 By P.A. Lazzarini, D.G. Armstrong, R.T. Crews, C. Gooday, G. Jarl, K. Kirketerp-Moller, V. Viswanathan, and S.A. Bus
By P.A. Lazzarini, D.G. Armstrong, R.T. Crews, C. Gooday, G. Jarl, K. Kirketerp-Moller, V. Viswanathan, and S.A. Bus
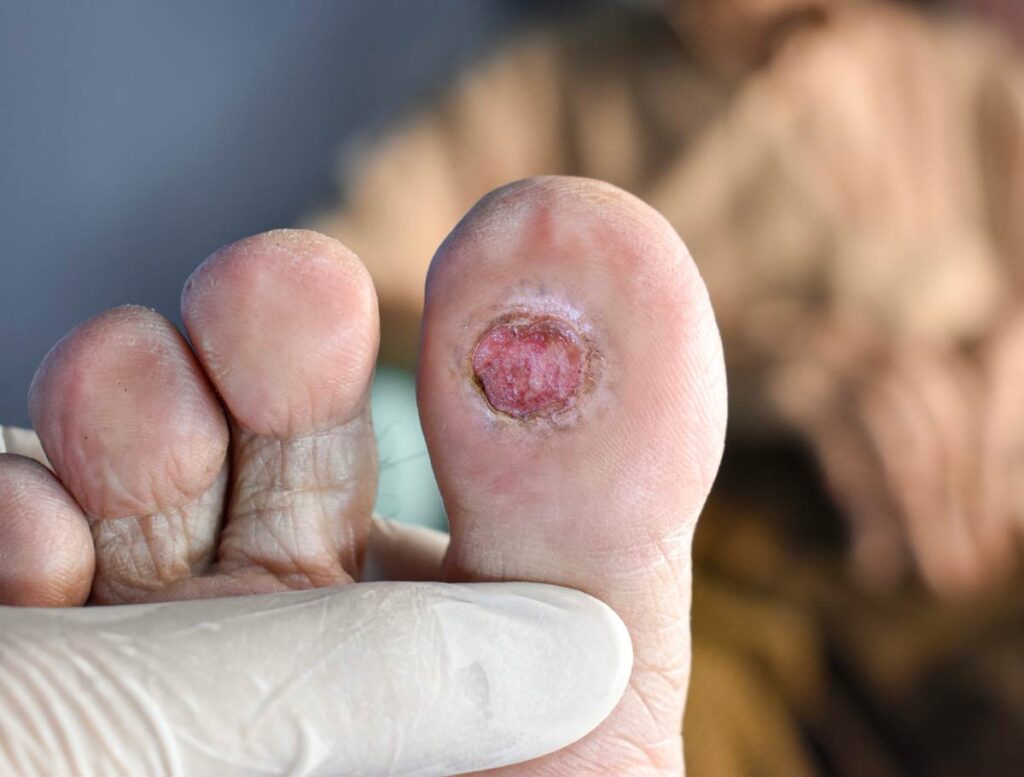
Offloading treatment is crucial to heal diabetes-related foot ulcers (DFU). This systematic review aimed to assess the effectiveness of offloading interventions for people with DFU.
Methods: These authors searched PubMed, EMBASE, Cochrane databases, and trials registries for all studies relating to offloading interventions in people with DFU to address 14 clinical question comparisons. Outcomes included ulcers healed, plantar pressure, weight-bearing activity, adherence, new lesions, falls, infections, amputations, quality of life, costs, cost-effectiveness, balance, and sustained healing. Included controlled studies were independently assessed for risk of bias and had key data extracted. Meta-analyses were performed when outcome data from studies could be pooled. Evidence statements were developed using the GRADE approach when outcome data existed.
Results: From 19,923 studies screened, 194 eligible studies were identified (47 controlled, 147 non-controlled), 35 meta-analyses performed, and 128 evidence statements developed. We found:
- Non-removable offloading devices likely increase ulcers healed compared to removable offloading devices (risk ratio [RR] 1.24, 95% CI 1.09–1.41; N = 14, n = 1083), and may increase adherence, cost-effectiveness, and decrease infections, but may increase new lesions.
- Removable knee-high offloading devices may make little difference to ulcers healed compared to removable ankle-high offloading devices (RR 1.00, 0.86–1.16; N = 6, n = 439), but may decrease plantar pressure and adherence.
- Any offloading device may increase ulcers healed (RR 1.39, 0.89–2.18; N = 5, n = 235) and cost-effectiveness compared to therapeutic footwear, and may decrease plantar pressure and infections.
