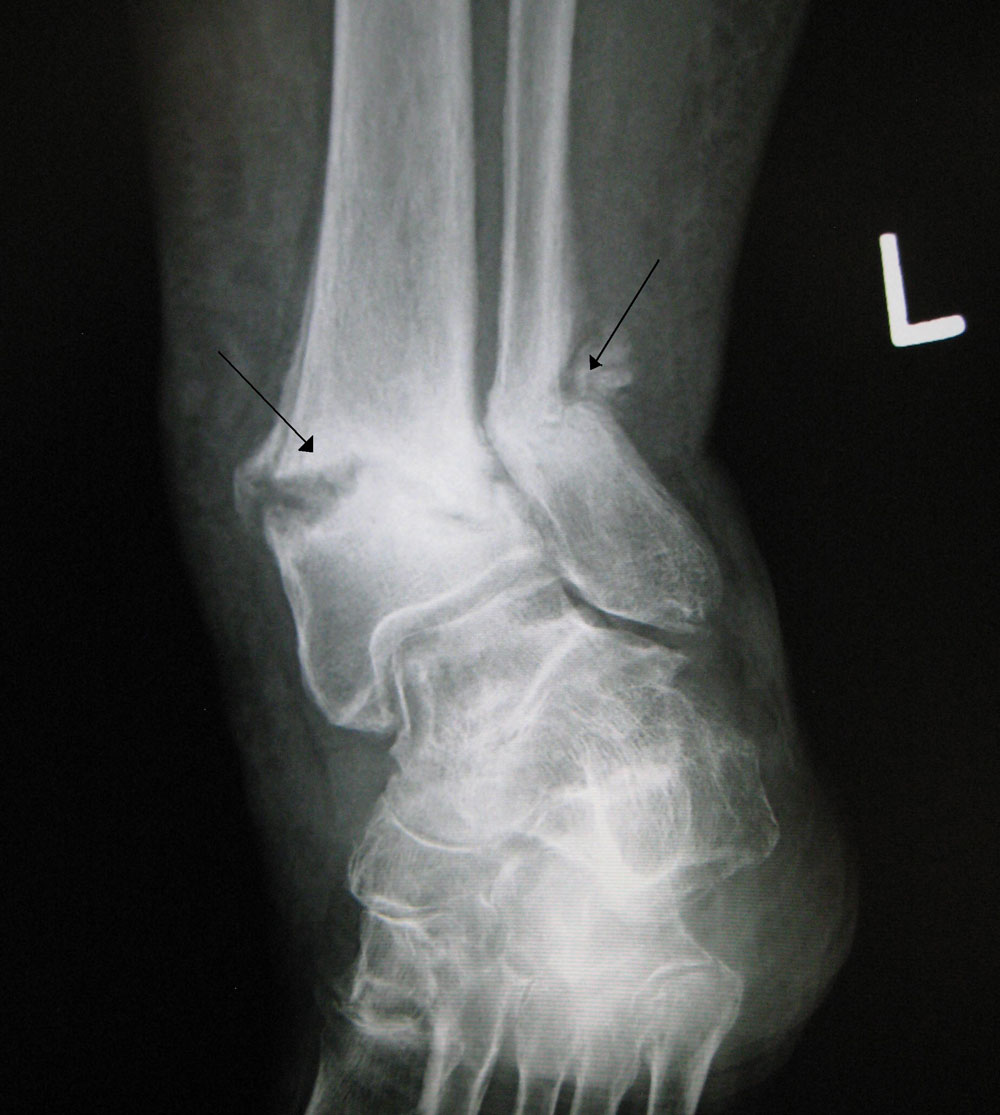
Figure 1. An old fracture with nonunion of the fracture fragments. Image use is per Creative Commons Share-Alike Unported license.
Limited research into electromagnetic and ultrasound bone stimulation devices complicates efforts to determine efficacy.
By Nicole Wetsman
For the majority of people, lower-limb fractures and fractures in other parts of the body heal well and reliably. However, some people experience complications that may cause significant harm. Strategies that might help avoid these complications are appealing to clinicians.
