To improve nonoperative management of Achilles tendon ruptures, the ankle should be immobilized at an angle that apposes the tendon ends as closely as possible without overlap. This study suggests the ideal ankle angle may be smaller than previously reported.
istock 2186453
by Walter H. Wray III, MD, Conor Regan, MD, Sagar Patel, BS, Ryan May, BS, and Selene G. Parekh, MD, MBA
Current research shows that the incidence of acute Achilles tendon ruptures is on the rise, especially in western countries during the past decade.1,2 There is currently no fully accepted consensus opinion on the treatment of these injuries.3-5
Surgical treatment is successful in terms of its low re-rupture rate, but carries with it complications involving wound healing, nerve injury, and the risks of anesthesia.6-9 Traditional nonsurgical treatment has a low complication rate and costs, but results in a higher re-rupture rate than surgical treatment.10-12
The results of nonsurgical treatment of acute Achilles tendon ruptures can potentially be improved by defining an optimal ankle flexion angle at which the tendon ends will be apposed for optimal healing.
Materials and Methods
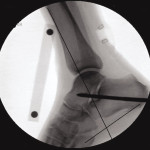
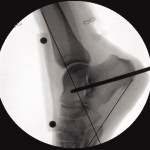
Ten unpaired cadaveric legs harvested at the distal half of the femur were studied. A uniform transverse laceration was made 4 cm proximal to the calcaneal insertion on each of the 10 legs. A skin stapler was then used to place staples on the proximal and distal tendon stumps to serve as radio-opaque markers. A joint-spanning external fixator was applied to the knee and locked in 0º, 45º, or 90º of flexion, determined using fluoroscopy. An external fixator pin was also placed into the posterior calcaneus and across the subtalar joint, with the hindfoot in 5º to 7º of valgus, both to serve as a fulcrum to accurately move the ankle and to eliminate any contribution of the subtalar or transverse tarsal joints to our measurements.
The distance between the staples at the cut ends of the Achilles tendon was then measured at six ankle positions, starting at 20º of ankle dorsiflexion and progressing in 10-degree increments to 30º of plantar flexion. These angles were calculated at the intersection of a line drawn along the anterior tibial cortex and another line drawn between the most inferior point on the calcaneus and the fifth metatarsal base. All six measurements were made with the knee in extension and then repeated with the knee at 45º and 90º of flexion (Figures 1,2). The measurements were made both grossly, using a metric ruler, and on fluoroscopic images, using a standardized length radio-opaque marker. The statistical model used for this study was a simple repeated measures model using a compound symmetric correlation structure.
Results
Knee flexion and extension was found to have no significant effect on the diastases in the Achilles tendon stumps (p = 0.21). The tendon ends were apposed at a mean ankle angle of 28.0º of plantar flexion (95% CI 25.0-33.6).
The distance between the tendon stumps is predicted to decrease by 0.76 cm for every 10º increase in plantar flexion angle (95% CI =0.73-0.79 cm). Looking at the plots of the relationship between ankle angle and distance (Figure 3), the predicted decrease in distance of 0.76 cm for every 10º increase in angle is very reliable in this data set.
Discussion
Acute Achilles tendon ruptures are common and the incidence has recently been on the rise.13-15 These injuries are especially prevalent among men in their thirties and forties who intermittently play competitive sports, although they can occur in almost any segment of the population. Nearly 80% of acute Achilles tendon ruptures occur 2 cm to 6 cm above the insertion on the calcaneus. This most common variety of Achilles rupture is seen with sudden dorsiflexion of an ankle while it is in a plantarflexed position.
Currently, there is much debate over whether surgical or nonsurgical treatment should be the preferred treatment for acute Achilles tendon ruptures. Surgical treatment has been most widely employed for younger, athletic patients, because casting is associated with higher rates of re-rupture and because patients in this population typically have a great desire to return to pre-operative levels of function. Nonsurgical treatment is generally prescribed for elderly patients with lower functional demands and poorer wound healing capability. There is, however, a large amount of crossover between groups, depending on the individual patients and surgeons. Surgical treatment, with either traditional open techniques or minimally invasive methods, has the advantages of a low rate of re-rupture (1% to 3%), a larger number of patients returning to sports, and a nearer return to normal plantar flexion strength.16 Disadvantages include wound healing complications affecting nearly one-third of patients, as well as sural nerve injuries.10,17 Nonsurgically treated patients have lower rates of wound complications, but have much higher re-rupture rates (2% to 18%).1 Recent studies have detailed the efficacy of nonoperative treatment of Achilles tendon ruptures with early weight bearing in a functional brace.19-21 Re-rupture rates for this modality of treatment range from 6% to 17%.18-20
There are numerous recommendations on optimal angle of plantar flexion for nonsurgical treatment. McComis recommended initial casting in the “gravity equinus” position with transition to a custom molded orthosis in 45º of plantar flexion.18 Weber recommended semi-rigid cast taping in 20º degrees of plantar flexion with tendon apposition confirmed by ultrasonography.19 Hufner recommended initial casting, then transition to a removable boot with a three centimeter heel lift. No specific angle of plantar flexion was recommended, but continuation of non-operative treatment required tendon apposition at 20º of plantar flexion as seen on ultrasonography.20
The optimal angle of immobilization has yet to be clearly defined. Our study suggests that immobilization in 28º of plantar flexion may be optimal for Achilles tendon ruptures that occur in the most common location of the watershed area. If ultrasonography is available in the clinic, an attempt may be made to confirm tendon apposition at that ankle angle. Further studies are needed to determine if the optimal angle of plantar flexion varies with more proximal and distal sites of rupture.