- Digital flexor tenotomies with offloading devices likely increase ulcers healed (RR 2.43, decrease plantar pressure and infections, but may increase new transfer lesions.
- Achilles tendon lengthening with offloading devices likely increase ulcers healed (RR 1.10, 0.97–1.27; N = 1, n = 64) and sustained healing compared to devices alone, but likely increase new heel ulcers.
Discussion
Summary of main findings: We systematically reviewed all studies investigating offloading interventions for people with DFU and identified 194 eligible studies (including 47 controlled studies), performed 35 meta-analyses and developed 128 evidence statements. For the critical outcome of ulcers healed, we found with moderate certainty that non-removable knee-high offloading devices are likely to be superior to all other offloading interventions to heal plantar forefoot or midfoot DFU, with low certainty that any offloading devices may be superior to therapeutic footwear, and with no certainty that any other nonsurgical offloading interventions are superior to offloading devices. Whereas in combination with offloading devices, we found with moderate certainty that digital flexor tenotomies and Achilles tendon lengthening are likely to be superior to offloading devices alone to heal plantar lesser digit and metatarsal head ulcers, respectively, and with low certainty that metatarsal head resections and joint arthroplasties may be superior to heal other plantar metatarsal head ulcers and hallux ulcers.
Comparison with other reviews: Over the last decade there have been over 20 systematic reviews on different offloading interventions in people with DFU. Therefore, we limit our comparisons of findings in our new review to those of our previous review of all offloading interventions, and all other reviews performing meta-analyses on different offloading interventions.
Compared to our previous review, our new review has made many methodological improvements. These include investigating additional comparisons and outcomes, identifying additional included studies, performing meta-analyses, more rigorously assessing effect sizes and certainty of evidence, and using Summary of Findings (SoF) tables in line with the GRADE approach. These improvements resulted in our new review including multiple meta-analyses (35 vs. 0), SoF tables (20 vs. 0), and many more evidence statements (128 vs. 47) in line with GRADE and Cochrane standards, than our previous review. Thus, the findings in this new review should supersede those of our previous review.
Four other reviews have performed meta-analyses on nonremovable offloading devices. Those authors also found that non-removable offloading devices likely heal more ulcers than removable offloading devices (Others: RR 1.15–1.43 vs. Our review: RR 1.24). Further, like us, the only review to also conduct Certainty of Evidence (CoE) assessments also assessed the supporting evidence to be of moderate certainty for this critical ulcers healed outcome, and only downgraded for serious inconsistency based on moderate heterogeneity.
Otherwise, only one review pooled any other of our important outcomes for offloading devices, and also found non-removable devices may develop more new lesions (they only investigated skin maceration) than removable devices (Other: RR 1.38 vs. Our: RR 1.77). Thus, all reviews to date support the superiority of non-removable knee-high offloading devices over removable offloading devices to heal plantar forefoot or midfoot DFU but suggest non-removable devices may also result in the development of more new lesions than removable devices.
Similarly, two other reviews also found total contact casts (TCCs) likely make little-to-no difference to ulcers healed compared to non-removable walkers (Others: RR 1.02–1.06 vs. Our: RR 1.05). However, the only review to also assess CoE, assessed the supporting evidence to be of low certainty due to very serious imprecision, whereas we assessed it to be moderate certainty due to serious imprecision. The difference in assessments was likely due to our review including additional participants from new trials in our meta-analysis, hence improving the precision of the effect. Thus, all reviews suggest non-removable walkers are equally as effective as TCCs to heal plantar forefoot or midfoot DFU.
Only one other review performed a meta-analysis comparing different removable offloading devices. Unlike us, they found removable knee-high offloading devices may heal less ulcers compared to removable ankle-high devices (they called these devices therapeutic footwear), whereas we found little-to-no difference (Other: RR 0.75 vs. Our: RR 1.00). Further, they assessed the CoE as very low certainty due to serious indirectness based on studies using different devices and very serious imprecision. However, we assessed as low certainty also due to serious indirectness, but only serious imprecision. Again, the difference in assessments for effects and certainty are likely due to our review including many more additional participants from new trials and hence improving the precision of the effect. Thus, these latest findings suggest different removable offloading device heights may have a similar effect on healing plantar forefoot or midfoot DFUs.
Two other reviews also found offloading devices likely heal more ulcers than therapeutic footwear (Others: RR 1.62–1.68 vs. Our: RR 1.39). However, the only review to also assess the CoE, assessed the certainty as moderate due to serious indirectness, whereas we assessed the certainty as low due to very serious inconsistency based on high statistical heterogeneity. However, we noted in our sensitivity analysis a much greater effect in favor of non-removable offloading devices over therapeutic footwear (RR 1.98). Thus, all reviews suggest any offloading devices are more effective than any therapeutic footwear to heal plantar forefoot or midfoot DFU.
