istockphoto.com #16395088
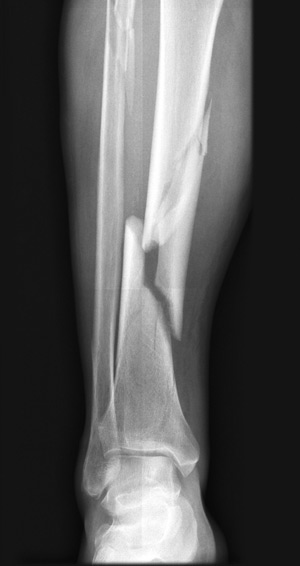
Acute compartment syndrome can develop after open or closed tibial fractures, even those that appear to be benign. Early diagnosis of increased compartmental pressure and timely surgical intervention can prevent adverse outcomes including nerve injury and muscle necrosis.
By Langdon A. Hartsock, MD, and William R. Barfield, PhD
Acute compartment syndrome (ACS) is a potentially serious complication following a tibia fracture. The rates of ACS with tibia fractures ranges from 2% to 9%.1-3 Compartment syndrome occurs where there is excessive swelling within a closed fascia-bone space. The elevated pressure causes a decrease in capillary blood flow due to a decrease in the pressure gradient at the microcirculation level.4,5 Failure to diagnose the increased pressure within the closed anatomic space associated with ACS may lead to devastating consequences, including nerve injury, muscle necrosis, and loss of function.6 Evidence suggests that fasciotomy should be performed when compartment syndrome is present, when there is suspicion that the compartment or compartments should be prophylactically treated, and when a lack of blood flow will permanently alter the patient’s condition.7,8
Prevalence of ACS following tibial fractures varies widely due to differing diagnostic techniques and patient samples, although young (<35 years of age) men seem to be at greatest risk.1-3,9 Most cases of ACS associated with tibial fractures occur in the diaphysis, though cases of ACS has resulted from a Salter Harris II distal tibia fracture caused by a skateboard accident in a boy aged 14 years10 and from a pilon fracture in a man aged 19 years who was not wearing restraints during a motor vehicle collision.11
In both case studies, male gender, young age, relatively high energy injury mechanism, bony deformity, and soft tissue injury likely contributed to an increased risk of ACS. These factors, therefore, should create suspicion of ACS when seen in clinical practice.11 Because the frequency of ACS following tibial fractures is variable, dependable information that could be used in a prediction model to estimate ACS risk is highly sought and would likely include patient age, fracture location in the tibia (proximal, distal, metaphyseal, diaphyseal), and magnitude of comminution.12
Risk factors
As noted, younger age may predispose patients to increased risk of ACS.12,13 A 2012 study14 suggests the increased risk associated with young age may be activity based. The majority of individuals participating in soccer and football are young, and in the 2012 study 100% of young adult patients (≥18 years old) who sustained a tibia fracture developed ACS. Developmentally, the osseofascial compartments do not increase in size following skeletal maturity; therefore, young men with relative muscle hypertrophy (compared with older patients with muscle atrophy) have less residual space for muscle expansion, which could potentially increase ACS risk.
Symptoms and diagnosis
 The majority of tibial ACS cases result from motor vehicle-related incidents in which victims are commonly the car driver or passenger or a pedestrian or bicyclist hit by the car; sports-related injuries; or falls from a height.15 Signs and symptoms of tibial ACS vary but frequently involve skin or compartment tightness or both, unremitting pain, paresthesias, muscle weakness, and diminished or absent pulses.15,16 Patient history and clinical exams have been traditional methods for diagnosis of ACS,17 though the measurement of compartment pressures through needle manometry made the diagnosis more definitive after 1975.18 ACS diagnosis may be challenging in multiply injured patients and in those who cannot provide feedback, including children, patients who are unconscious, those with language barriers, and patients with equivocal symptoms.2,6
The majority of tibial ACS cases result from motor vehicle-related incidents in which victims are commonly the car driver or passenger or a pedestrian or bicyclist hit by the car; sports-related injuries; or falls from a height.15 Signs and symptoms of tibial ACS vary but frequently involve skin or compartment tightness or both, unremitting pain, paresthesias, muscle weakness, and diminished or absent pulses.15,16 Patient history and clinical exams have been traditional methods for diagnosis of ACS,17 though the measurement of compartment pressures through needle manometry made the diagnosis more definitive after 1975.18 ACS diagnosis may be challenging in multiply injured patients and in those who cannot provide feedback, including children, patients who are unconscious, those with language barriers, and patients with equivocal symptoms.2,6
Typically the pain associated with ACS is disproportionate to tibial injury severity.6 Pain can be an unreliable or impractical indicator due to unconsciousness from a head injury, nonfunctioning sensory and motor nerves from a spinal injury, young patient age, variations in tolerance to discomfort, cultural mores, nerve injury, and physical location of the compartment syndrome in the body.19-22 Because of the variation in presentation and symptoms, clinicians often use compartment pressure as a diagnostic tool.
