By Paul J. Betschart, DPM
Many foot and ankle specialists focus on the musculoskeletal conditions of patients. Skin and nail conditions of the feet, however, are some of the most common complaints that patients have. This 2-part series will describe the most common conditions patients present with to my office and provide some effective treatment options.
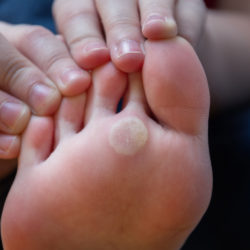 Corns and Callouses
Corns and Callouses
Corns and callouses are likely the number one skin condition seen in lower extremity practice. The profession of Podiatry has at its roots providing nonsurgical care for this annoying and often painful condition. Corns and callouses are discrete keratotic lesions, meaning they are composed of compressed layers of keratin, the outer layer of skin. This layer has no living cells and no nerve endings, thus the lack of pain encountered when removed sharply. Pain from these lesions is typically due to the pressure from weigh bearing or shoe gear that presses the lesions into the underlying soft tissue which does have nerve endings. These lesions typically form in areas of pressure or friction as the body attempts to protect itself.
Corns and callouses are basically the same condition, just different sizes, which is why the terms are often used interchangeably. The term “corn” usually refers to a smaller, more concentrated lesion, whereas the term “callous” is often used to refer to broader, larger lesions. Common areas of formation of these lesions include the tops of the toes, the tips of the toes, between the toes, the bottom of the foot under the metatarsals, and the edge of the heel. They can arise anywhere there is an underlying boney prominence if it is rubbing in the shoe or on the bottom of the foot. Diagnosis is made through visual inspection and is confirmed with reduction.
Treatment of corns and callouses is initiated with reduction of their thickness to reduce pressure on underlying structures. This is commonly performed by podiatrists using a sharp surgical blade or a grinding tool. Chemical reduction with urea or salicylic acid compounds is another option, though slower to achieve relief. Padding of the areas to reduce shoe or weight-bearing pressure is also helpful at symptom control. Identifying and managing underlying structural and/or biomechanical abnormalities is essential in providing long-term relief for these lesions. This often involves shoe gear modification, foot orthoses or bracing, and potentially, surgical procedures to correct deformities or reduce boney prominences. Periodic reduction of recurrent lesions is commonly needed if underlying forces are not adequately controlled. Typical intervals are 1–3 months apart.
 Verruca
Verruca
Verrucae, also known as warts, are commonly confused with corns or callouses. At first glance, they can look similar due to the increased keratotic layer formed over and around the wart due to pressure from weight bearing. Upon reduction of the keratin layer, one will note that the wart extends to the deeper levels of the skin. Interruption of skin lines is a common diagnostic sign as are the small capillaries that feed the wart tissue, which show as pin-point bleeding on reduction beneath the keratotic layer. Smaller verrucae, under 3mm often have not developed much of a capillary bed yet, so can be readily mistaken for a corn, especially if near a boney prominence. Verrucae on the bottom of the foot are called plantar warts, referring to the plantar surface of the foot. Warts on other areas of the foot are called common warts or verruca vulgaris. Diagnosis is usually made through clinical examination. Occasionally, biopsy may be needed for definitive diagnosis.
Verrucae have been treated in a number of ways throughout history. In modern medicine, treatments include topical debriding agents such as salicylic acid, blistering agents, drying agents, immunotherapy, and surgical removal. There are no oral antiviral medications nor vaccines that have been developed for this form of the human papilloma virus. An off-label use of a common anti-acid medication, cimetidine can be a helpful adjunctive therapy, especially with children. It is thought that this medication somehow modulates the immune response to the virus. I have had success with this treatment, even as monotherapy in children as young as 3 years. Cimetidine can be obtained in a liquid elixir, which is helpful when treating younger patients.
I have used many combinations of treatments for verrucae throughout my years of practice. The most effective method that I have found has been the combination of a chemical blistering agent followed by laser photo dynamic therapy. This technique has proved highly effective, even with large and/or multiple lesions. After debridement of the keratotic layer, the blistering agent Cantharone® is applied to the lesion and covered for 24 hours. The area can then be washed and re-dressed if needed for protection. One week later, the blistered area is debrided and a solution of methylene blue is applied to the area and allowed to dry. The area is then treated with laser energy at low levels for 2 minutes in each area. The laser energy interacts with the dye molecules in the target tissue to cause programmed cell death, eliminating any remaining abnormal tissue. Large or multiple lesions may require additional treatments. Recurrence is rare after resolution following this technique. Verrucae that fail to respond to concerted efforts should be considered for biopsy to rule out a malignancy.