For other non-surgical offloading interventions, only one review pooled findings, and also found felted foam with removable devices may decrease plantar pressure more than a device alone (Other: MD 107 kPa lower vs. Our: MD 98 kPa lower). Further, they assessed the CoE as moderate certainty due to serious imprecision, whereas we assessed CoE as very low certainty as these findings were based on non-controlled studies only and had serious indirectness. We also noted in sensitivity analyses that these effects reduced after 3–7 days of application (MD 70 kPa lower). Thus, these reviews suggest felted foam with devices may reduce plantar pressure more than devices alone.
For surgical offloading interventions, one review also found Achilles tendon lengthening with non-removable devices likely healed slightly more ulcers than devices alone (Other: RR 1.06 vs. Our: RR 1.10), and increased sustained healing (note they analyzed ulcer recurrence, the reverse outcome to sustained healing) (Other: RR 0.45 vs. Our: RR 3.41), but they did not assess CoE. Otherwise, two other reviews that reported they performed meta-analyses, actually reported pooled non-weighted findings, which are challenging to compare. However, they also found Achilles tendon lengthening with devices likely heal slightly more ulcers than devices alone, metatarsal head resections with devices may heal more ulcers than devices alone, and joint arthroplasties with devices may also heal slightly more ulcers than devices alone. Thus, all reviews suggest that some surgical offloading interventions in combination with offloading devices may heal more ulcers and keep them healed compared to offloading devices alone for some specific plantar DFU locations.
Limitations and strengths: First, our comprehensive systematic search strategy should mean we identified the vast majority of eligible studies by using clearly defined clinical (PIC) question comparisons, broad search terms, validated search strategies, and independent experts to screen and assess all studies. Yet, there is still a possibility we may have missed some eligible studies, as we did not hand search references, did not update our search since April 2022, and our previous reviews did not include some additional outcomes included in this review. To minimize missing eligible studies, we hand searched references of prior reviews, searched clinical trials registries, included all eligible trials nearing completion, and extracted data on all additional outcomes from included papers in our previous reviews.
Second, our systematic approach to our qualitative assessments should mean we minimized missing any important evidence, by prioritizing the most important clinical question comparisons and outcomes with external experts and persons with lived experience of DFU, defining all populations, interventions, comparators and outcomes using international standards, systematically assessing study designs, risk of bias, levels of evidence and extracting data from all included trials. We note though we did not use latest Cochrane risk of bias tools, but instead used previous Cochrane tools and a specific IWGDF tool for DFU studies to be consistent with our previous reviews.
Third, this review is one of the first in the DFU field to robustly adhere to best practice GRADE methodological approaches, by also using recommended (meta-)analyses, consistent reporting of effect sizes (RR or MD), GRADE evidence tables to assess CoE, and GRADEPro online applications to develop controlled language evidence statements, and to summarize all findings into SoF tables for each comparison. However, we note we used total risk of bias scores from previous Cochrane tools rather than risk of bias items from latest Cochrane tools to inform our CoE ratings and started our CoE assessments for level 2 studies at high instead of low as used in other reviews. We also occasionally pooled data from different controlled study designs, plus reported high I2-statistic values. To address all this though, we performed multiple sensitivity analyses and erred on the side of downgrading our CoE assessments for risk of bias and inconsistency and we note all evidence statements supported only by level 2 studies have been downgraded to (very) low CoE. Thus, we are confident this is the most comprehensive, robust, and clinically valuable offloading systematic review published to date.
Implications for Practice
First, the largest implication for practice from this systematic review is that some offloading interventions are likely much more effective in practice than others to heal DFU. For instance, non-removable offloading devices will likely heal more plantar DFU than nearly all other offloading interventions. Digital flexor tenotomies and Achilles tendon lengthening in combination with offloading devices will also likely heal more plantar lessor digit DFU and some plantar metatarsal head DFU respectively, than offloading devices alone. Any offloading device will probably heal more plantar DFU than therapeutic footwear or any other non-surgical offloading intervention. Finally, metatarsal head resections and joint arthroplasties with offloading devices will also probably heal more plantar metatarsal head DFU and plantar hallux DFU respectively, than devices alone.