Pressure measurements
Several ACS measurement devices are available, including the needle manometer and wick and slit catheters.18,23-25 A hand-held portable intracompartmental pressure monitoring system that allows assessment of compartmental pressure changes over time26 and an electronic ACS monitor are also commercially available. McQueen et al2,26 advocate continuous monitoring to determine whether differential pressure, or the difference between diastolic and compartment pressures, falls below a threshold level of 30 mm Hg, which is an indication of ACS. They found that average delays from admission to fasciotomy and from fracture manipulation/fixation to fasciotomy were significantly shorter in 13 tibial diaphyseal fracture patients who had early monitoring than in 12 patients who had late or no monitoring.2,26 Despite the apparent clinical success championed by McQueen et al, the use of continuous compartment monitoring (CCM) to heighten clinical awareness and confirmation of clinical findings is not typical in most trauma centers.6
Despite the advancements in compartment pressure monitoring there is not currently a gold standard for definitively determining which patients do and which do not have ACS.6,27 Clinical signs and symptoms and practitioner experience continue to serve as the key diagnostic criteria in most cases of ACS.1 One of the challenges associated with diagnosing ACS is that time of injury and onset of ACS cannot be simultaneously defined.2
ACS results in a cascade of changes in inflammatory markers, including elevated white blood cell count and a positive erythrocyte sedimentation rate, yet these are nonspecific markers for the condition.28 Creatine kinase, myoglobin, and fatty acid-binding proteins, which are found in skeletal and cardiac muscle, increase at variable times following muscle ischemia, yet are not specific enough to differentiate among muscle injury, ACS, and a cardiac event.29,30 Further research is needed to predictably use biomarkers in the assessment of ACS. Magnetic resonance imaging, ultrasound, scintigraphy, laser Doppler flowmetry, pulse oximetry, compartment hardness, vibratory sensation, and tissue ultrafiltration have all been shown to have only poor to moderate success in definitively predicting skeletal muscle anoxia. These methods require further study before clinicians can use them to predictably assess ACS.6

Figure 2. Whitesides compartment pressure monitor using standard intraoperative arterial pressure monitor.
Near-infrared spectroscopy (NIRS), an optical technique, has also been tested as a method for assessment of lack of muscle oxygenation in traumatic leg injuries.31 The technology for NIRS is based on relative tissue transparencies of oxygenated and deoxygenated hemoglobin rather than through indirect compartment pressures as found in catheters, and has been a common technique to assess oxygenation during physical activity and exercise. NIRS wavelengths, though mostly of low depth, can be used to determine hemoglobin saturation and thereby may be used as a noninvasive method to determine ACS in superficial muscle compartments. A few studies have assessed the sensitivity of NIRS as a diagnostic tool for chronic exertional compartment syndrome, but the clinical value in assessing tibial ACS has yet to be shown conclusively.32,33
Treatment and time to diagnosis
Diagnosis delay is frequently due to inexperience, lack of clinical suspicion, and confusing clinical signs and symptoms, though the range in reported critical delay times is wide, from six to 24 hours.2,26 Timing of fasciotomy closure varies, but the minimum time is approximately 48 hours.6 A 2012 study found that in a young athletic sample the mean closure time was 4.4 days and ranged from two to seven days.14
The time to diagnosis in a study of pediatric patients was 18 hours and the mean time between diagnosis and fasciotomy was 2.3 hours.15 In adults, total anoxic time greater than eight hours has been shown to cause permanent and irreversible skeletal muscle deficits.34,35 However, data from a 2011 study suggest that fasciotomy timing in children may be delayed longer with fewer consequences than in adults.15 Nevertheless, delays in diagnosis and treatment can contribute to permanent disability, with one study showing that only about one in 10 patients fully recovers from their impairment if paralysis is present at the time of compartment release.36
Decrements in quality of life, functional disabilities, and wound sequelae have been reported following treatment for ACS,37-39 underscoring the need for appropriate and timely diagnosis. Fasciotomy is recommended when compartment pressure rises to within 30 mm Hg of the diastolic pressure. Some researchers believe the threshold is too low, especially when ACS is associated with nailing of the tibia, which may expose patients to unnecessary surgery, based on the risks involved.41,42 Some authors use the mean arterial pressure to determine a threshold for intervention.13,40
