lerEXPO Highlights
By Tyler Gonzalez MD MBA FAAOS
 Introduction: The Achilles’ Heel of Achilles Pain
Introduction: The Achilles’ Heel of Achilles Pain
For millions of people, chronic heel pain is a relentless and frustrating battle. Conditions like insertional Achilles tendinopathy and Haglund’s deformity make every step a painful reminder of a problem that refuses to go away. For decades, the standard surgical solution has been an open procedure involving a large incision, cutting away the problematic bone spur, debridement and repair of the tendon and a long recovery.
But what if the conventional wisdom was wrong? What if the key to fixing the pain wasn’t removing the spur at all? A minimally invasive procedure, the MIS Zadek osteotomy is gaining traction among leading surgeons for its surprisingly effective and counter-intuitive approach. It challenges the very foundation of how we think about treating heel pain.
As a fellowship-trained board-certified orthopedic surgeon and leading expert in the procedure, Dr. Gonzalez is focusing his research to unravel the biomechanical mysteries behind its success.
1. The Biggest Surprise: You Can Leave the Bone Spur
The most radical concept behind the MIS Zadek procedure is what it doesn’t do. It succeeds by deliberately leaving behind the very tissues—the bone spur and the diseased “crab meat” tendon—that surgeons have spent decades learning to cut out. But do we really need to?
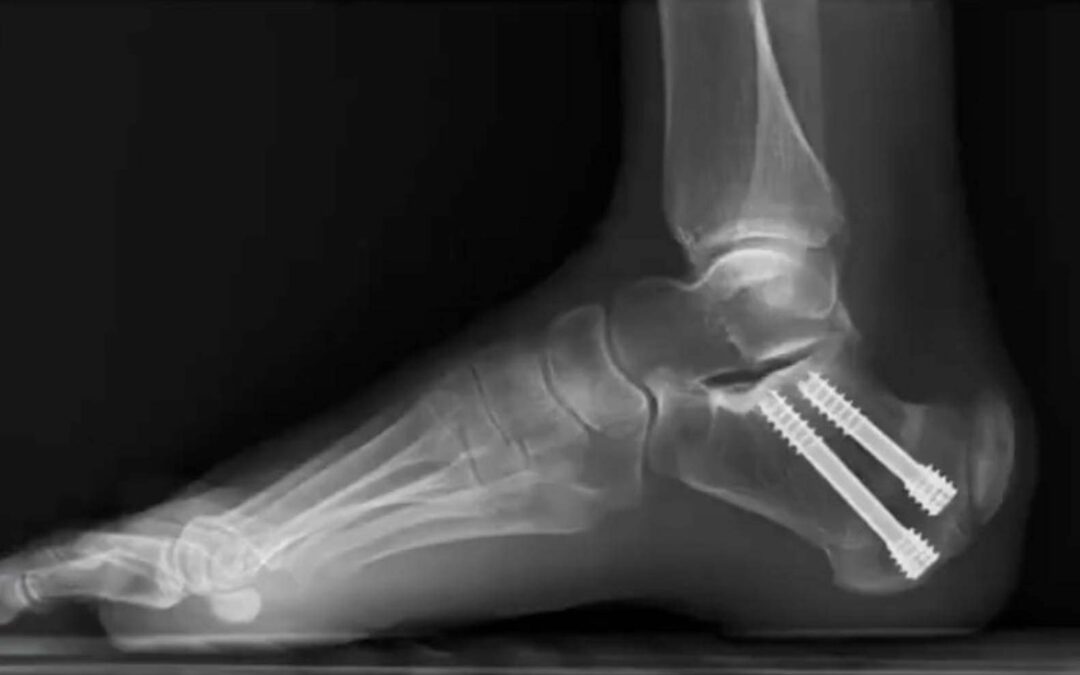
The core premise of the Zadek procedure is to change the biomechanical environment to allow the body to heal itself. By making a small cut in the heel bone and removing a wedge, the surgeon alters the angle by which the Achilles tendon inserts on the calcaneus. This decompresses the entire area, alleviating the tension and strain that caused the inflammation and pain in the first place, while allowing the tendon to heal naturally.