Second, different types of the same offloading device category may make little difference to healing but may result in differences to other important outcomes. For instance, it seems different types of non-removable devices probably make little difference to healing plantar DFU, but non-removable walkers will probably decrease plantar pressure, new lesions and falls, and improve patient satisfaction and cost-effectiveness more than TCCs. Similarly, different types of removable devices probably make little difference to healing ulcers, but knee-high devices will probably yield a greater decrease in plantar pressure, activity, and new lesions and be more cost-effective, while ankle-high devices may decrease falls and initial costs, and increase balance, adherence and satisfaction.
Third, the effect an offloading intervention has on important surrogate outcomes, such as plantar pressure, weight-bearing activity, and adherence, seem to combine to produce their effect on healing. For example, removable knee-high devices seem to have the benefit of reducing more plantar pressure and activity than removable ankle-high devices, but at the expense of increasing non-adherence, and in turn, these outcomes seem to counterbalance to produce similar effects on healing. This also suggests that if adherence to knee-high devices could be improved to similar levels found for ankle-high devices, then knee-high devices would probably be superior for healing due to the additional benefits on plantar pressure and activity, but this hypothesis needs further testing.
Fourth, it seems the greater the benefit an offloading intervention has on healing, the greater the benefit it will also have on other important outcomes, such as decreasing the likelihood of infections and amputations, and potentially increasing sustained healing. However, these greater benefits also seem to come with greater risks of some harm for other important outcomes, such as increasing the likelihood of new lesions and falls and decreasing patient satisfaction. Thus, it is important that a clinician and person with a DFU understand and carefully balance the potential benefits on healing, infections and amputations, with the potential harms on new lesions, falls, and satisfaction outcomes, when selecting the best offloading intervention(s) for the person’s situation.
Lastly, all these interventions still only have low-to-moderate certainty of supporting evidence for their beneficial effects on healing ulcers, and typically (very) low certainty for their beneficial or harmful effects on other outcomes. Therefore, we recommend it is important that clinicians help people with DFU in their care to consider the beneficial and harmful effects of different offloading interventions, and the certainty of evidence for these effects, when selecting offloading interventions that are best for each person and their values. For example, the evidence suggests the benefits of choosing a non-removable device over a removable device are that they will likely heal the person’s DFU faster, may reduce their chance of developing infections and having amputations, and be more cost-effective over their treatment duration. However, the evidence also suggests the harms of choosing a non-removable over a removable device are that they may also increase the chance of developing a new lesion (abrasion, blister, callus, ulcer, etc.), may cost more initially, and they may be a little less satisfied when using the device.
Therefore, one person with a DFU who values better healing, infection, or amputation outcomes more greatly, may select a non-removable device. Whereas another who values avoidance of new lesions, intervention satisfaction, or initial cost outcomes more greatly, may select a removable device. Thus, we suggest clinicians use the summarized findings in [the original article] along with the updated IWGDF guideline on offloading interventions for people with DFU, to help people with DFU in their care to select the best offloading intervention for the person.
Implications for research: With no high CoE, and very few outcomes with moderate certainty, further trials are needed in most areas of the field, however we specifically recommend several key areas.
First, whilst non-removable devices are most effective on healing as they maximize adherence, they also seem to increase some harms. We also found (with low certainty) that non-removable walkers compared with TCCs may limit these harms, by yielding greater reductions in plantar pressure and new lesions, paired with increased user satisfaction. Thus, more high-quality trials are needed to determine if non-removable walkers may be a superior nonremovable option to traditional TCCs.
Second, while all removable devices are likely inferior to nonremovable devices due to lower adherence, and different removable devices may make little difference to healing compared with each other, they also seem to have different benefits on other outcomes that if harnessed collectively may improve healing. Thus, we recommend more high-quality trials are needed to determine which removable devices are most effective at maximizing the collective benefits on plantar pressure, adherence, and satisfaction, such as existing removable devices, new smart devices, or combination interventions of different devices with psychological interventions.
Third, while a new high-quality surgical trial showed digital flexor tenotomies likely improve healing of lessor digit ulcers, more high-quality trials in other surgical offloading procedures are still needed to improve certainty, such as for Achilles tendon lengthening, metatarsal head resections, metatarsal osteotomies, and joint arthroplasties. Further trials are also required to determine which offloading devices are best combined with these surgical interventions or even if offloading devices are needed.
Fourth, although some new controlled studies suggest the offloading interventions most effective for less complex plantar forefoot DFU may also be those most effective for more complex DFU, more high-quality trials are needed to better inform clinicians about effective offloading treatments for infected, ischaemic, rearfoot, and particularly non-plantar ulcers. Further, this review found some evidence that different devices may have different effects on different forefoot locations, and thus, future trials should report outcomes on specific forefoot DFU locations, such as the hallux.