CAUTION! Verrucae are contagious so care should be taken to avoid spread to others. Moist environments such as bathtubs, showers, and pool decks are common areas of spread. Sanitization of these surfaces with a dilute bleach solution can be effective. Avoid sharing footwear with others and allow shoes to dry fully between wearings.
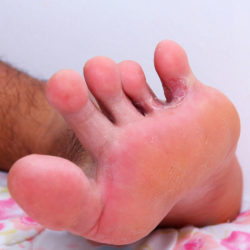 Tinea Pedis
Tinea Pedis
Tinea pedis, commonly called athlete’s foot, is a fungal infection of the outer skin layers of the foot. The most common type of fungus that causes tinea pedis is the class called dermatophytes, meaning skin lovers. Two common areas of occurrence of tinea pedis are between the toes and on the sole of the feet. Fungal infections between the toes tend to be moist, whereas fungal infections on the soles tend to be dry. Typically, peeling of the outer skin layers is seen in patchy areas along with small, dry blisters. The most common symptom is itching which can lead to skin abrasions from scratching. These abrasions can become secondarily infected by bacteria, causing abscess or cellulitis. Diagnosis is usually made by clinical evaluation. Laboratory evaluation of skin scrapings may also be performed to help identify unusual organisms. This is especially helpful in treatment-resistant cases. Treatment with topical anti-fungal preparations for 2 – 4 weeks is usually curative. Oral anti-fungal medications may be needed for 1 – 2 weeks in severe infections and those not responding to topical treatments. Recurrence of tinea pedis is common, especially in susceptible individuals. Prevention of recurrence revolves around moisture management and reduction of exposure to fungal organisms. Fungi thrive in dark, moist environments like the inside of shoes. Footwear must dry thoroughly between wearings. Feet should be dried well after washing, especially between the toes. An anti-fungal powder or spray can be applied to the feet regularly to absorb moisture and reduce fungal organisms. If using moisturizers on the feet, avoid applying between the toes as these areas can get too moist increasing the risk of fungal infection. People with recurrent fungal infections should consider sanitizing all footwear regularly, using a commercial spray or ultraviolet sterilizer.
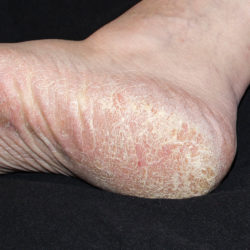 Hyperkeratosis
Hyperkeratosis
Hyperkeratosis is a group of skin conditions that result in skin that is excessively dry and scaling. The scaling can become very thick, especially around the edges of the foot. The thickened areas can develop cracks that can extend into the deeper skin layers, increasing the potential for bacterial infection. Mild hyperkeratosis can be treated with a variety of over-the-counter moisturizers applied 1 – 2 times daily. More severe cases may require more potent softening agents, such as urea preparations in concentrations of 40% – 50% applied to the affected areas 2 – 4 times a day. Sharp reduction of heavy scaling by a medical professional can also be helpful at relieving symptoms. Areas with full thickness skin cracks can be treated with topical corticosteroid preparations 2 – 4 times daily for 2 – 4 weeks.
Eczema
 Eczema or dermatitis is another common keratotic skin condition. Dermatitis starts with inflammation in the deeper skin layers and can develop thickening of the outer layers with scaling, peeling, and cracking. Itching is a common complaint. Scratching can contribute to the thickening of the skin. Microscopic examination of skin scrapings and occasionally full thickness skin biopsy may be needed to differentiate dermatitis from tinea pedis.
Eczema or dermatitis is another common keratotic skin condition. Dermatitis starts with inflammation in the deeper skin layers and can develop thickening of the outer layers with scaling, peeling, and cracking. Itching is a common complaint. Scratching can contribute to the thickening of the skin. Microscopic examination of skin scrapings and occasionally full thickness skin biopsy may be needed to differentiate dermatitis from tinea pedis.
There are several potential causes of dermatitis with the most common being exposure to toxins (contact dermatitis), allergic (atopic dermatitis), and hereditary dermatitis. Treatment is made by addressing any underlying causes and using topical corticosteroid preparations of various potencies. Exfoliation of keratotic areas with topical urea preparations and/or sharp debridement can be helpful in improving symptoms. Non-responding cases may require a short course of oral corticosteroids or a biologic agent, such as Dupixent.