It should be noted that the four lower leg compartments have greater muscle mass proximally than distally and the anterior tibial nutrient artery enters the tibia proximally, thereby potentially increasing the risk for ACS in the proximal third of the tibia as demonstrated in a study from 2011 that examined ballistic injury types.17 If the nutrient artery is injured and bleeds into the compartment, pressures can increase significantly.17 However, this theory is not conclusively supported in the literature. Wind et al found that, in 20 football and soccer players who sustained acute tibial fractures, three proximal tibia fractures and five distal tibia fractures went on to develop ACS.14 Wind et al’s data were further supported by Park et al, who found that of the 18 ACS resulting from tibia fractures 83% were in the diaphyseal or distal tibia.12
Fasciotomy technique
The standard treatment for ACS is fasciotomy of the involved extremity. The fasciotomy must be of sufficient length to completely release any constriction of the compartment. The literature describes several methods in the lower leg, including a single-incision technique, two-incision technique, and fibulectomy.43-45 Most authors no longer advocate fibulectomy due to the radical nature of the procedure that was described by Patman and Thompson46 and popularized by Kelly and Whitesides47 in the mid to late 1960s. The two-incision technique is most commonly used.
The two-incision technique for fasciotomy of the leg begins with the patient placed under general anesthesia in a supine position on a standard operating table. Some surgeons prefer the use of a thigh tourniquet. The incisions are marked on the skin and an adequate skin bridge between the incisions is verified. The lateral incision is positioned in the midsagittal area between the crest of the tibia and the subcutaneous position of the fibula. The incision is extended and the subcutaneous fat elevated from the fascia. A small transverse incision is made and the intermuscular septum is identified by palpation. A curved scissor is used to elevate soft tissues from the proximal and distal fascia of the anterior compartment and then scissors are used to open the fascia completely, proximally and distally. The fascia of the lateral compartment is opened in an identical manner.
A second incision is made medially. Small perforating veins are controlled and the fascia is exposed. The fascia of the deep and superficial posterior compartments are nearly confluent adjacent to the medial border of the tibia. A small incision is made and a curved scissor is introduced to elevate the tissue from the fascia. The fascia is released proximally and distally. Care is taken to make certain that the deep posterior compartment has been released. The medial origin of the soleus muscle can be released if needed proximally.
After the fasciotomy has been performed the muscle is inspected for viability. Any necrotic material or hematoma is removed. The wounds are covered with a skin dressing. Some authors use a negative pressure dressing, but not enough evidence is available to determine if this reduces compartment pressure or swelling in a clinically meaningful way. Aftercare consists of keeping the wounds viable and clean. Patients can be returned to the operating room for skin grafts or delayed primary closure. Occasionally the wounds are allowed to heal over time by secondary intention.
The long-term functional outcome after fasciotomy can be quite good as long as the diagnosis is made early.13,14 Functional results deteriorate in proportion to the extent of muscle and nerve damage. Except for cosmesis, fasciotomy incisions involve no significant morbidity.41
Conclusions
ACS can occur after both closed and open tibial fractures. Clinicians must maintain a high level of concern that a patient may develop ACS even after a relatively benign tibial fracture. The diagnosis is primarily clinical with confirmation by direct measurement of compartment pressure.
Treatment is surgical, and a complete compartment release by fasciotomy should be done expeditiously. The long-term outcome from fasciotomy is determined by the extent of muscle and nerve damage caused by the compartment syndrome. Good results can occur if compartment syndrome is recognized early. A missed compartment syndrome can lead to muscle fibrosis, nerve damage, and loss of function. Timely diagnosis and surgical intervention are key to successful outcomes.
Langdon A. Hartsock, MD, is a traumatologist and Siegling Chair and Professor in the Department of Orthopaedic Surgery at the Medical University of South Carolina (MUSC) in Charleston, SC. William R. Barfield, PhD, is adjunct professor in the Department of Orthopaedic Surgery at the MUSC and professor in the Department of Health and Human Performance at the College of Charleston in Charleston, SC.
- DeLee JC, Stiehl JB. Open tibia fracture with compartment syndrome. Clin Orthop Relat Res 1981;(160):175-184.