Fifth, whilst some new controlled studies came from low-to-middle income countries or those with hotter climates, there is still a need for more trials in those settings, including developing and trialing lighter, cooler, and less expensive devices, without losing the key mechanical offloading features of existing devices.
Sixth, although for the first time we were able to pool various important outcomes, the certainty of evidence for these outcomes was nearly always (very) low. Thus, we continue to recommend that future trials report these other important outcomes, consistent with international standards, so as to continue to be able to pool the effects for these important outcomes in future.
Seventh, unlike peak plantar pressures thresholds for DFU prevention, we note there are still no objective thresholds for other outcomes that indicate DFU healing. Thus, we recommend studies explore if such thresholds for plantar pressure, activity, adherence, or a combination plantar tissue stress measure may inform how much offloading is most effective for healing and in turn guide the development of future offloading interventions tested against such thresholds.
Last, in addition to the above recommended quantitative studies, we recommend more qualitative research should explore patients’ perceptions as to the importance of outcomes, benefits and harms of different offloading interventions to truly understand the perspectives of people with DFU.
Conclusions
This new systematic review shows there is a moderate certainty of supporting evidence for some offloading interventions to heal DFU, but most offloading interventions used in practice have low or very low CoE, and some others have no supporting evidence at all. The offloading interventions with moderate certainty to be most effective to heal plantar forefoot or midfoot DFU are non-removable knee-high offloading devices (either non-removable walkers or TCCs) and digital flexor tenotomies and Achilles tendon lengthening in combination with offloading devices for specific plantar forefoot DFU locations. Otherwise, all removable offloading devices have low certainty that they are more effective to heal plantar forefoot or midfoot DFU than any other non-surgical offloading intervention, such as therapeutic footwear, felted foam, or wheelchairs. Although the evidence for offloading interventions to heal non-plantar, rearfoot, ischemic, or infected DFU is very limited, the evidence suggests the most effective interventions for plantar forefoot or midfoot DFU are also probably those most effective for these more complex DFU. However, high-quality trials of nearly all interventions are still required before any offloading interventions have a high certainty of supporting evidence for their effects on the critical outcome of healing DFU, and the other important outcomes for people with DFU, such as new lesions, falls, infections, amputations, quality of life, and costs.
P.A. Lazzarini is a conjoint Principal Research Fellow at Metro North Hospital & Health Service and Queensland University of Technology in Brisbane, Australia. He is a podiatrist by background and founded Australia’s first diabetes foot disease research program.
D.G. Armstrong is a Professor of surgery and Director of the Southwestern Academic Limb Salvage Alliance at the Keck School of Medicine at the University of Southern California (USC) and Director of the USC Center to Stream Healthcare in Place in Los Angeles, Califiornia.
R.T. Crews is Associate Professor of Podiatric Medicine & Surgery at the Dr. William M. School College of Podiatric Medicine in North Chicago, Illinois.
C. Gooday is the Principal Podiatrist on the Diabetes Podiatry Team at the Elsie Bertram Diabetes Centre at Norfolk and Norwich University Hospitals in Norwich, United Kingdom.
G. Jarl is Associate Professor of Medicine in the Department of Prosthetics and Orthotics and the University Health Care Research Center, Faculty of Medicine and Health at Örebro University in Örebro, Sweden.
K. Kirketerp-Moller is an orthopaedic surgeon and Head of the Copenhagen Wound Healing Center at Bispebjerg University Hospital and serves as a consultant at Steno Diabetes Center, both in Copenhagen, Denmark.
V. Viswanathan is a diabetologist with MV Hospital for Diabetes in Chennai, India.
Professor Dr. Sicco Bus is a human movement scientist and a professor of clinical biomechanics and principle investigator at Amsterdam University Medical Centers in the Netherlands.
This article has been excerpted from Lazzarini PA, Armstrong DG, Crews RT, et al. Effectiveness of offloading interventions for people with diabetes-related foot ulcers: a systematic review and meta-analysis. Diabetes Metab Res Rev. 2024;e3650. https://doi.org/10.1002/dmrr.3650. Editing has occurred, including the renumbering or removal of tables, and references have been removed for brevity. Use is per CC Attribution 4.0 International License.








I am an orthotists with 35yrs experience. These articles to me prove one thing. that these people are good at getting funding for research papers. either you know what you’re doing or you don’t and sad to say probably 80% of the medical field does not know how to help people with the problems of this article.