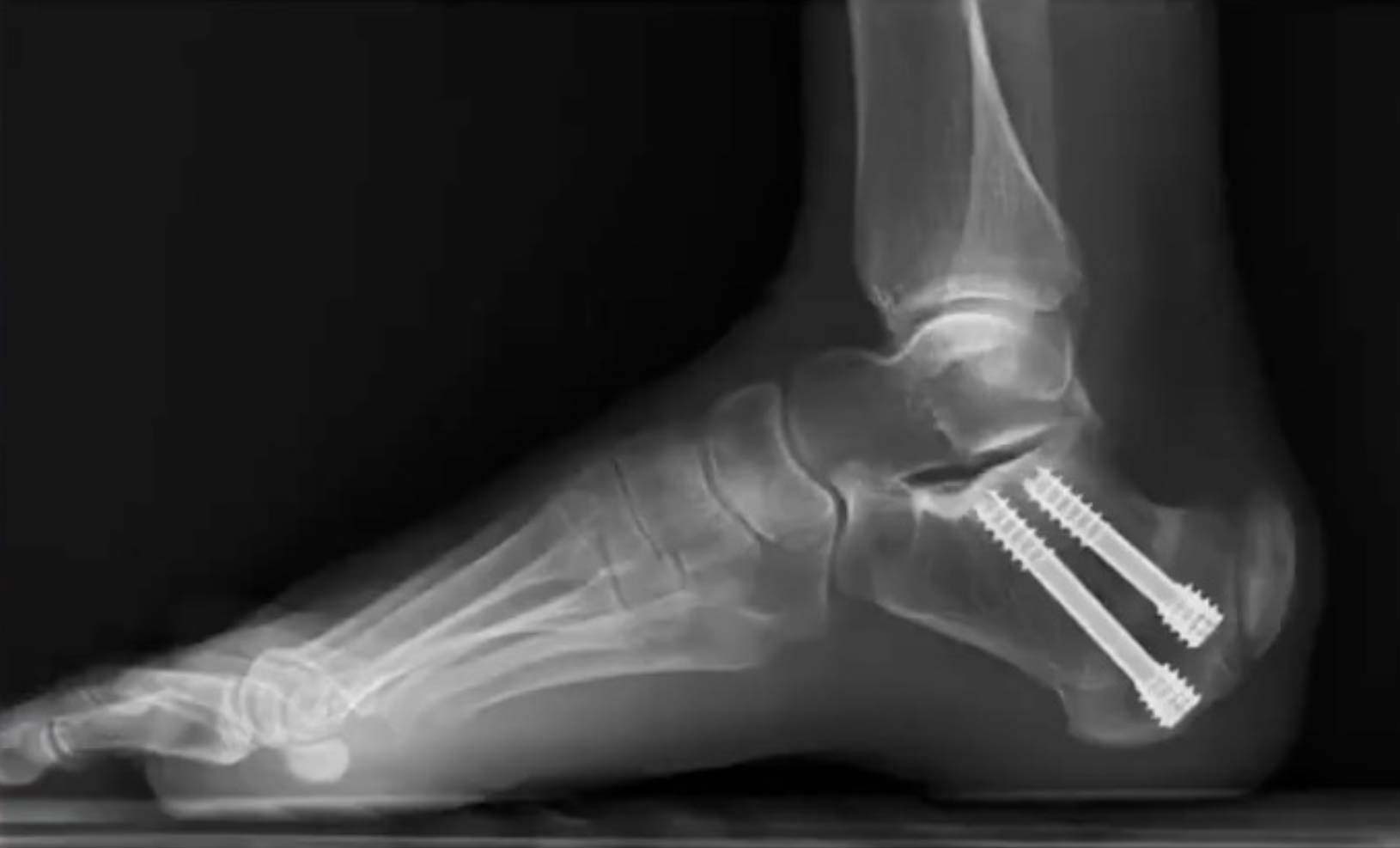 To answer the critical question of whether the spur needs to be removed to provide patients with relief of their posterior heel pain, Dr. Gonzalez’s team studied over 100 patients who underwent the MIS Zadek procedure. That found improvement in functional outcomes in over 94% of patients with IAT–all without ever touching the spur or Achilles tendon itself. To piggyback on these findings, they compared outcomes following the MIS Zadek procedure with the traditional open procedure where the spur is removed and Achilles debrided and repaired. They found that patients in both groups had equivalent functional outcomes.
