The relationship between calf-pump insufficiency and ulceration has long been established.1 The accompanying venous hypertension is associated with histologic and hemodynamic alterations in capillary and lymphatic microcirculation that result in pathophysiologic changes in the tissues.1 Capillary leak, fibrin deposition, erythrocyte and leukocyte sequestration, thrombocytosis, and inflammation combine to produce impaired oxygenation of the skin and deep tissues.2 Over time, non-treated venous hypertension will produce the clinical signs of edema, skin hyperpigmentation, subcutaneous tissue fibrosis, and will result in venous leg ulcer (VLU) formation.2
Venous leg ulcers are a common disabling condition that are difficult to treat and often recur.1 These wounds can take months and even years to heal. The hallmark of VLU treatment is the use of high-level compression bandages or garments to provide support to the lower extremity venous system.1 Primary dressings are utilized to manage exudate, prevent infection, and optimize the wound environment. Studies have shown that while compression therapy increases healing in VLUs, a proportion of these wounds remain unhealed.1 Therefore additional therapies are needed in patients suffering from recalcitrant VLUs.
Current literature suggests that pentoxifylline can improve outcomes in patients suffering from chronic VLUs.3 Pentoxifylline is a xanthine derivative known to influence microcirculatory blood flow and oxygenation of ischemic tissues.4 This medication is often used in the treatment of peripheral vascular disease.5 Pentoxifylline is often thought of as a vasodilator, but the drug’s MOA is to increase red and white cell filterability, and decrease whole blood viscosity, platelet aggregation and fibrinogen levels.6 Pentoxifylline has been shown to have utility in supporting wound healing of chronic venous ulcers with or without compression therapy.7
Herein, we will describe a case report of a chronic VLU recalcitrant to multiple wound therapies that demonstrated a positive response to the addition of pentoxifylline therapy. Patient is an 84-year-old Caucasian female with a history of a chronic venous leg ulcer for 5 years on the left lower extremity. Other past medical history includes peripheral vascular disease (PVD), venous stasis dermatitis, varicose veins, hyperthyroidism, coronary artery disease (CAD), edema, scoliosis, mitral valve prolapse, hypertension, degenerative joint disease (DJD), and Raynaud’s syndrome.
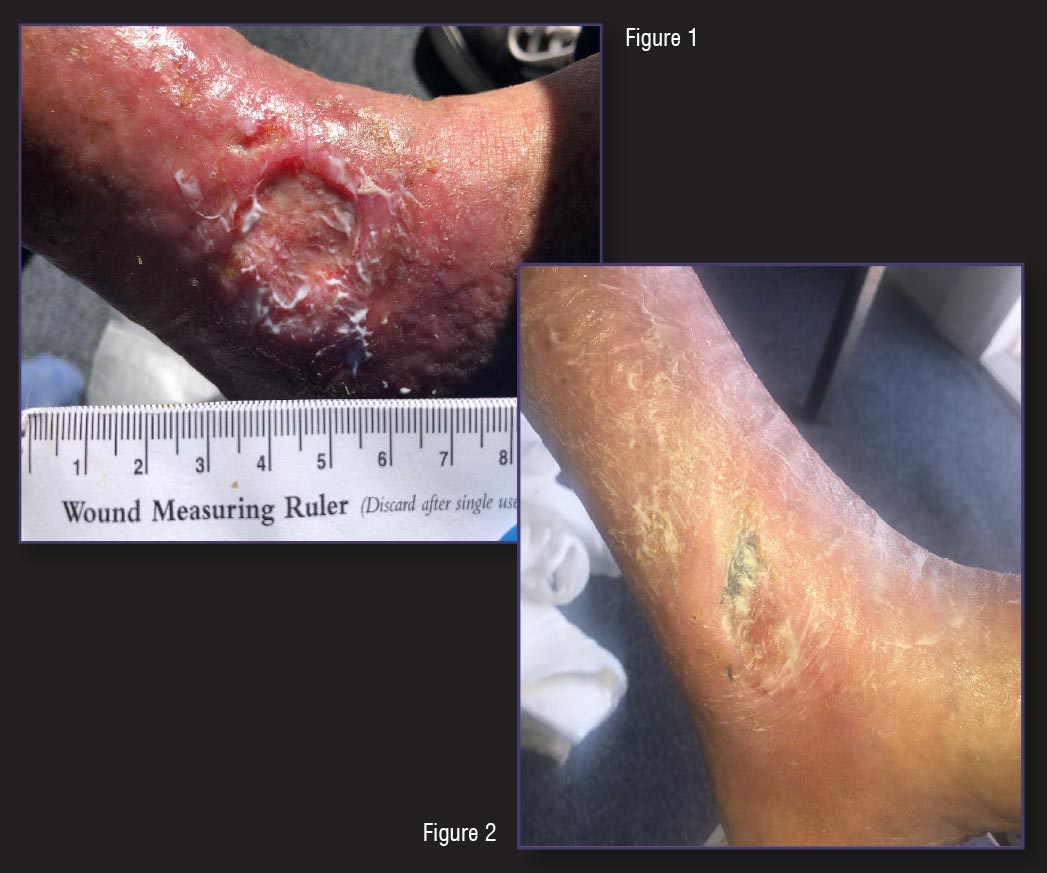
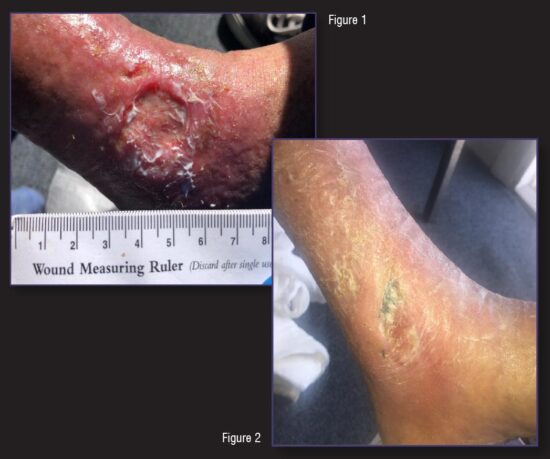
Upon intake, the wound was noted to be full thickness with a slough-covered base and irregular borders illustrating epibole. There was moderate serosanguineous drainage noted and wound measurements were 2.6cm x 3.0cm x 0.2cm. Non-pitting edema was noted in the lower leg (Figure 1). Patient was referred to vascular surgery and had a venous ablation and phlebectomy performed. But the VLU continued to worsen. Additionally, multiple wound care treatments were used throughout the course of therapy which included the use of silver dressings, collagen, alginates, cortisone cream, oral antibiotics, and Manuka honey combined with compression bandages. During this time the patient’s wound failed to progress. Patient was referred to a local dermatologist for evaluation and was told she would have to learn to “live with it.” Due to the diligence of our clinician, an additional referral to another dermatologist was obtained for a second opinion. As a result, the patient was started on pentoxifylline and within a month the wound measurements and periwound tissue quality was markedly improved (Figure 2).
