
iStockPhoto.com # 168465181
Does obesity affect balance and serve as an indicator of fall risk in this vulnerable population?
Excerpt By Thurmon E. Lockhart
The burden of obesity is rising at an alarming rate for older adults. The prevalence of obesity (BMI >30 kg/m2) is higher in older adults aged 60 and over (37%) than in younger adults5 and is associated with risk factors for various health conditions (e.g., cardiovascular diseases, stroke and diabetes). Obese individuals also have higher chances of sustaining injuries compared to their lean counterparts. Falls were identified as the most common cause of injury (36% of all injuries) in obese adults and obese older adults fell almost twice as frequently (27%) as their lean counterparts (15%).
Although epidemiological studies clearly link increased fall risk to obesity in older adults, the mechanism through which obesity increases falls and fall risk is unknown. Indeed, an array of obesity-related physiological and biomechanical factors induce postural/gait alterations that may increase fall risks. For example, obesity is associated with an anteriorly displaced center of mass (COM) and influences trunk posture while standing and walking, which may impair static and dynamic stability. Obesity may also influence the development or progression of a wide variety of musculoskeletal conditions that may influence body movement and postural stability,17,18 leading to more falls. Furthermore, additional postural and gait-control constraints associated with obesity are largely unidentified and their role unknown.
This article has been excerpted from Frames CW, Soangra R, Lockhart TE, et al. Dynamical Properties of Postural Control in Obese Community-Dwelling Older Adults,” which appeared in Sensors; 2018;18:1692. References have been removed for brevity. Use is per the Creative Commons Distribution 4.0 International License. To read the full article, go to https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6021983/
In this study, to quantify the dynamical properties of postural stability, several nonlinear measures, expressed as time series of center of pressure (COP) trajectories in both force plate and inertial measurement units (IMU), were employed. These measures were anticipated to provide further insights into postural control mechanisms associated with obesity. In order to improve accessibility of routine analysis of gait and posture in assessing fall risk of an individual, a wearable wireless accelerometer-based gait and postural analysis system (along with the traditional force plate) was employed.
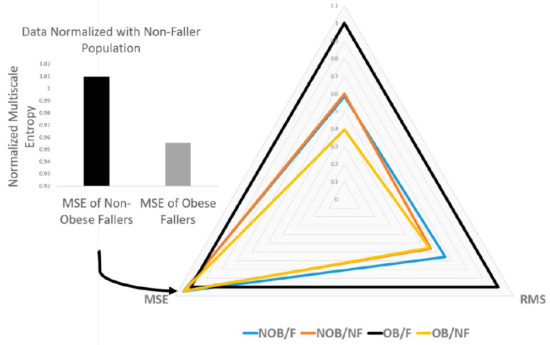
Figure 1. Radar plot of significant discriminative parameters. F, faller; NF, nonfaller; NOB, nonobese; OB, obese.
Dynamic postural control, defined as the ability to maintain equilibrium despite the presence of small disturbances or control errors, is a fundamental motor task that must be rapidly adapted in the face of a dynamically varying environment. Within physiological systems, variability from internal and external stressors is often synonymous with error. However, over the past three decades, focus has shifted from the amount of variability in the system to the time-dependent structure of variability to represent the system’s global health. Using a dynamical systems theoretical framework, it has been reported that physiological systems are inherently complex and nonlinear in nature. A variety of mathematical analyses have been developed since then to calculate how the system dynamics change throughout the lifespan or due to pathology.
Within system dynamics, the loss of complexity hypothesis was introduced, which suggested as adults age, the complexity of their dynamics decreases. In the years following, the loss of adaptability and optimal movement variability models were developed with a bidirectional consideration, suggesting that too little or too much complexity reflects a less adaptive system.51 These new models bridged the observations supporting the loss of complexity hypothesis while also explaining the increased complexity observed in certain tasks and populations. With these conceptual frameworks in mind, researchers have generally interpreted the degree of complexity within system dynamics as indicative of its adaptive capacity—a reflection of the system’s global health.
The aim of this study was to determine if obesity affects balance in community-dwelling older adults and serves as an indicator of fall risk.
Methods
Ninety-eight community-dwelling older adults (mean age 74.3±7.6 years) participated in the study. This sample size was selected to provide a smaller confidence interval on the estimated error rate when classifying fallers and non-fallers.36 Study participants were divided into three groups based on their BMI: normal (19≤BMI<25 kg/m2), overweight (25≤BMI<30 kg/m2), and obese (30≤BMI<40 kg/m2).36 Fall history was recorded retrospectively for two years with emphasis on frequency and characteristics of the falls. Any person with at least one fall in the prior year was classified as a faller and the others as non-fallers.
The study was conducted in four separate community centers throughout Virginia using the same set of instruments (IMU and force plate) on four different days. All measurements were performed barefoot in quiet standing, looking in the forward direction, with foot placement standardized. Participants were asked to stand in two visual conditions: eyes open (EO) and eyes closed (EC). Each measurement lasted for 60 seconds and was repeated twice. The sampling rate was 100 Hz. A rest of three minutes was provided between each measurement.

Figure 2. Ensemble patterns of postural stability of fallers and non-fallers exhibiting fallers with lager area of sway with lower sample entropy.
Key Findings
- Postural and gait stability is compromised in obese fallers.
- Acceleration-based gait and postural parameters are able to distinguish between obese fallers and non-fallers.
Discussion
This study investigated the effects of obesity on fall risk in community-dwelling older adults, utilizing nonlinear analyses on signals acquired from force plate and IMU measurements. A significant increase in linear parameters (mean radius, ellipse area, sway range, root mean square [RMS], standard deviation [SD]) was identified for obese older adults. Nonlinear regularity measures through multiscale entropy revealed that the presence of obesity and fall risk had a loss of complexity (Figure 1).
In the present study, entropy-based estimations of organizational variability delineate the adaptive capacity of obese participants to maintain balance. Obese older adults were found to have significantly lower approximate entropy (ApEn) and sample entropy (SaEn) values during prolonged quiet standing in the anterior-posterior (AP) direction, indicating greater regularity and possibly decreased complexity. The findings coincide with previous investigations37 linked with the theory of decreased complexity attributed to pathology and aging.47 Bodily degrees of freedom are constrained in the AP direction compared to the medio-lateral (ML) direction, whereby coordination of the physiological system, coupled with environmental stressors, lead behavioral processes into less complex, more stable response modes—a more regular sway pattern with closed-loop short-term dependencies to restore balance. The motor system is unable to adjust to the demands inherent to obesity; therefore, movements transition to a more rigid postural-control behavior (repeated patterns and decreased complexity) in the AP direction that diminish both adaptability and stability. In this context, the increase in regularity and possible decrease in complexity may be a result of impaired feedback control or impaired proprioception leading to a reduced adaptive capacity of the postural system.

Postural stability was assessed in this study using the Lockhart Monitor app, which is available in the Apple App Store. The app also assesses walking speed.
Conclusion
Obesity in older adults is recognized as an important issue with fall risk implications. However, little is known about the relationship between obese elderly persons and their gait characteristics. The present study suggests that body weight influences postural balance in obese elderly individuals and both traditional biomechanical parameters and nonlinear measures could help detect fall risk in persons who are obese (Figure 2). Inertial sensors can be used to detect fall risk caused by higher body mass in elderly individuals. Findings indicate that a change in temporal structure of COP variability as measured by a simple IMU system can detect postural changes due to obesity in elderly persons.