Previous findings
In a previous cadaver-based study, Sekiya et al found that the severed ends of the Achilles tendon were apposed at 60º of ankle plantar flexion.21 In contrast, our results demonstrate that extreme plantar flexion of the ankle at 50º or more may not be needed to fully appose the ruptured Achilles tendon stumps. In our study, plantar flexion beyond the average of 28º was predicted to result in impeded tendon end apposition resulting from overlap of tendon ends of 7.6mm per 10˚ of plantar flexion. This was calculated based on extrapolation of our data based on the trends of the data sets. Both studies have low numbers of specimens, so larger studies may be more conclusive.
Sekiya also used a hinged footplate device to establish and measure plantar flexion. This footplate device may have tensioned the plantar fascia, causing it to pull the calcaneus and distal Achilles tendon remnant distally. This would increase the diastasis between the tendon ends and, in turn, the resultant angle of plantar flexion needed to appose the tendon ends. Our study used a pin through the calcaneus and talus without tension on the plantar fascia, and our plantar flexion angles were determined radiographically. We believe that a well molded splint, cast, or boot with radiographic confirmation of the ankle angles would be more accurately approximated by our model than by a rigid footplate.
In our experience, patients who are immobilized at 20º of plantar flexion are more compliant and satisfied with the treatment plan than patients immobilized at 45º to 50º of plantar flexion. At 20 degrees, patients can wear custom molded orthoses that fit inside their normal shoes, custom made shoes, functional boots with rocker-

Figure 3: Data plots with regression lines showing tendon stump apposition at 28° of plantar flexion regardless of knee flexion angle
bottom soles, or even boots such as the Variostabil (Adidas, Herzogenaurach, Germany) that some patients find more aesthetically pleasing. (For custom molded orthoses worn inside shoes, the height of the heel and final angle of plantar flexion of the heel with the orthoses inside the shoe must be considered.) However, at 45º to 50º of plantar flexion, application of such functional footwear is more difficult. Patients must increase flexion at the hip and knee to swing the foot, causing further alterations in gait mechanics. It is also possible that patients may have more difficulty establishing dorsiflexion after immobilization in higher degrees of plantar flexion. This may require longer periods of physical therapy or permanent decrease in range of motion.
Our data also confirm that knee flexion angle contributes very little to the distance between ruptured Achilles tendon stumps. This supports earlier conclusions about the effects of knee flexion on tendon end displacement.21,22 In terms of clinical implications, these collected findings would support the use of a short leg cast to allow for knee range of motion while facilitating complete apposition of the Achilles tendon ends.
The limitations of this study include the low number of specimens, the slightly differing degrees of preservation between specimens, and the use of a cadaveric model to perform these measurements. The low number of specimens results in the possibility of a type I error. This was minimized with our statistical analysis, which showed internal consistency of measurements from one specimen to the next. We also recognize that the angles as measured on fluoroscopy are subject to human error and therefore are approximate. Therefore, the fluoroscopic measurements were confirmed with gross measurements. Finally, being a cadaveric study, the sharply severed tendons in this study do not take into account the surrounding altered fibers present in clinical rupture. Therefore, we cannot predict if healthy tendons will be apposed with the same degree of accuracy.
Conclusions
Our results show that maximal plantar flexion is not necessary to fully appose the tendon ends in an acute Achilles tendon rupture. The tendon stumps are ideally positioned at 28º of plantar flexion, regardless of knee position. This information may be used in future clinical studies to determine if using a lesser degree of initial plantar flexion allows for more rapid progression to a plantigrade foot during rehabilitation.