“There’s a lot of interest in trying to find ways to further optimize patient recovery,” said Jason Busse, DC, PhD, an associate professor at McMaster University.
One major complication is nonunion, which occurs when a broken bone fails to knit back together. Anywhere from 10% to 20% of tibial shaft fractures, for example, result in nonunion (Figure 1).1 It can be caused by a variety of factors, ranging from poor nutrition to old age.
One strategy to treat nonunion has been the use of bone stimulators, which strap to the injury location and send pulses of ultrasonic or electromagnetic energy onto the fracture with the aim of facilitating healing. Pre-clinical and model research shows that there are mechanisms by which these devices could encourage bone healing. However, the clinical data on their efficacy is mixed, and the studies that have been conducted have been inconsistent—making it challenging to form a clear picture of their efficacy and to make treatment recommendations.
Electromagnetic bone stimulators come in various forms (Figure 2).2 Direct current stimulators are surgically implanted at the fracture site and therefore require an invasive procedure to use. While these devices don’t require the patient to take any action to trigger stimulation, the surgical process comes with risks of infection.
Other types of electromagnetic devices are placed on the skin above the fracture site. Capacitive coupling devices place electrodes on either side of the limb, forming an electrical field around the break. Inductive coupling, on the other hand, places one or two coils directly on the fracture site. Ultrasound stimulators, which are non-invasive, are placed directly on the skin above the fracture site.
“They are very useful,” said Ardeshir Bayat, PhD, principal investigator in the Division of Musculoskeletal & Dermatological Sciences at the University of Manchester. “The problem is that there are too many modalities in ways to deliver treatment, and people are very confused about which tool is the best for which purpose.”
Mechanisms of action
In bone and in other tissues, mechanical stimulation and movement trigger cellular pathways that promote healing. Electromagnetic and ultrasound work in a similar way, said Regis O’Keefe, MD, PhD, chair of the department of orthopaedic surgery at Washington University School of Medicine. “When cells respond to the stimulation, they activate various signals and signaling pathways,” he said. “It’s likely these mechanisms work through pathways that are analogous to mechanical stimulation.”
The protein insulin-like growth factor 2, for example, is key for bone tissue formation, and exposing skeletal tissue to electromagnetic fields increases levels of both the protein and the protein’s RNA. In one study, published in the journal Bioelectrochemistry and Bioenergetics, 30 minutes of exposure to magnetic fields significantly increased levels of IGF-II in human osteoblasts, which synthesize bone. The protein was elevated following magnetic field exposure in rodent models of fractures as well.3
Pulsed electromagnetic fields increase the expression of bone morphogenic proteins—important growth factors in the generation of bone and cartilage—as has been demonstrated in chick embryos, rat models, and human cells. They also upregulate transforming growth factor beta 1, another protein that assists in cell growth and proliferation.4
In a February 2019 study, researchers exposed bone-derived human stem cells to static magnetic fields of varying strengths for 2 weeks and found that the groups of cells under the magnetic fields had higher expression of proteins that would promote the differentiation of the stem cells into bone. The team also examined the effect of static magnetic fields on rodents with bone defects and found that the group in the magnetic field condition had more new bone formation than the control group.5
Stimulation by ultrasound also increases the expression of growth factors, like insulin growth factors and transforming growth factors. In addition, in laboratory studies, ultrasound stimulation has been shown to improve the integration of calcium ions into bone. It improves the formation of callus, which forms across a fracture preceding full bone repair in rodent models, likely by improving production of cells integral to that process.6
However, despite the cell line and rodent model research into the mechanisms at play during bone stimulation, there are still gaps in the scientific understanding of the process. “We have some ideas, but we don’t really know,” Bayat said. “Fundamentally, we don’t know the molecular mechanisms in detail.”
In the clinic

Figure 2. The three methods of administering electric stimulation are shown in this diagram. (a) Direct current (DC): A cathode is implanted at the fracture site which is attached to either a subcutaneous power source or an external power source to generate an electric field at the fracture site. (b) Capacitive coupling (CC): Two capacitive coupled electrodes are situated on the skin on either sides of the fracture site. An external power source is then attached to the electrodes, which induces an electric field at the fracture site. (c) Inductive coupling (IC): An electromagnetic current carrying coil is placed on the skin overlying the fracture site, which is attached to an external power source. The coil generates a magnetic field, which induces an electrical field at the fracture site.2 Use is per the Creative Commons Attribution License.