To answer the critical question of whether the spur needs to be removed to provide patients with relief of their posterior heel pain, Dr. Gonzalez’s team studied over 100 patients who underwent the MIS Zadek procedure. That found improvement in functional outcomes in over 94% of patients with IAT–all without ever touching the spur or Achilles tendon itself. To piggyback on these findings, they compared outcomes following the MIS Zadek procedure with the traditional open procedure where the spur is removed and Achilles debrided and repaired. They found that patients in both groups had equivalent functional outcomes.
Perhaps this anecdote from one of his patients illustrates this point best. A 52-year-old marathon runner with a massive bone spur and debilitating heel pain came to Dr. Gonzalez for a third opinion. Other surgeons had offered her a large open procedure including removal of her spur and a tendon transfer, which she did not want. Instead, Dr. Gonzalez did an MIS Zadek osteotomy Just 7 months after surgery, she was running 7 miles a day, completely pain-free. One year out from surgery she came in first place in her first half marathon since surgery!
“Your spur is not going to go away, but your pain is going to go away. And that’s what they care about, right?”
2. The “Goldilocks” Principle: Wedge Size is Everything
The technical key to the Zadek osteotomy is a dorsal closing wedge osteotomy to change its angle and decompress the Achilles tendon. But how big should that wedge be? It turns out that size is critical.
To determine just how much size matters, Dr. Gonzalez and his colleagues launched a cadaveric study. The data revealed a surprising truth: a small 7.5 mm wedge was not effective in producing any significant change in ankle dorsiflexion following the MIS Zadek osteotomy, while a larger, 15 mm wedge produced a significant gain in dorsiflexion. They were able to describe a direct correlation between the size of the wedge removed, and the functional improvement the Zadek procedure can offer.
During their discussion, Dr. Jeff Dykis offered a perfect analogy for this concept: “Goldilocks and the 3 bears.” This has led researchers to ask what the sweet spot for the wedge size is perhaps not too big, or not too small–but “just right.” It is now generally accepted that a wedge usually 10 mm is to be removed from the calcaneus to allow patients the maximal biomechanical advantage postoperatively, however not smaller than this. Based on current data and extensive clinical experience, the guesstimated sweet spot is somewhere between 10 mm and 12 mm. If < 10 mm is removed, there is likely not enough wedge removed from the calcaneus to allow for adequate decompression on the Achilles which may result in a poor outcomes.
3. A Biomechanical Reset: It Can Make You Stronger, Not Weaker
A common and logical fear among patients and surgeons is that a procedure designed to functionally lengthen the Achilles tendon complex, such as the Zadek, may lead to weakness. After all, if you give the tendon more slack, wouldn’t the patient lose push-off power?
To this, Dr. Gonzalez offered a compelling counterargument rooted in foundational biomechanics. The Zadek procedure is not weakening the muscle; instead, it is “restoring the normal length-tension relationship in the muscle-tendon-bone complex.” In essence, it’s not creating slack but rather returning an overly taut system to its optimal, more efficient state.
To scientifically test this theory, Dr. Gonzalez’s team completed a gait analysis study at the University of South Carolina. The study compared postoperative gait mechanics and push-off strength in patients 1 year following the MIS Zadek procedure compared to traditional open Haglund’s surgery. The findings are remarkable: the data shows that patients who underwent the MIS Zadek procedure do not lose any push-off strength or propulsion. In contrast, patients who had the open procedure have demonstrated some measurable, statistically significant weakness and push off in their operative limb in comparison to their contralateral side. This suggests the MIS approach may not only resolve pain but also better preserve the foot’s natural biomechanical function.
4. Back to the Future: A 1930s Surgery, Reinvented
While the minimally invasive technique is modern, the biomechanical principle behind the Zadek procedure is not new at all. It represents a brilliant revival of a long-forgotten surgical concept.