Walter H. Wray III, MD, is a resident physician in the division of orthopaedic surgery at Duke University Medical Center. Conor Regan, MD, is a resident physician in the department of orthopaedic surgery at the University of North Carolina School of Medicine. Sagar Patel, BS, is a medical student in the department of orthopaedic surgery at Warren Alpert Medical School, Brown University and Rhode Island Hospital. Ryan May, BS, is a biostatistician in the Gillings School of Global Public Health at the University of North Carolina at Chapel Hill. Selene G. Parekh, MD, MBA, is associate professor of orthopaedic surgery at Duke University Medical Center and adjunct faculty in the Fuqua Business School at Duke University.
References
1. Maffulli N. Rupture of the Achilles tendon. J Bone Joint Surg Am 1999;81(7):1019–1036.
2. Schepsis AA, Jones H, Haas AL. Achilles tendon disorders in athletes. Am J Sports Med 2002;30(2):287–305.
3. Khan RJ, Fick D, Keogh A, et al. Treatment of acute Achilles tendon ruptures. A meta-analysis of randomized, controlled trials. J Bone Joint Surg Am 2005;87(10):2202-2210.
4. Hattrup SJ, Johnson KA. A review of ruptures of the Achilles tendon. Foot Ankle 1985;6(1):34-38.
5. Cetti R, Christensen SE, Ejsted R, et al. Operative versus nonoperative treatment of Achilles tendon rupture: A prospective randomized study and review of the literature. Am J Sports Med 1993;21(6):791-799.
6. Moller M, Movin T, Granhed H, et al. Acute rupture of tendon Achillis. A prospective randomised study of comparison between surgical and nonsurgical treatment. J Bone Joint Surg Br 2001;83(6):843–848.
7. Speck M, Klaue K. Early full weightbearing and functional treatment after surgical repair of acute achilles tendon rupture. Am J Sports Med 1998;26(6):789–793.
8. Cetti R, Henriksen LO, Jacobsen KS. A new treatment of ruptured Achilles tendons. A prospective randomized study. Clin Orthop Relat Res 1994;(308):155–165.
9. Wong J, Barrass V, Maffulli N. Quantitative review of operative and nonoperative management of Achilles tendon ruptures. Am J Sports Med 2002;30(4):565-575.
10. Nistor L. Surgical and non-surgical treatment of Achilles tendon rupture. A prospective randomized study. J Bone Joint Surg Am 1981;63(3):394–399.
11. Wills CA, Washburn S, Caiozzo V, Prietto CA. Achilles tendon rupture. A review of the literature comparing surgical versus nonsurgical treatment. Clin Orthop Relat Res 1986;(207):156–163.
12. Popovic N, Lemaire R. Diagnosis and treatment of acute ruptures of the Achilles tendon. Current concepts review. Acta Orthop Belg 1999;65(4):458–471.
13. Nyyssönen, Lüthje P, Kröger H. The increasing incidence and difference in sex distribution of Achilles tendon rupture in Finland in 1987-1999. Scand J Surg 2008;97(3):272-275.
14. Suchak AA, Bostick G, Reid D, et al. The incidence of Achilles tendon ruptures in Edmonton, Canada. Foot Ankle Int 2005;26(11):932-936.
15. Maffulli N, Waterston SW, Squair J, et al. Changing incidence of Achilles tendon rupture in Scotland: a 15-year study. Clin J Sport Med 1999;9(3):157-160.
16. Inglis AE, Scott WN, Sculco TP, Patterson AH. Ruptures of the tendo achillis. An objective assessment of surgical and non-surgical treatment. J Bone and Joint Surg Am 1976;58(7):990-993.
17. Schroeder D, Lehmann M, Steinbrueck K. Treatment of acute achilles tendon ruptures: open vs. percutaneous repair vs. conservative treatment. A prospective randomized study. Orthop Trans 1997;21:1228.
18. McComis GP, Nawoczenski DA, DeHaven KE. Functional bracing for rupture of the Achilles tendon. Clinical results and analysis of ground-reaction forces and temporal data. J Bone Joint Surg Am 1997;79(12):1799-1808.
19. Weber M, Niemann M, Lanz R, Muller T. Nonoperative treatment of acute rupture of the Achilles tendon: results of a new protocol and comparison with operative treatment. Am J Sports Med 2003;31(5):685-691.
20. Hufner TM, Brandes DB, Thermann H, et al. Long-term results after functional nonoperative treatment of Achilles tendon rupture. Foot Ankle Int 2006;27(3):167-171.
21. Sekiya JK, Evensen KE, Jebson PJ, Kuhn JE. The effect of knee and ankle position on displacement of Achilles tendon ruptures in a cadaveric model. Implications for nonoperative management. Am J Sports Med 1999;27(5):632-635.
22. Orishimo KF, Burstein G, Mullaney MJ, et al. Effect of knee flexion angle on Achilles tendon force and ankle joint plantarflexion moment during passive dorsiflexion. J Foot Ankle Surg 2008;47(1):34-39.