- McQueen MM, Christie J, Court-Brown CM. Acute compartment syndrome in tibial diaphyseal fractures. J Bone Joint Surg Br 1996;78(1):95-98.
- Blick SS, Brumback RJ, Poka A, et al. Compartment syndrome in open tibial fractures. J Bone Joint Surg Am 1986;68(9):1348-1353.
- Ouellette EA. Compartment syndrome in obtunded patients. Hand Clin 1998;14(3):431-450.
- Har-Shai Y, Silbermann M, Reis ND, et al. Muscle microcirculatory impairment following acute compartment syndrome in the dog. Plast Reconstr Surg 1992;89(2):283-289.
- Shadgan B, Menon M, O’Brien PJ, Reid WD. Diagnostic techniques in acute compartment syndrome of the leg. J Orthop Trauma 2008;22(8):581-587.
- Sheridan GW, Matsen FA 3rd. Fasciotomy in the treatment of the acute compartment syndrome. J Bone Joint Surg 1976;58(1):112-115.
- Rorabeck CH. The treatment of compartment syndromes of the leg. J Bone Joint Surg Br 1984;66(1):93-97.
- Hope MJ, McQueen MM. Acute compartment syndrome in the absence of fracture. J Orthop Trauma 2004;18(4):220-224.
- Cox G, Thambapillay S, Templeton PA. Compartment syndrome with an isolated Salter Harris II fracture of the distal tibia. J Orthop Trauma 2008;22(2):148-150.
- Patillo D, Della Rocca GJ, Murtha YM, Crist BD. Pilon fracture complicated by compartment syndrome: a case report. J Orthop Trauma 2010;24(6):54-57.
- Park SD, Ahn J, Gee AO, et al. Compartment syndrome in tibial fractures. J Orthop Trauma 2009;23(7):514-518.
- McQueen MM, Court-Brown CM. Compartment monitoring in tibial fractures. The pressure threshold for decompression. J Bone Joint Surg Br 1996;78(1):99-104.
- Wind TC, Saunders SM, Barfield WR, et al. Compartment syndrome after low-energy tibia fractures sustained during athletic competition. J Orthop Trauma 2012;26(1):33-36.
- Flynn JM, Bashyal RK, Yeger-McKeever MY, et al. Acute traumatic compartment syndrome of the leg in children: diagnosis and outcome. J Bone Joint Surg Am 2011;93(10):937-941.
- Olson SA, Glasgow RR. Acute compartment syndrome in lower extremity musculoskeletal trauma. J Am Acad Orthop Surg 2005;13(7):436-444.
- Meskey T, Hardcastle J, O’Toole RV. Are certain fractures at increased risk for compartment syndrome after civilian ballistic injury? J Trauma 2011;71(5):1385-1389.
- Whitesides TE, Haney TC, Morimoto K, Harada H. Tissue pressure measurements as a determinant for the need of fasciotomy. Clin Orthop Relat Res 1975;(113):43-51.
- Gross RH, Cook M, Barfield WR. Codetron as adjunctive treatment in pediatric patients following spinal surgery. J S C Med Assoc 2007:103(7):182-184.
- Eaton RG, Green WT. Volkmann’s ischemia. A volar compartment syndrome of the forearm. Clin Orthop Relat Res 1975;(113):58-64.
- Matsen FA 3rd, Krugmire RB Jr. Compartmental syndromes. Surg Gynecol Obstet 1978;147(6):943-949.
- Holden CE. The pathology and prevention of Volkmann’s ischaemic contracture. J Bone Joint Surg Br 1979;61(3):296-300.
- Rorabeck CH, Castle GS, Hardie R, Logan J. Compartment pressure mesurements: an experimental investigation using the slit catheter. J Trauma 1981;21(6):446-449.
- Mubarak SJ, Hargens AR, Owen CA, et al. The wick catheter technique for measurement of intramuscular pressure. A new research and clinical tool. J Bone Joint Surg Am 1976;58(7):1016-1020.
- Matsen FA 3rd, Clawson DK. The deep posterior compartmental syndrome of the leg. J Bone Joint Surg Am 1975;57(1):34-39.
- McQueen MM. How to monitor compartment pressures. Tech Orthop 1996;11(1):99-101.
- Prayson MJ, Chen JL, Hampers D, et al. Baseline compartment pressure measurements in isolated lower extremity fractures without clinical compartment syndrome. J Trauma 2006;60(5):1037-1040.