Psoriasis
 Psoriasis is an autoimmune skin condition that causes the skin cells to multiply at much faster rates resulting in the formation of red, raised scaly lesions. The feet are not the most common part of the body for psoriasis to present but they are not spared. Lesions of psoriasis are more common on the top of the foot and legs. Plantar surface psoriatic plaques can be painful to walk on. Psoriasis can cause the toenails to become brittle and thickened, appearing similar to fungal toenails. Diagnosis is usually made by clinical picture. Skin biopsy may be needed to confirm diagnosis or differentiate from other skin conditions. Many different treatments have been used for psoriasis over the years. Examples include coal tar, UV light therapy, vitamin A derivatives, corticosteroids, photodynamic therapy, immune suppressive agents, and biologic agents.
Psoriasis is an autoimmune skin condition that causes the skin cells to multiply at much faster rates resulting in the formation of red, raised scaly lesions. The feet are not the most common part of the body for psoriasis to present but they are not spared. Lesions of psoriasis are more common on the top of the foot and legs. Plantar surface psoriatic plaques can be painful to walk on. Psoriasis can cause the toenails to become brittle and thickened, appearing similar to fungal toenails. Diagnosis is usually made by clinical picture. Skin biopsy may be needed to confirm diagnosis or differentiate from other skin conditions. Many different treatments have been used for psoriasis over the years. Examples include coal tar, UV light therapy, vitamin A derivatives, corticosteroids, photodynamic therapy, immune suppressive agents, and biologic agents.
Neoplasia, aka Cancer
Malignant skin tumors are rare in the lower extremity. The majority of abnormal skin growths are benign or noncancerous. The most common benign skin growths are nevi or moles. These dark colored lesions are collections of cells with high levels of the skin pigment melanin. Nevi are typically small and regular in shape and color. Warts can also fall into the category of skin tumors. These are caused by an infection of the skin cells with human papilloma virus. (Detailed discussion of warts is above.)
 Another common skin tumor is the dermal fibroma. These are benign proliferations of fibrous tissue in the dermis, the deepest skin layer. These flesh-colored lesions are usually small and isolated. A common location is in the skin surrounding the nails. A similar-appearing lesion is the neurofibroma. This lesion is composed of neural tissues as well as fibrous tissue. Although benign, the condition neurofibromatosis can result in multiple lesions all over the body. Actinic or solar keratoses are another common skin growth. These small, raised, flesh-colored lesions are thought to be caused by sun exposure.
Another common skin tumor is the dermal fibroma. These are benign proliferations of fibrous tissue in the dermis, the deepest skin layer. These flesh-colored lesions are usually small and isolated. A common location is in the skin surrounding the nails. A similar-appearing lesion is the neurofibroma. This lesion is composed of neural tissues as well as fibrous tissue. Although benign, the condition neurofibromatosis can result in multiple lesions all over the body. Actinic or solar keratoses are another common skin growth. These small, raised, flesh-colored lesions are thought to be caused by sun exposure.
Benign skin tumors tend to be slow growing and do not spread locally or to distant sites. Benign skin growths should be monitored over time to look for changes that could foretell malignant changes. Any suspicious skin lesion or a benign lesion which has changed considerably should be examined microscopically. Biopsy can usually provide an accurate diagnosis of the skin tumor and guide further treatment.
The most common malignant skin tumors that occur in the feet are malignant melanoma and squamous cell carcinoma. Both can be very aggressive and spread locally and to distant sites, including the lungs, liver, and brain. Early suspicion and microscopic evaluation are key to preventing morbidity and mortality from these tumors. Characteristics of melanoma that raise suspicion revolve around the ABCs:
A stands for area. Lesions larger than 6mm are considered suspicious.
B stands for border irregularity. Benign nevi tend to have smooth borders. Irregularity of the edges of a pigmented lesion raises suspicion of malignancy.
C stands for color variation. Benign skin lesions tend to be uniform in color. Variations in color throughout a skin lesion are a suspicious sign.
Squamous cell carcinoma is often difficult to identify clinically. It often presents as a non-healing wound or ulceration on the extremities. Any wound that fails to heal with adequate wound care should be considered suspicious. On rare occasions, chronic wounds, such as diabetic foot ulcers or pressure ulcers can undergo malignant degeneration. As above, stalled wound healing should be considered suspicious for malignant change.
Part 2 of this series, which will appear next month, will focus on common nail conditions.
Paul J. Betschart, DPM, FACFAS, is a podiatrist in private practice in Danbury, Connecticut. A Fellow of the American College of Foot and Ankle Surgeons, his goal is to help his patients achieve optimal health from the ground up.