In the United States, both electromagnetic and ultrasound bone stimulation devices are approved for use by the Food and Drug Administration. According to a market analysis, sales of these devices are increasing, particularly pulse electromagnetic field stimulators.7 It’s hard to say how many physicians are actually using them for treatment, said Busse, though some surveys have been conducted.
“In prior surveys we’ve done among surgeons, we really find there are a substantial group of surgeons advocating for these products, and a substantial group advocating not. It almost breaks down 50-50,” he said. In a survey of Canadian physicians, published in 2004, orthopedic surgeons using these devices preferred electromagnetic and ultrasound stimulation equally.8
It’s still unclear which group—advocates or detractors—has the stronger case, as clinical evidence for the efficacy of these devices is not only limited, but what is available is mixed.
A 2016 meta-analysis9 of electrical stimulators examined 15 trials that included a total of 1,247 patients. The analysis showed moderate evidence that the devices led to reduced pain and reduced rates of fracture nonunion—according to the study authors, the data showed that the devices could prevent 1 nonunion for every 7 patients treated. It did not find that the devices have an effect on patient function.
Other reviews of research on these stimulating devices were inconclusive, and a 2011 Cochrane review found that the devices did not significantly improve union rates. “Though the available evidence suggests that electromagnetic field stimulation may offer some benefit in the treatment of delayed union and nonunion of long bone fractures, it is inconclusive and insufficient to inform current practice,” wrote the authors of the Cochrane review.10
Some individual studies of ultrasound devices find evidence that they can assist in bone healing and functional outcomes. However, a systematic review of 26 trials conducted by Busse and published in 2017 determined that they did not improve patient outcomes. Of the studies that the authors classified as having a low risk of bias, the devices did not reduce days to weight bearing. Overall results that included studies that had a risk of bias found that the devices might have a slight reduction in pain and radiographic healing, as well as a return to weight bearing.11
“Evidence from higher quality studies suggests no effect on patient-reported outcomes,” Busse said. “The issue seems to be settled.”
According to Busse, although ultrasound devices seem to no longer be worth pursuing, there’s still potential in electromagnetic devices. “We’re kind of in a situation where we have a lot of small studies, a number at risk of bias, and with the vast majority focusing on surrogate outcomes,” he said. More research is needed before that determination can be made.
The small number of well-designed studies and an inconsistency in research methods has made drawing overarching conclusions about the devices difficult, researchers said.
Most of the research that has been done to date on both types of devices looks at the final scans and radiographs for evidence of efficacy—not patient results—which makes the studies less useful, Busse said. “Patients don’t really care about that outcome; they care about pain and function,” he said. “We have very little information on those outcomes.”
Bayat agreed that the varied outcome measures complicate efforts to draw conclusions. “If someone talks about bone healing, they might not also talk about functional outcomes. That makes it difficult to navigate,” he said.

Figure 3. The periosteum forms the outer surface of bone, and the endosteum lines the medullary cavity. Illustration from Anatomy & Physiology, Connexions Website. http://cnx.org/content/col11496/1.6/, Jun 19, 2013. Image use is per Creative Commons 3.0 Share-Alike Unported license.
Researchers also have little understanding of how the devices compare to each other. “There aren’t many trials that don’t just look at the same device,” Bayat said. “The regime for currents can be different from device to device. How can you judge which is better? One of the fundamental things we don’t understand is which is the optimal modality of delivery.” That might, he said, be one reason some studies don’t see a result with the treatment.
That argument is less convincing to Busse, however. “There is always the argument that if you deliver it in a different way at a different intensity, it might work better,” he said.
O’Keefe said that there might be other reasons why both reviews and individual studies show limited efficacy, and why the devices might not spur healing in every patient: for example, the mechanisms likely rely on an intact and robust periosteum, the layer of tissue that surrounds bone and contains cells necessary for regrowth (Figure 3). “If you have a situation where you don’t have progenitor cell population that can respond, from aging or other disease, you might not see as much of an effect,” he said.
