differential diagnosis list when evaluating patients with chronic, non-healing wounds. Over the past 40 years, skin cancer incidence has been on the rise, growing on average 4-8% annually.1 Due to this increasing commonality of skin cancers, wound care providers are likely to frequently encounter these malignancies over the course of their clinical practice. Non-melanoma cancers make up the majority (97%) of skin cancers with basal cell carcinomas accounting for 80% of these lesions and squamous cell carcinomas rounding out the remaining 20%.1 Wounds that present with common characteristics of a particular etiology, such as plantar surface neuropathic ulcers in patients with diabetes or gaiter region leg wounds in patients with a history of peripheral vascular disease and venous reflux, may not necessitate immediate concern. The possibility of malignancy should, however, be considered when ulcers fail to improve with 2-3 months of appropriate wound care or develop atypical signs, such as rolled wound margins, exuberant granulation tissue, malodorous drainage, increase in size, friable bleeding tissue base, or increases in devitalized tissue.
For those wounds that do not fit a typical pattern or etiology, appear suddenly, or change in size, color, or border irregularity spontaneously, and have not responded to regular wound care in as little as 3 weeks, ruling out the possibility of neoplasm or an underlying inflammatory condition is a necessary part of successful wound management. About 10% of the wounds seen in clinical practice can be tied to more atypical causes and will require biopsy. If a chronic wound has been unresponsive to good wound care, re-evaluation of the etiology is warranted. A good rule of thumb for when to biopsy a chronic wound is three months of appropriate therapy without discernible evidence of wound healing.
The association between neoplasms and chronic ulcers are not uncommon. This can occur as a malignant transformation of a long-standing ulcer or as a result of a primary ulcerating skin carcinoma. Unlike the contracting edge found in a healing wound, the edges of a tumor are constantly expanding. Therefore, punch biopsies should always be taken from the wound edge where these transitional cells are found. For larger lesions, a second biopsy from the center of the wound base can aid in diagnosis.
Some clinicians may be reluctant to perform a punch biopsy on a non-healing ulcer, but research has shown that most biopsied sites heal well without complications. As part of a recent study of 412 patients with chronic wounds being evaluated for moderate to high bacteria levels, 6mm punch biopsies were obtained.2 It should be noted that this is two-times larger than the standard 3mm biopsy recommended be obtained for histopathological evaluation. There was a low incidence of adverse events among this patient cohort: Only 0.24% of patients reported adverse events with only one patient developing an infection that completely cleared with oral antibiotics.3 Delays in diagnosis may have serious implications affecting patient outcomes. It is important to reassess the differential diagnosis in any wounds displaying abnormal clinical behavior.
Case Report
Herein we present a case report of a misdiagnosed malignancy of the foot to highlight the importance of proper and timely tissue biopsies.
A 61-year-old African American male presented to the wound clinic with a chief complaint of non-healing wound on the lateral aspect of the right foot. The wound has been present for over 18 months and had continued to increase in size. He was seen a year ago in another clinic and was told the wound was due to fungus. The patient was prescribed an antifungal cream and has been applying it to the wound daily as directed. Recently, the wound began to bleed and his pain level increased. He became concerned and made this appointment for a second opinion. His past medical history includes type 2 diabetes and hypertension.
Upon evaluation it was noted that the wound measured 4.3cm x 2.5cm x 0.3cm and the base consisted of a mix of hypergranulation tissue and hyperkeratotic tissue with a central fissure (Figure 1). Based on the wound appearance and history. there was suspicion that this wound was caused by a malignant process. At this time, a 3mm punch biopsy was obtained which included a sample of all tissue types (normal, hypergranular, and hyperkeratotic) from the distal wound border. This specimen was sent to a dermatopathologist for evaluation.
The biopsy specimen exhibited nests of large squamous epithelial cells with abundant eosinophilic cytoplasm arising from the epidermis and extending into the dermis consistent with squamous cell carcinoma (Figure 1). The case was presented at the hospital tumor board where it was determined Mohs surgery would be the most appropriate treatment plan. The patient is now scheduled for this procedure.
Nota Bene
- Melanomas in Blacks, Asians, and native Hawaiians most often occur on nonexposed skin with less pigment, with up to 60% to 75% of tumors arising on the palms, soles, mucous membranes, and nail regions.
- In nonwhites, the plantar portion of the foot is often the most common site of skin cancer, being involved in 30% to 40% percent of cases.
- People of color have higher percentages of acral lentiginous melanoma (ALM, melanoma of the palms, soles, and nailbeds) than Caucasians, whereas superficial spreading melanoma is the most frequent subtype in Caucasians and Hispanics.
- Squamous cell carcinoma is the most common skin cancer in Blacks.
Source: The Skin Cancer Foundation (skincancer.org)
Conclusion
When it comes to the diagnosis of malignant wounds, timely tissue biopsy is key. A punch biopsy to obtain an adequate sample of epidermal and dermal tissue will aid the timely diagnosis of these lesions. Treatment of malignancy will vary greatly based on the tumor biology, location, stage, and the overall health of the patient. Working directly with a skilled dermatopathologist or histopathologist to evaluate your biopsies is invaluable. When an invasive malignant tumor is diagnosed, the first referral should be to an oncologist. If it is determined that the malignancy is solely located in the skin, surgical excision to remove the lesion is the best course of treatment. Performing a frozen section of the wound margins while in surgery is critical to make certain the entire tumor is removed. It is important to adequately mark the tumor for orientation to aid the pathologist. A common practice is to throw a long suture at the proximal edge and a short suture on the medial edge.
Large destructive tumors, such as a fibrosarcoma, or aggressive lesions, such as invasive melanomas greater than 1mm, may necessitate amputation. Ordering an MRI to evaluate the extent of soft tissue involvement prior to surgery is extremely helpful in determining the level of amputation and incision planning. Amputations should be performed to provide optimal functional outcomes for the patient. Proper patient management in these cases is multidisciplinary, often requiring collaborative efforts between the podiatrist, oncologist, physical therapist, and pedorthist.
Windy Cole, DPM, CWSP, serves as Adjunct Professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine and Student Rotation Coordinator, UH Richmond Medical Wound Center, both in Cleveland, Ohio. She is a dedicated healthcare advocate with interests focused on medical education, diabetic foot care, wound care, limb salvage, clinical research, and humanitarian efforts. Dr. Cole has published extensively on these topics and is a sought-after speaker both nationally and internationally. Dr. Cole also serves as a member of the Editorial Advisory Board for LER.
- Nicoletti G, Brenta F, Malovini A, Musumarra G, Scevola S, Faga A. Study to determine whether intraoperative frozen section biopsy improves surgical treatment of non-melanoma skin cancer. Mol Clin Oncol. 2013;1(2):390-394.
- Le L, Baer M, Briggs P, et al. Diagnostic accuracy of point-of-care fluorescence imaging for the detection of bacterial burden in wounds: results from the 350-patient fluorescence imaging assessment and guidance trial. Adv Wound Care (New Rochelle). 2020;Sep 25.
- Serena TE, Cole W, Coe S, et al. The safety of punch biopsies on hard-to-heal wounds: a large multicentre clinical trial. J Wound Care. 2020;29(Sup2c):S4-S7.