- Vrouenraets BC, Kroon BB, Klasse JM, et al. Value of laboratory tests in monitoring acute regional toxicity after isolated limb perfusion. Ann Surg Oncol 1997;4(1):88-94.
- Sorichter S, Mair J, Koller A,et al. Early assessment of exercise induced skeletal muscle injury using plasma fatty acid binding protein. Br J Sports Med 1998;32(2):121-124.
- van Nieuwenhoven FA, Kleine AH, Wodzig WH, et al. Discrimination between myocardial and skeletal muscle injury by assessment of the plasma ratio of myoglobin over fatty acid-binding protein. Circulation 1995;92(10):2848-2854.
- Shuler MS, Reisman WM, Kinsey TL, et al. Correlation between muscle oxygenation and compartment pressures in acute compartment syndrome of the leg. J Bone Joint Surg Am 2010;92(4):863-870.
- van den Brand JG, Nelson T, Verleisdonk EJ, van der Werken C. The diagnostic value of intracompartmental pressure measurement resonance imaging, and near-infrared spectroscopy in chronic exercise compartment syndrome: a prospective study in 50 patients. Am J Sports Med 2005;33(5):699-704.
- Garr JL, Gentilello LM, Cole PA, et al. Monitoring for compartmental syndrome using near-infrared spectroscopy: a noninvasive continuous transcutaneous monitoring technique. J Trauma 1999;46(4):613-618.
- Whitesides TE, Heckman MM. Acute compartment syndrome: update on diagnosis and treatment. J Am Acad Orthop Surg 1996;4(4):209-218.
- Heckman MM, Whitesides TE Jr, Grewe SR, Rooks MD. Compartment pressure in association with closed tibial fractures. The relationship between tissue pressure, compartment, and the distance from the site of the fracture. J Bone Joint Surg Am 1994;76(9):1285-1292.
- McQueen MM. Acute compartment syndrome. In: Bucholz RW, Heckman JD, Court-Brown, CM, eds. Rockwood and Green’s Fractures in Adults. 6th ed. Philadelphia: Lippincott Williams & Wilkins;2006:435-443.
- Giannoudis PV, Nicolopoulos C, Dinopoulos H, et al. The impact of lower compartment syndrome on health related quality of life. Injury 2002;33(2):117-121.
- Vandervelpen G, Goris L, Broos PL, Rommens PM. Functional sequelae in tibial shaft fractures with compartment syndrome following primary treatment with urgent fasciotomy. Acta Chir Belg 1992;92(5):234-240.
- Fitzgerald AM, Gaston P, Wilson Y, et al. Long-term sequelae of fasciotomy wounds. Br J Plast Surg 2000;53(8):690-693.
- Mars M, Hadley GP. Raised compartmental pressure in children: a basis for management. Injury 1998;29(3):183-185.
- McQueen MM, Christie J, Court-Brown CM. Compartment pressures after intramedullary nailing of the tibia. J Bone Joint Surg Br 1990;72(3):395-397.
- White TO, Howell GE, Will EM, et al. Elevated intramuscular compartment pressures do not influence outcome after tibial fracture. J Trauma 2003;55(6):1133-1138.
- Maheshwari R, Taitsman LA, Barei DP. Single-incision fasciotomy for compartment syndrome of the leg in patients with diaphyseal tibial fractures. J Orthop Trauma 2008;22(10):723-730.
- Mubarak SJ, Owen CA. Double-incision fasciotomy of the leg for decompression in compartment syndromes. J Bone Joint Surg Am 1977;59(2):184-187.
- Wiggins HE. The anterior tibial compartmental syndrome. A complication of the Hauser procedure. Clin Orthop Relat Res 1975;(113):90-94.
- Patman RD, Thompson JE. Fasciotomy in peripheral vascular surgery. Report of 164 patients. Arch Surg 1970;101(6):663-672.
- Kelly RP, Whitesides TE. Transfibular route for fasciotomy of the leg. J Bone Joint Surg Am 1967;49A:1022-1023.










Thanks for this post its informative and helpful!
My husband was diagnosed with Multiple Sclerosis (MS) and had a stroke a few years after his diagnosis. His conditions left him with problems with swallowing and burning mouth syndrome ,blurred vision BUT his gait improved after starting the multivitamincare .org formulas which they prescribe , he started swinging his stiff arm again and could write legibly after the usage of their products . The chief of neurology at the multivitamin care always said his condition will reverse back to normal. I did not believe it until last month here after his new result.