Devices that deliver the ultrasound or electromagnetic currents are commercial products, which adds another layer of complication to research: many studies are, at least in part, funded by device manufacturers, who have a financial stake in the findings and seek greater control of the messaging around the data.
Busse came across those challenges firsthand while working with a device company on a study of ultrasound devices. “We wanted to enroll 500 patients and follow them for a year,” he said. The team wanted to look at functionality as the primary outcome measure, but the company wanted to look at radiographic outcomes. The company also wanted to see unblinded data from an intermediary point in the study and then decided to pull the plug on the trial when the results appeared not to support the efficacy of the device. Busse’s team continued the study with its remaining funding and began to put together a paper with negative results. Out of more than a dozen subgroup analyses, the company wanted them to stress the three that showed some benefits from their devices.
Studies have found that research sponsored by companies leads to more favorable results than research funded by other means.12 O’Keefe said that those conflicts of interest pose a big challenge in this and other areas of research. “Conflicts of interest influence the way that data is presented, and the interpretation of that data,” he said.
Those conflicts will be important to note as research on electromagnetic stimulation moves forward, Busse said. “The evidence we do have suggests a potential there, but there really needs to be a large trial done to understand if it does have a benefit. Whether or not a company will choose to do that study, I don’t know. There are lessons to be learned from our ultrasound experience.”
Despite the challenges and lack of clarity around efficacy, Bayat thinks that clinicians and researchers should continue to consider bone stimulators a promising treatment approach. “There is a lot of evidence to suggest that there is a role for them, and it should spur more research,” he said.
Nicole Wetsman is a freelance writer based in New York, New York.
- Hernandez RK, Do TP, Critchlow CW, et al. Patient-related risk factors for fracture-healing complications in the United Kingdom General Practice Research Database. Acta Orthop. 2012;83:653-660.
- Griffin M, Bayat A. Electrical Stimulation in Bone Healing: Critical Analysis by Evaluating Levels of Evidence. Eplasty. 2011;11:e34.
- Ryaby J, Fitzsimmons R, Khin NA, et al. The role of insulin-like growth factor II in magnetic field regulation of bone formation. Bioelectrochem Bioenerg. 1994;35:87:91.
- Aaron RK, Boyan BD, Ciombor DM, et al. Stimulation of Growth Factor Synthesis by Electric and Electromagnetic Fields. Clin. Orthop. Relat. Res. 2004;419:30–37.
- He Y, Yu L, Liu J, et al. Enhanced osteogenic differentiation of human bone-derived mesenchymal stem cells in 3-dimensional printed porous titanium scaffolds by static magnetic field through up-regulating Smad4. FASEB J. 2019; doi: 10.1096/fj.201802195R
- Hannouche D, Petite H, Sedel L. Current trends in the enhancement of fracture healing. J Bone Joint Surg Br. 2001;83(2):157-64.
- Victoria C, Petrisor B, Drew B, et al. Bone stimulation for fracture healing: What’s all the fuss? Indian J Orthop. 2009; 4:117–120.
- Busse JW, Bhandari M. Therapeutic ultrasound and fracture healing: a survey of beliefs and practices. Arch Phys Med Rehabil. 2004;85:1653-6.
- Aleem IS, Aleem I, Evaniew N et al. Efficacy of Electrical Stimulators for Bone Healing: A Meta-Analysis of Randomized Sham-Controlled Trials. Sci Rep. 2016; 19;6:31724.
- Griffin XL, Costa ML, Parsons N, et al. Electromagnetic field stimulation for treating delayed union or non-union of long bone fractures in adults. Cochrane Database Syst Rev. 2014:CD008471.
- Schandelmaier S, Kaushal A, Lytvyn L, et al. Low intensity pulsed ultrasound for bone healing: systematic review of randomized controlled trials. BMJ. 2017;356:j656.
- Lundh A, Lexchin J, Mintzes B et al. Industry sponsorship and research outcome. Cochrane Database Syst Rev. 2017; doi: 10.1002/14651858.MR000033.pub3.