Conclusion
This case report illustrated the utility of pentoxifylline as an adjunct treatment to compression bandaging and local wound care in the treatment of a recalcitrant venous ulcer. Most adverse effects associated with this medication are gastrointestinal disturbances.8 Pentoxifylline should not be used in nursing mothers or in patients with renal failure. A Cochrane review of VLU trials investigating the use of pentoxifylline as an adjunctive therapy to support wound healing suggested 400 mg tablet taken 3 times per day did increase the chance of VLU resolution.7 It has been theorized that the fibrolytic action of pentoxifylline is the mechanism of action for the drug’s utility in VLU healing, although further investigation is needed to determine the true mechanisms by which pentoxifylline works on venous ulcers.
Acknowledgement: Case was submitted by Scott Casinger, NP.
Windy Cole, DPM, CWSP, is an adjunct professor and Director of Wound Care Research at Kent State University College of Podiatric Medicine. Dr Cole also serves as the National Director of Professional Development and Clinical Education for Woundtech. She is board certified by the American Board of Foot and Ankle Surgery and the American Board of Wound Management. She is a wound care advocate on the forefront of wound research and was the 2020 World Union of Wound Healing Silver Medal Award recipient for her work in Technology-driven Research. And she is a member of the LER Editorial Advisory Board.
- Tang JC, Marston WA, Kirsner RS. Venous ulcer treatment guidelines. Wound Repair Regen. 2012:20(5):619-637.
- Chi YW, Raffetto JD. Venous leg ulceration pathophysiology and evidence-based treatment. Vasc Med. 2015;20(2):168-181.
- Zito PM, Murgia RD III. Pentoxifylline (Trental) in venous insufficiency and venous leg ulcers. J Derm Nurses Assoc. 2018;10 (6):294-296.
- Stellin GP, Waxman K. Current and potential therapeutic effects of pentoxifylline. Compr Ther. 1989;15(5):11-13.
- Puchmayer V. Modern therapeutic trends in the conservative treatment of ischemic disease of lower extremities. [Czech] Vnitr Lek. 1995;41(3):204-206.
- Colgan MP. Oxpentifylline treatment of venous leg ulcers (Letter). BMJ 1990;300(6730):972-975.
- Belacro G, Cesarone MR, Nicolaides AN, et al. Treatment of venous ulcers with pentoxifylline: a 6-month, randomized double-blind, placebo-controlled trial. Angiology. 2002;53(Suppl1):S45-47.
- Jull AB, Arroll B, Parag V, Waters J. Pentoxifylline for treating venous leg ulcers. Cochrane Database Syst Rev. 2012;12: Art. No.: CD001733. DOI: 10.1002/14651858.CD001733.pub3







I’ve been exploring vein reduction options and didn’t realize how many non-invasive treatments are available now. Having a guide like this really clears up some of the confusion around where to start
Where can I get the Drugs