The procedure was first developed and published by Dr. Isadore Zadek in 1939. However, this original technique involved a large, open incision on the side of the heel. While the biomechanical concept was effective and patients had resolution of their posterior heel pain, this procedure was largely abandoned due to high rates of wound complications associated with such a significant incision in an area with delicate blood supply.
Today, modern MIS techniques have allowed surgeons to bring this effective concept back from the history books. Using specialized tools like a Shannon burr through incisions barely a few millimeters long, surgeons can now perform the osteotomy and achieve the same powerful biomechanical correction without the historical drawbacks of an open approach.
5. The Ultimate Safety Net: No Burned Bridges
A critical consideration for any surgery is what happens if it doesn’t work. What are the options for revision? This is where the MIS Zadek procedure offers one of its most significant advantages.
If the MIS Zadek procedure were to fail, a surgeon can still perform a traditional open Haglund’s resection as a next step. You never burn that bridge. The initial, less-invasive surgery does not preclude the more traditional approach if it later becomes necessary.
Perhaps even more surprising is the discovery that the MIS Zadek procedure can be successfully used to revise a failed open surgery. Some patients who underwent the traditional, open resection did not get better after surgery; these same patients have since seen significant improvement after a revision with the Zadek osteotomy says Dr. Gonzalez. This is quite a profound finding: a minimally invasive procedure designed to correct the biomechanics of the foot and ankle is able to succeed when the direct, open removal of tissue has already failed. Again, we find ourselves asking “why” or perhaps “how” this correction is so powerful; there is much that we continue to learn about the Zadek procedure. Nevertheless, using the MIS Zadek as a revision intervention does continue to yield promising results.
This versatility makes the MIS Zadek a lower-risk primary intervention for treating insertional Achilles tendinopathy.
Conclusion: A Shift in Thinking
The MIS Zadek procedure represents more than just a new technique; it signals a fundamental shift in surgical philosophy. We are moving the focus away from cutting out potentially “pathological” tissue, and toward correcting the underlying biomechanics that caused the problem in the first place. By restoring the body’s natural function through a minimally invasive procedure, surgeons are finding they can achieve superior results, with lower wound complication rates and faster recoveries.
As technology and our understanding of biomechanics continue to evolve, it prompts a thought-provoking question: Could the future of surgery be less about what we remove and more about what we restore?
Tyler A. Gonzalez, MD, MBA, is a fellowship-trained and board-certified orthopedic foot and ankle surgeon at Prisma Health Orthopedics in Columbia. After completing his bachelor’s degree at the University of California, Berkeley, he received a Master of Business Administration and his MD from UCLA in Los Angeles. He completed his residency in orthopedic surgery at Harvard Medical School in Boston and his fellowship in foot and ankle surgery at Cedar Sinai Medical Center in Los Angeles.
Throughout his career, Dr. Gonzalez has focused on improving patient care, medical education and research. His interest and passion in translational, clinical and biomechanical research has prompted over 100 peer-reviewed scientific publications and presentations. He routinely lectures at regional, national and international forums on foot and ankle topics and on improving value-based patient care.
Dr. Gonzalez is an active reviewer for publications, including Foot and Ankle International, Foot and Ankle Orthopaedics, and Foot and Ankle Specialist. He is a member of various foot and ankle surgery societies and is president and co-founder of Orthopaedic Foot and Ankle Society, Inc., a collaboration of foot and ankle surgeons to improve the delivery of healthcare, innovate on current surgical technologies and advance overall patient care.
He has a clinical interest in minimally invasive surgery, minimally invasive bunion correction, ankle replacements, ankle arthroscopy, foot and ankle arthritis, Charcot Marie Tooth disease, sports-related injuries, cartilage preservation and replacement surgery, bunion and hammertoe surgery, ligament/tendon disorders, dance medicine, and orthopedic trauma and fracture care.
This article is a summary of Dr. Gonzalez’s presentation, “Minimally Invasive Calcaneal Osteotomies,” from the 2025 Gait Keepers Journal Club on May 27. To view the full presentation with questions and answers–and see the agenda for the program, visit https://gaitkeepers.lerexpo.com/en/#agenda . Continuing education credits are available for this and many of the lerEXPO programs.